Expansion Sock
HANFT; JASON R.
U.S. patent application number 17/066437 was filed with the patent office on 2021-04-15 for expansion sock. This patent application is currently assigned to HEEL-IT, LLC. The applicant listed for this patent is Heel-lt, LLC. Invention is credited to JASON R. HANFT.
| Application Number | 20210106070 17/066437 |
| Document ID | / |
| Family ID | 1000005293297 |
| Filed Date | 2021-04-15 |






| United States Patent Application | 20210106070 |
| Kind Code | A1 |
| HANFT; JASON R. | April 15, 2021 |
EXPANSION SOCK
Abstract
An expansion sock includes one or more expansion zones formed of a different type of knitted fabric than adjacent zones. The expansion zones permit the sock to be used on a person's bandaged foot because the bandaged portions of the foot can be accommodated without either increased pressure on the bandages while minimizing excess, bunched material adjacent thereto.
| Inventors: | HANFT; JASON R.; (South Miami, FL) | ||||||||||
| Applicant: |
|
||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Assignee: | HEEL-IT, LLC South Miami FL |
||||||||||
| Family ID: | 1000005293297 | ||||||||||
| Appl. No.: | 17/066437 | ||||||||||
| Filed: | October 8, 2020 |
Related U.S. Patent Documents
| Application Number | Filing Date | Patent Number | ||
|---|---|---|---|---|
| 15821273 | Nov 22, 2017 | |||
| 17066437 | ||||
| Current U.S. Class: | 1/1 |
| Current CPC Class: | A41B 2400/34 20130101; A41B 11/003 20130101; A41B 2500/10 20130101; A41D 2500/10 20130101; A41D 2400/32 20130101; A41B 2400/60 20130101 |
| International Class: | A41B 11/00 20060101 A41B011/00 |
Claims
1. An expansion sock for use with a bandaged foot of a patient, the sock comprising: a calf portion configured and sized to expand circumferentially around a leg of the patient having the bandaged foot, the calf portion extending from a top edge proximate to the calf of the patient toward the foot of the patient and adapted to terminate in a bottom edge located above the malleoli when the sock is worn by the patient; a foot portion having a top edge extending from the bottom edge of the calf portion; wherein the foot portion, when worn by the patient, is sized and shaped to circumferentially enclose the foot of the patient; wherein the foot portion includes a heel-ankle section, a midfoot section, and a forefoot section, the heel-ankle section sized to cover at least the heel and both of the malleoli, the forefoot section having a closed end located and dimensioned to cover the metatarsal heads and the toes, and the midfoot section located and extending between the heel-ankle section and the forefoot section; wherein the sock consists essentially of knitted fabric enclosing a first volume in the calf portion and a second volume in the foot portion when the sock is in an unworn, relaxed state; wherein the calf portion, the heel-ankle section, and the midfoot section consist essentially of a first type of the knitted fabric, the first type of the knitted fabric characterized by a first force at specified elongation (FASE) at 100% selected and configured to generate a first compressive force less than 20 mmHg when any of portion, the heel-ankle section, or the midfoot section is expanded to 15% of the first volume of the relaxed state, whereby, when the sock is worn, the calf portion fits the leg and the heel-ankle section and midfoot section fit the heel-ankle and midfoot, respectively; and wherein the forefoot section consists essentially of a second type of knitted fabric to define an expansion zone, the second type of knitted fabric characterized by a second force at specified elongation (FASE) at 100% less than the first FASE, the second type of knitted fabric configured to generate a second compressive force less than 20 mmHg when the expansion zone is expanded beyond 15% of the second volume, whereby, when the sock is worn, the forefoot portion fits the bandaged foot of the patient.
2. The sock of claim 1, wherein the second type of knitted fabric is selected to generate less than 20 mmHg compressive force when the expansion zone is expanded to any volume in the range of between 50% and 200% of the relaxed state.
3. The sock of claim 1, wherein the forefoot section is adapted to extend circumferentially around the forefoot to overlie the top of the foot above the metatarsal heads, and upper and lower surfaces and sides of the toes, when worn by the patient.
4. The sock of claim 1, wherein the calf portion includes an upper calf portion located at the top edge of the calf portion, and wherein the knitted fabric of at least one of the upper calf portion, the heel-ankle portion, and the forefoot portion further comprises padded fabric.
5. The sock of claim 1, wherein the calf portion includes an upper calf portion located at the top edge of the calf portion, wherein the calf portion comprises a forward calf portion comprising padded fabric and extending longitudinally and substantially from the upper calf portion to the bottom edge of the calf portion, and wherein the forward calf portion has a transverse width and is located on the circumference of the calf portion to overlie the antibial crest when worn by the patient.
6. The sock of claim 1, wherein at least one of the first and second compressive forces generated by the first and second types of fabric, respectively, is 15 mm HG or less.
7. The sock of claim 1, wherein the knitted fabric comprises at least one material selected from the group consisting of (1) antimicrobial material; (2) machine-washable material; (3) multilayer material; (4) low-friction material; (5) heat-retaining material; (6) heat-resisting material; (7) insulating material; and (8) wicking material.
8. An expansion sock for use with a bandaged foot of a patient, the sock comprising: a calf portion configured and sized to expand circumferentially around a leg of the patient having the bandaged foot, the calf portion extending from a top edge proximate to the calf of the patient toward the foot of the patient and adapted to terminate in a bottom edge located above the malleoli when the sock is worn by the patient; a foot portion having a top edge extending from the bottom edge of the calf portion; wherein the foot portion, when worn by the patient, is sized and shaped to circumferentially enclose the foot of the patient; wherein the foot portion includes a heel-ankle section, a midfoot section, and a forefoot section, the heel-ankle section sized to cover at least the heel and both of the malleoli, the forefoot section having a closed end located and dimensioned to cover the metatarsal heads and the toes, and the midfoot section located and extending between the heel-ankle section and the forefoot section; wherein the sock consists essentially of knitted fabric enclosing a first volume in the calf portion and a second volume in the foot portion when the sock is in an unworn, relaxed state; wherein the calf portion, the heel-ankle section, and the midfoot section consist essentially of a first type of the knitted fabric, the first type of the knitted fabric characterized by a first force at specified elongation (FASE) at 100% selected and configured to generate a first compressive force less than 20 mmHg when any of the calf portion, the heel-ankle section, or the midfoot section, is expanded to 15% of the first volume of the relaxed state, whereby, when the sock is worn, the calf portion fits the leg and the heel-ankle section and midfoot section fit the heel-ankle and midfoot, respectively; wherein the forefoot section consists essentially of a second type of knitted fabric to define an expansion zone, the second type of knitted fabric characterized by a second force at specified elongation (FASE) at 100% less than the first FASE, the second type of knitted fabric configured to generate a second compressive force less than 20 mmHg when the expansion zone is expanded to any volume in the range of between 50% and 200% of the second volume of the relaxed state, whereby, when the sock is worn, the forefoot portion fits the bandaged foot of the patient; wherein the forefoot section is adapted to extend circumferentially around the forefoot to overlie the top of the foot above the metatarsal heads, and upper and lower surfaces and sides of the toes, when worn by the patient; wherein the calf portion includes an upper calf portion located at the top edge of the calf portion, and wherein the knitted fabric of at least one of the upper calf portion, the heel-ankle portion, and the forefoot portion further comprises padded fabric; wherein the calf portion comprises a forward calf portion comprising padded fabric and extending longitudinally and substantially from the upper calf portion to the bottom edge of the calf portion, and wherein the forward calf portion has a transverse width and is located on the circumference of the calf portion to overlie the antibial crest when worn by the patient; and wherein the knitted fabric of the foot portion comprises at least one material selected from the group consisting of an anti-microbial material, a low-friction material, an insulating material, and a wicking material.
9. The sock of claim 8, wherein the knitted fabric of the foot portion includes a plantar area sized and located to underlie the plantar surface of the foot and incorporating all of the sock materials.
10. The sock of claim 8, wherein at least one of the first and second compressive forces generated by the first and second types of fabric, respectively, is 15 mm HG or less.
11. The sock of claim 8, wherein the knitted fabric of the foot portion comprises the at least one anti-microbial material, the material having at least one composition selected from the group consisting of PTFE, silver, phenolic compounds, copper metals, heavy metals, QAC, ammonium compounds, hydrophilic coatings, polymers, biocides, fungicides, antiviral compounds.
12. The sock of claim 8, wherein the knitted fabric of the foot portion comprises the at least one low-friction material, the low-friction material selected from the group consisting of PTFE, nylon, TEFLON, polyesters, LYCRA, SPANDEX, silicone, rayon, wool, and bamboo.
13. The sock of claim 8, wherein the knitted fabric of the foot portion comprises the at least one insulating material, the insulating material selected from the group consisting of polyester, wools, microencapsulated phase change materials (PCMs), polyurethanes, and technical fabric.
14. The sock of claim 8, wherein the knitted fabric of the foot portion comprises the at least one wicking material, the wicking material selected from the group consisting of polyester, wools, microencapsulated phase change materials (PCMs), polyurethanes, and technical fabric.
Description
CROSS REFERENCE TO RELATED APPLICATIONS
[0001] The present application is a continuation of U.S. application Ser. No. 15/821,273 filed on Nov. 12, 2017.
FIELD
[0002] This disclosure relates to socks, and in particular, to an expansion sock for use by patients having a bandaged foot.
BACKGROUND
[0003] A person's foot may undergo any number of injuries, sprains, wounds, or other disorders and afflictions, whether caused by direct accident, or as secondary effects of other trauma, heart conditions, blood conditions, diabetes, or any number of other medical conditions (collectively referred to herein as "foot injuries"). When people with foot injuries become patients under the care of medical practitioners, there are any number of treatments which the patient's foot may undergo. Such treatments may include, without limitation, surgical procedures, such as to correct bunions, orthopedic or other foot conditions, tissue or bone repair procedures, wound or ulcer treatment, and the like, or medical procedures may involve bracing or other supportive and corrective orthoses.
[0004] Inevitably, treatment of foot injuries may involve bandaging all or portions of the foot, whether for short or extended periods of time. Treatment of foot injuries generally involves bandages beyond the mere surface application of an adhesive bandage that substantially remains within the planar contours of the foot. Bandages for foot injuries may instead involve multiple layers, often with gauze, casting material and the like, and thereby the bandaged foot assumes a profile which extends beyond the normal outer surfaces of a healthy or unbandaged foot. Feet recovering from treatments or from foot injuries may also assume an expanded profile by mere swelling alone.
[0005] Generally, during treatment or convalescence, the bandaged foot needs to be placed either in any number of immobilizing devices, such as boots, cam walkers, casts, splints, surgical shoe, and other limb orthoses, or in suitable footwear, depending on the nature of the foot injury.
[0006] The increased dimensions of the bandaged foot, as opposed to its normal profile, pose challenges to covering the foot (including the toes) with a sock, when such sock coverage is necessary or desirable.
[0007] Frequently, the patient winds up having exposed portions of the foot during convalescence or treatment, even when such foot is received in a suitable walker, brace, or other convalescent or therapeutic footwear, not to mention the challenges of such bandaged foot being placed in a regular shoe.
[0008] There are numerous drawbacks and disadvantages to having portions of the foot uncovered by a suitable sock, ranging not only from exposure to the elements, but also including potential for a re-injury of the foot, or even injured self-esteem as the exposed foot may be visible to the public. In a similar vein, enclosing the bandaged foot with a suitable sock often aids in healing and convalescence, improved self-esteem, and may keep the foot from excess cold or heat. Suitable enclosure of the bandaged foot may isolate the foot from microbes, bacteria or infectious agents, as well as adding to comfort, in that exposed portions of the foot or the bandage itself do not experience uncomfortable pressure from the brace, boot or other immobilizing device potentially associated with convalescence.
[0009] Neither traditional socks nor compression socks are suitable to accommodate the needs or address the challenges of appropriately accommodating a bandaged foot having increased dimension compared to a non-bandaged one. A traditional sock large enough to accommodate the expanded foot bandage may gather, crease, or otherwise form discontinuities adjacent the bandage, or may not fit the patient's calf. Compression socks generally constrict the foot portion more than the calf portion and thus constrict the bandaged foot area. Accordingly, it would be beneficial to address the foregoing challenges, drawbacks and disadvantages.
SUMMARY
[0010] In one possible implementation, an expansion sock for use with a bandaged foot has a calf portion which goes around the leg of the patient and extends down to join with a foot portion which is sized and shaped to enclose the foot of the patient. For purposes of this disclosure, the foot portion can be conceptually divided into a heel-ankle section, a mid-foot section, and a forefoot section. For the sock to fit the patient's calf, the calf portion is configured to have knitted material that generates a comfortable amount of compressive force, less than 20 mmHg when the calf portion is expanded stretching by about 15% in volume from its relaxed state.
[0011] Furthermore, according to this disclosure, one or more parts of the foot portion have a second type of knitted fabric which is more expandable than the fabric in the calf portion. By "more expandable" it is meant that, in one possible implementation, the fabric in the foot portion defines an expansion zone and it is able to maintain a compressive force of less than 20 mmHg, even when the expansion zone is required to stretch beyond 15% of the volume of the foot portion in the relaxed state, such as when accommodating a bandage in such foot portion.
[0012] In other implementations, the fabric of the foot portion can generate less than 20 mmHg of compressive force even when the expansion zone is expanded to a volume ranging between 50% and 200% of the volume of the relaxed state.
[0013] In various implementations, the knitted fabric which expands more easily to form the expansion zone may be located in the heel-ankle section, the mid-foot section, the forefoot section, or any combination of the foregoing. The location of the expansion zones may be adapted to anticipated uses with patients suffering from particular types of bandaged feet.
[0014] Certain foot injuries may benefit from avoiding excess friction between overlying portions of the sock material, may also benefit from having the sock material be anti-microbial, insulative, or having enhanced wicking properties to reduce foot perspiration. Accordingly, in various implementations, the expansion sock of the present disclosure may have knitted fabric which comprises materials exhibiting one or more of the foregoing properties.
[0015] In still further implementations, the expansion sock may include padded fabric at various locations to aid in convalescence, protection or comfort or combinations of any of the foregoing. For example, padding may be provided in the forefoot region to deal with metatarsal surgery, injury, support, or other medical conditions, or convalescence from associated medical procedures. Similarly, orthopedic or other medical conditions, wounds, ulcers, and the like afflicting the heel may be addressed by suitable padding, and injuries to the calf, especially to the shin area, may be addressed by padded portions located on the expansion sock to correspond to the antibial crest when worn by the patient.
[0016] These and other features of the foregoing inventions are further appreciated by reference to the following drawings, in which:
DESCRIPTION OF THE DRAWINGS
[0017] FIG. 1 is an isometric view showing one implementation of an expansion sock according to the present disclosure worn by a patient with a bandaged foot in a suitable mobilizing or therapeutic device;
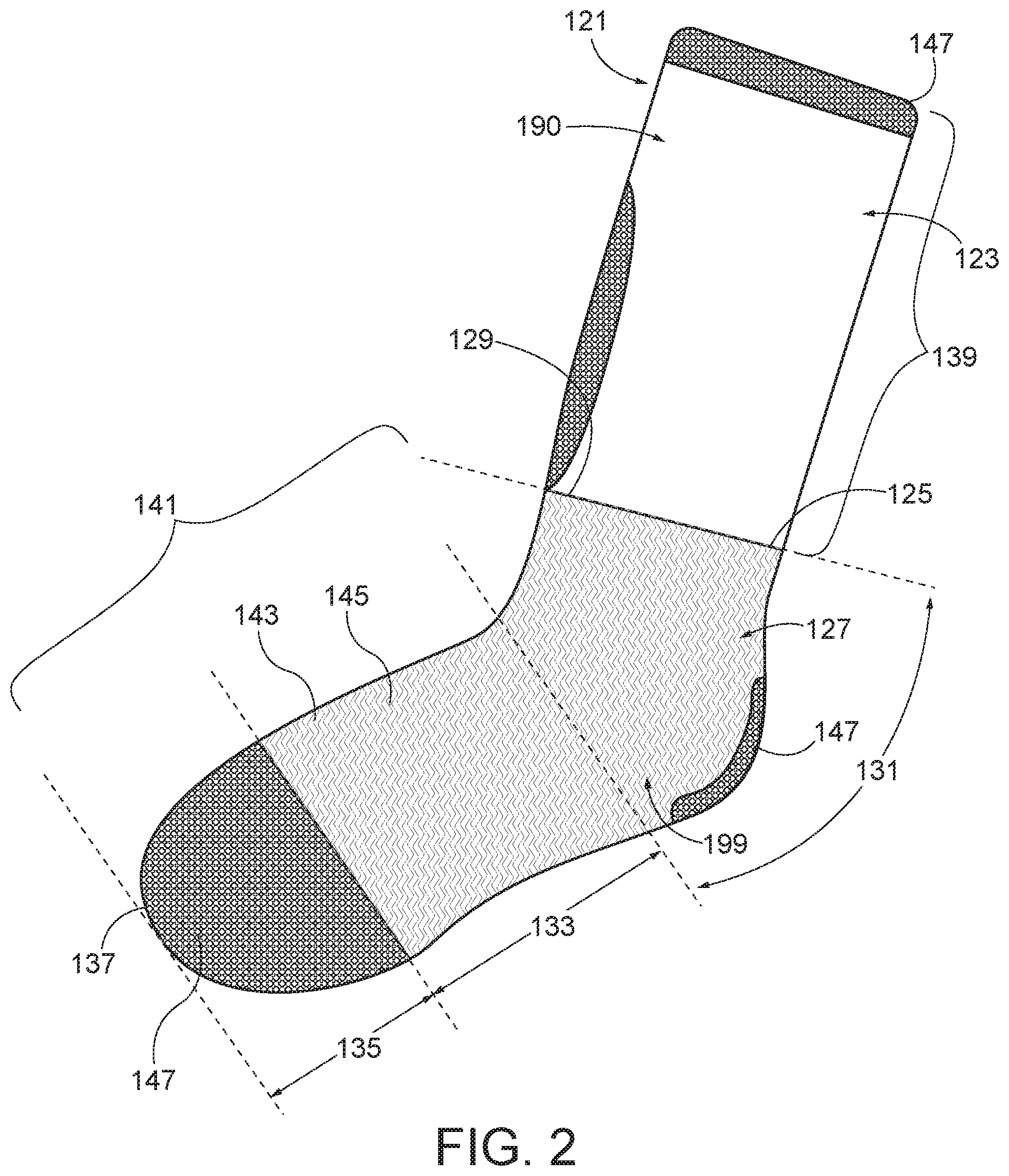
[0018] FIG. 2 is a side elevational view of another possible implementation of the present disclosure of an expansion sock;
[0019] FIGS. 3 and 4 are front- and rear-elevational views of the implementation shown in FIG. 2;
[0020] FIGS. 5 and 6 are front- and side-elevational views of another possible implementation of an expansion sock according to the present disclosure, shown when the sock is being worn by the patient over a bandaged foot.
DESCRIPTION
[0021] Certain implementations of an expansion sock according to this disclosure are shown in FIGS. 1-6 herein. Referring to FIG. 1, an expansion sock 21 is shown being worn by a patient on a bandaged foot a, including leg b. The sock may have a calf portion 23 configured and sized to expand circumferentially around a corresponding calf of a leg b of the patient having bandaged foot a. Calf portion 23 extends toward the foot a of the patient and terminates in a bottom edge 25, which bottom edge 25 is located so that, when the sock 21 is worn by the patient, the bottom edge 25 is proximate to, but above, malleoli c.
[0022] A foot portion 27 has a top edge 29 extending from bottom edge 25 and is sized and shape to circumferentially enclose bandaged foot a of the patient. As described in further detail below, foot portion 27 includes one or more expansion zones 43, which include areas of knitted fabric in which the knitted fabric is more expandable than that of calf portion 23. By "more expandable" it is meant that foot portion 27 is able to stretch where necessary to accommodate the larger profile or volume caused by a bandage which extends away from the normal outer surface of the foot, and such expansion is accomplished without significantly increasing the compressive force felt by the foot, and in a way that does not cause excessive bunching of fabric in non-expanded, adjacent areas of such foot portion 27. Accordingly, in the example illustrated in FIG. 1, the increase in profile or volume to an otherwise normal foot is in the form of a bulge caused by a bandage over the great toe d. The areas of foot portion 27 overlying the bulge have expanded to accommodate such bulge without significantly increasing compressive force on such bulge beyond that otherwise felt in normal areas of the foot, and without causing excess material or bunching of material in non-bandaged areas as well.
[0023] Referring now to FIGS. 2-4, another possible implementation of an expansion sock according to this disclosure is shown and will be described hereinafter. Expansion sock 121 includes calf portion 123 sized and configured to fit over an unbandaged calf of a patient, and foot portion 127 is configured to fit over a bandaged foot, the portions 123, 127 adjoining each other at opposing, respective bottom and top edges 125, 129.
[0024] Foot portion 127 may be conceptually divided into three sections, a heel-ankle section 131, a mid-foot section 133, and a forefoot section 135. Heel-ankle section 131 is sized to cover at least the heel and extend above the malleoli c (FIG. 1). Forefoot section 135 has a closed end 137 and is located and dimensioned to cover metatarsal heads and toes of the patient's foot, and mid-foot section 133 extends between heel-ankle and forefoot sections 131, 135.
[0025] In one possible implementation, the expansion sock consists essentially of knitted fabric, with the word "knitted" intended to encompass any number of natural, synthetic, polymeric, rubberized, elastic, or other types of fabric, whether knitted in the conventional sense of having a woven pattern, or knitted in the sense of being imprinted or formed so as to be capable of varying in dimension or orientation in response to force
[0026] Calf portion 123, in one suitable implementation, may consist essentially of a first type of the knitted fabric 190. This fabric 190 is selected so as to have the normal feel and comfort of a sock worn on the unbandaged calf of the patient. In such case, the knitted fabric 190 may be characterized by a corresponding force at specified elongation (FASE) at 100% to accomplish such normal fit. Although those skilled in the art may define compression, comfort and fit in slightly different ways, one suitable metric used in therapeutic circles is to express sock fit is in terms of compressive force measured in mmHg. Compressive forces of less than 15 or 20 mmHg have been considered as being normal comfort or non-medical compression suitable for wearing under normal circumstances over a normal unbandaged calf, as contemplated by the present disclosure. In other possible implementations, there are other alternative ways to referencing compressive force, in which it is appropriate to express normal sock fit as a percentage of expansion from its relaxed state. According to such, those skilled in the art may consider that expansion to no more than 15% of the relaxed volume is a suitable design for a knitted sock to "fit."
[0027] In terms of Force at Specified Elongation, various testing methods for yarns of may be employed in the selection of fabrics for calf and foot portions. One suitable testing method is set out in ASTM D2731-15, "Standard Test Method for Elastic Properties of Elastomeric yarns (CRE Type Tensile Testing Machines)."
[0028] While the calf portion 23, 123 and its knitted fabric 190 are configured to expand by amounts within the normal range and exert normal compression suitable to keep a sock up on a calf, foot portion 127 includes one or more portions or areas having knitted fabric 199 which defines one or more expansion zones 143 capable of expanding more readily than the knitted fabric 190 of calf portion 23, 123. Expansion zones 143 are capable of expanding to accommodate the increased bulk of a bandage on the foot, without either causing excess compressive force on the bandage and thereby causing discomfort or further injury, and also without having excess material susceptible to bunching or folding, which likewise might abrade or otherwise cause blistering or other discomforts to the foot. In the implementation illustrated in FIGS. 2-4, at least one of or more of heel-ankle section 131, mid-foot section 133, and forefoot section 135 may consist essentially of a more expandable, second type of knitted fabric and define one or more corresponding expansion zones 143 thereby. In the example illustrated in FIGS. 2-4, all three of sections 131, 133 and 135, comprising the entire foot portion 127, are formed out of the more expandable fabric, and define a single continuous expansion zone 143. Discontinuous expansion zones 143, occupying all or portions of sections 131, 133, and 135, may likewise be formed by defining areas of differing fabric expansion properties.
[0029] When the knitted fabric 199 of expansion zone or zones 143 is described herein as being different from the fabric 190 of the calf portion, or being "a second type" of fabric, it will be appreciated by those skilled in the art that such descriptions refer to the different properties of such fabric 199, as compared to fabric 190 in calf portion 123. Thus, for example, the more expandable properties of knitted fabric 199 in expansion zone(s) 143, as opposed to that in calf portion 23, 123, may arise from threads of the same material in the expansion zones as in the calf portions, but the threads of fabric 199 are thinner (have a lower denier), or have looser or different weaves, or are treated, combined with, or alternated with polymeric or other types of fibers. Fabric 199 in expansion zones 143 may likewise be considered different, or of second type, compared to that in calf portions in the sense of being formed of fibers of a different material, fiber, or of a non-woven but flexible material.
[0030] In its relaxed (unworn) state, as seen in FIGS. 2-4, the sock 121 and its knitted fabric may be thought of as enclosing a first volume 139 by means of calf portion 123, and a second volume 141 by means of knitted fabric in foot portion 127. Although any number of knitted fabrics may be suitable to provide the additional expansion contemplated herein, one suitable implementation has a foot portion 127 with an FASE at 100% which is less than the FASE at 100% of the calf portion 123, such foot portion 127 being configured to generate a compressive force less than 20 mmHg when expansion zone 143 is expanded beyond 15% of second (relaxed state) volume 141. In other implementations, the knitted fabric of expansion zone 143 may be configured so that the compressive force remains less than 20 mmHg when expansion zone 143 is expanded to any volume in the range of between 50% and 200% of the relaxed state of second volume 141 of the foot portion.
[0031] In still further implementations, only one or two sections of 131, 133 and 135 are configured with the more expandable fabric. Such implementations may be more suitable when the expansion sock 121 is contemplated for use with foot injuries located in one of those sections 131, 133 and 135, as illustrated in FIGS. 2-4. The more expandable areas of knitted fabric defining corresponding expansion zones 43, 143 may extend completely about the foot circumference of sections 131, 133, or 135; or may occupy only a patch, a portion, or other circumscribed area in the sections 131, 133, or 135, or in any area of foot portion 127 in which a bandage may need to be accommodated.
[0032] Forefoot section 135 defines an expansion zone extending circumferentially around the forefoot and thereby overlies the top of bandaged foot a (FIG. 1), as well as the upper and lower surfaces and sides of the toes, when worn by the patient. Still further variations may be contemplated in terms of the location of more expandable types of fabric relative to portions of the foot within the expansion sock 21, 121. So, for example, expandable knitted fabric 199 of foot portion 127 may include an upper area 145 sized and located to underlie the upper surface of bandaged foot a, whereas the opposite, lower, plantar section of foot portion 127 is formed of another, less expandable type of fabric, such as fabric 190.
[0033] In those embodiments where only portions of foot portion 127 comprise the more expandable, knitted fabric 199, the increased expandability may be determined or expressed in any suitable manner. For example, fabric 199 may have an FASE at 100%, 200% or other suitable tensile test percentage which is less than the comparable FASE of fabric 190 at adjacent areas of foot portion 127 made of the first type of (less expandable) fabric. The expansion zones in such embodiments may likewise be expressed as allowing expansion beyond 15%, or between 50% and 200%, or between 75% and 300%, while not increasing the compressive force beyond 50% of the compressive force of "normal fit." The expansion percentages of this disclosure, such as beyond 15%, between 50% and 200%, and between 75% and 300%, are determinable, in one possible implementation, by base reference to the surface area of the second type of knitted fabric when in its relaxed state. Alternatively, expansion of an area of the second type of knitted fabric may be measured with base reference to a sock volume corresponding to the expansion area.
[0034] Given the tubular or cylindrical nature of socks in general, expansion socks according this disclosure may have expansion zones 143 located on areas of the foot portion 127 which may not directly overlie or align with the bandaged portions of the foot, but which zones may nonetheless expand as described to allow displacement of the fabric overlying the bandage within the volume parameters described herein. For example, such implementation may have an expandable area at one longitudinal location along the length of the socks, located adjacent the plantar surface of a foot inserted therein. As such, if bandaging is located at the same longitudinal location along the length of the sock, but on the upper surface of the foot rather than the plantar surface, then the expansion zone on the plantar surface will expand in area, permitting the fabric adjacent to the upper to be displaced by the bandage, the resulting net expansion of volume or expansion zone area of such location exceeding 15% from its relaxed state, while not significantly increasing compression on such bandage.
[0035] Referring now more particularly to FIGS. 5-6, another possible implementation of the disclosure includes expansion sock 221, which makes use of the more expandable type of knitted fabric 299 in heel-ankle section 231 and forefoot section 235, to form corresponding expansion zones 243. The other portions of the sock are as described with reference to the embodiment of FIGS. 2-4 with the exception of mid-foot section 233, which is formed of less expandable knitted fabric 290 adapted to fit unbandaged portions of the patient's foot. As shown in FIGS. 5-6, the injury at the big toe has been accommodated by expansion of knitted fabric in forefoot section 235 beyond 15% of its relaxed volume and without increasing compressive force beyond 20 mmHg.
[0036] In addition to the features described above with reference to expansion sock 21, 121, and 221, any of the foregoing embodiments may include within, or in addition to, the knitted fabrics additional materials to impart additional desirable properties to the expansion sock. Thus, for example, calf portion 123 (FIGS. 2-4) may include padded material or fabric 147, and similar padded material 147 may be provided in heel-ankle section 131 and forefoot section 135.
[0037] In certain implementations, it is desirable to provide padding in the expansion sock 21, 121, and 221 corresponding to the shin when worn by the patient. To that end, calf portion 123 may include a forward calf portion 149 sized and configured to include padded material overlying the antibial crest when worn by the patient.
[0038] Certain foot disorders and conditions, such as ulcers, wounds, and other foot injuries, can be found in diabetics, and these and other patients may benefit from still further material properties being included in expansion socks in this disclosure. Thus, for example, knitted material in foot portion 127 may comprise antimicrobial material, low friction material, heat retaining material, heat resisting material, insulating material, and wicking material. Alone or in in any combination, such materials may assist in healing of the foot injury and avoiding complications of infection or other undesirable delays in recovering or convalescence. With regard to antimicrobial material, suitable properties may include active ingredients that kill or otherwise reduce the spread of bacteria, fungus, yeasts, or viruses. Examples include, but are not limited to, PTFE, silver, zinc, phenolic compounds, copper metals, heavy metals, QAC, QUAT (ammonium compounds), hydrophilic coatings, polymers, biocides, fungicides, antivirals, and any compositions, materials, or treatments that inhibit growth, attachment, or attraction of bacteria, fungus, yeasts, or viruses.
[0039] Low friction sock materials may be used in expansion sock 21 and have properties that reduce the coefficient of friction between any or all of the foot and sock 21 relative to each other; the sock 21 and the adjacent device, floor, ground or other support surface; and, ultimately, the foot relative to such support surfaces (where sock 21 is intermediate or serves as a contact layer between the two). Low-friction materials suitable for sock 21 may include PTFE, nylon, TEFLON, polyesters, LYCRA, SPANDEX, silicone, rayon, wool, bamboo, and multiple layers of these or other fabrics.
[0040] Sock materials may be used in expansion sock 21 that insulate the foot received therein from being either to hot or too cold, and/or which minimize accumulation of perspiration through wicking. Such materials include, without limitation, polyester, wools, microencapsulated phase change materials (PCMs), polyurethanes, and a variety of technical fabrics. Materials and fabrics may also provide the foregoing properties by virtue of weave density (denier), material infusion, blending, coating, spinning of one fabric over a core of another fabric, and technical fabrics with any and all of the foregoing customized to meet requirements related to insulation and wicking.
[0041] Although expansion sock 21 has been illustrated with reference to a particular immobilizing device, it would be appreciated that expansion socks according to the present disclosure may serve as a contact layer between the bandaged foot received in or retained by any number of other healing environments, such as with an overlying cast, splint, or other immobilizing devices; the expansion socks of the present disclosure may likewise be used in CAM walkers, boots, or similar limb orthopedic devices, or may be worn in therapeutic or regular footwear.
[0042] In addition to the broadly declined knitted fabrics suitable for the expansion socks of the present disclosure, still further expansion sock implementations may comprise knitted. material on either one layer, or may use multiple layers of knitted fabric of the same or differing properties, material, denier, thread-types and the like.
[0043] Having described the features of the expansion sock in the present disclosure, its advantages will be readily apparent. The bandaged foot of a patient may be enclosed with all its attendant advantages of substantially isolating it from further contaminants and undesirable elements, while minimizing the discomfort which might be associated with excessive pressure on the bandage portion of the foot, as well as the discomfort resulting from ill-fitting material at or adjacent to the bandaged portion of the foot.
[0044] Having described implementations of the expansion sock herein, it will be appreciated that this disclosure is not limited to the precise details, methodologies, materials, or geometries set forth herein, nor is this disclosure limited to the illustrated implementations or variations thereof described herein. Accordingly, still further variations and implementations are within the spirit and scope of this disclosure.
* * * * *
D00000

D00001

D00002

D00003

D00004

D00005

D00006

XML
uspto.report is an independent third-party trademark research tool that is not affiliated, endorsed, or sponsored by the United States Patent and Trademark Office (USPTO) or any other governmental organization. The information provided by uspto.report is based on publicly available data at the time of writing and is intended for informational purposes only.
While we strive to provide accurate and up-to-date information, we do not guarantee the accuracy, completeness, reliability, or suitability of the information displayed on this site. The use of this site is at your own risk. Any reliance you place on such information is therefore strictly at your own risk.
All official trademark data, including owner information, should be verified by visiting the official USPTO website at www.uspto.gov. This site is not intended to replace professional legal advice and should not be used as a substitute for consulting with a legal professional who is knowledgeable about trademark law.