Fast absolute-reflectance method for the determination of tear film lipid layer thickness
Huth , et al.
U.S. patent number 10,368,738 [Application Number 14/298,176] was granted by the patent office on 2019-08-06 for fast absolute-reflectance method for the determination of tear film lipid layer thickness. This patent grant is currently assigned to Johnson & Johnson Surgical Vision, Inc.. The grantee listed for this patent is Johnson & Johnson Surgical Vision, Inc.. Invention is credited to Stan Huth, Denise Tran.
| United States Patent | 10,368,738 |
| Huth , et al. | August 6, 2019 |
Fast absolute-reflectance method for the determination of tear film lipid layer thickness
Abstract
A method of determining tear film lipid layer thickness. The method includes the steps of measuring a tear film aqueous plus lipid layer relative reflectance spectrum using a wavelength-dependent optical interferometer; converting the measured tear film aqueous plus lipid layer relative reflectance spectrum to a calculated absolute reflectance spectrum; and comparing the calculated absolute reflectance spectrum to a theoretical absolute lipid reflectance spectrum to determine a tear film lipid layer thickness.
| Inventors: | Huth; Stan (Newport Beach, CA), Tran; Denise (Irvine, CA) | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Applicant: |
|
||||||||||
| Assignee: | Johnson & Johnson Surgical
Vision, Inc. (Santa Ana, CA) |
||||||||||
| Family ID: | 53276279 | ||||||||||
| Appl. No.: | 14/298,176 | ||||||||||
| Filed: | June 6, 2014 |
Prior Publication Data
| Document Identifier | Publication Date | |
|---|---|---|
| US 20150351627 A1 | Dec 10, 2015 | |
| Current U.S. Class: | 1/1 |
| Current CPC Class: | A61B 3/101 (20130101) |
| Current International Class: | A61B 3/10 (20060101) |
| Field of Search: | ;351/200,205,206,207,208,209,210,215,221 |
References Cited [Referenced By]
U.S. Patent Documents
| 5045704 | September 1991 | Coates |
| 6236459 | May 2001 | Negahdaripour et al. |
| 6916096 | July 2005 | Eberl et al. |
| 7281801 | October 2007 | Wang |
| 7758190 | July 2010 | Korb et al. |
| 7866819 | January 2011 | Tuan |
| 7963522 | June 2011 | Hoover |
| 8192026 | June 2012 | Gravely et al. |
| 8585204 | November 2013 | Korb et al. |
| 8591033 | November 2013 | Korb et al. |
| 8602557 | December 2013 | Huth |
| 9456741 | October 2016 | Huth et al. |
| 9610011 | April 2017 | Huth et al. |
| 9681802 | June 2017 | Huth et al. |
| 2004/0212781 | October 2004 | Mihashi et al. |
| 2006/0109423 | May 2006 | Wang |
| 2007/0174014 | July 2007 | Halm |
| 2007/0215801 | September 2007 | Walsh et al. |
| 2008/0273171 | November 2008 | Huth et al. |
| 2009/0201465 | August 2009 | Huth |
| 2010/0253907 | October 2010 | Korb et al. |
| 2013/0141698 | June 2013 | Huth et al. |
| 2013/0169933 | July 2013 | Wang |
| 2013/0229624 | September 2013 | Korb et al. |
| 2013/0293842 | November 2013 | Grenon |
| 2014/0104574 | April 2014 | Grenon et al. |
| 2014/0118699 | May 2014 | Huth et al. |
| 2015/0351626 | December 2015 | Huth et al. |
| 2015/0351628 | December 2015 | Huth et al. |
| 2016/0345821 | December 2016 | Huth et al. |
| 2017/0280991 | October 2017 | Huth et al. |
| 2017/0280992 | October 2017 | Huth et al. |
| 2013163367 | Oct 2013 | WO | |||
Other References
|
Francine Behar-Cohen et.el. "ultraviolet damage to the eye revisited: eye-sun protection factor (E_SPF), a new ultraviolet protection label for eyewear", Aug. 2014, Clinical Ophthamology, vol. 8, pp. 87-104. cited by examiner . Atchison et. al., "Chromatic dispersions of the ocular media of human eyes", Jan. 2005, J. opt. soc. Am. A, vol. 22, No. 1, 29-37. cited by examiner . International Search Report for Application No. PCT/US2015/030385, dated Jul. 27, 2015, 3 pages. cited by applicant . Bosch S., et. al., "A Method for the Measurement of Reflectances of Spherical Surfaces," Measurement Science and Technology, 1993, vol. 4 (2), pp. 190-192. cited by applicant . Fogt N., et al., "Interferometric Measurement of Tear Film Thickness by Use of Spectra Oecillations," Journal of Optical Society of America, 1998, vol. 15 (1), pp. 268-275. cited by applicant . Gardner et al., "Tear Film Thickness: Responsiveness to Potential Cognitive Demands", American Academy of Optometry, Tampa Dec. 2004, 1 page. cited by applicant . Geldis et al., "The Impact of Punctual Occulsion on Soft Contact Lends Wearing Comfort and the Tear Film," Eye and Contact Lens, pp. 261-265, 2008, vol. 34 (5). cited by applicant . Goto E., et al., "Computer-Synthesis of an Interference Color Chart of Human Tear Lipid Layer. By a Colorimetric Approach," Investigative Ophthalmology and Visual Science, 2003, vol. 44(11), pp. 4693-4697. cited by applicant . Goto E., et al., "Differentiation of Lipid Tear Deficiency Dry Eye by Kinetic Analysis of Tear Interference Images," Archives of Ophthalmology, 2003, vol. 121 (2), pp. 173-180. cited by applicant . Hinel E., et al., "Concurrent interferometric Measures of Lipid Layer Thickness and Tear Film Thinning Before and After Application of Lipid Emulsion Drop", American Academy of Optometry, Anaheim Oct. 2008, 1 page. cited by applicant . International Preliminary Report on Patentability and Written Opinion for Application No. PCT/US08/062682, dated Nov. 10, 2009, 12 pages. cited by applicant . International Search Report for Application No. PCT/US08/062682, dated Nov. 5, 2008, 6 pages. cited by applicant . Kimball et al., Evaporation is the Primary Mechanism of Pre-Corneal Tear Film Thinning, [online], Oct. 2008 [retrieved on Feb. 25, 2009]. Retrieved from the Internet:< URL: http://www.aaopt.org/Submission/Search/SubmissionViewer.asp''SID=2>. cited by applicant . Kimball et al., Improving Interferometric Tear Thickness Measurements by Using Longer Wavelengths. [online], [retrieved on Feb. 25, 2009]. Retrieved from the Internet:< URL: http://www.aaopt.org/Submission/Search/SubmissionViewer.asp''SID=7>. cited by applicant . King S., et al., "Three Interferometric Methods for Measuring The Thickness of Layers of The Tear Film," Optometry and Vision Science, 1999, vol. 76 (1), pp. 19-32. cited by applicant . King S., et al., "Why does Dry Eye Affect Inferior Cornea More than Superior Cornea", American Academy of Optometry, 2002. pp. 1-2. cited by applicant . King-Smith et al., "In vivo Measurements of the Thickness of Human Corneal Endothelium and Descemets Membrane Using Interferometry. E-Abstract 157." Investigative Opthalmology & Visual Science, 2002, vol. 43. cited by applicant . King-Smith et al., "Noninvasive Measurement of the Thickness of the Human Corneal Endothelium and Descemet's Membrane", American Academy of Optometry, Dec. 8, 2001, pp. 1-2. cited by applicant . King-Smith et al., "Roughness of the Corneal Surface by Interferometry", Association for Research in Vision and Ophthalmology, May 6, 2007, 1 page. cited by applicant . King-Smith et al., "The Thickness of the Human Precorneal Tear Film. Evidence from Reflection Spectra," Investigative & Visual Science, pp. 3348-3359, 2000, vol. 41 (11). cited by applicant . King-Smith et al., "The Thickness of the Tear Film," Current Eye Research, pp. 357-368, 2004. vol. 29 (4-5), Taylor & Francis Health Sciences. cited by applicant . King-Smith P., et al., Interferometric Analysis of Reflections from the Tear Film and Ocular Surface, [online], [retrieved on Feb. 25, 2009]. Retrieved from the Internet:< URL: http://www.aaopt.org/Submission/Search/SubmissionViewer.asp''SID=4>. cited by applicant . King-Smith P., et al., "Measurement of the Thickness of the Lipid Layer of the Tear Film Using Reflection Spectra." Association for Research in Vision and Ophthalmology, Inc., 2008. Grand Floridian A, Program 1540. cited by applicant . King-Smith P.E., et al., "A Tear Layer of Thickness 1.6 to 7.3 Micrometer Determined from Reflectance Spectra," Investigative Ophthalmology & Visual Science, 1998, vol. 39 (4), pp. 2446-B303. cited by applicant . King-Smith P.E., et al., "Can the Mucus Layer of the Tear Film be Deomstrated by Interferometry", Investigative Ophthalmology & Visual Science, 2004, vol. 45, pp. 1-2. cited by applicant . King-Smith P. E., et al., "Further Evidence that the Thickness of the Normal Human Tear Film is about 3 Micrometre," Investigative Ophthalmology & Visual Science, 2000, vol. 41 (4), pp. 337-B337. cited by applicant . King-Smith P.E., et al., "Interferometric Imaging of the Full Thickness of the Precorneal Tear Film," Journal of the Optical Society of America A, Optics, Image Science, and Vision, 2006, vol. 23 (9), pp. 2097-2104. cited by applicant . King-Smith P.E., et al., "Is the Thickness of the Tear Film About 40 Micrometre or About 3 Micrometre", Investigative Ophthalmology & Visual Science, 1999, vol. 40 (4), pp. 2876-B751. cited by applicant . King-Smith P.E., et al., "Measurement of Tear Film Thickness by Spectro-Photometry," Investigative Ophthalmology & Visual Science, 1996, vol. 37 (3), pp. 4984-B594. cited by applicant . King-Smith P.,et al., "Is Inferior Tear Film Thinner than Superior Tear Film", Investigative Ophthalmology & Visual Science, 2003, vol. 44, pp. 2476. cited by applicant . Korb D.R., et al., "Tear Film Lipid Layer Thickness as a Function of Blinking," Cornea, 1994, vol. 13 (4), pp. 354-359. cited by applicant . Korb D.R., et al., "The Effect of Two Novel Lubricant Eye Drops on Tear Film Lipid Layer Thickness in Subjects With Dry Eye Symptoms," Optometry and Vision Science, 2005, vol. 82 (7) , pp. 494-601. cited by applicant . Nichols, et al., "Assessing Visual Parameters in Dry Eye Disease," Cornea and Contact Lens, [retrieved on Feb. 25, 2009]. Retrieved from the Internet:< URL: http://www.aaopt.org/Submissions.Search/SubmissionViewer.asp''SID=2>. cited by applicant . Nichols et al., "Lipid Layer Thickness and Tear Film Thinning Before and After Application of a Lipid Emulsion Drop,," Association for Research in Vision and Ophthalmoogy, 2008. cited by applicant . Nichols et al., "Tear Film Thickness and Thinning Rate Following a Six-Week Trial of 2% Diquafosol Tetrasodium vs. Placebo in Dry Eye Patients," 2006. cited by applicant . Nichols et al., "The Impact of Contact Lens Care Solutions on the Thickness of the Tear Film and Contact Lens," Cornea, Clinical Sciences, pp. 825-832, 2005, vol. 24 (7). cited by applicant . Nichols J.J., et al., "Hydrogel Contact Lens Binding Induces by Contact Lens Rewetting Drops," Optometry and Vision Science, 2008, vol. 85(4), pp. 236-240. cited by applicant . Nichols J.J., et al., "Thickness of The Pre- and Post-Contact Lens Tear Film Measured In Vivo by Interferometry," Investigative Ophthalmology & Visual Science, 2003, vol. 44 (1), pp. 68-77. cited by applicant . Nichols J.J., et al., "Thinning Rate of the Precorneal and Prelens Tear Films," Investigative Ophthalmology & Visual Science, 2005, vol. 46 (7), pp. 2353-2361. cited by applicant . Nicols et al, "Role of Lipid Layer as a Barrier to Pre-Lens Tear Film Thinning", American Academy of Optometry, Anaheim Oct. 25, 2008, 1 page. cited by applicant . Scaffifi R.C., et al., "Comparison of the Efficacy of Two Lipid Emulsion Eyedrops in Increasing Tear Film Lipid Layer Thickness," Eye Contact Lens, 2007, vol. 33 (1), pp. 38-44. cited by applicant . Schlote T., et al., "Marked Reduction and Distinct Patterns of Eye Blinking in Patients With Moderately Dry Eyes During Video Display Terminal Use," Graefe's Archive for Clinical and Experimental Ophthalmology, 2004, vol. 242 (4), pp. 306-312. cited by applicant . Schott BK7 Refractive Index Reference, Which is Equivalent to and Replaces Schott Technical Information Document TIE-29, 2005, 17 pages, retrieved from Internet: <URL:http://ltiw3.iams.sinica.edu.tw/support/OpticsGuide/chap04_Materi- al_Properties.pdf>. cited by applicant . Stenzel O., "The Physics of Thin Film Optical Spectra: An Introduction," in: Springer Series in Surface Sciences, 2005, vol. 44, ERTL G., Eds., Springer-Verlag Berlin Heidelberg, pp. 71-98. cited by applicant . Tiffany J.M., et al., "Refractive Index of Meibomian and Other Lipids," Current Eye Research, 1986, vol. 5 (11), pp. 887-889. cited by applicant . Yap M., "Tear Break-up Time is Related to Blink Frequency," Acta Ophthalmologica, 1991, vol. 69 (1), pp. 92-94. cited by applicant . Zhu H., et al., "A Mathematical Model for Ocular Tear and Solute Balance," Current Eye Research, 2005, vol. 30 (10), pp. 841-854. cited by applicant . International Search Report and Written Opinion for Application No. PCT/US2015/030392, dated Oct. 5, 2015, 12 pages. cited by applicant . Examination Report for European Patent Application No. 15735765.8, dated Feb. 1, 2018, 4 pages. cited by applicant . Notice of Allowance for U.S. Appl. No. 14/831,678, dated Feb. 16, 2017, 9 pages. cited by applicant . Notice of Allowance for U.S. Appl. No. 15/627,077, dated May 4, 2018, 7 pages. cited by applicant . Non-Final Rejection for U.S. Appl. No. 14/298,036, dated Nov. 2, 2015, 7 pages. cited by applicant . Notice of Allowance for U.S. Appl. No. 14/298,036, dated May 4, 2016, 7 pages. cited by applicant . Supplemental Notice of Allowance for U.S. Appl. No. 14/298,036, dated Aug. 17, 2016, 7 pages. cited by applicant . Non-Final Office Action for U.S. Appl. No. 15/172,083, dated Oct. 5, 2016, 5 pages. cited by applicant . Notice of Allowance for U.S. Appl. No. 15/172,083, dated Dec. 2, 2016, 7 pages. cited by applicant . Non-Final Office Action for U.S. Appl. No. 15/625,815, dated Jul. 2, 2018, 4 pages. cited by applicant . Examination Report for European Patent Application No. 15735765.8, dated Oct. 18, 2018, 4 pages. cited by applicant . International Preliminary Report on Patentability and Written Opinion for International Patent Application No. PCT/US2015/030385, dated Dec. 15, 2016, 12 pages. cited by applicant . Examination Report No. 1 for Australian Patent Application No. 2015268808, dated May 3, 2019, 3 pages. cited by applicant . Examination Report No. 1 for Australian Patent Application No. 2015268810, dated May 3, 2019, 3 pages. cited by applicant. |
Primary Examiner: Tallman; Robert E.
Attorney, Agent or Firm: Withrow & Terranova, P.L.L.C.
Claims
What is claimed is:
1. A method of determining tear film lipid layer thickness, comprising the steps of: measuring a tear film aqueous plus lipid layer relative reflectance spectrum using a wavelength-dependent optical interferometer; converting the measured tear film aqueous plus lipid layer relative reflectance spectrum to a calculated absolute reflectance lipid spectrum, wherein the calculated absolute reflectance lipid spectrum is calculated based on wavelength-dependent refractive indices for air, lipid, and aqueous phases and wherein the wavelength-dependent refractive indices for lipid are based upon a Sellmeier equation form; and comparing the calculated absolute reflectance lipid spectrum to a theoretical absolute reflectance lipid spectrum to determine a tear film lipid layer thickness.
2. The method of claim 1, wherein the tear film aqueous plus lipid layer relative reflectance spectrum is measured relative to a reference material.
3. The method of claim 2, wherein converting the measured tear film aqueous plus lipid layer relative reflectance spectrum to the calculated absolute reflectance lipid spectrum comprises multiplying the measured tear film aqueous plus lipid layer relative reflectance spectrum at a plurality of wavelengths times an absolute reference lipid spectrum for the reference material obtained at the plurality of wavelengths.
4. The method of claim 3, wherein the reference material has a radius of curvature of 7.75 mm.
5. The method of claim 3, wherein converting the measured tear film aqueous plus lipid layer relative reflectance spectrum to the calculated absolute reflectance lipid spectrum further comprises dividing by a correction factor to correct for differences between the theoretical absolute reflectance lipid spectrum and the calculated absolute reflectance lipid spectrum.
6. The method of claim 3, wherein converting the measured tear film aqueous plus lipid layer relative reflectance spectrum to the calculated absolute reflectance lipid spectrum further comprises dividing by 100.
7. The method of claim 1, wherein comparing the calculated absolute reflectance lipid spectrum to the theoretical absolute reflectance lipid spectrum comprises iteratively comparing the calculated absolute reflectance lipid spectrum to a plurality of theoretical absolute reflectance lipid spectra.
8. The method of claim 7, wherein iteratively comparing the calculated absolute reflectance lipid spectrum to the plurality of theoretical absolute reflectance lipid spectra comprises minimizing a sum of least squares differences between the calculated absolute reflectance lipid spectrum and the plurality of theoretical absolute reflectance lipid spectra.
9. The method of claim 8, wherein minimizing the sum of least squares differences comprises using a Levenburg-Marquardt algorithm.
10. The method of claim 7, wherein iteratively comparing the calculated absolute reflectance lipid spectrum to the plurality of theoretical absolute reflectance lipid spectra comprises starting the iteration with the theoretical absolute reflectance lipid spectrum for a 65 nm thick lipid layer.
11. The method of claim 1, wherein comparing the calculated absolute reflectance lipid spectrum to the theoretical absolute reflectance lipid spectrum does not include a comparison of the calculated absolute reflectance lipid spectrum to a theoretical absolute reflectance aqueous spectrum to determine a tear film aqueous layer thickness and a comparison of the calculated absolute reflectance lipid spectrum to a theoretical film stack to determine corneal surface refractive index.
12. A system for determining tear film lipid layer thickness, comprising: a wavelength-dependent optical interferometer; and a controller in communication with the wavelength-dependent optical interferometer, the controller configured to measure a tear film aqueous plus lipid layer relative reflectance spectrum using the wavelength-dependent optical interferometer, convert the measured tear film aqueous plus lipid layer relative reflectance spectrum to a calculated absolute reflectance lipid spectrum, wherein the calculated absolute reflectance lipid spectrum is calculated based on wavelength-dependent refractive indices for air, lipid, and aqueous phases and wherein the wavelength-dependent refractive indices for lipid are based upon a Sellmeier equation form, and compare the calculated absolute reflectance lipid spectrum to a theoretical absolute reflectance lipid spectrum to determine a tear film lipid layer thickness.
13. The system of claim 12, wherein the tear film aqueous plus lipid layer relative reflectance spectrum is measured relative to a reference material.
14. The system of claim 13, wherein the controller, in order to convert the measured tear film aqueous plus lipid layer relative reflectance spectrum to a calculated absolute reflectance lipid spectrum, is further configured to multiply the measured tear film aqueous plus lipid layer relative reflectance spectrum at a plurality of wavelengths times an absolute reference lipid spectrum for the reference material obtained at the plurality of wavelengths.
15. The system of claim 14, wherein the reference material has a radius of curvature of 7.75 mm.
16. The system of claim 14, wherein the controller, in order to convert the measured tear film aqueous plus lipid layer relative reflectance spectrum to the calculated absolute reflectance lipid spectrum, is further configured to divide by a correction factor to correct for differences between the theoretical absolute reflectance lipid spectrum and the calculated absolute reflectance lipid spectrum.
17. The system of claim 14, wherein the controller, in order to convert the measured tear film aqueous plus lipid layer relative reflectance spectrum to the calculated absolute reflectance lipid spectrum, is further configured to divide by 100.
18. The system of claim 12, wherein the controller, in order to compare the calculated absolute reflectance lipid spectrum to the theoretical absolute reflectance lipid spectrum, is further configured to iteratively compare the calculated absolute reflectance lipid spectrum to a plurality of theoretical absolute reflectance lipid spectra.
19. The system of claim 18, wherein the controller, in order to iteratively compare the calculated absolute reflectance lipid spectrum to the plurality of theoretical absolute reflectance lipid spectra, is further configured to minimize a sum of least squares differences between the calculated absolute reflectance lipid spectrum and the plurality of theoretical absolute reflectance lipid spectra.
20. The system of claim 19, wherein the controller, in order to minimize the sum of least squares differences, is further configured to use a Levenburg-Marquardt algorithm.
21. The system of claim 18, wherein the controller, in order to iteratively compare the calculated absolute reflectance lipid spectrum to the plurality of theoretical absolute reflectance lipid spectra, is further configured to start the iteration with the theoretical absolute reflectance lipid spectrum for a 65 nm thick lipid layer.
22. The system of claim 12, wherein the controller, in order to compare the calculated absolute reflectance lipid spectrum to the theoretical absolute reflectance lipid spectrum, is further configured not to include a comparison of the calculated absolute reflectance lipid spectrum to a theoretical absolute reflectance aqueous spectrum to determine a tear film aqueous layer thickness and a comparison of the calculated absolute reflectance lipid spectrum to a theoretical film stack to determine corneal surface refractive index.
Description
CROSS-REFERENCE TO RELATED APPLICATIONS
The present application is related to U.S. patent application Ser. No. 14/298,036 to Huth and Tran, "Method for Rapid Calculation of Tear Film Lipid and Aqueous Layer Thickness and Ocular Surface Refractive Index from Interferometry Spectra," filed Jun. 6, 2014, now issued as U.S. Pat. No. 9,456,741 which is incorporated herein by reference in its entirety.
BACKGROUND
The present invention relates to determination of tear film lipid layer thickness.
Dry eye disease is most often caused by excessive tear film evaporation, leading to hyperosmolarity of the tear film, resulting in ocular surface inflammation and exacerbation of the problem. Excessive tear film evaporation is often caused by an abnormal tear film lipid layer, either in amount or in quality. The amount or quality of tear film lipid can manifest itself in changes in thickness of the lipid layer. Generally, a thicker lipid layer is associated with a normal tear film, whereas the opposite is often the case for dry eye. Present clinical measurements of the tear film lipid layer are for the most part qualitative or semi-quantitative in nature. Korb, in U.S. Pat. Nos. 8,591,033 and 8,585,204, disclose a quantitative method for measuring the thickness of the tear film lipid layer. However, this method does not measure the lipid layer over the central cornea where tear film thinning and breakup due to evaporation is maximal and where it is believed a better diagnosis of dry eye can be obtained. Huth, in U.S. Pat. No. 8,602,557 B2 (incorporated herein by reference in its entirety) also disclose a quantitative method for measuring the thickness of the tear film lipid layer as part of a method to simultaneously measure the tear film aqueous layer and the corneal surface refractive index. However, this method requires as long as 475 seconds to complete the calculations for a single tear film spectrum.
SUMMARY
Thus, it is the object of the present invention to overcome the limitations of the prior art, and to increase the sensitivity, accuracy and precision of the measurement of the tear film lipid layer. Fast, accurate and precise lipid layer thickness-determination methods are also needed for the quantitative evaluation of the effects of novel dual-function lipid-supplementation tear formulas on the tear film lipid layer. Such methods are also needed to evaluate the effects of other eye drops, ophthalmic dry eye drugs and MPS solutions, and contact lenses on the tear film lipid layer.
In one embodiment, the invention provides a method of determining tear film lipid layer thickness. The method includes the steps of measuring a tear film aqueous plus lipid layer relative reflectance spectrum using a wavelength-dependent optical interferometer; converting the measured tear film aqueous plus lipid layer relative reflectance spectrum to a calculated absolute reflectance spectrum; and comparing the calculated absolute reflectance spectrum to a theoretical absolute lipid reflectance spectrum to determine a tear film lipid layer thickness.
In another embodiment the invention provides a system for determining tear film lipid layer thickness. The system includes a wavelength-dependent optical interferometer and a controller. The controller is in communication with the interferometer and is configured to measure a tear film aqueous plus lipid layer relative reflectance spectrum using the interferometer, convert the measured tear film aqueous plus lipid layer relative reflectance spectrum to a calculated absolute reflectance spectrum, and compare the calculated absolute reflectance spectrum to a theoretical absolute lipid reflectance spectrum to determine a tear film lipid layer thickness.
Other aspects of the invention will become apparent by consideration of the detailed description and accompanying drawings.
BRIEF DESCRIPTION OF THE DRAWINGS
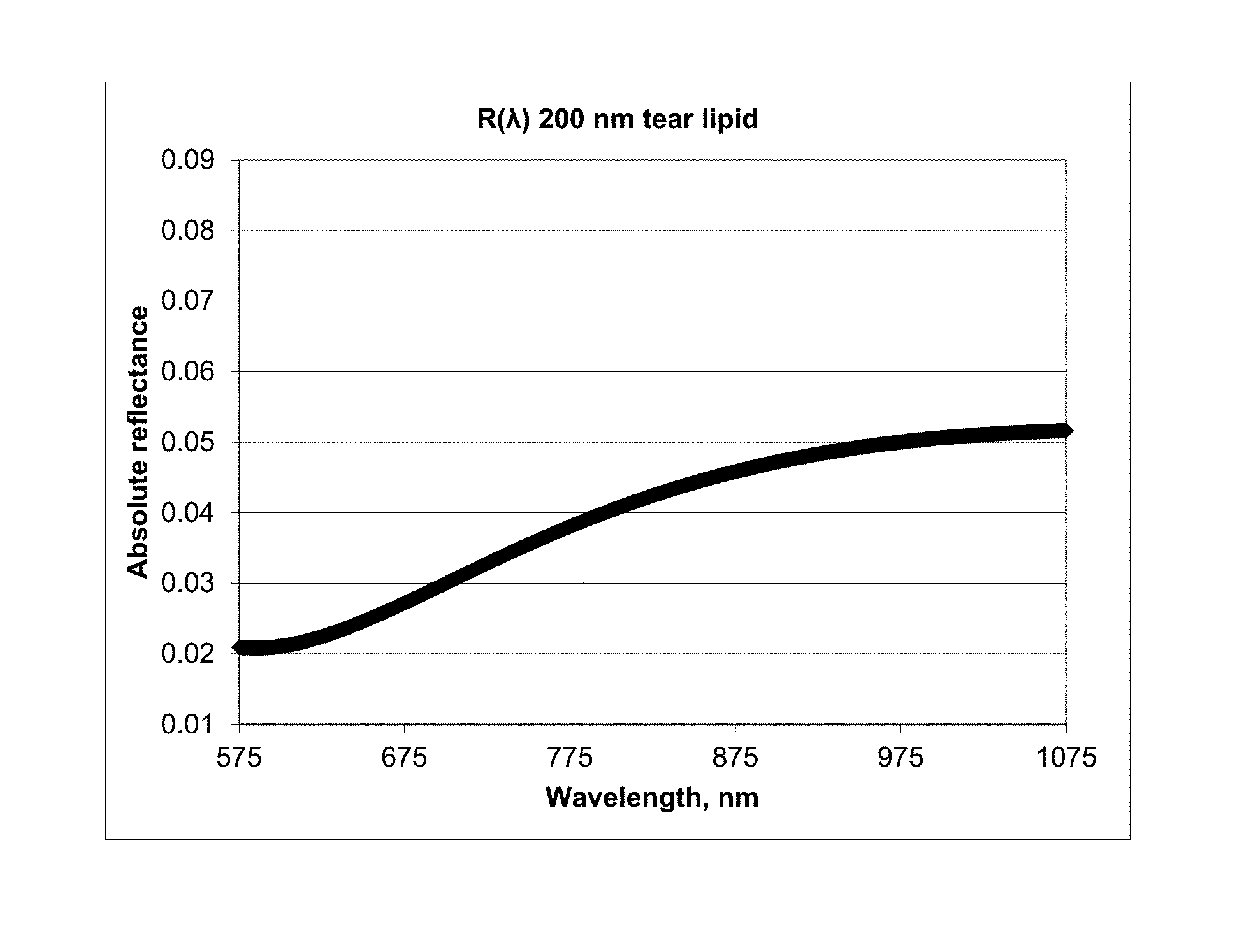
FIG. 1 shows absolute reflectance for a 200 nm tear lipid film layer measured in a wavelength range of 575 nm to 1075 nm.
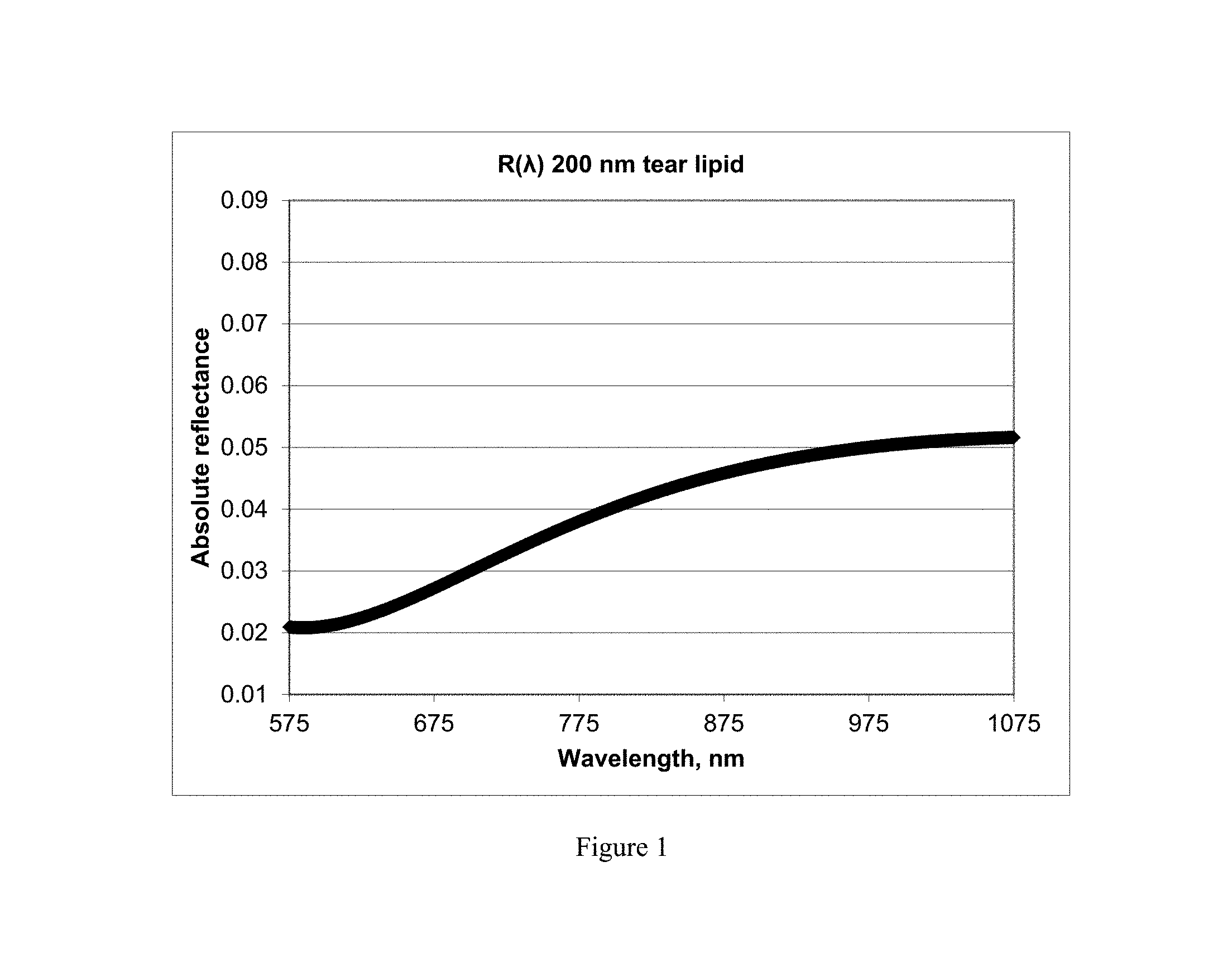
FIG. 2 shows calculated absolute reflectance spectra for lipid layers thicknesses in a range of 0-140 nm.
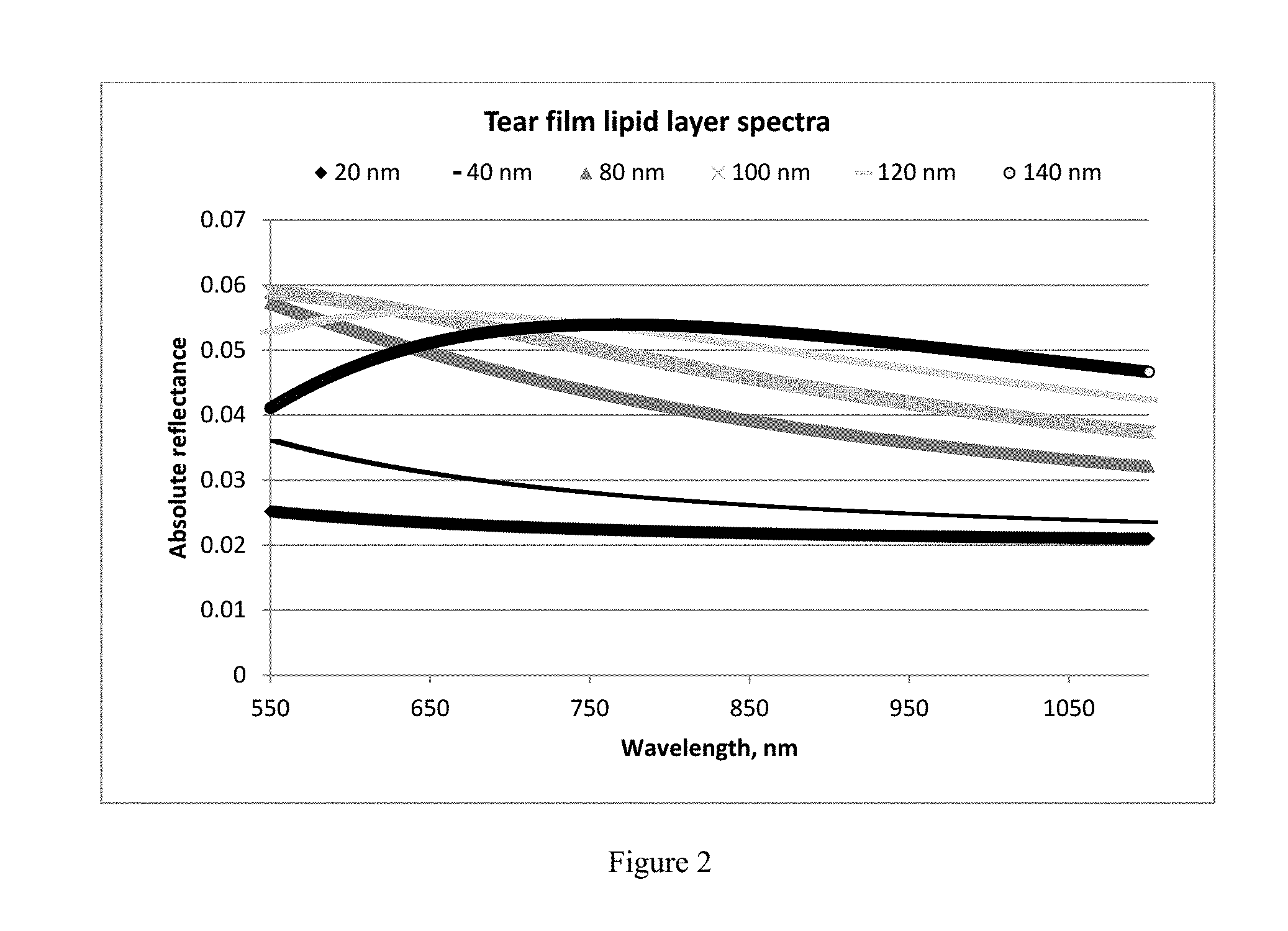
FIG. 3 shows an unmodified tear film lipid spectrum obtained using an interferometer.
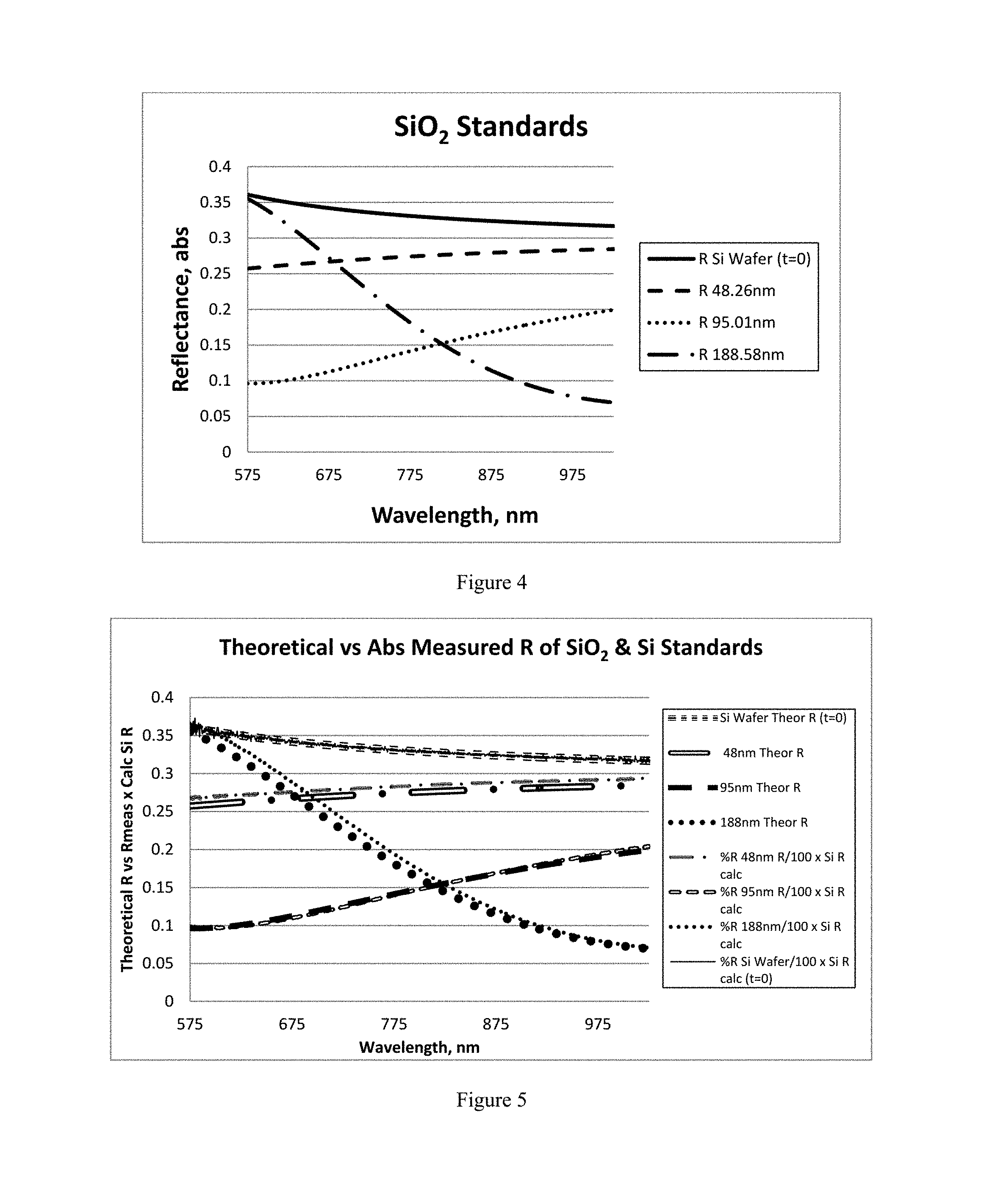
FIG. 4 shows absolute reflectance spectra for SiO.sub.2 layers having thicknesses from 0-188.6 nm.
FIG. 5 shows the results of converting measured relative SiO.sub.2 spectra to calculated absolute reflectance spectra, where each absolute reflectance spectrum obtained from measured data is compared to an equivalent calculated theoretical spectrum.
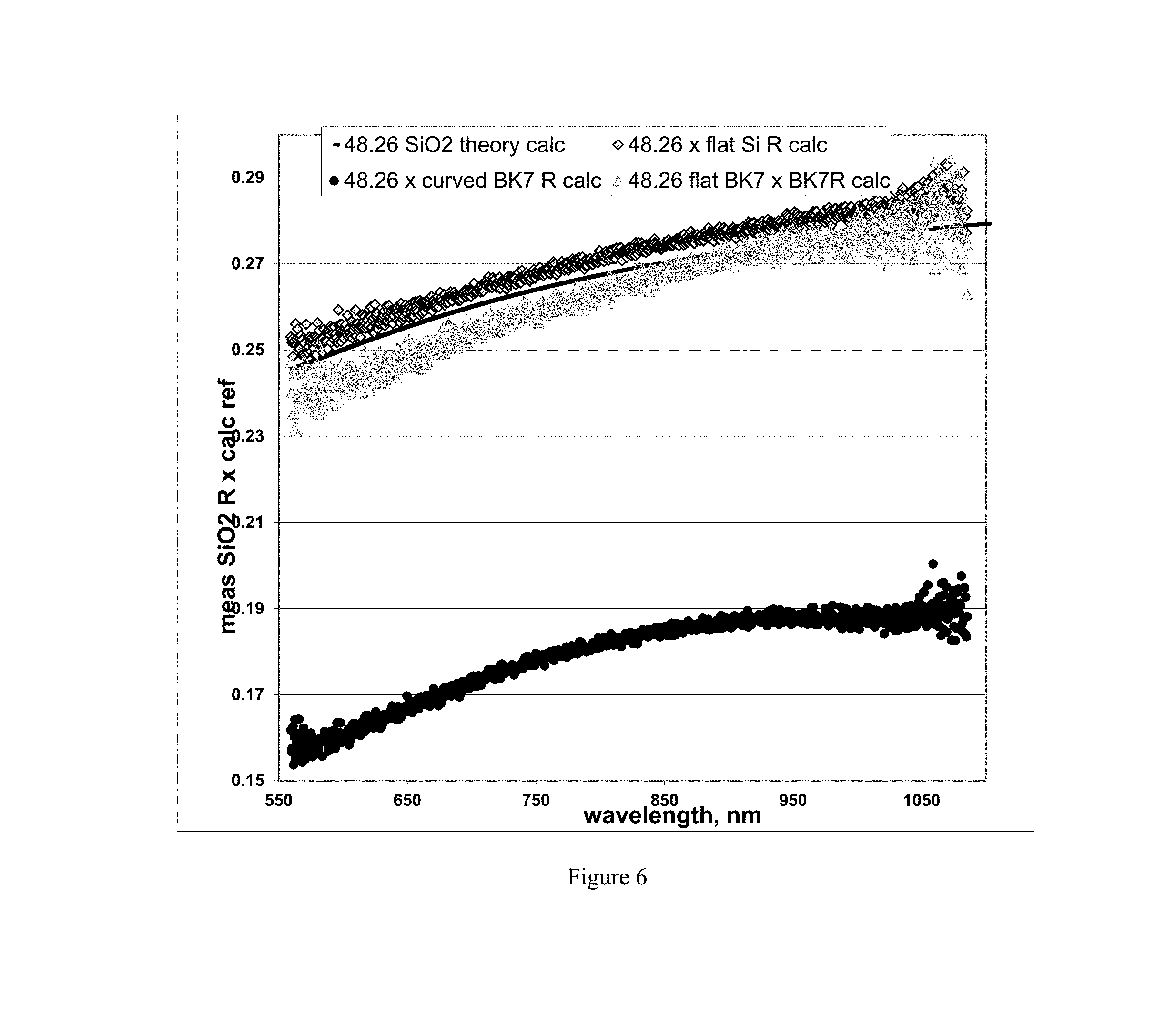
FIG. 6 shows the comparison between a calculated theoretical spectrum for a 48.26 nm SiO2 thin film standard compared to calculated absolute reflectance spectra obtained by converting measurements of the relative reflectance spectra for the 48.26 nm SiO.sub.2 thin film standard which were measured relative to various reference materials, including a flat silicon wafer, a flat BK7 glass plate, and a curved BK7 glass lens having an identical radius of curvature as the human cornea, i.e. 7.75 mm.
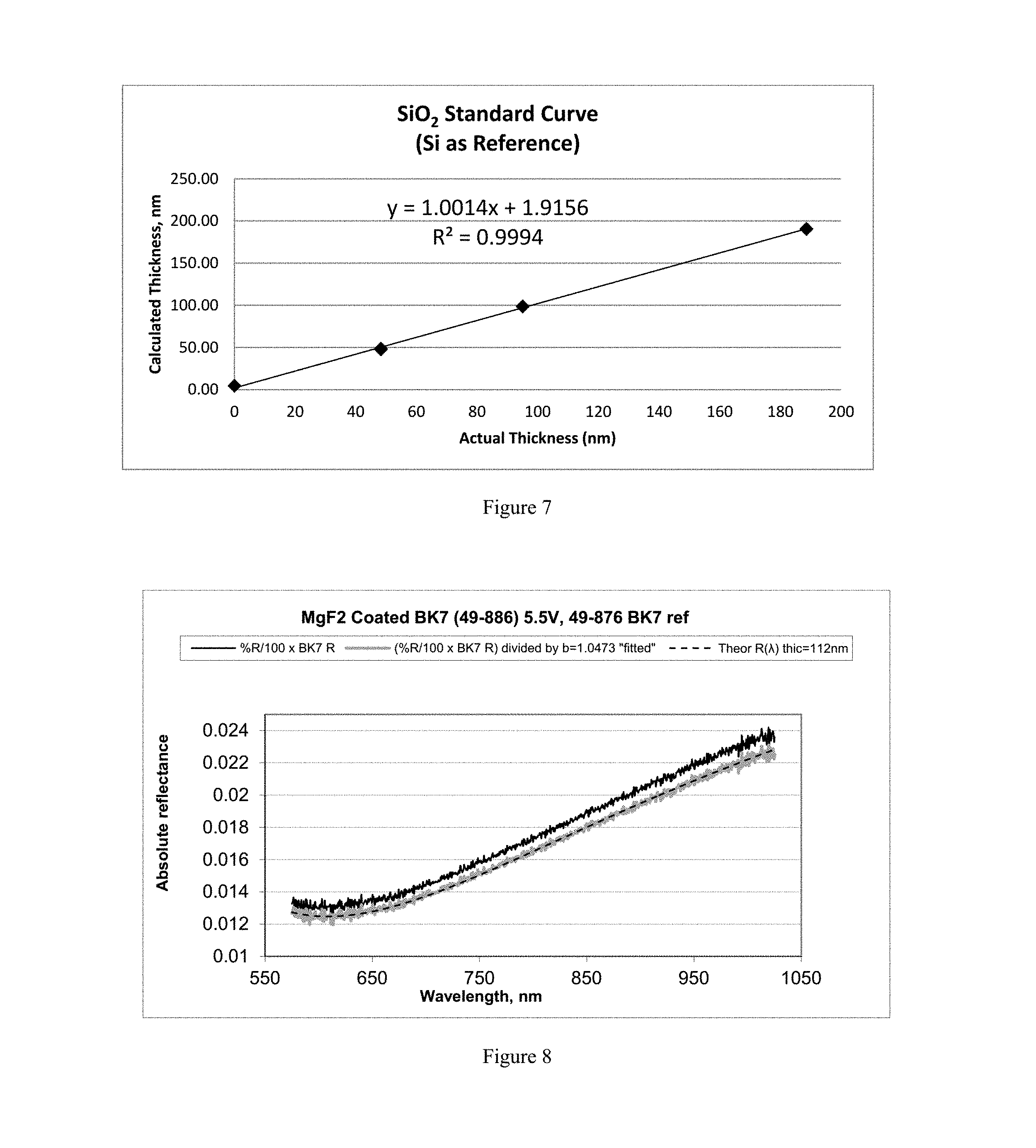
FIG. 7 shows a standard curve comparing the actual thickness (in nm) of the SiO2 thin film standards to the thickness determined using the methods disclosed herein.
FIG. 8 shows a theoretical spectrum (dashed line, ----) vs. b-term fitted spectrum (light grey line, overlapping dashed line) and spectrum without the b-term fit (black line).
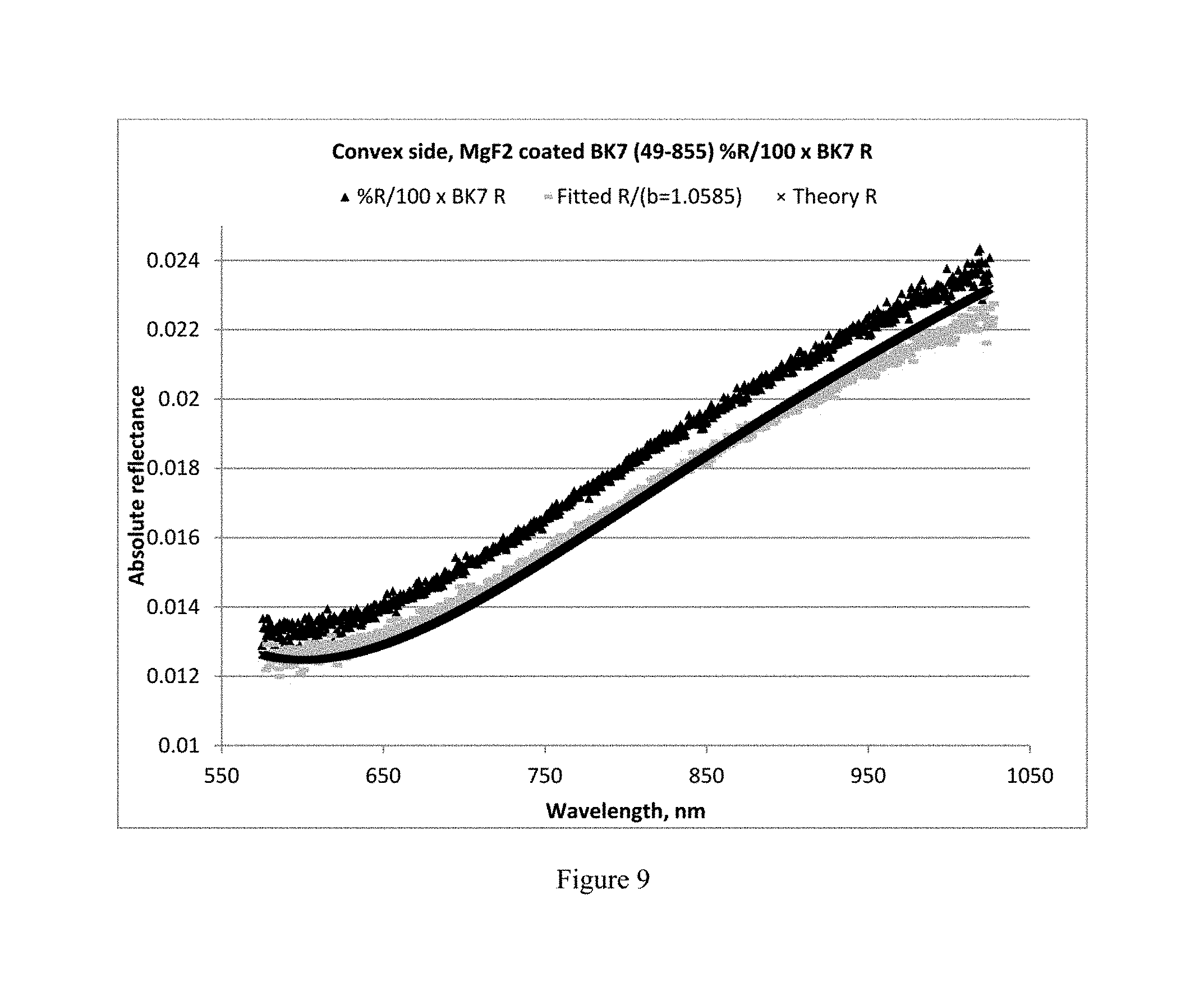
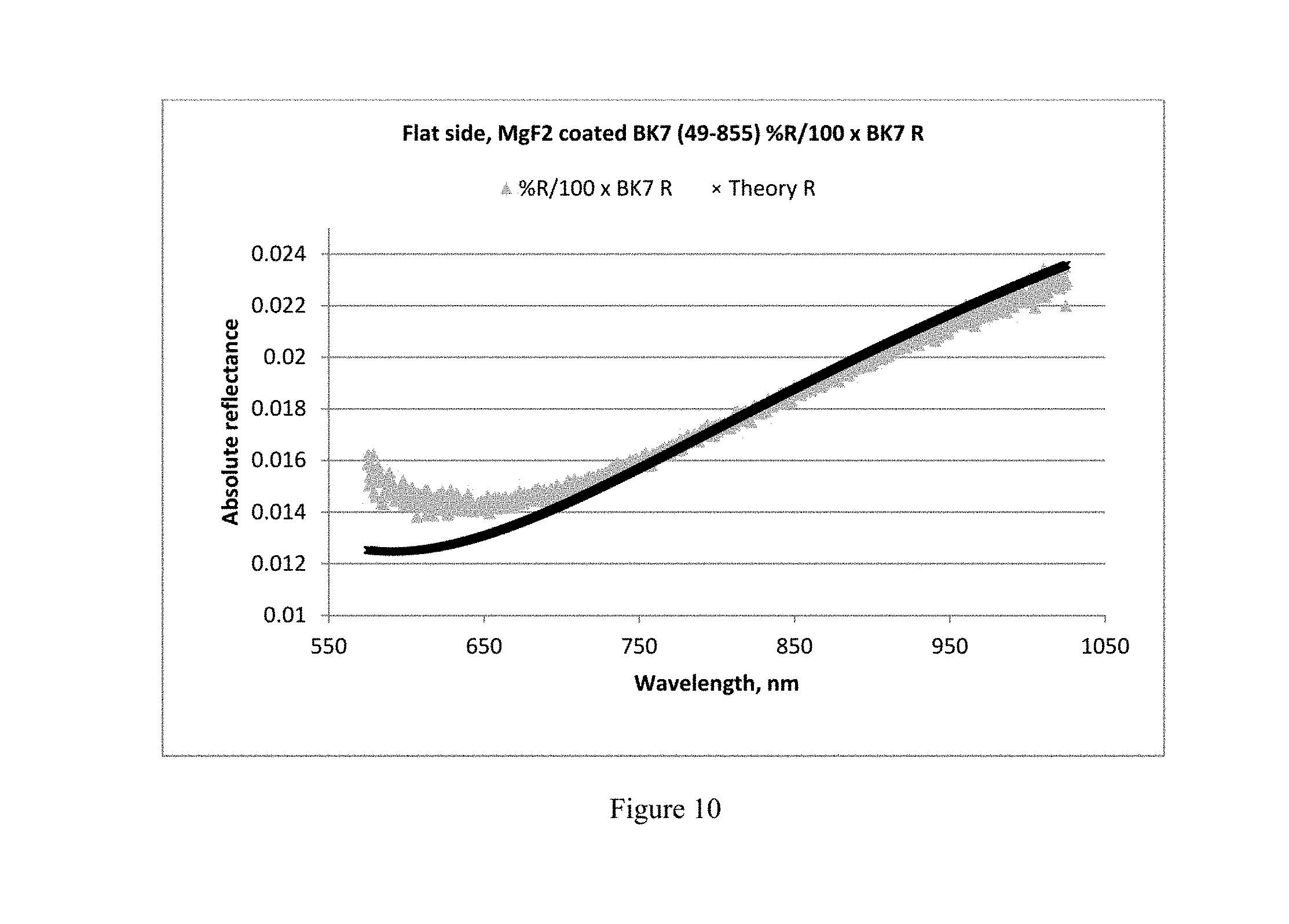
FIGS. 9 and 10 show calculated absolute reflectance spectra for the MgF.sub.2 coating on the convex (FIG. 9) and the flat (FIG. 10) faces of a coated BK7 lens, both compared to a calculated theoretical spectrum for the MgF.sub.2 coating.
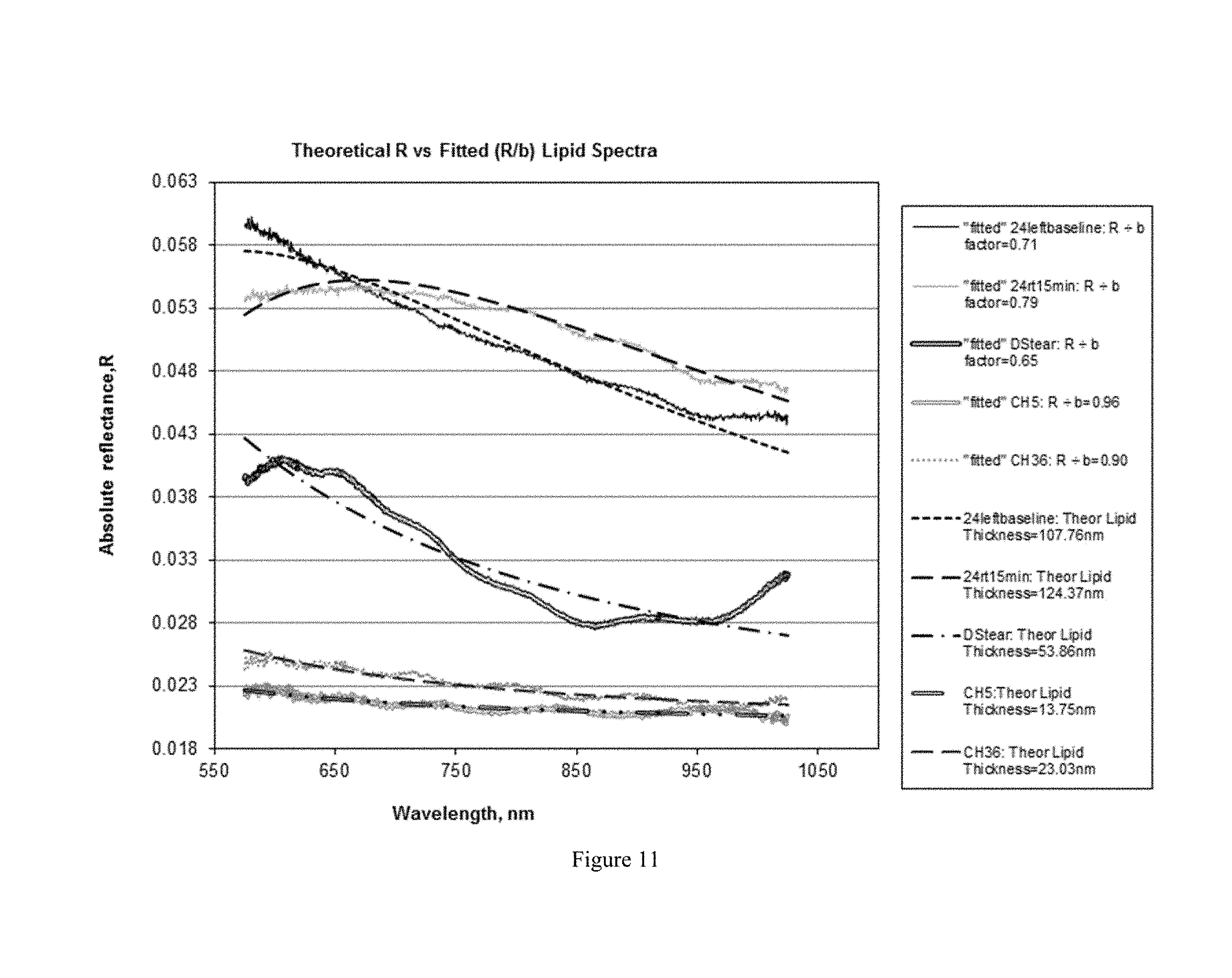
FIG. 11 shows calculated absolute reflectance spectra for tear film lipid spectra compared to calculated theoretical spectra.
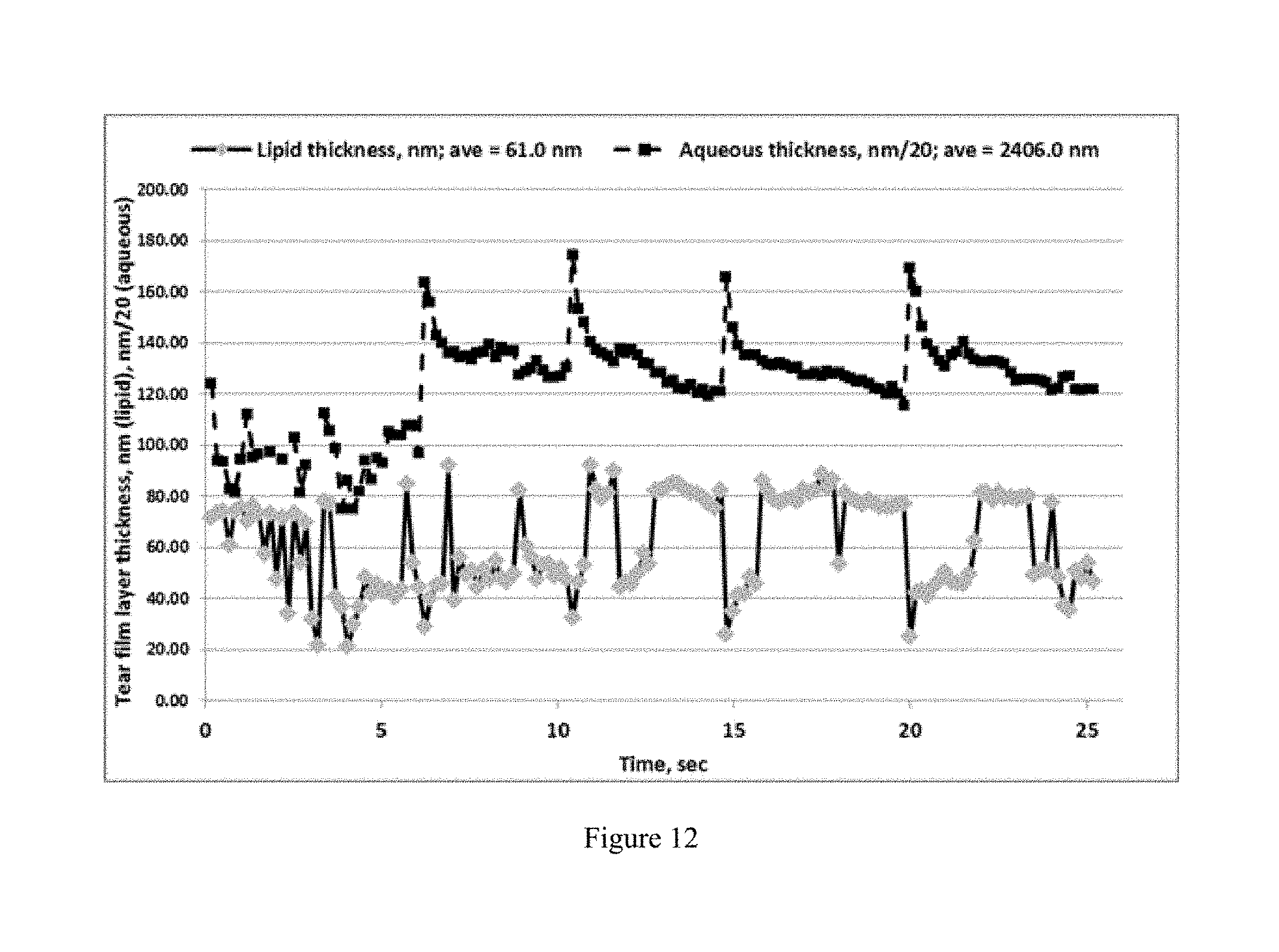
FIG. 12 shows thicknesses of the lipid (diamonds) vs. aqueous (squares) tear film layers during blinking (downward spikes in lipid thickness measurements) of the subject's eyelids.
DETAILED DESCRIPTION
Before any embodiments of the invention are explained in detail, it is to be understood that the invention is not limited in its application to the details of construction and the arrangement of components set forth in the following description or illustrated in the following drawings. The invention is capable of other embodiments and of being practiced or of being carried out in various ways.
Human tear film lipid layer thickness is believed to be between 20-200 nm. Central corneal tear film lipid layer thickness rarely exceeds about 120 nm, however, and also can be less than 20 nm in thickness. Normal wavelength-dependent optical interferometric methods for the determination of thin film thickness, based upon the analysis of the increasing number of cosine-function spectral oscillations with thickness, are unsuitable for this range. This is so because even at 200 nm thickness, only half an oscillation is visible within the 575-1075 nm spectral wavelength range of the typical optical interferometer (FIG. 1).
Accordingly, the answer to this problem is to base the thicknesses upon absolute optical reflectivity, also illustrated in FIG. 1, where absolute reflectivity of a 200 nm lipid layer is 0.02=2% at 575 nm. Thus, one needs to compare the absolute reflectivity spectrum of a tear lipid layer to a standard reflectivity spectrum such as seen in FIG. 1. The approach to achieving this is disclosed herein.
Interferometry measurements are typically determined as relative percent light reflection values, where the measurements from a subject's tear film and cornea are expressed relative to measurements obtained from a reference material (e.g. a particular glass material having a radius of curvature comparable to that of a cornea, e.g. ranging from 7-9 mm, in particular 7.75 mm). The ratio of the light reflectance from the subject's tear film and cornea, R(.lamda.) sample, to the light reflectance from the reference, R(.lamda.) reference, is multiplied by 100 by typical spectrometer and CCD detector software, so that the final relative light reflection values are expressed as percentages; the percentage values are determined for a range of wavelengths to obtain a spectrum. Thus, the y-axis of a measured spectrum corresponds to 100.times.R(.lamda.) sample/R(.lamda.) reference.
As an initial step in the development of the methods of the present invention, the theoretical absolute spectra for lipid layers of various thicknesses were calculated. Given that these theoretical absolute spectra have similar shapes or slopes to one another, but different absolute optical reflectivity at different wavelengths, correlating the theoretical absolute spectra with observed spectra requires determining the absolute reflectance spectrum from the measured data and correlating the absolute spectra with the theoretical spectra. Experimentation is required, however, to account for discrepancies between theoretical predicted spectra and actual measured spectra. Lipid layer standards of known thicknesses are not available and so it is not possible to perform calibrations using lipids. Instead, a series of calibrations was performed using commercially-available standards having layers of silicon dioxide of known thicknesses, comparable to thicknesses of tear film lipid layers. The measured spectra for the silicon dioxide standards were compared to the predicted theoretical absolute spectra for silicon dioxide layers of the same thicknesses and a correction algorithm was produced which can be used to obtain the absolute reflectance values for measured tear film lipid layers. The correction algorithm accounts for changes in light reflection arising from the geometry of a curved reference lens or from non-orthogonal placement of a flat reference surface with respect to incident light and from out-of-focus light reflection.
In various embodiments, the disclosed methods are modifications of a procedure for calculation of absolute reflectance of the presumed tear structure, involving an air interface with a single lipid layer overlying an aqueous layer.
In the aforementioned procedure, n.sub.0, n.sub.1, and n.sub.2 are the refractive indices of the air, lipid layer, and aqueous layer, respectively, for which fixed values of n.sub.0=1, n.sub.1=1.48, and n.sub.2=1.33 have been used. In one embodiment of the present invention, the respective complex refractive indices are used for n.sub.1 and n.sub.2, each of which changes with wavelength.
The Fresnel indices of reflection r.sub.1 and r.sub.2 for the air-lipid and lipid-aqueous interfaces are, respectively: r.sub.1=(n.sub.0-n.sub.1)/(n.sub.0+n.sub.1) and r.sub.2=(n.sub.1-n.sub.2)/(n.sub.1+n.sub.2)
Since energy is proportional to the square of amplitude, R(.lamda.)=R.times.R*=|R.sup.2|, where R* is the conjugate complex numbers of R. Thus, from Euler's equation: R(.lamda.)=(r.sub.1.sup.2+r.sub.2.sup.2+2r.sub.1r.sub.2 cos 2.delta..sub.1)/(1+r.sub.1.sup.2r.sub.2.sup.2+2r.sub.1r.sub.2 cos 2.delta..sub.1)= 1-(8n.sub.0n.sub.1.sup.2n.sub.2)/((n.sub.0.sup.2+n.sub.1.sup.2)(n.sub.1.s- up.2+n.sub.2.sup.2)+4n.sub.0n.sub.1.sup.2n.sub.2+(n.sub.0.sup.2-n.sub.1.su- p.2)(n.sub.1.sup.2-n.sub.2.sup.2)cos 2.delta..sub.1)
where a phase difference between two waves r.sub.1 and r.sub.2, is 2.delta..sub.1 and 2.delta..sub.1=(4.pi./.lamda.)n.sub.1d cos .phi..sub.1
where .phi..sub.1 is the angle of refraction of the incident light upon the lipid layer,
which=9.369.degree. for the wavelength-dependent optical interferometer used in the methods of the present invention, thus cos .phi..sub.1=0.986659.
The complex refractive indices for n.sub.1 (lipid) and n.sub.2 (aqueous) are used: n.sub.1= nd=y=sqrt(1+(((-851.03)*x*x)/(x*x-(816.139)))+(((420.267)*x*x)/(x*x-(-706- .86))) plus(((431.856)*x*x)/(x*x-(2355.29))))
where x=wavelength
and where nd=Sellmeier equation form of tear meibomian lipid refractive index derived from primary refractive index data from Tiffany, J M. Refractive index of meibomian and other lipids. Current Eye Research. 5(11), 1986; 887-889: 430 nm: nd=1.5126; 450 nm:1.5044; 510 nm: 1.4894; 590 nm:1.4769; 710 nm:1.4658. The Sellmeier equation coefficients were derived by fitting the limited Tiffany data (no data exist beyond 710 nm, where most of the spectral range of the interferometer exists (spectral range: 559-1085 nm)) first to a polynomial (nd=5.04e-7.times.2-0.00736x+1.73481, wherein x=wavelength) to generate forecasted refractive index values at 600, 620, 640 and 680 nm, followed by fitting the Tiffany+forecasted refractive index data set to the Sellmeier equation format wherein refractive index data beyond 710 nm could be calculated and utilized. The Sellmeier equation format for lipid refractive index data is believed to provide more accurate refractive index information, which is critical for accurate lipid layer thickness calculations. n.sub.2=1.32806+0.00306*(1000/.lamda.)^2
Using the above equations, an Excel spreadsheet is created in which the values of the three refractive indices n.sub.0, n.sub.1 and n.sub.2 are calculated (except for n.sub.0, which is always 1) for the wavelengths within the wavelength range measured by the interferometer (e.g., for wavelengths between 559-1085 nm). Then, using the expanded Euler's equation with all terms, R(.lamda.) is calculated for a series of lipid layer thicknesses, d. The results from 575-1075 nm are seen in FIG. 2, presenting a series of absolute-value reflectance spectra for lipid layers of various thicknesses.
The spectrum (not shown) for a lipid layer of 0 nm thickness is very flat, lies just below that of a 20 nm thick lipid layer and produces an absolute reflectance of 0.02% of the incident light at 550 nm. It can be seen in FIG. 2 that there is little difference in the slopes of the lipid layer spectra between 20-100 nm thicknesses, further reinforcing the need to base lipid layer thickness calculations upon absolute reflectance values rather than parameters such as the slope or shape of the spectra. Thus, a 20 nm lipid layer will reflect about 0.025=2.5% of the incident light at 550 nm, whereas a 100 nm lipid layer will reflect about 0.06=6% of the incident light at 550 nm. At 120 nm thickness and larger, the slope of absolute reflectance begins to change from a negative slope to a flat slope. Beyond 140 nm thickness, as seen in FIG. 1 for a 200 nm thickness, the slope becomes positive. Slope evaluation at 120 nm and beyond becomes a valuable tool to distinguish between a thin or thick lipid layer.
Thus, for the majority of tear film lipid layers between 0-100 nm thickness, it is not a simple exercise to measure a tear lipid spectrum with a wavelength-dependent optical interferometer and compare it to one of the above absolute reflectance spectra. This is illustrated in FIG. 3, which shows an unmodified measured tear lipid spectrum.
Accordingly, each measured spectrum must be converted to a calculated absolute spectrum and then compared to the absolute reflectivity derived from theory. This comparison must be accomplished mathematically.
This new procedure required development and validation with thin film standards. Since thin lipid film standards are not available, thin SiO.sub.2 film standards, produced via vapor deposition of SiO.sub.2 onto pure flat Silicon wafer substrates were used. These standards are commercially available (VLSI Standards, Inc. San Jose, Calif. 95134-2006) and calibrated to within 0.1-0.01 nm thickness by NIST. The following SiO.sub.2 standards were employed (the 0 nm standard was a pure silicon wafer without SiO.sub.2; Table 1).
TABLE-US-00001 TABLE 1 SiO.sub.2 Actual thickness, nm 0 48.26 95.01 188.58
Absolute reflectivity of these SiO.sub.2 films were calculated, using the same procedure with the expanded Euler equation above, substituting the complex refractive indices below for n.sub.1 and n.sub.2 (n.sub.0=air=1, as before). SiO.sub.2n.sub.1=-9.3683E-11x.sup.3+2.5230E-07x.sup.2-2.3810E-04x+1.5302E- +00 Sin.sub.2=SQRT(1+((5.66474*.lamda.*.lamda.)/((.lamda.*.lamda.)-119153)- )+((5.29869*.lamda.*.lamda.)/(.lamda.*.lamda.-(51556.1)))+((-24642*.lamda.- *.lamda.)/((.lamda.*.lamda.)-(-146300000000))))(conversion of raw n.sub.2 data to the Sellmeier equation form)
The latter equation for the refractive index of pure silicon is in the form of the Sellmeier equation. This equation form is considered to provide very accurate values of the refractive index as a function of wavelength. Not all refractive index data are provided in this form, however. The resulting absolute reflectance spectra are seen in FIG. 4.
Interferometer-measured spectra for SiO.sub.2 standards, as for measured tear film lipid spectra, are expressed as relative % reflectance, since the measured reflectance from a thin film is measured relative to the measured reflectance from a reference. The y-axis of a measured spectrum corresponds to 100.times.R(.lamda.) meas. sample/R(.lamda.) meas. reference.
A number of different references can be used, although the best reference for tear film spectra is one with the same radius of curvature as the cornea (r=7.75 mm), to allow for the same reflectance geometry. In certain embodiments, a spherically-curved BK7 glass reference lens is used for this purpose. A pure flat silicon wafer can also be used as the reference for the SiO.sub.2 standards, since both surfaces are flat. The conversion procedure to convert a measured SiO.sub.2 or tear film spectrum to a calculated absolute reflectance spectrum is to first divide by 100 and then to multiply the (R(.lamda.) meas. Sample/R(.lamda.) meas. Reference).times.R(.lamda.) absolute reference. Here, R(.lamda.) absolute reference is the calculated theoretical reflectivity of the reference and the abbreviation for absolute when used throughout this disclosure will be: abs. This result can then be compared mathematically to a theoretical SiO2 or tear lipid spectrum, as illustrated in FIG. 4 for SiO.sub.2. In order to accomplish this procedure, one has to first calculate R(.lamda.) absolute reference (for pure Silicon or BK7). The equation which is used is derived from the following equations.
If incident light is unpolarized, and since R=|r|.sup.2 (since reflected intensity is proportional to the square of the modulus of the electric field amplitude and the dielectric function), then total R=(r.sub.s.sup.2+r.sub.p.sup.2)/2.
Also, from Snell's law, where sin .psi.=(n.sub.1/n.sub.2) sim .phi., cos .psi.=(1-(n.sub.1.sup.2/n.sub.2.sup.2)sin.sup.2.phi.).sup.1/2.
Then, from the theory of interface reflection between two isotropic materials (e.g. air and an isotropic solid such as Si or BK7), the indices of reflection are determined as follows: r.sub.s=(n.sub.1 cos .phi.-n.sub.2 cos .psi.)/(n.sub.1 cos .phi.+n.sub.2 cos .psi.)= (n.sub.1 cos .phi.-n.sub.2(1-(n.sub.1.sup.2/n.sub.2.sup.2)sin.sup.2.phi.).sup.1/2)- /(n.sub.1 cos .phi.+n.sub.2(1-(n.sub.1.sup.2/n.sub.2.sup.2)sin.sup.2.phi.).sup.1/2), and r.sub.p=(n.sub.2 cos .phi.-n.sub.1 cos .psi.)/(n.sub.2 cos .phi.+n.sub.1 cos .psi.)= (n.sub.2 cos .phi.-n.sub.1(1-(n.sub.1.sup.2/n.sub.2.sup.2)sin.sup.2.phi.).sup.1/2)/(n.- sub.2 cos .phi.+n.sub.1(1-(n.sub.1.sup.2/n.sub.2.sup.2)sin.sup.2.phi.).sup- .1/2)
These equations may also be written as: r.sub.s=(n.sub.1 cos .phi.-(n.sub.2.sup.2/n.sub.1.sup.2 sin.sup.2.phi.).sup.1/2)/(n.sub.1 cos .phi.+(n.sub.2.sup.2-n.sub.1.sup.2 sin.sup.2.phi.).sup.1/2), since(n.sub.2.sup.2-n.sub.1.sup.2 sin.sup.2.phi.).sup.1/2)=n.sub.2((n.sub.2.sup.2/n.sub.2.sup.2)-(n.sub.1.s- up.2/n.sub.2.sup.2)sin.sup.2.phi.).sup.1/2=n.sub.2(1-(n.sub.1.sup.2/n.sub.- 2.sup.2)sin.sup.2.phi.).sup.1/2 and r.sub.p=(n.sub.2 cos .phi.-n.sub.1(1-(n.sub.1.sup.2/n.sub.2.sup.2)sin.sup.2.phi.).sup.1/2)/(n.- sub.2 cos .phi.+n.sub.1(1-(n.sub.1.sup.2/n.sub.2.sup.2)sin.sup.2.phi.).sup- .1/2)
Then, since n.sub.1=air=1, the equations above can be combined using the relationship R abs=(r.sub.s.sup.2+r.sub.p.sup.2)/2=R(.lamda.) abs Si or R(.lamda.) abs BK7 (i.e. to obtain calculated absolute reflectance values for silicon or BK7 glass): R(.lamda.)abs Si=(((0.986659-D3*SQRT(1-(0.162799/D3)^2))/(0.986659+D3*SQRT(1-(0.162799/- D3)^2)))^2+(((SQRT(1-(0.162799/D3)^2))-D3*0.986659)/((SQRT(1-(0.162799/D3)- ^2))+D3*0.986659))^2)/2
where D3=Sellmeier refractive index for Si at each .lamda.,
and where 0.986659=cos .phi. and
0.162799=sin .phi. and where each wavelength is an exact wavelength measured by the interferometer.
R(.lamda.) abs BK7 is calculated for each wavelength using the same equation, except D3=Sellmeier refractive index for BK7 at each .lamda.. Sellmeier BK7n=SQRT(1+(1.03961212*G3*G3)/(G3*G3-0.00600069867)+(0.2317923- 44*G3*G3)/(G3*G3-0.0200179144)+(1.01046945*G3*G3)/(G3*G3-103.560653)) where G3=interferometer wavelength in microns (BK7 refractive index ref=Schott technical information document TIE-29 (2005)).
FIG. 5 shows the results of converting measured SiO.sub.2 spectra (using a 4V or 4.5V light source voltage, 20 msec single scan) to calculated absolute reflectance spectra for various silicon reference standards. The measured relative spectra are first divided by 100 and then multiplied times R(.lamda.) abs Si reference (Si abs R calculated) to obtain R(.lamda.) abs SiO.sub.2 sample spectra.
It can be seen that there are some relatively small differences between the theoretical and calculated absolute spectra. These differences can be mathematically calculated using an algorithm which compares the calculated absolute spectra to theoretical absolute spectra of various SiO.sub.2 films of varying thicknesses. In one particular embodiment, this is accomplished by creating a Statistica software program (StatSoft.RTM., Tulsa, Okla.) based upon the expanded Euler equation from above: V5=(1-48*v1*v2**2*v3)/((v1**2+v2**2)*(v2**2+v3**2)+4*v1*v2**2*v3+(- (v1**2-v2**2)*(v2**2-v3**2)*(cos(4*3.14159*v2*a*0.98666/v4))))))
where
v5=R(.lamda.) SiO.sub.2 measured sample.times.R(.lamda.) abs Si reference (Si abs R calculated)/100
and where
v1=n.sub.0 air=1,
v2=n.sub.1(.lamda.) SiO.sub.2,
v3=n.sub.2 (.lamda.) Si,
v4=measured .lamda., and
the variable a, the fitted film thickness.
As shown below, the wavelength range for SiO.sub.2 thin film standards must be limited to 575-1025 nm, to avoid signal weakness/potential optical aberration at the wavelength extremes. Thus, the program requires the input of five columns of calculated and measured data input as variables (i.e. v1-v5). The Non-linear Estimation method within the Statistica software is used, wherein the equation for v5 above is input as the function to be estimated into the space provided in the user specified regression, least squares module. The Statistica software program uses the Levenburg-Marquardt algorithm to achieve a minimum in the sum of squares of the differences between theoretical R and the product of R(.lamda.) SiO.sub.2 measured sample.times.R(.lamda.) abs Si reference (Si abs R calculated)/100 at each wavelength. In various embodiments, other mathematical algorithms for fitting data are available within Statistica and other software platforms and can also be employed. This software module requires the number of calculation/fitting iterations to be selected. In one embodiment, fifty iterations were found to be acceptable, although other lower or higher numbers of iterations are also acceptable and can be readily determined by an evaluation of the p-level of the fit. All p-levels for thin films were found to be 0.00 and are thus highly significant.
The program also requires a starting value for the variable a-term, the fitted film thickness. This is indicated in the column labeled "STAT Input" in Table 2 below for the SiO.sub.2 thin film standards. It was discovered through experiments with tear film spectra, presented below, that a starting value for the a-term that is too far from the actual thin film thickness value may converge to an incorrect result. It is believed that this may be a result of convergence to a local minimum in the least squares sum. Considerable time may be required to run the program multiple times with different starting values until the correct value is found. Moreover, the correct tear film lipid layer thickness is not known prior to calculation and thus the correct starting value is not known. Thus, selecting the proper starting value is important not only for a fast method, but also to achieve correct results. The human tear film lipid layer thickness typically ranges between 0 and 120 nm in thickness. Thus, in one particular embodiment a starting value of 65 nm has been determined to produce correct results for tear film lipid layer thickness between 0 and about 100 nm thickness as well as for SiO.sub.2 thin film standards between 0 and 95 nm. Other starting values may be employed where necessary in cases where a 65 nm starting value is incorrect, as is the case for the 188.58 nm SiO.sub.2 thin film standard, in which case a 200 nm starting value was used.
Subsequently, the validity of the method was demonstrated using a curved BK7 glass reference lens having an identical radius of curvature as the human cornea, 7.75 mm. This particular lens is used as a reference when making measurements of the human tear film in order to achieve optics as close as possible to those during the human tear film measurements.
A similar mathematical process was completed using measured SiO.sub.2 thin film standard spectra with different reference materials. FIG. 6 shows absolute reflectance spectra obtained by converting measurements of the relative reflectance spectra for the 48.26 nm SiO.sub.2 thin film standard which were measured relative to various reference materials, including a flat silicon wafer, a flat BK7 glass plate, and a curved BK7 glass lens having an identical radius of curvature as the human cornea, i.e. 7.75 mm. The absolute spectra, determined from measured relative spectra, are graphed relative to the calculated absolute spectrum for a 48.26 nm SiO.sub.2 thin film. FIG. 6 shows that when either a flat Silicon wafer or flat BK7 reference lens is used instead of the curved BK7 lens, the spectra determined from the measured relative reflectance spectra closely match the respective theoretical spectrum. However, when the curved BK7 glass lens was used as the reference, the absolute reflectance spectrum that was obtained does not overlay the theoretical spectrum and instead is shifted downward. Without being limited as to theory, this is likely because the geometry of light reflection from the flat 48.26 nm SiO.sub.2 and the flat BK7 standards is not the same as the light reflection from the curved BK7 glass lens.
Similar results were obtained with the other SiO.sub.2 thin film standards (not shown). What became evident is that a final multiplier term (b) is required. The measured spectra must be multiplied by the b-term to match the theoretical spectra. Moreover, the b-term is a variable which changes between measured spectra. The b-term is in essence a light focusing term and corrects for non-identical focusing between the reference lens measurement and the human tear film measurement. Thus, the expanded Euler equation becomes: V5=(1-((8*v1*v2**2*v3)/((v1**2+v2**2)*(v2**2+v3**2)+4*v1*v2**2*v3+((v1**2- -v2**2)*(v2**2-v3**2)*(cos(4*3.14159*v2*a*00.98666/v4))))))*b
where
v5=R(.lamda.) SiO.sub.2 measured sample.times.R(.lamda.) abs Si reference (Si abs R calculated)/100
and where
v1=n.sub.0 air=1,
v2=n.sub.1(.lamda.) SiO.sub.2,
v3=n.sub.2 (.lamda.) Si,
v4=measured .lamda., and
the variable a, the fitted film thickness, and
the variable b, the final correction term which moves the measured spectrum up or down on the theoretical R axis (y-axis) to achieve a match with theory.
In one embodiment, the software program requires the b-term to be on the right-hand side of the equation and at the end of the equation, since it requires starting input values for any variables (here a and b) to be in the same order (left to right) in which they appear in the equation program line and the variable input value program line. Since the right side of the above equation is the calculated theoretical reflectance which iteratively matches the calculated measured absolute reflectance on the left hand side, the b-term may have a value less than 1 (a b-term on the right side of 0.5 would be equivalent to a b-term on the left side of 2.0). It was determined through experiments varying the starting value of the b-term from 0 to 1.30 that the b-term value can start at a relatively wide range of values, for example between 0.40-0.80 or between 0 and 1.30, so that the program achieves the correct thickness. The center of the b-term range is about 0.66 and thus this is a good starting value.
All scan times herein for the SiO.sub.2 thin film standards are single 20 msec scans, whereas tear film spectra are typically sums of twelve 21 msec scans. The program is very fast, calculating results for a single spectrum in under a second and results for 50 spectra in 11 seconds. The results for the SiO.sub.2 thin film standards are shown in Table 2 below.
TABLE-US-00002 TABLE 2 Avg. Actual Meas. Meas. SiO2 SiO2 SiO2 Thickness, STAT Thickness, Thickness, nm Input nm nm B 0 65 a 4.42 0.66 b 1.002 48.26 65 a 47.57 48.12 0.66 b 1.026 48.26 65 a 48.37 0.66 b 0.994 48.26 65 a 48.43 0.66 b 1.035 95.01 65 a 98.54 98.56 0.66 b 1.062 95.01 65 a 98.57 0.66 b 1.062 95.01 65 a 98.55 0.66 b 1.063 188.58 200 a 190.53 190.55 0.66 b 1.033 188.58 200 a 190.55 0.66 b 1.032 188.58 200 a 190.56 0.66 b 1.030
FIG. 7 shows a standard curve comparing the actual thickness (in nm) of the SiO.sub.2 standards to the thickness determined using the methods disclosed herein. As can be seen, the values obtained using the disclosed methods closely match the actual thicknesses of the silicon dioxide standards. These are excellent results, with only a 1.8 nm error on average, maximum error of 3.6 nm and standard curve and slope=1.0014 and 1.9156 nm, respectively, demonstrating that the basic mathematics of the disclosed methods are correct. The observed absolute error results are expected to decrease with higher scan-number values for each standard and longer scan times.
Table 3 shows the results of experiments with tear film interferometry spectra and demonstrates that using a starting value for the tear film lipid layer thickness (i.e. the a-term) which is too far from the actual lipid thickness value can produce incorrect results. Lipid thickness values for these spectra were verified with the '557 method. Starting values for the b-term in all cases were 0.66. Spectrum subj18rt11 is that of a tear film during Oasys contact lens wear, indicating that the method of the present invention is suitable for measuring tear film lipid layers during contact lens wear.
TABLE-US-00003 TABLE 3 Statistica Statistica lipid thickness b-term Stat lipid starting Spectrum result, nm result thickness (a-term, nm) sub7base#49 82.17 0.2738 50, 90, 100 ok sub1#118 25.26 0.9987 65, 75 ok; 100 no: 130.79 w b = .4416 sub2AY 51.99 0.9949 40, 50, 65, 75 ok; 100 no: 102.95 w b = .6396 sub21#43 31.78 0.3701 40, 50, 65, 70 ok; 75 no: 110.86 w b = .1828 sub2CV 78.18 0.9974 50, 65, 75, 100 ok subj18rt11 7.94 0.9322 65 ok; 73, 100 no: 132.28 w b = .3757
FIG. 8 shows the results of using the methods disclosed herein to measure a thin MgF.sub.2 film on a curved BK7 lens surface. This sample serves as a surrogate for a human tear lipid film on the curved aqueous corneal surface. The results show the MgF.sub.2 film to be 111.98 nm thick. Here, the b-term started at 1 and converged to a value of 1.0473. The measured and theoretical spectra overlay one another exactly, further confirming the method herein. FIG. 8 shows a theoretical spectrum (dashed line, ----) vs. b-term fitted spectrum (light grey line, overlapping dashed line) and spectrum without the b-term fit (black line). Materials: MgF.sub.2-coated BK7 lens, Edmund Optics (Barrington N.J. 08007) part 49-886, radius of curvature=7.75 mm, used with uncoated BK7 ref lens, Edmund Optics part 49-876, radius of curvature=7.75 mm.
Given that the above results were obtained using the novel methods disclosed herein, there is potential uncertainty as to whether the MgF.sub.2 film thickness is 111.98 nm. Thus, a more rigorous method confirmation experiment was conducted using a 12.7 mm diameter, 7.75 mm radius of curvature MgF.sub.2-coated plano-convex BK7 lens (Edmunds part no. 49-855). Using the methods disclosed herein with an interferometer light source voltage of 5.5V, the MgF.sub.2 coating thickness was measured on both sides. The convex side was measured using a 7.75 mm radius of curvature uncoated BK7 lens as reference and the b-term mathematics process was employed. The plano (flat) side was measured using a flat uncoated BK7 reference lens. The thickness calculations for flat samples do not always require the use of the b-term. The b-term is useful when employing flat references when the reference surface is not placed orthogonally to the incident light from the interferometer. Otherwise, the mathematics are identical to those used for curved surfaces. FIGS. 9 and 10 present the results. In FIG. 9, Dark triangles=% R/100.times.BK7 R; Light lines=Fitted R/(b=1.0585); and Dark x=Theory R. In FIG. 10, Light triangles=% R/100.times.BK7 R; and Dark x=Theory R.
The methods herein determined MgF.sub.2 coating thicknesses to be 110.49 nm and 108.73 nm for the convex and flat sides, respectively. This is consistent with the assumption that the convex and flat surfaces were coated identically. As a further confirmation of the thickness of the MgF.sub.2 coating, a spectroscopic Ellipsometer (model alpha SE, J. A. Woollam, Lincoln, Nebr. 68508-2243) was employed to measure thickness of the coating on the flat surface. However, the convex surface coating could not be measured with the ellipsometer due to beam geometry requiring flat samples. The ellipsometer measured a coating thickness for the flat surface of 110.0.+-.0.64 nm, in excellent agreement with the interferometer result of 108.73 nm for this surface (.DELTA. thickness=1.27 nm). Since ellipsometer measurements are considered correct within thin film technology hierarchy, and both the convex and flat surfaces are assumed to have identical coating thicknesses, the b-term method for thin films on curved surfaces has been additionally verified to have an error of only about 1 nm.
Finally, the previously developed Statistica software program was applied to tear film lipid spectra, where the input data are v5=R(.lamda.) meas tear lipid sample.times.R(.lamda.) abs BK7 reference (BK7 abs R calc)/100 and where v1=n.sub.0 air=1, v2=n.sub.1(.lamda.) lipid, v3=n.sub.2 (.lamda.) aqueous, v4=measured .lamda., the variable `a` is the fitted lipid film thickness, and the variable `b` is the final correction term which moves the measured spectrum up or down on the theoretical R axis (y-axis) to achieve a match with theory (FIG. 11).
The measured spectra in FIG. 11 were plotted by dividing v5 by the fitted b-term at each wavelength. FIG. 11 shows lipid film thicknesses varying from 13.75 nm to 23.03 nm, 53.86 nm, 107.76 nm and 124.37 nm. It should be noted that the tear spectra in FIG. 11 include cosine-function oscillations from the aqueous layer (the smaller oscillations). These can be subtracted using a modified software program. Also, it is clear from the spectrum of the 188.6 nm SiO2 standard (not shown), that spectral data beyond 950-1000 nm may involve some optical error, perhaps from optical aberration. The spectrum of the 48.26 nm SiO.sub.2 standard used with the curved BK7 reference in FIG. 7 also shows some optical error above 950-1000 nm. Thus, a refined software program may delete data beyond 950 nm. Nonetheless, it is seen that the lipid spectra match the theoretical spectra very well. Note, these spectra were acquired over 504 msec, to simultaneously measure the aqueous layer. It is known that the lipid layer thickness may change over this time interval. This can cause measured spectra such as the 53.86 nm spectrum to deviate somewhat from theory. In various embodiments, spectra will be acquired in intervals as short as 20-100 msec to resolve this question. Alternatively, the shape of the 53.86 nm spectrum may arise from lipid film thickness variation within the 133 um.times.12.5 um spot. In various embodiments, the spot size will be reduced to resolve this question.
A modified Statistica software program was created, using a series of input values, where the input data are v6-v155=R(.lamda.) meas tear lipid samples and where v1=n.sub.0 air=1, v2=n.sub.1(.lamda.) lipid, v3=n.sub.2 (.lamda.) aqueous, v4=measured .lamda. and where v5=R(.lamda.) abs BK7 reference (BK7 abs R calc)/100 and where the variable a=the fitted lipid film thickness and the variable b=the final correction term which moves the measured spectrum up or down on the theoretical R axis (y-axis) to achieve a match with theory. Here the Euler equation becomes: v6-v155=(1-((8*v1*v2**2*v3)/((v1**2+v2**2)*(v2**2+v3**2)+4*v1*v2**2*v3+((- v1**2-v2**2)*(v2**2-v3**2)*(cos(4*3.14159*v2*a*0.98666/v4))))))*b/v5.
Statistica software program code follows for the first several spectrum calculations (v6 and v7). Here, the starting value for lipid thickness=65 nm=a-term starting value. The b-term starting value is set to 0.66. Measured spectra wavelength is edited to 575-950 nm:
TABLE-US-00004 S1.DeleteCases 1, 30 and S1.DeleteCases 730, 994 Option Base 1 Sub Main Dim AO As AnalysisOutput Dim AWB As Workbook Dim S1 As Spreadsheet Set S1 = ActiveDataSet S1.DeleteCases 1, 30 S1.DeleteCases 730, 994 Dim newanalysis2 As Analysis Set newanalysis2 = Analysis (scNonlinearEstimation, S1) With newanalysis2.Dialog .NonlinearMethod = scNlnUserSpecifiedRegressionLeastSquares End With newanalysis2.Run With newanalysis2.Dialog .UserFunction = "v6 = ((1- ((8*v1*v2**2*v3)/((v1**2+v2**2)*(v2**2+v3**2)+4*v1*v2**2*v3+ ((v1**2-v2**2)*(v2**2-v3**2)*(cos(4*3.14159*v2*a*0.98666/v4)))))))* b/v5" .CasewiseDeletionOfMD = True End With newanalysis2.Run With newanalysis2.Dialog .EstimationMethod = scNlnLevenbergMarquardt .MaxNumberOfIterations = 50 .ConvergenceCriterion = 6 .StartValues = "65 .66 " End With newanalysis2.Run With newanalysis2.Dialog .AlphaForLimits = 95 .PLevelForHighlighting = 0.05 End With Set AO = newanalysis2.RouteOutput(newanalysis2.Dialog.Summary) AO.Visible = True If AO.HasWorkbook Then Set AWB = AO.Workbook Else Set AWB = Nothing End If newanalysis2.GoBack With newanalysis2.Dialog .UserFunction = "v7 = ((1- ((8*v1*v2**2*v3)/((v1**2+v2**2)*(v2**2+v3**2)+4*v1*v2**2*v3+ ((v1**2-v2**2)*(v2**2-v3**2)*(cos(4*3.14159*v2*a*0.98666/v4)))))))* b/v5" .CasewiseDeletionOfMD = True End With newanalysis2.Run With newanalysis2.Dialog .EstimationMethod = scNlnLevenbergMarquardt .MaxNumberOfIterations = 50 .ConvergenceCriterion = 6 .StartValues = "65 .66 " End With newanalysis2.Run With newanalysis2.Dialog .AlphaForLimits = 95 .PLevelForHighlighting = 0.05 End With Set AO = newanalysis2.RouteOutput(newanalysis2.Dialog.Summary) AO.Visible = True If AO.HasWorkbook Then Set AWB = AO.Workbook Else Set AWB = Nothing End If
The remaining program code follows the above repeating sequence for additional spectra calculations.
A sample portion of the v1-v6 inputs for a single spectrum (columns 1-6, left to right, where v6=measured % reflectance for tear lipid spectrum #1) follows in Table 4. Note these columns extend to the last measured wavelength (1085.11 nm, not shown), and the first 30 rows (shown as input data examples here) and rows where .kappa..gtoreq.950.6843 nm are deleted by the software.
TABLE-US-00005 TABLE 4 1 1.48173057 1.33783826 559.409653 0.00042340272 36.8916 1 1.48165317 1.33782012 559.929243 0.000423370425 36.1339 1 1.48157604 1.33780203 560.448833 0.000423338215 36.167 1 1.48149916 1.33778399 560.968423 0.00042330609 36.2099 1 1.48142254 1.337766 561.488013 0.000423274049 36.5871 1 1.48134618 1.33774806 562.007604 0.000423242093 36.8416 1 1.48127008 1.33773018 562.527194 0.000423210221 36.2501 1 1.48119423 1.33771234 563.046784 0.000423178432 36.5386 1 1.48111863 1.33769455 563.566375 0.000423146727 35.974 1 1.48104329 1.33767681 564.085965 0.000423115104 35.8217 1 1.48096819 1.33765911 564.605555 0.000423083565 35.6451 1 1.48089335 1.33764147 565.125145 0.000423052107 35.7768 1 1.48081875 1.33762388 565.644736 0.000423020732 35.82 1 1.48074441 1.33760633 566.164326 0.000422989438 35.8625 1 1.48067031 1.33758883 566.683916 0.000422958225 35.8153 1 1.48059646 1.33757138 557.203506 0.000422927093 35.9704 1 1.48052285 1.33755398 557.723096 0.000422896042 35.9033 1 1.48044948 1.33753663 568.242687 0.000422865072 35.8368 1 1.48037636 1.33751932 568.762277 0.000422834181 35.5937 1 1.48030348 1.33750206 569.281867 0.00042280337 35.6052 1 1.48023084 1.33748485 569.801457 0.000422772638 35.6605 1 1.48015843 1.33746768 570.321048 0.000422741985 35.3016 1 1.48008627 1.33745056 570.840638 0.000422711411 35.7279 1 1.48001434 1.33743349 571.360228 0.000422680916 35.6287 1 1.4799428 1.3374165 571.878762 0.00042265056 35.2528 1 1.47987134 1.33739952 572.398352 0.00042262022 34.7073 1 1.47980012 1.33738259 572.917943 0.000422589957 35.3448 1 1.47972913 1.3373657 573.437533 0.000422559772 35.0115 1 1.47965838 1.33734886 573.957123 0.000422529664 35.5492 1 1.47958785 1.33733207 574.476713 0.000422499632 35.069 1 1.4795177 1.33731535 574.995248 0.000422469737 35.1151 1 1.47944763 1.33729865 575.514838 0.000422439857 34.7243
FIG. 12 illustrates the results of using the lipid thickness method herein to measure tear lipid layer thickness 150.times. over a 25.2 second period. It was found that in a few cases, a 65 nm starting value for the a-term resulted in a correct, but negative value, for the thickness. In any case, such results occur infrequently. A test of the current method with these 150 spectra produced only 5 such results (3.3%), which is considered acceptable. It is not currently known why correct values with negative signs are observed. All of the negative-sign results observed thus far have occurred with lipid layer thickness values less than 39.45 nm, which are further away from the 65 nm starting value than many spectra. In any case, positive-value results are obtained for the aforementioned negative-value spectra by using a lower starting value for the a-term. Aqueous layer thickness and blinking were measured simultaneously according to known methods. Blinks are easily visualized by the spiking in the aqueous layer thickness at the same time as the blink. This technological capability to accurately and quickly measure the tear film lipid layer has not previously been demonstrated. The results show that the lipid layer averages 61.0 nm and thickens on average about 50 nm very quickly after a blink, within on average 0.588 seconds. These results are generally consistent with Korb, et. al, (Korb, D R, et. al. Tear Film Lipid Layer Thickness as a Function of Blinking. Cornea 13 (4):354-359. 1994), who showed that individuals with a lipid layer thickness of 75-150 nm demonstrated a mean increase in lipid layer thickness of 33 nm following forceful blinking They are also consistent with Goto, et. al, (Goto, E and Tseng, C G. Differentiation of Lipid Tear Deficiency Dry Eye by Kinetic Analysis of Tear Interference Images. Arch Ophthalmol. Vol. 121, February 2003, 173-180.), who showed that for those with 75 nm lipid films, mean lipid spread time following a blink was 0.36.+-.0.22 seconds. FIG. 12 shows that contrary to one conventional theory, lipid layer thickening following a blink does not precede aqueous layer thickening. However, this is a single small test of the technology, and not a rigorous test of tear film spreading theory.
In various embodiments, the disclosed methods may be carried out on a computing system in communication with an interferometer (e.g. a wavelength-dependent interferometer). The computing system may include one or more computer systems in communication with one another through various wired and wireless communication means which may include communications through the Internet and/or a local network (LAN). Each computer system may include an input device, an output device, a storage medium (including non-transient computer-readable media), and a processor such as a microprocessor. Possible input devices include a keyboard, a computer mouse, a touch screen, and the like. Output devices include a cathode-ray tube (CRT) computer monitor, a LCD or LED computer monitor, and the like. Storage media may include various types of memory such as a hard disk, RAM, flash memory, and other magnetic, optical, physical, or electronic memory devices. The processor may be any suitable computer processor for performing calculations and directing other functions for performing input, output, calculation, and display of data in the disclosed system. Implementation of the computing system may include generating a set of instructions and data that are stored on one or more of the storage media and operated on by a controller. Thus, one or more controllers may be programmed to carry out embodiments of the disclosed invention. The data associated with the system may include image data, numerical data, or other types of data.
CONCLUSION
Novel mathematical algorithms and software methods have been independently developed to calculate absolute-reflectance of tear film lipid layers from measured tear film lipid layer reflectance using wavelength-dependent optical interferometry. The absolute reflectance measurements are used for the accurate and quick determination of lipid layer thickness. These algorithms are consistent with optical theory, with the exception of a single b-term, which may be empirically explained by light reflection from a curved surface or from non-orthogonal placement of a flat surface or from out-of-focus light reflection.
Thickness errors for the methods herein for thin films on curved surfaces in perfect focus are only a few nanometers (nm). In practice, collecting .gtoreq.50 tear lipid measurements, deleting out-of-focus spectra, and averaging the remaining spectra will keep lipid thickness errors small.
These methods are suitable for the quantitative evaluation of the effects of novel dual-function lipid-supplementation tear formulas on the tear film lipid layer. They are also useful for evaluating the effects of other eye drops, ophthalmic dry eye drugs and MPS solutions, and contact lenses on the tear film lipid layer.
Novel features of the present disclosure include the use of the expanded Euler equation with interferometer-dependent wavelength selection of wavelength-dependent Sellmaier equation-fitted complex refractive indices in the software program to calculate tear film lipid layer thickness, where v6, the measured reflectance variable R(.lamda.) in an expanded Euler equation, is known and the actual lipid thickness d becomes the fitted lipid film thickness variable "a" (e.g., variable reversal in the expanded Euler equation) and wherein the expanded Euler equation also has a variable b, which is the final correction term which mathematically adjusts measured reflectance R (moves the measured spectrum up or down on the theoretical R axis (y-axis)) to achieve a match with theory: v6=(1-((8*v1*v2**2*v3)/((v1**2+v2**2)*(v2**2+v3**2)+4*v1*v2**2*v3+((v1**2- -v2**2)*(v2**2-v3**2)*(cos(4*3.14159*v2*a*0.98666/v4))))))*b/v5
where
v1=n.sub.0 air=1,
v2=n.sub.1(.lamda.) lipid (Sellmeier-form),
v3=n.sub.2 (.lamda.) aqueous,
v4=measured .lamda., and
v5=R(.lamda.) abs BK7 reference (BK7 abs R calc)/100 and
wherein a Levenberg-Marquardt algorithm is used with a novel software program and a starting value for the a-term of 65 nm and for the b-term between 0 and 1.30 so that the program achieves the correct thickness and wherein spectral data without optical aberration between 575-950 nm are most preferred.
Other novel features include a method wherein a tear film lipid spectrum and slope is evaluated and a tear lipid layer thickness is estimated and this thickness estimate is thereafter used as the starting value for the a-term in the method above.
REFERENCES
The following references are herein incorporated by reference in their entirety: Scaffidi, R C, Korb, R. Comparison of the Efficacy of Two Lipid Emulsion Eyedrops in Increasing Tear Film Lipid Layer Thickness. Eye & Contact Lens: Science & Clinical Practice, 2007; 33(1):38-44. Goto, et al. Computer-Synthesis of an Interference Color Chart of Human Tear Lipid Layer, by a Colorimetric Approach. Invest. Ophthalmol. Vis. Sci., 2003; 44:4693-4697. Tiffany, J M. Refractive index of meibomian and other lipids. Current Eye Research, 5 (11), 1986, 887-889. Stenzel, O. The Physics of Thin Film Optical Spectra. Editors: G. Ertl, H. Luth and D. Mills. Springer-Verlag Berlin Heidelberg 2005: 71-98. Schott technical information document TIE-29 (2005). Korb, D R, et. al. Tear Film Lipid Layer Thickness as a Function of Blinking Cornea 13 (4):354-359. 1994. Goto, E and Tseng, C G. Differentiation of Lipid Tear Deficiency Dry Eye by Kinetic Analysis of Tear Interference Images. Arch Ophthalmol. Vol. 121, February 2003, 173-180.
Various features and advantages of the invention are set forth in the following claims.
* * * * *
References
D00000

D00001

D00002

D00003

D00004

D00005

D00006

D00007

D00008

D00009

D00010

XML
uspto.report is an independent third-party trademark research tool that is not affiliated, endorsed, or sponsored by the United States Patent and Trademark Office (USPTO) or any other governmental organization. The information provided by uspto.report is based on publicly available data at the time of writing and is intended for informational purposes only.
While we strive to provide accurate and up-to-date information, we do not guarantee the accuracy, completeness, reliability, or suitability of the information displayed on this site. The use of this site is at your own risk. Any reliance you place on such information is therefore strictly at your own risk.
All official trademark data, including owner information, should be verified by visiting the official USPTO website at www.uspto.gov. This site is not intended to replace professional legal advice and should not be used as a substitute for consulting with a legal professional who is knowledgeable about trademark law.