Robotically-assisted Surgical Device, Robotically-assisted Surgery Method, And System
IDA; Jota ; et al.
U.S. patent application number 16/599414 was filed with the patent office on 2020-04-16 for robotically-assisted surgical device, robotically-assisted surgery method, and system. The applicant listed for this patent is Medicaroid Corporation Ziosoft, Inc.. Invention is credited to Shusuke CHINO, Jota IDA, Yutaka KARASAWA, Yukihiko KITANO, Tsuyoshi NAGATA, Shinichiro SEO.
| Application Number | 20200113637 16/599414 |
| Document ID | / |
| Family ID | 70161964 |
| Filed Date | 2020-04-16 |

View All Diagrams
| United States Patent Application | 20200113637 |
| Kind Code | A1 |
| IDA; Jota ; et al. | April 16, 2020 |
ROBOTICALLY-ASSISTED SURGICAL DEVICE, ROBOTICALLY-ASSISTED SURGERY METHOD, AND SYSTEM
Abstract
A robotically-assisted surgical device assists robotic surgery with a surgical robot that includes at least one robot arm holding a surgical instrument. The robotically-assisted surgical device includes a processing unit and a display unit. The processing unit is configured to: acquire 3D data of a subject; acquire kinematic information regard to the robot arm; acquire information of an surgical procedure for operating the subject; acquire information regarding a position of at least one port which is to be pierced on a body surface of the subject; derive a 2D range on the body surface where errors are allowed for the piercing of the port based on the 3D data, the kinematic information, the information of the surgical procedure, and the position of the port; and cause the display unit to display the information regarding the position of the port and information indicating the 2D range.
| Inventors: | IDA; Jota; (Kobe-shi, JP) ; KITANO; Yukihiko; (Kobe-shi, JP) ; CHINO; Shusuke; (Minato-ku, JP) ; NAGATA; Tsuyoshi; (Minato-ku, JP) ; KARASAWA; Yutaka; (Minato-ku, JP) ; SEO; Shinichiro; (Minato-ku, JP) | ||||||||||
| Applicant: |
|
||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Family ID: | 70161964 | ||||||||||
| Appl. No.: | 16/599414 | ||||||||||
| Filed: | October 11, 2019 |
| Current U.S. Class: | 1/1 |
| Current CPC Class: | A61B 34/70 20160201; A61B 34/30 20160201; A61B 6/032 20130101; A61B 2034/305 20160201 |
| International Class: | A61B 34/30 20060101 A61B034/30; A61B 34/00 20060101 A61B034/00; A61B 6/03 20060101 A61B006/03 |
Foreign Application Data
| Date | Code | Application Number |
|---|---|---|
| Oct 11, 2018 | JP | 2018-192931 |
Claims
1. A robotically-assisted surgical device that assists minimally invasive robotic surgery with a surgical robot that includes at least one robot arm holding a surgical instrument, the robotically-assisted surgical device comprising a processing unit and a display unit, wherein the processing unit is configured to: acquire 3D data of a subject; acquire kinematic information regard to the robot arm; acquire information of a surgical procedure for operating the subject; acquire information regarding a position of at least one port which is to be pierced on a body surface of the subject; derive a 2D range on the body surface where errors are allowed for the piercing of the port based on the 3D data, the kinematic information, the information of the surgical procedure, and the position of the port; and cause the display unit to display the information regarding the position of the port and information indicating the 2D range.
2. The robotically-assisted surgical device according to claim 1, wherein there are at least two different distances between the position of the port and respective positions on a contour of the 2D range.
3. The robotically-assisted surgical device according to claim 1, wherein the processing unit is configured to perform a pneumoperitoneum simulation on volume data of the subject to generate the 3D data of a virtual pneumoperitoneum state.
4. The robotically-assisted surgical device according to claim 3, wherein the processing unit is configured to: perform a plurality of pneumoperitoneum simulations on volume data of the subject with different amounts of pneumoperitoneum to generate the 3D data of a plurality of virtual pneumoperitoneum states; derive a plurality of 2D ranges based on the 3D data of the plurality of virtual pneumoperitoneum states; and display the information regarding the position of the port and information regarding the plurality of 2D ranges.
5. The robotically-assisted surgical device according to claim 3, wherein the processing unit is configured to: perform a plurality of pneumoperitoneum simulations on volume data of the subject with different amounts of pneumoperitoneum to generate the 3D data of a plurality of virtual pneumoperitoneum states; derive a plurality of 2D ranges based on the 3D data of the plurality of virtual pneumoperitoneum states; derive a minimum allowable range which is a range on the body surface commonly included in the plurality of 2D ranges; and display the information regarding the position of the port and information regarding the minimum allowable range.
6. The robotically-assisted surgical device according to claim 1, wherein a shape of the 2D range includes a primitive shape.
7. The robotically-assisted surgical device according to claim 1, wherein the processing unit is configured to: cause the display unit to visualize the 3D data with an annotation of the information regarding the position of the port and information regarding a position of the 2D range.
8. The robotically-assisted surgical device according to claim 1, wherein the processing unit is configured to cause a projection unit to project visible light representing the information regarding the position of the port and information regarding a position of the 2D range to the body surface.
9. A robotically-assisted surgery method of a robotically-assisted surgical device that assists robotic surgery with a surgical robot that includes a robot arm holding a surgical instrument, the robotically-assisted surgery method comprising: acquiring 3D data of a subject; acquiring kinematic information regard to the robot arm of the surgical robot; acquiring information of a surgical procedure for operating the subject; acquiring information regarding a position of a port that is to be pierced on a body surface of the subject; deriving a 2D range on the body surface of the subject where errors are allowed for the piercing of the port based on the 3D data, the kinematic information of the surgical robot, the surgical procedure, and the position of the port, and displaying the information regarding the position of the port and information indicating the 2D range.
10. The robotically-assisted surgery method according to claim 9, wherein there are at least two different distances between the position of the port and respective positions on a contour of the 2D range.
11. The robotically-assisted surgery method according to claim 9, further comprising: performing a pneumoperitoneum simulation on volume data of the subject to generate the 3D data of a virtual pneumoperitoneum state.
12. The robotically-assisted surgery method according to claim 11, further comprising: performing a plurality of pneumoperitoneum simulations on volume data of the subject with different amounts of pneumoperitoneum to generate the 3D data of a plurality of virtual pneumoperitoneum states; deriving a plurality of 2D ranges based on the 3D data of the plurality of virtual pneumoperitoneum states; and displaying the information regarding the position of the port and information regarding the plurality of 2D ranges.
13. The robotically-assisted surgery method according to claim 11, further comprising: performing a plurality of pneumoperitoneum simulations on volume data of the subject with different amounts of pneumoperitoneum to generate the 3D data of a plurality of virtual pneumoperitoneum states; deriving a plurality of 2D ranges based on the 3D data of the plurality of virtual pneumoperitoneum states; deriving a minimum allowable range which is a range on the body surface commonly included in the plurality of 2D ranges; and displaying the information regarding the position of the port and information regarding the minimum allowable range.
14. The robotically-assisted surgery method according to claim 9, wherein a shape of the 2D range includes a primitive shape.
15. The robotically-assisted surgery method according to claim 9, further comprising: causing the display unit to visualize the 3D data with an annotation of the information regarding the position of the port and information regarding a position of the 2D range.
16. The robotically-assisted surgery method according to claim 9, further comprising: causing a projection unit to project visible light representing the information regarding the position of the port and information regarding a position of the 2D range to the body surface.
17. A robotically-assisted surgery system of a robotically-assisted surgical device that assists robotic surgery with a surgical robot that includes at least one robot arm holding a surgical instrument, the robotically-assisted surgery system comprising: acquiring 3D data of a subject; acquiring kinematic information regard to the robot arm of the surgical robot; acquiring information of an surgical procedure for operating the subject; acquiring information regarding a position of a port that is to be pierced on a body surface of the subject; deriving a 2D range on the body surface of the subject where errors are allowed for the piercing of the port based on the 3D data, the kinematic information of the surgical robot, the surgical procedure, and the position of the port, and displaying the information regarding the position of the port and information indicating the 2D range.
18. The robotically-assisted surgery system according to claim 17, wherein there are at least two different distances between the position of the port and respective positions on a contour of the 2D range.
19. The robotically-assisted surgery system according to claim 17, further comprising: performing a pneumoperitoneum simulation on volume data of the subject to generate the 3D data of a virtual pneumoperitoneum state.
20. The robotically-assisted surgery system according to claim 19, further comprising: performing a plurality of pneumoperitoneum simulations on volume data of the subject with different amounts of pneumoperitoneum to generate the 3D data of a plurality of virtual pneumoperitoneum states; deriving a plurality of 2D ranges based on the 3D data of the plurality of virtual pneumoperitoneum states; and displaying the information regarding the position of the port and information regarding the plurality of 2D ranges.
Description
CROSS-REFERENCE TO RELATED APPLICATIONS
[0001] This application is based on and claims priority under 35 USC 119 from Japanese Patent Application No. 2018-192931 filed on Oct. 11, 2018, the contents of which are incorporated herein by reference.
TECHNICAL FIELD
[0002] The present disclosure relates to a robotically-assisted surgical device that assists robotic surgery with a surgical robot, a robotically-assisted surgery method, and a system.
BACKGROUND ART
[0003] In the related art, when robotic surgery is operated using a surgical robot, a port is pierced to insert forceps into the body of a patient being operated. The position of the port is approximately determined depending on a surgical procedure, but the optimal position thereof has yet to be established. US2014/0148816A discloses port placement planning. Specifically, a surgical port placement system disclosed in US2014/0148816A generates a surgical port placement model based on a plurality of parameter sets associated with a plurality of past surgical procedures, receives a given parameter set for a given surgical procedure including physical characteristics of a given patient, and plans at least one port position for the given patient for the given surgical procedure based on live given parameter set and the surgical port placement model.
SUMMARY OF INVENTION
[0004] The present disclosure provides a robotically-assisted surgical device capable of recognizing piercing accuracy required for piercing a port, a robotically-assisted surgery method, and a system.
[0005] According to one aspect of the disclosure, a robotically-assisted surgical device assists minimally invasive robotic surgery with a surgical robot that includes at least one robot arm holding a surgical instrument. The robotically-assisted surgical device includes a processing unit and a display unit. The processing unit is configured to: acquire 3D data of a subject; acquire kinematic information regard to the robot arm; acquire information of surgical procedure for operating the subject; acquire information regarding a position of at least one port which is to be pierced on a body surface of the subject; derive a 2D range on the body surface where errors are allowed for the piercing of the port based on the 3D data, the kinematic information, the information of the surgical procedure, and the position of the port; and cause the display unit to display the information regarding the position of the port and information indicating the 2D range.
[0006] According to another aspect of the disclosure, a robotically-assisted surgery method is a method of a robotically-assisted surgical device that assists robotic surgery with a surgical robot that includes a robot arm holding a surgical instrument. The robotically-assisted surgery method includes: acquiring 3D data of a subject; acquiring kinematic information regard to the robot arm of the surgical robot; acquiring information of a surgical procedure for operating the subject; acquiring information regarding a position of a port that is to be pierced on a body surface of the subject; deriving a 2D range on the body surface of the subject where errors are allowed for the piercing of the port based on the 3D data, the kinematic information of the surgical robot, the surgical procedure, and the position of the port, and displaying the information regarding the position of the port and information indicating the 2D range.
[0007] According to further another aspect of the disclosure, a robotically-assisted surgery system is a system of a robotically-assisted surgical device that assists robotic surgery with a surgical robot that includes at least one robot arm holding a surgical instrument. The robotically-assisted surgery system includes: acquiring 3D data of a subject; acquiring kinematic information regard to the robot arm of the surgical robot; acquiring information of a surgical procedure for operating the subject; acquiring information regarding a position of a port that is to be pierced on a body surface of the subject; deriving a 2D range on the body surface of the subject where errors are allowed for the piercing of the port based on the 3D data, the kinematic information of the surgical robot, the surgical procedure, and the position of the port, and displaying the information regarding the position of the port and information indicating the 2D range.
[0008] According to the present disclosure, the piercing accuracy required for piercing the port can be recognized.
BRIEF DESCRIPTION OF DRAWINGS
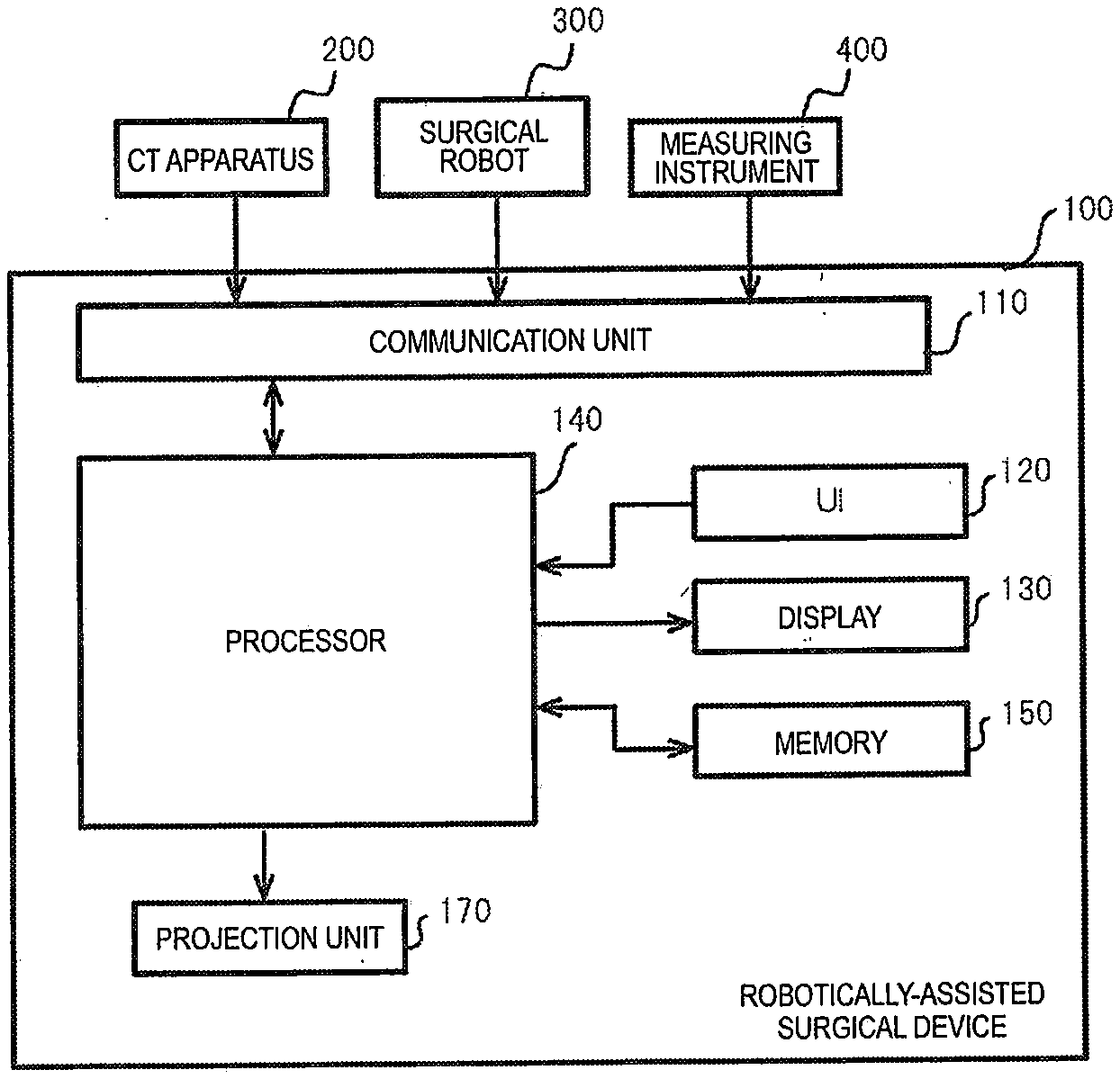
[0009] FIG. 1 is a block diagram illustrating a hardware configuration example of a robotically-assisted surgical device according to a first embodiment;
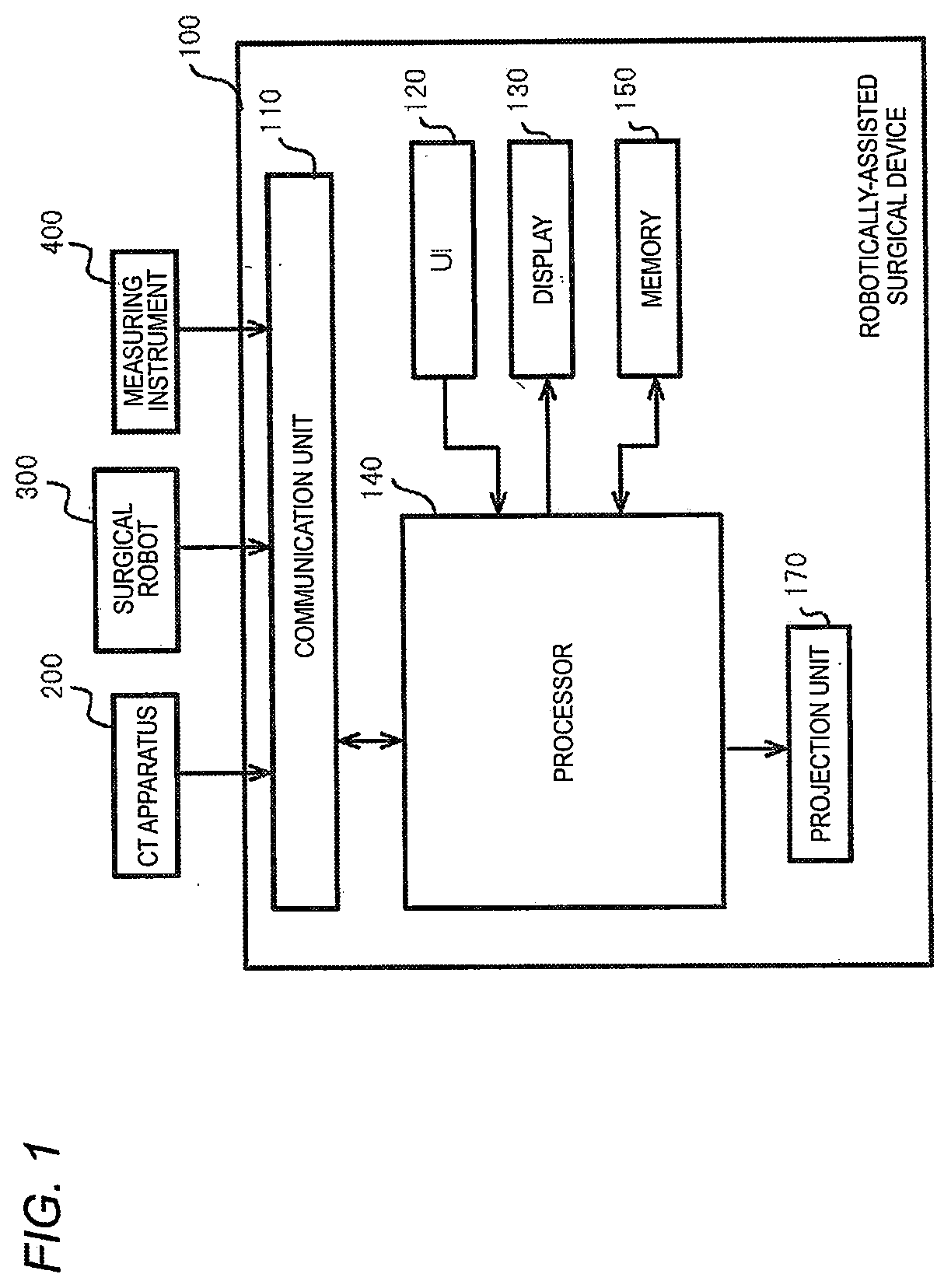
[0010] FIG. 2 is a block diagram illustrating a functional configuration example of the robotically-assisted surgical device;
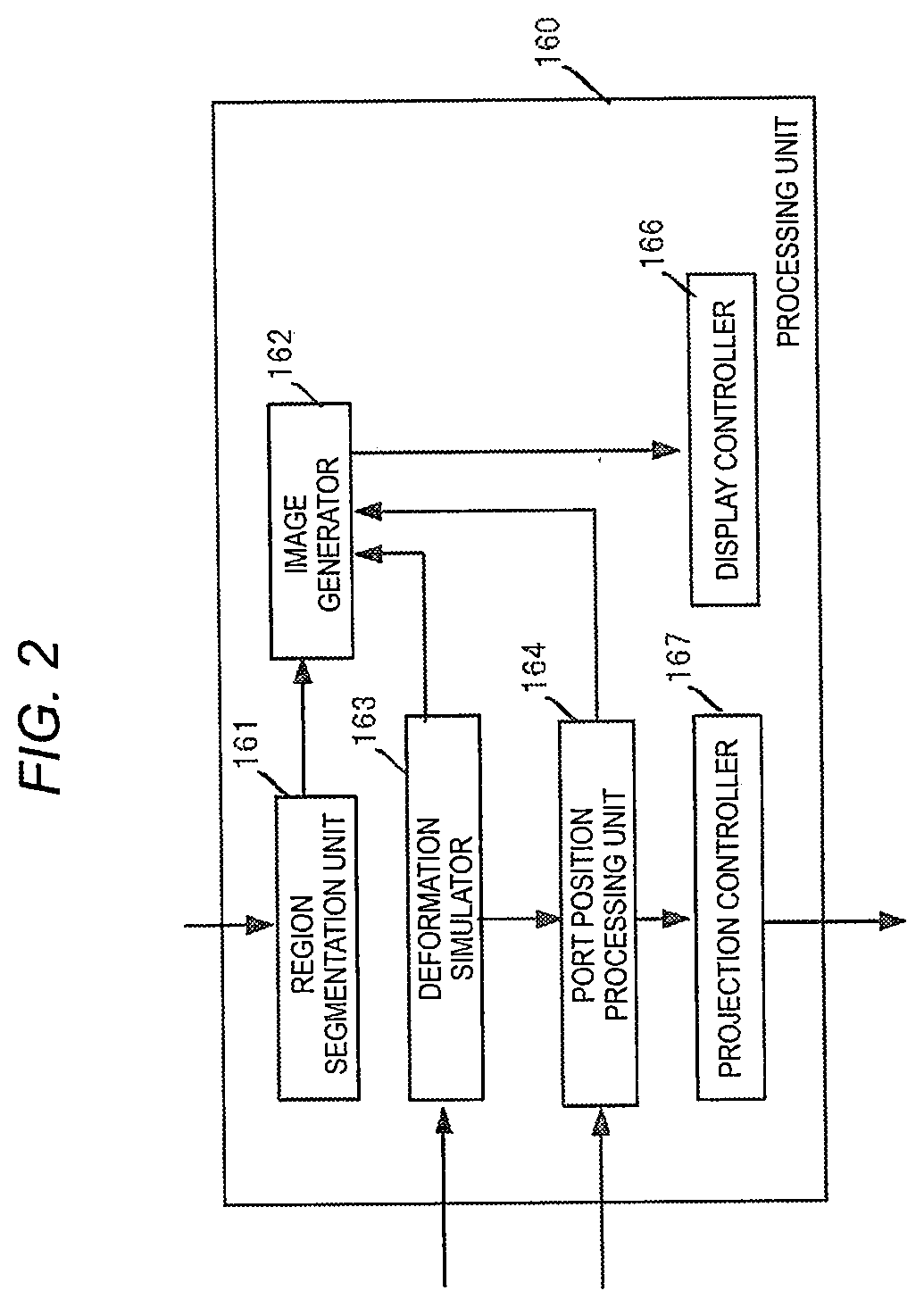
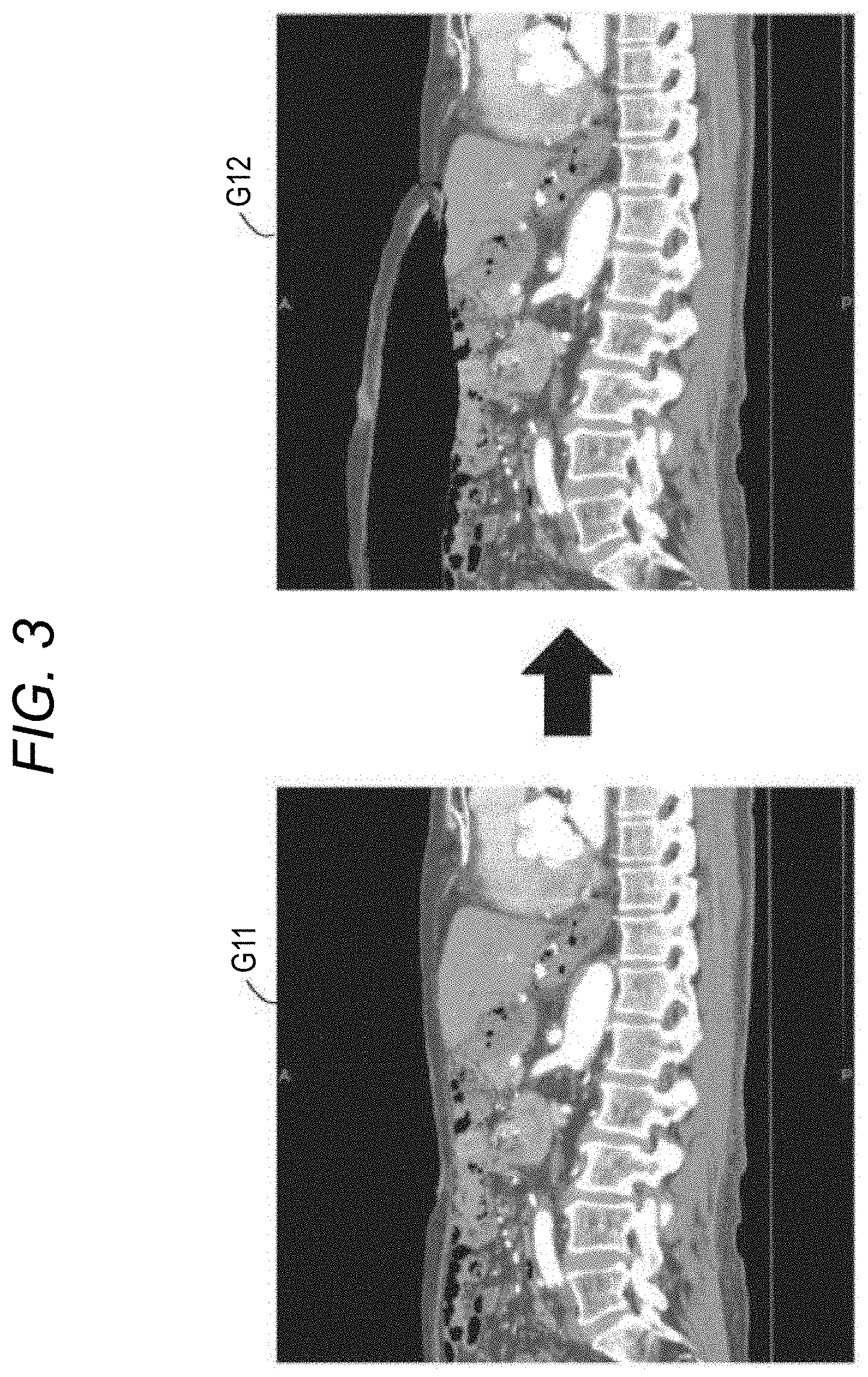
[0011] FIG. 3 is a view illustrating examples of MPR images of an abdomen before and after performing a pneumoperitoneum simulation;
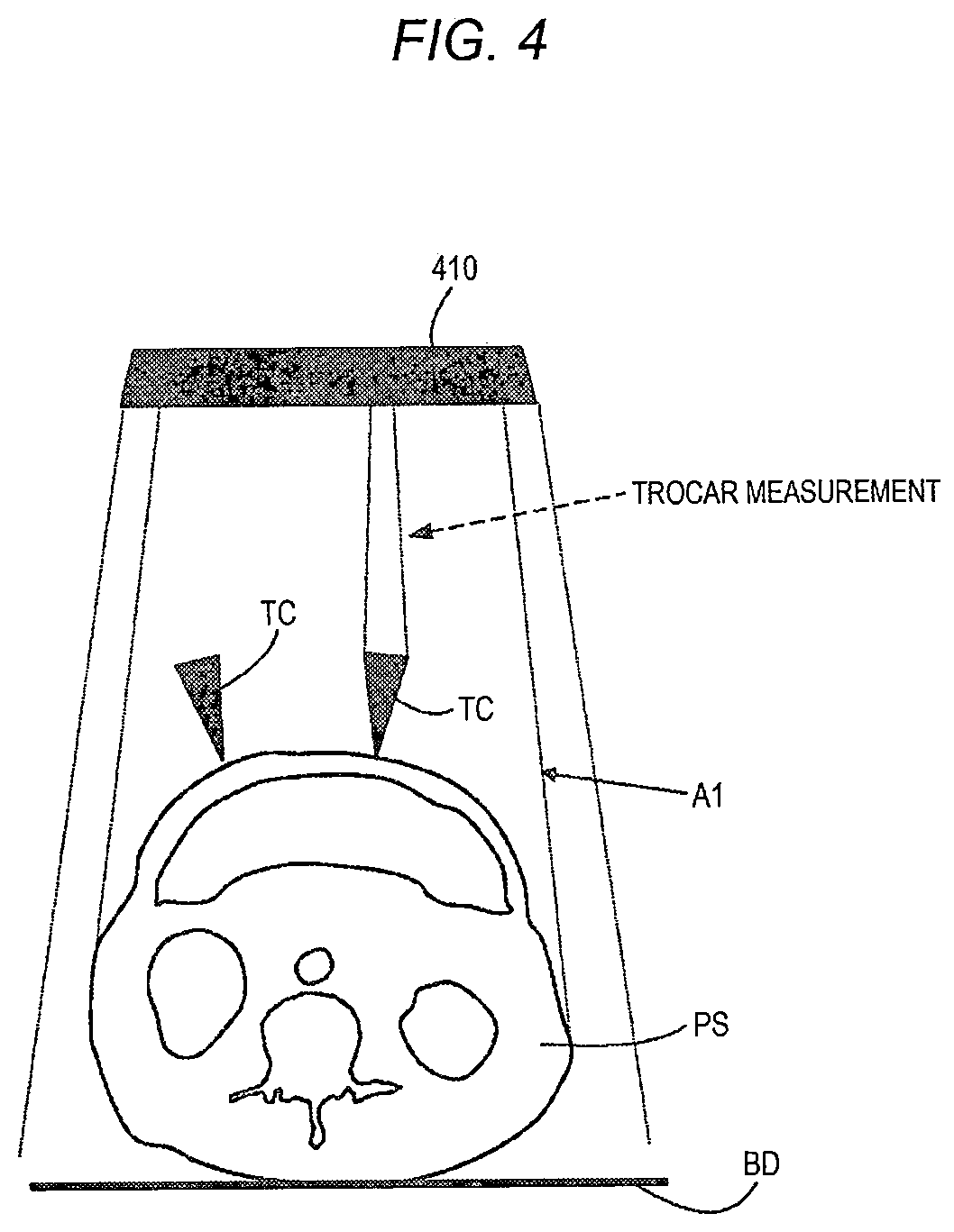
[0012] FIG. 4 is a view illustrating a measurement example of a port position of a pre-pierced port;
[0013] FIG. 5A is a view illustrating a first placement example of port positions placed on a body surface of a subject;
[0014] FIG. 5B is a view illustrating a second placement example of port positions placed on the body surface of the subject;
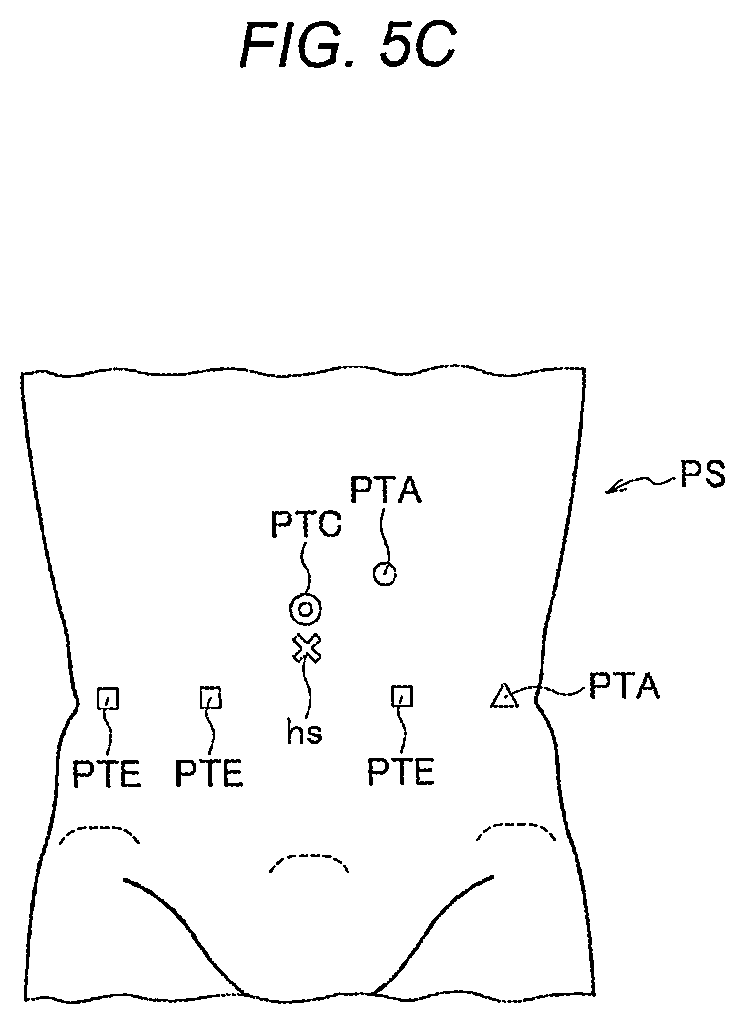
[0015] FIG. 5C is a view illustrating a third placement example of port positions placed on the body surface of the subject;
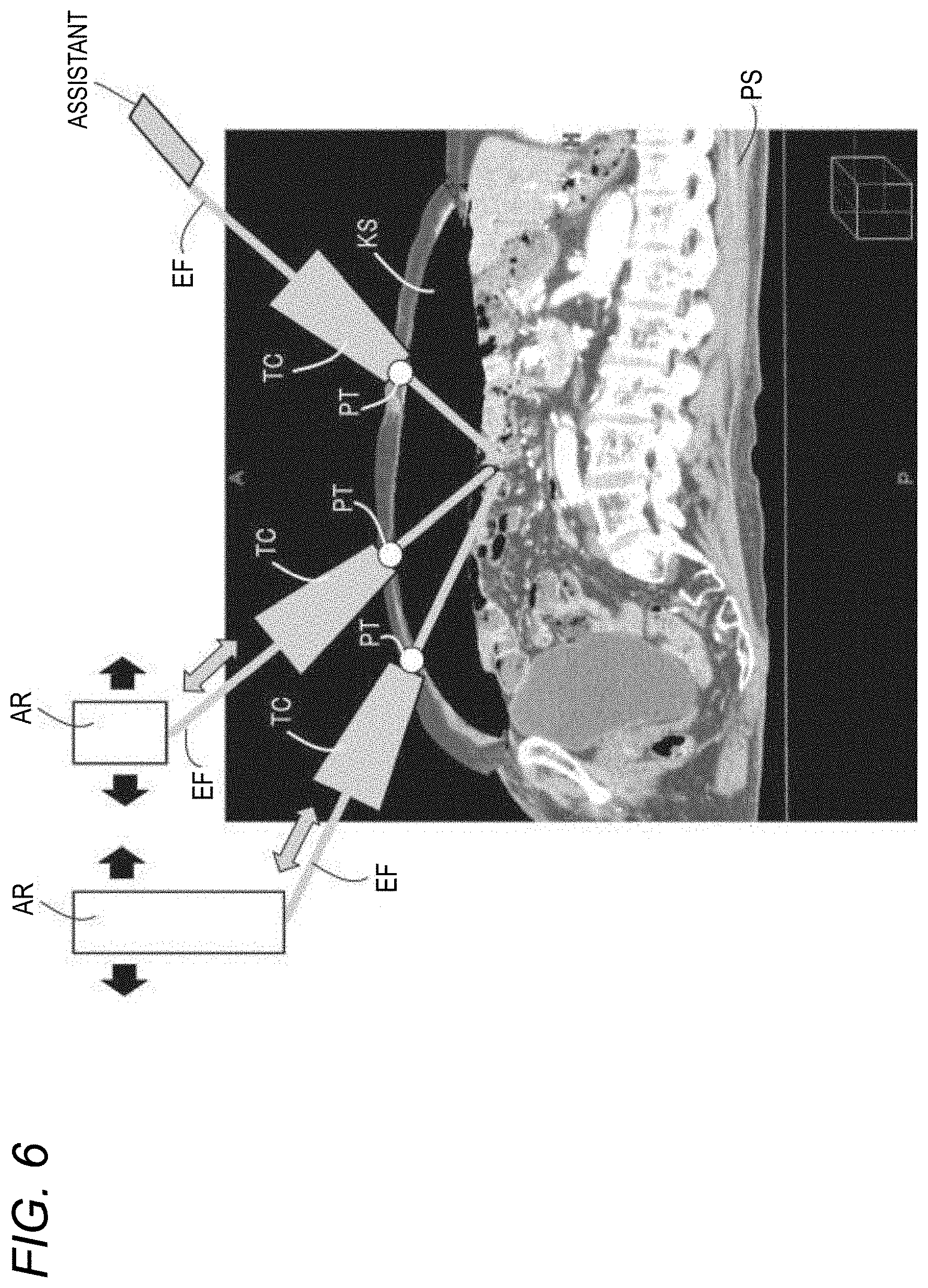
[0016] FIG. 6 is a view illustrating an example of a positional relationship between the subject, ports, trocars, and robot arms during robotic surgery;
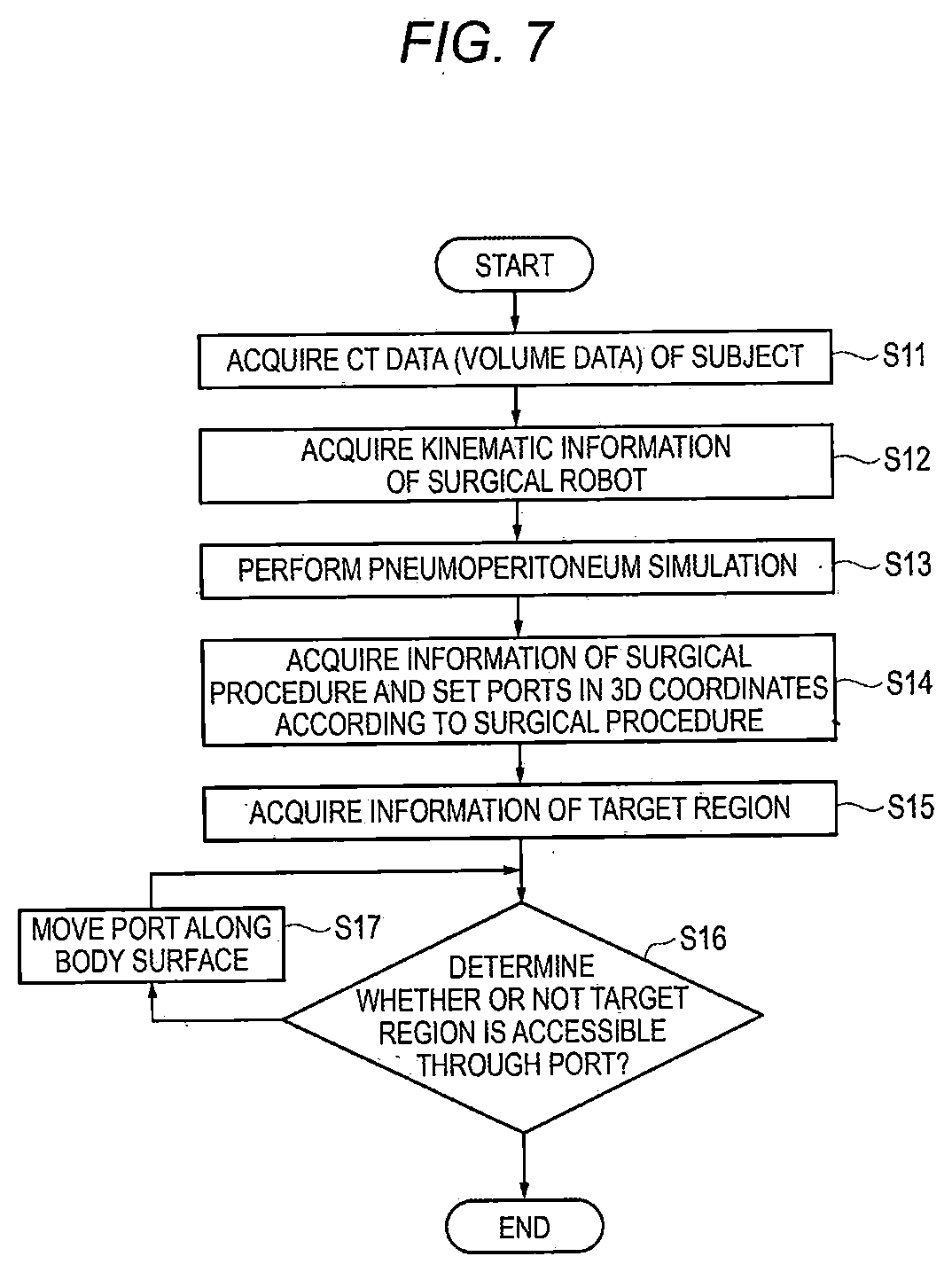
[0017] FIG. 7 is a flowchart illustrating an example of a procedure of a port position simulation by the robotically-assisted surgical device;
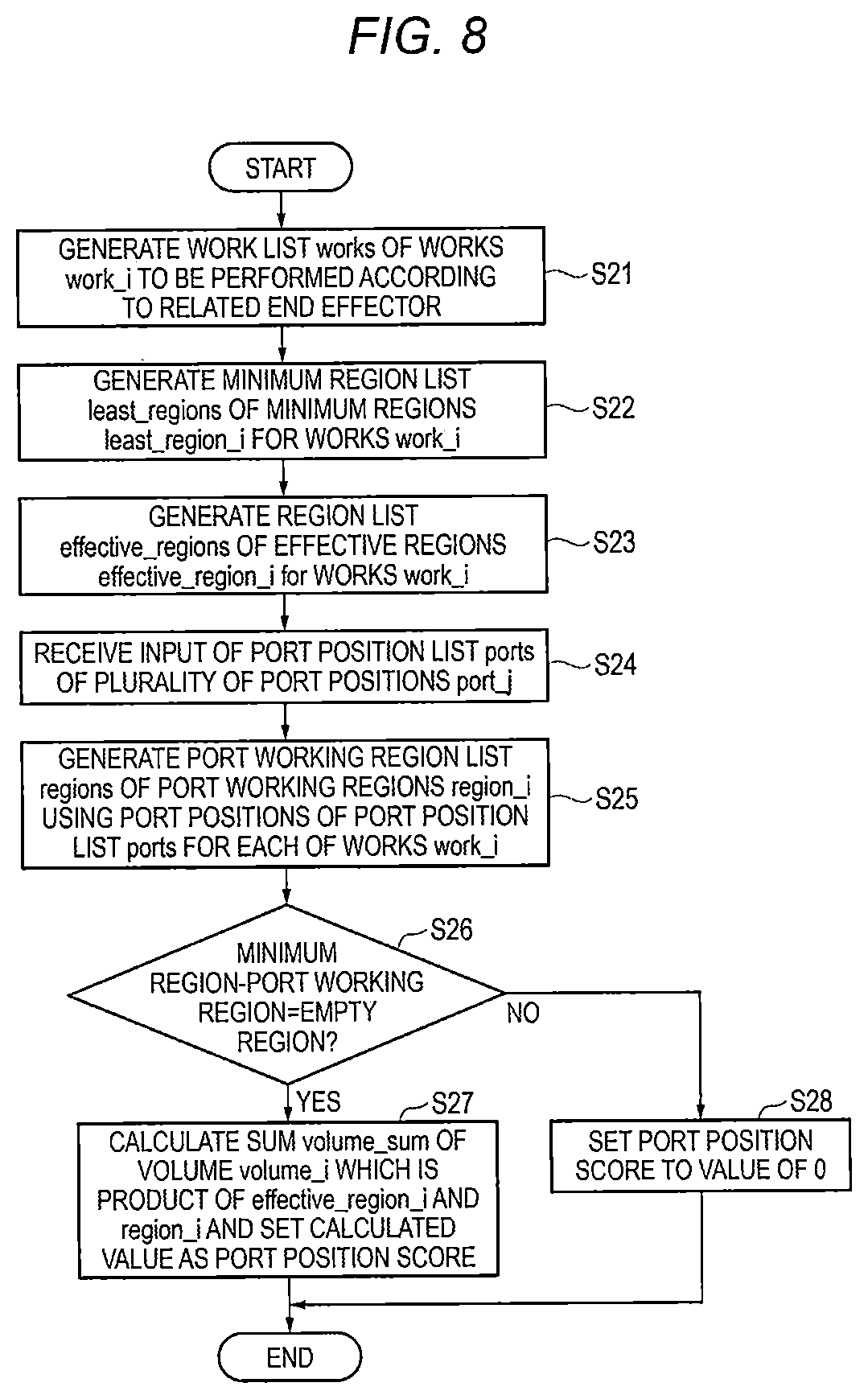
[0018] FIG. 8 is a flowchart illustrating an operation example when a port position score is calculated by the robotically-assisted surgical device;
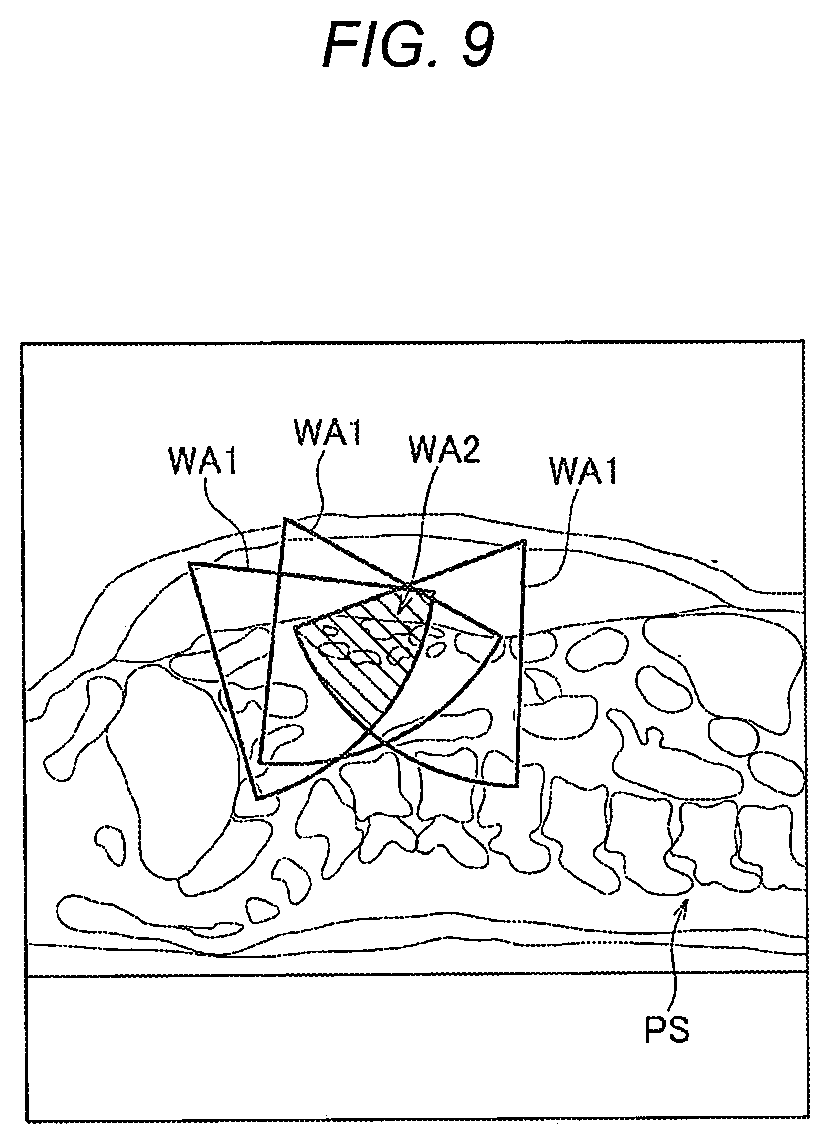
[0019] FIG. 9 is a view illustrating an example of working areas determined based on port positions;
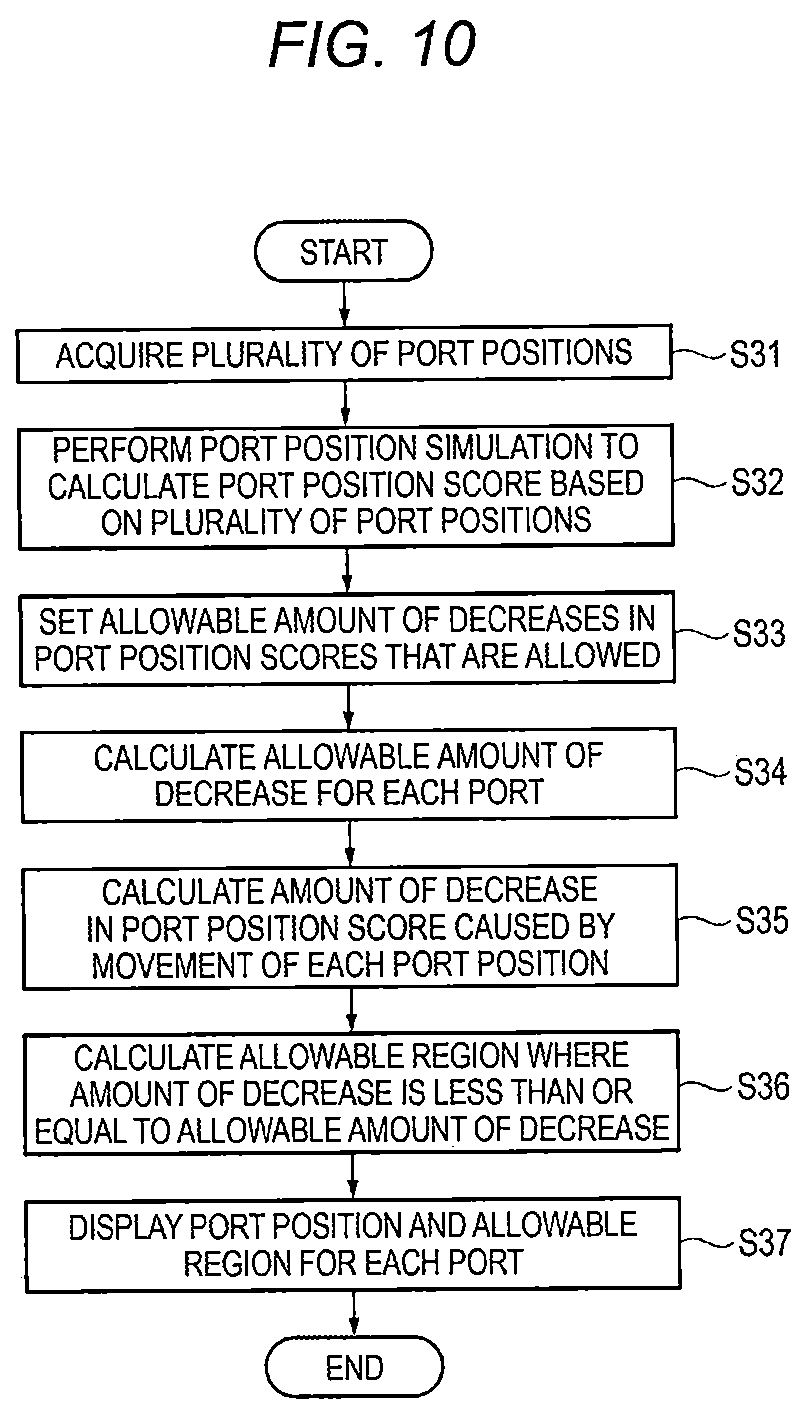
[0020] FIG. 10 is a flowchart illustrating a derivation procedure of allowable error information by the robotically-assisted surgical device;
[0021] FIG. 11 is a view illustrating a first example of an error for port positions in a thickness direction of the subject;
[0022] FIG. 12 is a view illustrating a second example of the error for port positions in the thickness direction of the subject;
[0023] FIG. 13 is a view illustrating a measurement example of a straight line distance;
[0024] FIG. 14 is a view illustrating a measurement example of a curved distance;
[0025] FIG. 15 is a view illustrating an adjustment example of the allowable error depending on the amount of pneumoperitoneum;
[0026] FIG. 16 is a view illustrating a first display example of guide information including information regarding an allowable region of a port to be pierced;
[0027] FIG. 17 is a view illustrating a second display example of guide information including information regarding an allowable region of a port to be pierced;
[0028] FIG. 18 is a view illustrating a display example of port positions according to Comparative Example:
[0029] FIG. 19 is a view illustrating a display example of port positions and allowable error information according to the embodiment; and
[0030] FIG. 20 is a view illustrating designation of a piercing position on a 2D plane and misplacement of the piercing position in a 3D space.
DESCRIPTION OF EMBODIMENTS
[0031] Hereinafter, embodiments of the present disclosure will be described using the drawings.
[0032] In the present disclosure, a robotically-assisted surgical device assists minimally invasive robotic surgery with a surgical robot that includes at least one robot arm holding a surgical instrument. The robotically-assisted surgical device includes a processing unit and a display unit. The processing unit is configured to: acquire 3D data of a subject, acquire kinematic information regard to the robot arm; acquire information of a surgical procedure for operating the subject; acquire information regarding a position of at least one port which is to be pierced on a body surface of the subject; derive a 2D range on the body surface where errors are allowed for the piercing of the port based on the acquired 3D data, the acquired kinematic information, the acquired information of the surgical procedure, and the acquired position of the port; and cause the display unit to display the information regarding the position of the port and information indicating the derived 2D range.
[0033] According to the present disclosure, the robotically-assisted surgical device displays the port position and the information indicating the 2D range, and thus, a user can recognize the degree to which the error is allowed during the piercing of the port PT. That is, the piercing accuracy required for piercing the port PT can be recognized.
[0034] (Circumstances for Achievement of Aspect of Present Disclosure)
[0035] In some cases, an assistant pierces a port according to preoperative planning. However, it is difficult to accurately pierce a port at a planned port position. For example, as illustrated in FIG. 20, when a port position to be pierced is preoperatively planned on a 2D plane, for example, a port is planned to be pierced at a position at a distance L1 from a navel, even with the same distance on the 2D plane, the position largely changes in a forward-backward direction of a subject as it moves toward a lateral part of the subject (refer to a range .alpha.). Therefore, it is difficult to accurately perform the measurement and to uniquely determine a port position to be pierced during port piercing.
[0036] In addition, in robotic surgery, pneumoperitoneum is performed in many cases. During pneumoperitoneum, carbon dioxide gas is injected into the abdominal cavity to secure a working space in the abdominal cavity. Since the degree of elevation of abdominal wall and condition in an abdominal cavity varies depending on the pneumoperitoneum state, a 3D position planned on a body surface of a patient is also variable.
[0037] In addition, in robotic surgery, arms with an end effector (forceps) that are included in a surgical robot may come into contact with each other such that a movable range of the arms is limited. In addition, during minimally invasive surgery using a surgical robot, application of stress to a port is limited. It is generally understood that, due to the above-described reasons, higher piercing accuracy during port piercing is required as compared to minimally invasive surgery by a human. As a result, it takes a long period of time for high-accuracy measurement.
[0038] In addition, various end effectors (forceps) are inserted into a subject through ports, and a work (treatment) is performed according to a surgical procedure. As the end effectors, effectors for various uses corresponding to works are present. The piercing accuracy for the ports varies depending on the contents of works or the uses of end effectors. Accordingly, like the ports, ports that require high piercing accuracy and ports that do not require high piercing accuracy may be present together. Accordingly, if a piercer (for example, an assistant) who performs piercing can recognize whether or not a port requires high piercing accuracy during piercing, the piercer can easily prepare for piercing the port.
[0039] In the following embodiment, a robotically-assisted surgical device capable of recognizing piercing accuracy required for piercing a port, a robotically-assisted surgery method, and a program will be described.
First Embodiment
[0040] FIG. 1 is a block diagram illustrating a configuration example of a robotically-assisted surgical device 100 according to a first embodiment. The robotically-assisted surgical device 100 assists robotic surgery with a surgical robot 300 and performs, for example, a preoperative simulation, an intraoperative simulation, and intraoperative navigation.
[0041] The surgical robot 300 includes a robot operation terminal, a robot main body, and an image display terminal.
[0042] The robot operation terminal includes a hand controller or a foot switch manipulated by an operator. The robot operation terminal operates a plurality of robot arms AR provided in the robot main body according to a manipulation of the hand controller or the footswitch by the operator. In addition, the robot operation terminal includes a viewer. The viewer may be a stereo viewer and may merge images input through an endoscope to display a 3D image. A plurality of robot operation terminals may be present such that a plurality of operators operate the plurality of robot operation terminals to perform robotic surgery.
[0043] The robot main body includes: a plurality of robot arms for performing robotic surgery; and an end effector EF (forceps, an instrument) as a surgical instrument that is mounted on the robot arm AR.
[0044] The robot main body of the surgical robot 300 includes four robot arms AR including: a camera arm on which an endoscope camera is mounted; a first end effector arm on which an end effector EF operated by a right-hand controller of the robot operation terminal is mounted; a second end effector arm on which an end effector EF operated by a left-hand controller of the robot operation terminal is mounted; and a third end effector arm on which an end effector EF for replacement is mounted. Each robot arm AR includes a plurality of joints and includes a motor and an encoder corresponding to each joint. Each robot arm AR has at least 6 degrees of freedom and preferably 7 or 8 degrees of freedom, operates in a 3D space, and may be movable in each direction in the 3D space. The end effector EF is an instrument that actually comes into contact with a treatment target in a subject PS during robotic surgery, and can perform various treatments (for example, gripping, dissection, exfoliation, or suture).
[0045] Examples of the end effector EF may include gripping forceps, exfoliating forceps, an electric knife, and the like. A plurality of different end effectors EF may be prepared for respective functions. For example, in robotic surgery, a treatment of dissecting a tissue with one end effector EF while holding or pulling the tissue with two end effectors EF may be performed. The robot arm AR and the end effector EF may operate based on an instruction from the robot operation terminal.
[0046] The image display terminal includes a monitor, a controller for processing an image captured by a camera of an endoscope to display the image on a viewer or a monitor, and the like. The monitor is checked by, for example, an assistant of robotic surgery or a nurse.
[0047] The surgical robot 300 receives a manipulation of the hand controller or the footswitch of the robot operation terminal by the operator, controls the operation of the robot arm AR or the end effector EF of the robot main body, and performs robotic surgery in which various treatments are performed on the subject PS. In robotic surgery, laparoscopic surgery is performed in the subject PS.
[0048] In robotic surgery, a port PT is pierced on the body surface of the subject PS, and pneumoperitoneum is performed through the port PT. In pneumoperitoneum, carbon dioxide may be injected to inflate the abdominal cavity of the subject PS. In the port PT, a trocar TC may be provided. The trocar TC includes a valve and maintains the inside of the subject PS to be airtight. In addition, in order to maintain the airtight state, air (for example, carbon dioxide) is intermittently introduced into the subject PS.
[0049] The end effector EF (shaft of the end effector EF) is inserted into the trocar TC. The valve of the trocar TC is opened during insertion of the end effector EF and is closed during the separation of the end effector EF. The end effector EF is inserted from the port PT through the trocar TC such that various treatments are performed according to the surgical procedure. Robotic surgery may be applied to not only laparoscopic surgery in which the surgery target is the abdomen but also arthroscopic surgery in which the surgery target includes a region other than the abdomen.
[0050] As illustrated in FIG. 1, the robotically-assisted surgical device 100 includes a communication unit 110, a user interface (UI) 120, a display 130, a processor 140, and a memory 150. The UI 120, the display 130, and the memory 150 may be included in the robotically-assisted surgical device 100 or may be provided separately from the robotically-assisted surgical device 100.
[0051] A CT (Computed Tomography) apparatus 200 is connected to the robotically-assisted surgical device 100 through the communication unit 110. The robotically-assisted surgical device 100 acquires volume data from the CT apparatus 200 and processes the acquired volume data. The robotically-assisted surgical device 100 may be configured by a PC (Personal Computer) and software installed on the PC. The robotically-assisted surgical device 100 may be configured as a part of the surgical robot 300.
[0052] The surgical robot 300 is connected to the robotically-assisted surgical device 100 through the communication unit 110. The robotically-assisted surgical device 100 may provide various data, information, or images from, for example, the surgical robot 300 to assist robotic surgery. The robotically-assisted surgical device 100 may acquire, from, for example, the surgical robot 300, information regarding a mechanism or the operation of the surgical robot 300 or data obtained before, during, or after robotic surgery such that various kinds of analysis or interpretation can be performed based on the acquired information or data. The analysis result or the interpretation result may be visualized.
[0053] A measuring instrument 400 is connected to the robotically-assisted surgical device 100 through the communication unit 110. The measuring instrument 400 may measure information (for example, a body surface position of the subject PS) regarding the subject PS (for example, a patient) to be operated by the surgical robot 300. The measuring instrument 400 may measure a position of the port PT provided on the body surface of the subject PS. The measuring instrument 400 may be, for example, a depth sensor 410. The depth sensor 410 may be included in the surgical robot 300 (for example, the robot main body) or may be provided in the ceiling or the like of an operating room where robotic surgery is performed. In addition, the measuring instrument 400 may receive an input of the result of manual measurement of an operation unit of the measuring instrument 400. In the manual measurement, for example, information regarding a patient or a port position on the body surface may be measured by a ruler or a tape measure.
[0054] In addition, the CT apparatus 200 is connected to the robotically-assisted surgical device 100. Alternatively, instead of the CT apparatus 200, a device capable of capturing various images may be connected to the robotically-assisted surgical device 100. This device may be, for example, an angiographic device or an ultrasound device. This device may be used to check the internal state of the subject PS before and during robotic surgery.
[0055] The CT apparatus 200 irradiates an organism with X-rays and acquires images (CT images) using a difference in X-ray absorption depending on tissues. The subject PS may be for example, a human body or an organism. The subject PS may not be a human body nor an organism. For example, the subject PS may be an animal or a phantom for surgical training.
[0056] A plurality of CT images may be acquired in a time series. The CT apparatus 200 generates volume data including information regarding any portion inside the organism. Here, any portion inside the organism may include various organs (for example, brain, heart, kidney, colon, intestine, lung, chest, lacteal gland, and prostate gland). By acquiring the CT image, it is possible to obtain a pixel value (CT value, voxel value) of each pixel (voxel) of the CT image. The CT apparatus 200 transmits the volume data as the CT image to the robotically-assisted surgical device 100 via a wired circuit or a wireless circuit.
[0057] Specifically, the CT apparatus 200 includes a gantry (not illustrated) and a console (not illustrated). The gantry includes an X-ray generator (not illustrated) and an X-ray detector (not illustrated) and acquires images at a predetermined timing instructed by the console to detect an X-ray transmitted through the subject PS and to obtain X-ray detection data. The X-ray generator includes an X-ray tube (not illustrated). The console is connected to the robotically-assisted surgical device 100. The console acquires a plurality of X-ray detection data from the gantry and generates volume data based on the X-ray detection data. The console transmits the generated volume data to the robotically-assisted surgical device 100. The console may include an operation unit (not illustrated) for inputting patient information, scanning conditions regarding CT scanning, contrast enhancement conditions regarding contrast medium administration, and other information. This operation unit may include an input device such as a keyboard or a mouse.
[0058] The CT apparatus 200 continuously captures images to acquire a plurality of 3D volume data such that a moving image can also be generated. Data of the moving image generated the plurality of 3D volume data will also be referred to as 4D (four-dimensional) data.
[0059] The CT apparatus 200 may capture CT images at each of a plurality of timings. The CT apparatus 200 may capture a CT image in a state where the subject PS is contrast-enhanced. The CT apparatus 200 may capture a CT image in a state where the subject PS is not contrast-enhanced.
[0060] In the robotically-assisted surgical device 100, the communication unit 110 performs communication of various data or information with other devices. The communication unit 110 may perform communication of various data with the CT apparatus 200, the surgical robot 300, and the measuring instrument 400. The communication unit 110 performs wired communication or wireless communication. The communication unit 110 may be connected to the CT apparatus 200, the surgical robot 300, and the measuring instrument 400 in a wired or wireless manner.
[0061] The communication unit 110 may acquire various information for robotic surgery from the surgical robot 300. The various information may include, for example, kinematic information of the surgical robot 300. The communication unit 110 may transmit various information for robotic surgery to the surgical robot 300. The various information may include, for example, information (for example, an image or data) generated by a processing unit 160.
[0062] The communication unit 110 may acquire various information for robotic surgery from the measuring instrument 400. The various information may include, for example, position information of the body surface of the subject PS or information of a port position pierced on the body surface of the subject PS that is measured by the measuring instrument 400.
[0063] The communication unit 110 may acquire volume data from the CT apparatus 200. The acquired volume data may be transmitted immediately to the processor 140 for various processes, or may be stored in the memory 150 first and then transmitted to the processor 140 for various processes as necessary. In addition, the volume data may be acquired via a recording medium.
[0064] The volume data acquired by the CT apparatus 200 may be transmitted from the CT apparatus 200 to an image data server such as (PACS: Picture Archiving and Communication Systems; not illustrated) and stored therein. Instead of acquiring from the CT apparatus 200, the communication unit 110 may acquire volume data from the image data server. This way, the communication unit 110 functions as an acquisition unit that acquires various data such as volume data.
[0065] The UI 120 may include a touch panel, a pointing device, a keyboard, or a microphone. The UI 120 receives an input operation from a user of the robotically-assisted surgical device 100. The user may include a doctor, a radiographer, or other paramedic staffs. The doctor may include an operator that manipulates a surgeon console to operate robotic surgery or an assistant that assists robotic surgery near the subject PS.
[0066] The UI 120 receives an operation such as a designation of a region of interest (ROI), a setting of luminance conditions, and the like in the volume data. The region of interest may include various tissues (such as blood vessels, bronchial tubes, organs, bones, brain, heart, feet, neck, and blood flow). The tissues may broadly include tissues of the subject PS such as diseased tissue, normal tissue, organs, and parts. In addition, the UI 120 may receive an operation such as a designation of the region of interest or a setting of luminance conditions in the volume data with respect to an image (for example, a 3D image or a 2D image described below) based on the volume data.
[0067] The display 130 may include a Liquid Crystal Display (LCD) and displays various information. The various information may include a 3D image or a 2D image obtained from the volume data. The 3D image may include, for example, a volume rendering image, a surface rendering image, a virtual endoscope image (VE image), a virtual ultrasound image, or a Curved Planar Reconstruction (CPR) image. The volume rendering image may include a RaySum image (also simply referred to as "SUM image"), a Maximum Intensity Projection (MIP) image, a Minimum Intensity Projection (MinIP) image, an average image, or a Raycast image. The 2D image may include an axial image, sagittal image, a coronal image, a Multi Planar Reconstruction (MPR) image, or the like. The 3D image and the 2D image may include a color fusion image.
[0068] The memory 150 includes a primary storage device such as various Read Only Memories (ROMs) or Random Access Memories (RAMs). The memory 150 may include a secondary storage device such as a Hard Disk Drive (HDD) or a Solid State Drive (SSD). The memory 150 may include a third storage device such as a USB memory or an SD card. The memory 150 stores various information. The various information includes information acquired via the communication unit 110, information and an image generated from the processor 140, setting information set by the processor 140, and various programs. The information acquired via the communication unit 110 may include, for example, information from the CT apparatus 200 (for example, volume data), information from the surgical robot 300, information from the measuring instrument 400, or information from an external server. The memory 150 is an example of a non-transitory recording medium in which a program is recorded.
[0069] A projection unit 170 projects visible light (for example, laser light) to the subject. The projection unit 170 projects the visible light to display various information (for example, the information of the port position) on the body surface of the subject PS (for example, the body surface of the abdomen). The visible light, that is, the information displayed on the body surface of the subject PS is recognized by the users (for example, an assistant).
[0070] The processor 140 may include a Central Processing Unit (CPU), a Digital Signal Processor (DSP), or a Graphical Processing Unit (GPU). The processor 140 executes the program stored in the memory 150 to function as the processing unit 160 controlling various processes and controls.
[0071] FIG. 2 is a block diagram illustrating a functional configuration example of the processing unit 160.
[0072] The processing unit 160 includes a region segmentation unit 161, an image generator 162, a deformation simulator 163, a port position processing unit 164, a display controller 166, and a projection controller 167.
[0073] The processing unit 160 integrates the respective units of the robotically-assisted surgical device 100. The respective sections included in the processing unit 160 may be implemented as different functions by one piece of hardware or may be implemented as different functions by a plurality of pieces of hardware. In addition, the respective sections included in the processing unit 160 may be implemented by a dedicated hardware component.
[0074] The region segmentation unit 161 may perform segmentation processing in the volume data. In this case, the UI 120 receives an instruction from a user and transmits information of the instruction to the region segmentation unit 161. The region segmentation unit 161 may perform segmentation processing from the volume data based on the information of the instruction using a well-known method to segment the region of interest. In addition, the region of interest may be set manually in accordance with the specific instruction from the user. In addition, when an observation target is predetermined, the region segmentation unit 161 may perform segmentation processing from the volume data to segment the region of interest including the observation target without the user instruction. The segmented region may include regions of various tissues (for example, blood vessels, bronchial tubes, organs, bones, brain, heart, feet, neck, blood flow, lacteal gland, chest, and tumor). The observation target may be a target to be treated by robotic surgery.
[0075] The image generator 162 may generate a 3D image or a 2D image based on the volume data acquired from the communication unit 110. The image generator 162 may generate a 3D image or a 2D image from the volume data acquired from the communication unit 110 based on a designated region or the region segmented by the region segmentation unit 161.
[0076] The deformation simulator 163 may perform a process relating to deformation in the subject PS as a surgery target. For example, the deformation simulator 163 may perform a pneumoperitoneum simulation of virtually performing pneumoperitoneum on the subject PS. A specific method of the pneumoperitoneum simulation may be a well-known method, for example, a method described in Takayuki Kitasaka, Kensaku Mori, Yuichiro Hayashi, Yasuhito Suenaga, Makoto Hashizume, and Junichiro Toriwaki, "Virtual Pneumoperitoneum for Generating Virtual Laparoscopic Views Based on Volumetric Deformation", MICCAI (Medical Image Computing and Computer-Assisted Intervention), 2004, P559-P567 which is incorporated herein by reference. That is, the deformation simulator 163 may perform the pneumoperitoneum simulation based on the volume data (volume data before pneumoperitoneum (non-pneumoperitoneum state)) acquired from the communication unit 110 or the region segmentation unit 161 to generate volume data after pneumoperitoneum (volume data in the pneumoperitoneum state). Through the pneumoperitoneum simulation, the user can simulate a state where pneumoperitoneum is performed on the subject PS without actually performing pneumoperitoneum on the subject PS to observe a state where pneumoperitoneum is virtually performed. Among pneumoperitoneum states, a state of pneumoperitoneum estimated by the pneumoperitoneum simulation will be referred to as "a virtual pneumoperitoneum state", and a state where pneumoperitoneum is actually performed will also be referred to as "an actual pneumoperitoneum state".
[0077] FIG. 3 is a view illustrating examples of MPR images of the abdomen before and after performing the pneumoperitoneum simulation. An image G11 illustrate the state before performing the pneumoperitoneum simulation, which is a state (non-pneumoperitoneum state) where the abdomen of the subject PS is not inflated. An image G12 illustrate the state after performing the pneumoperitoneum simulation, which is a state (virtual pneumoperitoneum state) where the abdomen of the subject PS is inflated and includes a pneumoperitoneum space KS. In robotic surgery, the subject PS is operated in the pneumoperitoneum state. Therefore, the pneumoperitoneum simulation is performed on the volume data acquired in the non-pneumoperitoneum state by the deformation simulator 163 and the volume data in the virtual pneumoperitoneum state is derived.
[0078] The deformation simulator 163 may virtually deform the observation target such as an organ or a disease in the subject PS. The observation target may be a surgery target to be operated by the operator. The deformation simulator 163 may simulate a state where an organ is pulled, pressed, or dissected by forceps of the end effector EF. In addition, the deformation simulator 163 may simulate, for example, movement of an organ by a postural change.
[0079] The port position processing unit 164 acquires information of a plurality of ports PT provided on the body surface of the subject PS. The information of the port PT may include, for example, identification information of the port PT, information regarding a position (port position) on the body surface of the subject PS where the port PT is pierced, information regarding the size of the port PT, or the like. The information of a plurality of ports may be stored in the memory 150 or the external server as a template. The information of the plurality of ports may be determined according to the surgical procedure. The information of the plurality of ports may be used for preoperative planning.
[0080] The port position processing unit 164 may acquire the information of the plurality of ports positions from the memory 150. The port position processing unit 164 may acquire the information of the plurality of port positions from the external server via the communication unit 110. The port position processing unit 164 may receive a designation of port positions of the plurality of ports PT via the UI 120 to acquire the information of the plurality of port positions. The information of the plurality of ports may be the information of a combination of the plurality of port positions.
[0081] The port position processing unit 164 acquires kinematic information of the surgical robot 300. The kinematic information may be stored in the memory 150. The port position processing unit 164 may acquire the kinematic information from the memory 150. The port position processing unit 164 may acquire the kinematic information from the surgical robot 300 or the external server via the communication unit 110. The kinematic information may vary depending on the surgical robot 300.
[0082] The kinematic information may include, for example, shape information regarding the shape of an instrument (for example, the robot arm AR or the end effector EF) for robotic surgery included in the surgical robot 300 or operation information regarding the operation thereof. This shape information may include information of at least a part, for example, the length or weight of each portion of the robot arm AR or the end effector EF, the angle of the robot arm AR with respect to a reference direction (for example, a horizontal plane), or the inclination angle of the end effector EF with respect to the robot arm AR. This operation information may include information of at least a part, for example, the movable range of the robot arm AR or the end effector EF in the 3D space, the position, velocity, or acceleration of the arm during the operation of the robot arm AR, or the position, velocity, or acceleration of the end effector EF relative to the robot arm AR during the operation of the end effector EF.
[0083] In kinematics, not only the movable range of one arm but also the movable range of another arm are considered and regulated such that the robot arms AR do not interfere with each other. Accordingly, the surgical robot 300 operates based on the kinematics of each robot arm AR of the surgical robot 300, and therefore, interference between the plurality of robot arms AR during operation can be avoided.
[0084] The port position processing unit 164 acquires information of the surgical procedure. The surgical procedure refers to the procedure of surgery on the subject PS. The surgical procedure may be designated via the UI 120. Each treatment in robotic surgery may be determined depending on the surgical procedure. Depending on the treatment, the end effector EF required for the treatment may be determined. Accordingly, the end effector EF mounted on the robot arm AR may be determined depending on the surgical procedure, and the type of the end effector EF mounted on the robot arm AR may be determined depending on the surgical procedure. In addition, a minimum region that is required for the treatment or a recommended region that is recommended to be secured for the treatment may be determined depending on the treatment.
[0085] The port position processing unit 164 acquires information of a target region. The target region may be a region including targets (for example, tissues (such as blood vessels, bronchial tubes, organs, bones, brain, heart, feet, and neck) to be treated by robotic surgery. The tissues may broadly include tissues of the subject PS such as diseased tissues, normal tissues, organs, and parts.
[0086] The port position processing unit 164 may acquire information regarding the position of the target region from the memory 150. The port position processing unit 164 may acquire the information of the position of the target region from the external server via the communication unit 110. The port position processing unit 164 may receive a designation of the position of the target region via the UI 120 to acquire the information regarding the position of the target region.
[0087] The port position processing unit 164 may execute a port position simulation. The port position simulation may be a simulation in which the user operates the UI 120 to determine whether or not desired robotic surgery can be performed on the subject PS. In the port position simulation, while simulating surgery, the user may operate the end effector EF inserted into each of the port positions in a virtual space to determine whether or not the target region as a surgery target is accessible. That is, in the port position simulation, while receiving the manual operation of the surgical robot 300, the user may determine whether or not a moving part (for example, the robot arm AR and the end effector EF) of the surgical robot 300 relating to robotic surgery is accessible to the target region as a surgery target without a problem. The port position processing unit 164 may obtain port position planning information through the port position simulation.
[0088] In the port position simulation, whether or not the target region is accessible may be determined based on the volume data of the subject PS, the acquired combination of the plurality of port positions, the kinematics of the surgical robot 300, the surgical procedure, the volume data of the virtual pneumoperitoneum state, and the like. While changing the plurality of port positions on the body surface of the subject PS, the port position processing unit 164 may determine whether or not the target region is accessible at each port position or may sequentially perform the port position simulation. The port position processing unit 164 may designate information regarding a finally preferable (for example, optimal) combination of port positions according to the user input via the UI 120. As a result, the port position processing unit 164 may plan the plurality of port positions to be pierced. The details of the port position simulation will be described below.
[0089] Using the plurality of port positions provided on the body surface of the subject PS, the port position processing unit 164 may derive (for example, calculate) a port position score representing the appropriateness for robotic surgery. That is, the port position score based on the combination of the plurality of port positions indicates the value of the combination of the plurality of port positions for robotic surgery. The port position score may be calculated based on the combination of the plurality of port positions, the kinematics of the surgical robot 300, the surgical procedure, the volume data of the virtual pneumoperitoneum state, and the like. The port position score is derived for each port position. The details of the port position score will be described below.
[0090] The port position processing unit 164 may adjust the port position based on the port position score. In this case, the port position processing unit 164 may adjust the port position based on the variation of the port position score according to the movement of the port position. The details of the port position adjustment will be described below.
[0091] As described above, the port position processing unit 164 may derive the plurality of port positions to be pierced according to the port position simulation. In addition, the port position processing unit 164 may derive the plurality of port positions to be pierced based on the port position score.
[0092] The display controller 166 causes the display 130 to display various data, information, or images. The display controller 166 may display the 3D image or the 2D image generated by the image generator 162. The display controller 166 may display an image showing the information of the plurality of ports PT (for example, the information of the port positions) generated by the image generator 162.
[0093] The display controller 166 may display an image which is generated by the image generator 162 and indicates information (allowable error information) indicating the error that is allowed for each port when piercing each port PT. In this case, the display controller 166 may display the allowable error information to superimpose the 3D image or the 2D image.
[0094] The projection controller 167 controls the projection of the visible light from the projection unit 170. The projection controller 167 may control, for example, a frequency or an intensity of the visible light, a position to which the visible light is projected, or a timing at which the visible light is projected.
[0095] The projection controller 167 causes the projection unit 170 to project the visible light to the subject PS and displays various information on the body surface of the subject PS (for example, the body surface of the abdomen). The projection controller 167 may project laser light to the body surface of the subject PS to mark a specific position on the body surface. The specific position may be, for example, the port position to be pierced or a position on the volume data where the observation target (for example, the affected part) is present when shifted from the specific position on the body surface in the normal direction. That is, the projection controller 167 may be a laser pointer indicating the port position. In this case, the port position may be displayed in a state where the port position is extended to a range indicating the allowable error.
[0096] In addition, the projection controller 167 may cause the projection unit 170 to project the visible light to the body surface of the subject PS to superimpose and display information assistant robotic surgery (for example, the information regarding the port position or the allowable error information) on the body surface of the subject PS. The superimposing information may be, for example, character information or graphic information. That is, the projection controller 167 may assist the user in robotic surgery using an augmented reality (AR) technique.
[0097] FIG. 4 is a view illustrating a measurement example of a port position of the pre-pierced port PT1. The measurement of the port position may be the 3D measurement. In FIG. 4, the subject PS (for example, a patient) is horizontally placed on a bed BD.
[0098] The depth sensor 410 may include: a light-emitting portion that emits infrared light; a light-receiving portion that receives infrared light; and a camera that captures an image. The depth sensor 410 may detect the distance front the depth sensor 410 to the subject PS based on the infrared light that is emitted from the light-emitting portion to the subject PS and reflected light that is reflected from the subject PS and received by the light-receiving portion. The depth sensor 410 may detect the upper, lower, left, and right sides of an object using the image captured by the camera. As a result, the depth sensor 410 may acquire information of a 3D position (3D coordinates) of each position (for example, the port position of the pre-pierced port PT1) on the body surface of the subject PS.
[0099] The depth sensor 410 may include a processor and an internal memory. The internal memory may store information regarding the shape of the trocar TC. Referring to the shape information of the trocar TC stored in the internal memory, the depth sensor 410 may detect (recognize) the trocar TC provided in the port FT pierced on the body surface of the subject PS to detect (measure) a 3D position of the trocar TC.
[0100] In addition, a predetermined mark may be formed on a surface of the trocar TC. The depth sensor 410 may capture an image using the predetermined mark on the trocar TC as a feature point to detect (recognize) the trocar TC by image recognition. As a result, the depth sensor 410 can improve the recognition accuracy of the trocar TC and can improve the measurement accuracy of the 3D position of the trocar TC.
[0101] In addition, the depth sensor 410 may include a stereo camera instead of the infrared sensor (the light-emitting portion and the light-receiving portion) such that the 3D position of the trocar TC can be measured by image processing. In this case, the depth sensor 410 may measure the 3D position of the trocar TC by recognizing the trocar TC by object recognition in an image captured by a stereo camera, detecting (recognizing) the position of the trocar TC on the body surface of the subject, and calculating the distance to the trocar TC.
[0102] The depth sensor 410 may measure each position or the position of the trocar TC on the body surface of the subject PS in a range that can be reached by the infrared light emitted from the infrared sensor or in a range where an image can be captured by the camera (refer to a range A1 in FIG. 4).
[0103] The deformation simulator 163 of the robotically-assisted surgical device 100 may acquire information regarding each position on the body surface of the subject PS in the actual pneumoperitoneum state, that is, information regarding the shape of the body surface of the subject PS in the actual pneumoperitoneum state from the depth sensor 410. In addition, the deformation simulator 163 may extract the contour (corresponding to the body surface) of the subject PS based on the volume data of the subject PS in the non-pneumoperitoneum state to acquire information regarding each position on the body surface of the subject PS in the non-pneumoperitoneum state, that is, information regarding the shape of the body surface of the subject PS in the non-pneumoperitoneum state.
[0104] The deformation simulator 163 may calculate a difference between each position on the body surface of the subject PS in the actual pneumoperitoneum state and each position on the body surface of the subject PS in the non-pneumoperitoneum state, that is, a difference between the shape of the body surface of the subject PS in the actual pneumoperitoneum state and the shape of the body surface of the subject PS in the non-pneumoperitoneum state. As a result, the deformation simulator 163 can recognize the amount of pneumoperitoneum for allowing the actual pneumoperitoneum state of the subject PS.
[0105] In addition, the deformation simulator 163 may correct a simulation method or a simulation result of the pneumoperitoneum simulation based on the difference between the actual pneumoperitoneum state and the virtual pneumoperitoneum state in the pneumoperitoneum simulation. That is, the deformation simulator 163 may correct a simulation method or a simulation result of the pneumoperitoneum simulation based on the actual amount of pneumoperitoneum. The deformation simulator 163 may store the correction information in the memory 150. In addition, the deformation simulator 163 may receive the amount of scavenging air from a pneumoperitoneum device via the communication unit 110 to correct a simulation method or a simulation result of the pneumoperitoneum simulation. As a result, the robotically-assisted surgical device 100 can improve the accuracy of the pneumoperitoneum simulation.
[0106] Next, an example of displaying a port position will be described.
[0107] The deformation simulator 163 performs the pneumoperitoneum simulation on the volume data obtained in the non-pneumoperitoneum state (for example, by preoperative CT scanning) to generate the volume data of the virtual pneumoperitoneum state. The image generator 162 may perform volume rendering on the volume data of the virtual pneumoperitoneum state to generate a volume rendering image. The image generator 162 may perform surface rendering on the volume data of the virtual pneumoperitoneum state to generate a surface rendering image.
[0108] The deformation simulator 163 may perform the pneumoperitoneum simulation on the volume data obtained in the non-pneumoperitoneum state (for example, by preoperative CT scanning) to generate deformation information regarding deformation from the non-pneumoperitoneum state to the virtual pneumoperitoneum state. The image generator 162 may generate a surface from the volume data acquired in the non-pneumoperitoneum state (for example, by preoperative CT scanning) to generate a surface rendering image. The image generator 162 may apply the shape information to the surface generated from the volume data acquired in the non-pneumoperitoneum state (for example, by preoperative CT scanning) to generate a surface rendering image of the virtual pneumoperitoneum state.
[0109] The display controller 166 may cause the display 130 to visualize the 3D data (the volume rendering image or the surface rendering image of the virtual pneumoperitoneum state) with an annotation of the port position derived from the port position processing unit 164. The display controller 166 causes the display 130 to display the allowable error information.
[0110] The projection controller 167 may project visible light to the port position on the body surface of the subject PS (for example, a patient) derived by the port position processing unit 164 to indicate the port position using the visible light and to visualize the port position. As a result, the user can perform a treatment such as piercing on the port position while checking the port position on the body surface of the subject PS. In addition, the projection controller 167 may project visible light to display the allowable error information on the body surface of the subject PS.
[0111] The projection controller 167 may project visible light to the subject PS to display information regarding the port position on the body surface of the subject PS (for example, a patient) derived by the port position processing unit 164. In this case, the projection controller 167 may display the information regarding the port position (for example, the identification information of the port or an arrow indicating the port position) to superimpose the subject PS using an AR technique. In addition, the projection controller 167 may display the allowable error information to be superimposed on the subject PS using an AR technique. As a result, referring to guide information by the visible light, the user can perform a treatment such as piercing on the port position while checking the information regarding the port position on the body surface of the subject PS.
[0112] Here, the deformation information will be described in detail.
[0113] The deformation simulator 163 detects movement (deformation) of each of the portions included in the volume data to generate the deformation information based on the plurality of volume data (CT images) obtained before and after pneumoperitoneum. In this case, the deformation simulator 163 performs movement analysis (deformation analysis) on the deformation of the plurality of volume data based on the plurality of volume data regarding the amount of pneumoperitoneum to acquire the deformation information in the volume data. A specific method of the deformation analysis is described in, for example, U.S. Pat. No. 8,311,300 and Japanese Patent No. 5408493 which is incorporated herein by reference. These methods are examples of non-rigid registration but may be rigid registration.
[0114] The deformation simulator 163 may acquire, as the deformation information, information regarding the amount of movement or information regarding the velocity at a given point of the volume data. When the method described in US2014/0148816A which is incorporated herein by reference is applied, the deformation simulator 163 separates the volume data into a 2D lattice node (k, l), and 2D coordinates (x, y) in a phase node (k, l, t) of a phase t of the 2D lattice is obtained. In this case, based on a difference between a plurality of nodes (k, l, t) obtained by changing the value of the phase t, the information regarding the amount of movement at the lattice point of the node (k, l) may be calculated. In addition, the deformation simulator 163 may differentiate the information regarding the amount of movement with time to calculate the information regarding the velocity. The information regarding the amount of movement or the velocity may be expressed by a vector.
[0115] When the deformation simulator 163 interpolates the deformation information of the 2D lattice at each point of the entire volume data, the deformation information of each point of the volume data can be obtained. When the deformation information of a predetermined point is applied to each point of a region including an observation site, the deformation information of each point of the region including the observation site can be obtained.
[0116] In addition, when the method described in Japanese Patent No. 5408493 is applied, the deformation simulator 163 may generate the deformation information based on volume data tk-1 and time information tk-1 thereof and volume data tk and time information tk thereof among the volume data (before and after pneumoperitoneum) aligned in time series. The deformation information may indicate information regarding a corresponding position on the plurality of volume data or correspondence of a corresponding object or information regarding the process of a change in the movement of the position and the object. A pixel of each volume data is an index indicating a position at any time between time k-1 and time k.
[0117] The deformation simulator 163 is not limited to the method of US2014/0148816A and may perform deformation analysis using another well-known registration method. The robotically-assisted surgical device 100 performs deformation analysis on each point or the observation site using the deformation information, and thus the movement of any position in the subject before and after pneumoperitoneum can be grasped.
[0118] Next a specific example of a standard port position will be described.
[0119] FIG. 5A is a view illustrating a first placement example of port positions placed on the body surface of the subject PS. FIG. 5B is a view illustrating a second placement example of port positions placed on the body surface of the subject PS. FIG. 5C is a view illustrating a third placement example of port positions placed on the body surface of the subject PS. The placement of a plurality of port positions may be determined, for example, according to the surgical procedure. In FIGS. 5A to 5C, the physical size of the subject PS or the position or size of a disease or the like of the observation target is not considered.
[0120] A plurality of port positions illustrated in FIGS. 5A to 5C are port positions that are planned to be pierced. There may be some errors between the port positions that are planned to be pierced and the port positions that are actually pierced. For example, there may be an error of about 25 mm.
[0121] The ports PT provided on the body surface of the subject PS may include a camera port PTC into which a camera CA is inserted, an end effector port PTE into which the end effector EF is inserted, and an auxiliary port PTA into which forceps held by an assistant are inserted. A plurality of ports PT may be present for each of the types (for example, for each of the camera port PTC, the end effector port PTE, and the auxiliary port PTA), or the sizes of the different types of ports PT may be the same as or different from each other. For example, the end effector port PTE into which the end effector EF for holding an organ or the end effector EF of which the movement in the subject PS is complex is inserted may be larger than the end effector port PTE into which the end effector EF as an electric knife is inserted. The placement position of the auxiliary port PTA may be planned relatively freely.
[0122] In FIG. 5A, large numbers of the end effector ports PTE and the auxiliary ports PTA are linearly arranged in the right direction of the subject PS and in the left direction of the subject PS, respectively, with respect to the port position of the camera port PTC as a reference (the vertex).
[0123] In FIG. 5B, large numbers of end effector ports PTE and the auxiliary ports PTA are linearly aligned with a position of a navel hs interposed therebetween. In addition, the camera port PTC is also placed near the navel hs.
[0124] In FIG. 5C, large numbers of end effector ports PTE and the auxiliary ports PTA are linearly aligned. The position of the navel hs is slightly shifted from the position on the straight line. In addition, the camera port PTC is also placed near the navel hs.
[0125] The reason why a large amount of ports PT are linearly placed is presumed to be that the user can easily recognize the port positions and feels safe. Among the plurality of ports PT, the camera port PTC may be placed at the center of the body surface of the subject PS.
[0126] FIG. 6 is a view illustrating an example of a positional relationship between the subject PS, the ports PT, the trocars TC, and the robot arms AR during robotic surgery.
[0127] In the subject PS, one or more ports PT are provided. In each of the ports PT, the trocar TC is placed. The end effector EF is connected (for example, is inserted) to the trocar TC and a work (treatment) can be performed using the end effector EF in the subject. The port position is disposed to be fixed and does not move during operation. Accordingly, the position of the trocar TC disposed at the port position does not also move. On the other hand, according to the treatment during operation, the robot arms AR and the end effectors are controlled based on the manipulation of the surgeon console, and the robot arms AR move. Accordingly, the positional relationship between the robot arms AR and the trocars TC changes and the angles of the trocars TC with respect to the body surface of the subject PS or the angles of the end effectors EF attached to the trocars TC change. In FIG. 6, a monitor held by an assistant is also illustrated as an end effector.
[0128] Next, the operation of the robotically-assisted surgical device 100 will be described.
[0129] First, the procedure of the port position simulation will be described. FIG. 7 is a flowchart illustrating an example of the procedure of the port position simulation.
[0130] First, the port position processing unit 164 acquires the volume data including the subject PS, for example, via the communication unit 110 (S11). The port position processing unit 164 acquires the kinematic information from the surgical robot 300, for example, via the communication unit 110 (S12). The deformation simulator 163 performs the pneumoperitoneum simulation (S13) to generate the volume data of the virtual pneumoperitoneum state of the subject PS.
[0131] The port position processing unit 164 acquires the information of the surgical procedure (S14). The port position processing unit 164 acquires and sets the positions (initial positions) of the plurality of ports PT according to the acquired surgical procedure (S14). In this case, the port position processing unit 164 may set the positions of the plurality of ports PT in terms of 3D coordinates.
[0132] The port position processing unit 164 acquires the information of the target region (S15).
[0133] The port position processing unit 164 determines whether or not each of the end effectors EF inserted from each of the ports PT is accessible to the target region based on the positions of the plurality of ports acquired in S14 and the position of the target region (S16). Whether or not each of the end effectors EP is accessible to the target region may correspond to whether or not each of the end effectors EF can reach all the positions in the target region. That is, whether or not each of the end effectors EF is accessible to the target region shows that whether or not robotic surgery can be performed by the end effector EF (optionally, the plurality of end effectors EF) according to the acquired surgical procedure, and when each of the end effectors EF is accessible to the target region, robotic surgery can be performed.
[0134] When at least one of the end effectors ET is not accessible to at least a part of the target region, the port position processing unit 164 moves, a port position of at least one port PT included in the plurality of ports PT to be pierced along the body surface of the subject PS (S17). In this case, the port position processing unit 164 may move the port position based on the user input via the UI 120. The port PT to be moved includes at least a port PT into which the end effector EF that is not accessible to at least a part of the target region is inserted.
[0135] When each of the end effectors EF is accessible to the target region, the processing unit 160 ends the process of the port position simulation of FIG. 7.
[0136] As described above, the robotically-assisted surgical device 100 performs the port position simulation such that whether or not each of the end effectors EF is accessible to the target region using the acquired plurality of port positions can be determined and thus whether or not robotic surgery can be performed by the surgical robot 300 using the acquired plurality of port positions can be determined. When the target region is not accessible using the plurality of port positions, the robotically-assisted surgical device 100 may change at least a part of the port positions via the UI 120 so as to determine again whether or not the target region is accessible using the changed plurality of port positions. The robotically-assisted surgical device 100 can plan a combination of a plurality of port positions that are accessible to the target region as the plurality of port positions to be pierced. This way, the robotically-assisted surgical device 100 can plan the port position by the user manually adjusting the port position.
[0137] Next, an example of calculating the port position score will be described.
[0138] The plurality of port positions are determined, for example, according to the surgical procedure, and it may be assumed that each port position is disposed at any positions on the body surface of the subject PS. Accordingly, as the combination of the plurality of port positions, various combinations of port positions may be assumed. One end effector EF mounted on the robot arm AR can be inserted from one port PT into the subject PS. Accordingly, a plurality of end effectors EF mounted on a plurality of robot arms AR can be inserted from a plurality of ports PT into the subject PS.
[0139] A range where one end effector EF can reach the subject PS through the port PT is a working area (individual working area WA1) where a work (treatment in robotic surgery) can be performed by one end effector EF. Accordingly, an area where the individual working areas WA1 of the plurality of end effectors EF superimpose each other is a working area (entire working area WA2) where the plurality of end effectors EF can simultaneously reach the inside of the subject PS through the plurality of ports PT. In a treatment according to the surgical procedure, a predetermined number (for example, three) of end effectors EF needs to be operated at the same time. Therefore, the entire working area WA2 where the predetermined number of end effectors EF can simultaneously reach the inside of the subject PS is considered.
[0140] In addition, the position where the end effector EF can reach the subject PS varies depending on the kinematics of the surgical robot 300, and thus is added to the derivation of a port position as a position where the end effector EF is inserted into the subject PS. In addition, the position of the entire working area WA2 in the subject PS that is required to be secured varies depending on the surgical procedure, and thus is added to the derivation of a port position corresponding to the position of the entire working area WA2.
[0141] The port position processing unit 164 may calculate the port position score for each of the acquired (assumed) combinations of the plurality of port positions. The port position processing unit 164 may plan a combination of port positions having a port position score (for example, a maximum port score) that satisfies predetermined conditions among the assumed combinations of the plurality of port positions. That is, the plurality of port positions included in the planned combination of the port positions may be planned as the plurality of port positions to be pierced.
[0142] A relationship between the port position and the operation of the moving part of the surgical robot 300 may satisfy a relationship described in, for example, Mitsuhiro Hayashibe, Naoki Suzuki, Makoto Hashizume, Kozo Konishi, Asaki Hattori, "Robotic surgery setup simulation with the integration of inverse-kinematics computation and medical imaging", computer methods and programs in biomedicine, 2006, P63-P72 and Pal Johan From, "On the Kinematics of Robotic-assisted Minimally Invasive Surgery", Modeling Identification and Control, Vol. 34, No. 2, 2013, P69-P82, which are incorporated herein by reference.
[0143] FIG. 8 is a flowchart illustrating an operation example when the port position score is calculated by the robotically-assisted surgical device 100.
[0144] Before the process of FIG. 8, the acquisition of the volume data of the subject PS, the acquisition of the kinematic information of the surgical robot 300, the execution of the pneumoperitoneum simulation, and the acquisition of the information of the surgical procedure are performed as in S11 to S14 of the port position simulation illustrated in FIG. 8. In addition, the kinematic information may include the information of each of the end effectors EF mounted on each robot arm according to the surgical procedure. The initial value of the port position score is 0. The port position score is an evaluation function (evaluation value) indicating the value of the combination of the port positions. A variable i is an example of identification information of a work, and a variable j is an example of identification information of a port.
[0145] The port position processing unit 164 generates a work list works, which is a list of works work_i in which each end effector EF is used, according to the surgical procedure (S21). The work work_i includes information for allowing each end effector EF to perform the work in the surgical procedure according to the surgical procedure. The work work_i may include, for example, gripping, dissection, or suture. The work may include a solo work that is performed by a single end effector EF or a cooperative work that is performed by a plurality of end effectors EF.
[0146] Based on the surgical procedure and the volume data of the virtual pneumoperitoneum state, the port position processing unit 164 determines a minimum region least_region_i, which is a region necessary for performing the works work_i included in the work list works (S22). The minimum region may be specified as a 3D region in the subject PS. The port position processing unit 164 generates a minimum region list least_regions, which is a list of the minimum regions least_region_i (S22).
[0147] Based on the surgical procedure, the kinematics of the surgical robot 300, and the volume data of the virtual pneumoperitoneum state, the port position processing unit 164 determines an effective region effective_region_i that is recommended for performing the work work_i included in the work list works (S23). The port position processing unit 164 generates an effective region list effective_regions, which is a list of the effective regions effective_region_i (S23). The effective region may include not only the minimum space (minimum region) for performing the work but also a space that is effective, for example, the end effector EF to operate.
[0148] The port position processing unit 164 acquires information of a port position list ports, which is a list of a plurality of port positions port_j (S24). The port position may be specified by 3D coordinates (x, y, z). The port position processing unit 164 may receive, for example, a user input through the UI 120 to acquire the port position list ports including one or more port positions designated by the user. The port position processing unit 164 may acquire the port position list ports that are stored in the memory 150 as a template.
[0149] Based on the surgical procedure, the kinematics of the surgical robot 300, the volume data of the virtual pneumoperitoneum state, and the acquired plurality of port positions, the port position processing unit 164 determines a port working region region_i, which is a region where each of the end effectors EF can perform each of the works work_i through each of the port positions port_j (S25). The port working region may be specified as a 3D region. The port position processing unit 164 generates a port working region list regions, which is a list of the port working regions region_i (S25).
[0150] The port position processing unit 164 subtracts the port working region region_i from the minimum region least_region_i for each of the works work_i to calculate a subtracted region (subtracted value) (S26). The port position processing unit 164 determines whether or not the subtracted region is an empty region (the subtracted value is negative) (S26). Whether or not the subtracted region is an empty region shows that whether or not a region that is not covered with the port working region region_i (a region that cannot be reached by the end effector EF through the port PT) is present in at least a part of the minimum region least_region_i.
[0151] When the subtracted region is an empty region, the port position processing unit 164 calculates a volume value volume_i, which is the product of the recommended region effective_region_i and the port working region region_i (S27). The port position processing unit 164 sums the volume values volume_i calculated for each of the works work_i to calculate a sum value volume_sum. The port position processing unit 164 sets the sum value volume sum as the port position score (S27).
[0152] That is, when the subtracted region is an empty region, it is preferable that the region that is not covered with the port working region is not present in the minimum region and this port position list ports (the combination of the port positions port_j) is selected. Therefore, in order to promote the selection of the port position list, the value for each of the works work_i is added to the port position score. In addition, by determining the port position score based on the volume value volume_i, as the minimum region or the port working region increases, the port position score increases, and this port position list ports is more likely to be selected. Accordingly, the port position processing unit 164 is more likely to select a combination of port positions in which the minimum region or the port working region is large and each treatment is easy in surgery.
[0153] On the other hand, when the subtracted region is not an empty region, the port position processing unit 164 sets the port position score of the port position list ports to a value of 0 (S28). That is, since the region that is not covered with the port working region is present in at least a part of the minimum region and the work of the target work work_i may not be completed, it is not preferable to select this port position list ports. Thus, in order to make the selection of the port position list ports difficult, the port position processing unit 164 sets the port position score to a value of 0 and excludes the port position list from candidates of the selection. In this case, when the subtracted region is an empty region in a case where another work work_i is performed using the same port position list ports, the port position processing unit 164 sets the port position score to a value of 0 as a whole.
[0154] The port position processing unit 164 may calculate a port position score for all the works work_i by repeating the respective steps of FIG. 8 for all the works work_i.
[0155] as described above, the robotically-assisted surgical device 100 derives the port position score, and when the robotic surgery is performed using the plurality of port positions provided on the body surface of the subject PS, the appropriateness of the combination of the port positions to be pierced can be grasped. The individual working area WA1 and the entire working area WA2 depend on the placement positions of the plurality of pons to be pierced. Even in this case, by using a score (port position score) for each combination of a plurality of port positions, the surgical robot 300 can derive a combination of a plurality of port positions in which, for example, the port position score is a threshold th1 or higher (for example, maximum), and the port positions with which robotic surgery can be easily performed can be set.
[0156] In addition, by appropriately securing the working area based on the port position score, the user can secure a wide visual field in the subject PS that cannot be directly visually observed in robotic surgery, a wide port working region can be secured, and unexpected events can be easily handled.
[0157] In addition, in robotic surgery, the port positions to be pierced are not variable. However, the robot arms AR on which the end effectors inserted into the port positions are mounted are movable in a predetermined range. Therefore, in robotic surgery, depending on the planned port positions, the robot arms AR may interfere with each other. Therefore, port position planning is important. In addition, the positional relationship between the surgical robot 300 and the subject PS cannot be changed during operation in principle. Therefore, port position planning is important.
[0158] FIG. 9 is a view illustrating an example of working areas determined based on the port positions. The individual working area WA1 is an individual working area corresponding to each of the port positions port_j. The individual working area WA1 may be a region in the subject PS that can be reached by each of the end effectors EF. An area where the respective individual working areas WA1 superimpose each other is the entire working area WA2. The entire working area WA2 may correspond to the port working region region_i. The robotically-assisted surgical device 100 can optimize each of the port positions using the port position score, and the suitable individual working areas WA1 and the suitable entire working area WA2 can be derived.
[0159] Next, the details of the port position adjustment will be described.
[0160] The port position processing unit 164 acquires information of the plurality of port positions (candidate positions), for example, based on the template stored in the memory 150 or the user instruction via UI 120. The port position processing unit 164 calculates the port position score for the case using the plurality of port positions based on the acquired combination of the plurality of port positions.
[0161] The port position processing unit 164 may adjust the position of the port PT based on the port position score. In this case, the port position processing unit 164 may adjust the position of the port PT based on the port position score for the acquired plurality of port positions and the port position score obtained when at least one port position among the plurality of port positions is changed. In this case, the port position processing unit 164 may also consider a small movement or a differential of the port position in each of the directions (x direction, y direction, and z direction) in a 3D space.
[0162] The x direction may be a direction along a left-right direction with respect to the subject PS. The y direction may be a forward-backward direction (thickness direction of the subject PS) with respect to the subject PS. The z direction may be an up-down direction (body axis direction of the subject PS) with respect to the subject PS. The x direction, the y direction, and the z direction may be three directions defined by Digital Imaging and Communications in Medicine (DICOM). The x direction, the y direction, and the z direction may be directions other than the above-described directions and are not necessarily the directions with respect to the subject PS.
[0163] For example, the port position processing unit 164 may calculate a port position score F (ports) for the plurality of port positions according to (Expression 1) to calculate a differential value F' of F.
F (port_j(x+.DELTA.x, y, z))-F (port_j(x, y, z))
F (port_j(x, y+.DELTA.y, z))-F (port_j(x, y, z)) (Expression 1)
F (port_j(x, y, z+.DELTA.z))-F (port_j(x, y, z))
[0164] That is, the port position processing unit 164 calculates the port position score F for the port position F (port_j(x+.DELTA.x, y, z)), calculates the port position score F for the port position F (port_j(x, y, z)), and calculates a difference therebetween. This difference value indicates a change in the port position score with respect to a small change of the port position F (port_j(x, y, z)) in the x direction, that is, the differential value F' of F in the x direction.
[0165] In addition, the port position processing unit 164 calculates the port position score F for the port position F (port_j(x, y+.DELTA.y, z)), calculates the port position score F for the port position F (port-j(x, y, z)), and calculates a difference therebetween. This difference value indicates a change in the port position score with respect to a small change of the port position F (port_j(x, y, z)) in the y direction, that is, the differential value F' of F in the y direction.
[0166] In addition, the port position processing unit 164 calculates the port position score F for the port position F (port_j(x, y, z+.DELTA.z)), calculates the port position score F for the port position F (port_j(x, y, z)), and calculates a difference therebetween. This difference value indicates a change in the port position score with respect to a small change of the port position F (port_j(x, y, z)) in the z direction, that is, the differential value F' of F in the z direction.
[0167] The port position processing unit 164 calculates a maximum value of the port position score based on the differential value F of each of the directions. In this case, the port position processing unit 164 may calculate a port position having the maximum port position score according to the steepest descent method based on the differential value F'. The port position processing unit 164 may adjust the port position to optimize the port position such that the calculated port position is a position to be pierced. Instead of the port position in which the port position score is the maximum, the port position may be, for example, a position in which the port position score is the threshold th1 or higher as long as the port position score is improved (increases).
[0168] The port position processing unit 164 may apply this port position adjustment to the adjustment of another port position included in the combination of the plurality of port positions or to the adjustment of port positions of another combination of a plurality of port positions. As a result, the port position processing unit 164 can plan the plurality of ports PT of which the respective port positions are adjusted (for example, optimized) as the port positions to be pierced.
[0169] Regarding the plurality of port positions (coordinates of the port positions), there may be an error of about a predetermined length (for example, 25 mm) between a piercing-planned position and an actual piercing position, and it is presumed that a port position planning accuracy of 3 mm at most is sufficient. Therefore, the port position processing unit 164 may set a plurality of port positions included in the combination of port positions as piercing-planned positions per predetermined length of the body surface of the subject PS, and the port position score may be calculated for each of the plurality of port positions. That is, the piercing-planned positions may be placed in a lattice shape (grid) of the predetermined length (for example, 3 mm) on the body surface of the subject PS. In addition, when it is assumed that the number of ports (for example, the number of intersections in a lattice shape) on the body surface is n and the number of ports included in the combination of port positions is m, the port position processing unit 164 may combine by sequentially selecting m port positions from n port positions and may calculate the port position score for each of the combinations. This way, when the grid is not excessively small as in a lattice shape having an interval of 3 mm, the calculation load of the port position processing unit 164 can be inhibited front being excessive, and the port position scores of all the combinations can be calculated.
[0170] The port position processing unit 164 may adjust the plurality of port positions using a well-known method. The port position processing unit 164 may plan the port positions to be pierced as the plurality of port positions included in the adjusted combination of port positions. The well-known method of the port position adjustment may include techniques described in the followings. Shaun Selha, Pierre Dupont, Robert Howe, David Torchiana, "Dexterity optimization by port placement in robot-assisted minimally invasive surgery", SPIE International Symposium on Intelligent Systems and Advanced Manufacturing, Newton, Mass., 28-31, 2001; Zhi Li, DejanMilutinovic, Jacob Rosen, "Design of a Multi-Arm Surgical Robotic System for Dexterous Manipulation", Journal of Mechanisms and Robotics, 2016; and US2007/0249911 A, which is incorporated herein by reference.
[0171] Next, the allowable error of a port position will be described.
[0172] The port position processing unit 164 derives (for examples, calculates) information (allowable error information) indicating errors that are allowed for each of ports. The port position processing unit 164 may calculate the allowable error information based on the port position score. The port position processing unit 164 may calculate the allowable error information based on the variation of the port position score according to the movement of the port position. The allowable error may be, for example, a value that is more than a threshold th2 (for example, error: 3 mm) representing the highest level of the piercing accuracy of the port position.
[0173] The allowable error information may be displayed on the body surface of the subject PS. In this case, the projection controller 167 may project visible light representing the allowable error information to the body surface of the subject PS. In addition, the display controller 166 may display the allowable error information to superimpose a rendering image obtained by rendering the volume data of the subject PS.
[0174] The allowable error information may be displayed as graphic information or character information. The graphic information may be displayed in a range including the allowable error that includes a port position to be pierced. This range may be a 2D range on the body surface of the subject PS. The 2D range may be a range having a circular shape (for example, an ellipse, a true circle, or other circles), a polygonal shape (for example, a rectangle, a square, a triangle, or other polygons), or other shapes. The circle or the polygon will also be referred to as "primitive shape". The allowable error information may be displayed as other information (for example, information regarding a display manner (a display color, a display size, a display pattern, or a flashing pattern)). For example, when the allowable error of the port PT is large, the port PT may be displayed by a first color, and when the allowable error of the port PT is small, the port PT may be displayed by a second color.
[0175] The robotically-assisted surgical device 100 displays the allowable error information and the user can recognize the allowable error information and can rapidly recognize an allowable range of the piercing of a port position to be pierced. Accordingly, for example, when a spatial (for example, planar) range represented by the allowable error information is large, the user can recognize that a port can be carelessly pierced at a port position to be pierced. In addition, for example, when a spatial (for example, planar) range represented by the allowable error information is small, the user can recognize that a port is required to be accurately pierced at a port position to be pierced. Accordingly, when the robotically-assisted surgical device 100 displays, for example, allowable error information having a large allowable error, the robotically-assisted surgical device 100 can reduce a mental burden of the user who pierces the port PT. In addition, when the robotically-assisted surgical device 100 displays, for example, allowable error information having a large allowable error, the robotically-assisted surgical device 100 can reduce the number of processes required for the user who pierces the port PT to place the port, and can reduce the operative duration. In addition, when the robotically-assisted surgical device 100 displays, for example, allowable error information having a small allowable error, the robotically-assisted surgical device 100 can notify the user that high accuracy is required for the piercing of the port PT.
[0176] FIG. 10 is a flowchart illustrating a derivation procedure of allowable error information by the robotically-assisted surgical device 100. In FIG. 10, the acquisition of the volume data of the subject PS, the acquisition of the kinematic information of the surgical robot 300, the execution of the pneumoperitoneum simulation, and the acquisition of the information of the surgical procedure are performed in advance as illustrated in FIG. 8.
[0177] The port position processing unit 164 acquires information of a plurality of port positions (positions of piercing candidates) (S31). The port position processing unit 164 performs the port position simulation to calculate the port position score based on the acquired plurality of port positions (S32). In this case, the port position processing unit 164 may calculate the port position score based on the surgical procedure, the kinematics of the surgical robot 300, the volume data of the virtual pneumoperitoneum state, and the acquired plurality of port positions. That is, here, the port position processing unit 164 may calculate the port position score for the acquired port positions.
[0178] The port position processing unit 164 acquires allowable decrease information (total allowable decrease information) regarding the degree of decreases in port position scores that are allowed for the acquired plurality of port positions (S33). The allowable decrease information may include information regarding the amount or ratio of the decreases in port position scores that are allowed for the port positions. The port position processing unit 164 may receive a user input via the UI 120 to acquire the total allowable decrease information. The port position processing unit 164 may acquire the total allowable decrease information from the memory 150. The port position processing unit 164 may acquire the total allowable decrease information from the external server is the communication unit 110.
[0179] The port position processing unit 164 acquires allowable decrease information (individual allowable decrease information) regarding the degree of a decrease in port position score that is allowed for each of the port positions (S34). The individual allowable decrease information of the respective ports PT may be the same or different. The port position processing unit 164 may derive (for example, calculate) the individual allowable decrease information based on the total allowable decrease information. In this case, the port position processing unit 164 may divide the amount of allowable decreases represented by the total allowable decrease information by the number of the ports PT to calculate the amount of an allowable decrease for each of the ports represented by the individual allowable decrease information.
[0180] In addition, the port position processing unit 164 may acquire the individual allowable decrease information without acquiring the total allowable decrease information in S33. In this case, the port position processing unit 164 may receive a user input via the UI 120 to acquire the individual allowable decrease information. The port position processing unit 164 may acquire the individual allowable decrease information from the memory 150. The port position processing unit 164 may acquire the individual allowable decrease information from the external server via the communication unit 110.
[0181] When at least one port position is moved, the port position processing unit 164 may derive (for example, calculate) decrease information indicating the degree of a decrease caused by the movement of the port position based on a port position score at the port position (a combination of port positions) before the movement and a port position score at the port position (a combination of port positions) after the movement (S35). The decrease information may include the amount or ratio of a decrease caused by the movement of the port position. In this case, the port position processing unit 164 may subtract the port position score at the port position after the movement from the port position score at the port position before the movement to calculate the amount of the decrease in port position score.
[0182] When the port position is moved, the port position processing unit 164 may calculate the amount of a change (amount of a decrease) in the port position score according to the above-described Expression 1. In this case, the amount of a decrease in the port position score before and after the movement of a port position by a predetermined distance (for example, a small distance) may correspond to the differential value F' of the port position score F.
[0183] In addition, the movement of the port position may be performed in any direction along the body surface of the subject PS. In this case, when a body surface is a plane, the port positions before and after the movement are positioned in a 2D plane along the body surface. In addition, when the body surface includes a curved surface, the port positions before and after the movement are positioned in a 3D space.
[0184] For each of the port positions of the subject PS, the port position processing unit 164 derives a region (allowable region PR) where the decrease information satisfies the allowable decrease information (S36). In this case, the port position processing unit 164 may calculate the allowable region PR where the amount of a decrease represented by the decrease information is less than or equal to the amount of an allowable decrease represented by the allowable decrease information. The allowable region PR may be a region in a 3D space. Accordingly, a contour of the allowable region PR is a position in a 3D space that matches the amount of an allowable decrease represented by the allowable decrease information with respect to the port position. The allowable region PR is an example of the allowable error information.
[0185] The port position processing unit 164 causes the display controller 166 or the projection controller 167 to display a port position and the allowable region PR for the port position for each of the ports PT (S37). In this case, the display controller 166 causes the display 130 to display the port position and the allowable region PR for the port position to superimpose the rendering image of the subject PS for each of the ports PT. In addition, the projection controller 167 may cause the projection unit 170 to project visible light representing the port position and the allowable region PR for the port position to the body surface of the subject PS for each port PT to display the port position and the allowable region PR.
[0186] The port position processing unit 164 may extract the contour of the volume data of the virtual pneumoperitoneum state to acquire information regarding the body surface of the subject PS on which pneumoperitoneum is performed. The port position processing unit 164 may derive (for example, calculate) a superimposing range where the body surface of the subject PS on which pneumoperitoneum is performed and the allowable ration PR superimpose each other. The image generator 162 may perform surface rendering on the volume data of the virtual pneumoperitoneum state to generate a surface rendering image of the derived superimposing range. The display controller 166 may cause the display 130 to display the surface rendering image of the superimposing range.
[0187] In addition, the allowable region PR in the rendering image may be displayed by other information instead of being directly displayed in the region. For example, the display controller 166 may display the allowable region PR by displaying the radius of a range obtained by projecting the allowable region PR to the surface of the rendering image. In addition, the projection controller 167 may display the allowable region PR by projecting visible light representing information indicating the radius of a range obtained by projecting the allowable region PR to the body surface of the subject PS.
[0188] In addition, instead of directly displaying the allowable region PR, the display controller 166 or the projection controller 167 may change the respective port positions using different display manners (for example, a display color, a display pattern, or a flashing pattern) corresponding to the sizes of the allowable regions PR. As a result, by checking the display manner, the user can recognize the size of the allowable region PR and can check whether the allowable error is large or small.
[0189] As described above, by deriving the allowable error information, the robotically-assisted surgical device 100 can derive the piercing accuracy required for the piercing of the port PT. In addition, the robotically-assisted surgical device 100 displays (visualizes) the allowable error information such that the user can visually recognize the allowable error information. Accordingly, the user can check, for example, whether or not the port to be pierced can be carelessly pierced or whether or not it is necessary to carefully pierce the port, and the preparation for the piercing becomes easy.
[0190] Next, errors for port positions in the thickness direction (y direction) of the subject PS will be described.
[0191] FIG. 11 is a view illustrating a first example of errors for port positions in the thickness direction (y direction) of the subject PS. FIG. 12 is a view illustrating a second example of errors for port positions in the thickness direction (y direction) of the subject PS. FIGS. 11 and 12 illustrate errors based on the straight line distances.
[0192] In many cases, the port positions are illustrated in a plan view when the subject PS horizontally placed on the bed BD is seen from the top (the negative side in the y direction, a so-called front view). The error for port positions illustrated in a plan view is the error in a direction along the bed BD and is the error in the xz direction. In practice, positions, which are not illustrated in a plan view, in the y direction perpendicular to the xz direction vary depending on the positions on the body surface.
[0193] In FIG. 11, pneumoperitoneum is performed on the subject PS, and a pneumoperitoneum space ks is present. In FIG. 11, both a port A1 and a port B1 have an error range of 10 mm in the x direction in a plan view. However, when the y direction other than the xz direction indicated in a plan view is taken into consideration, an end portion of the subject in the x direction, that is, the position of the port B1 has a larger error range on the body surface than a center portion of the subject in the x direction. Accordingly, the port B1 has a high influence of errors on the working area in the y direction. It is because the port position score in consideration of the working area changes depending on the position of the port that is variable within the error range.
[0194] In addition, even in FIG. 12, pneumoperitoneum is performed on the subject PS and a pneumoperitoneum space ks is present. As the information of the port position, FIG. 12 illustrates not only information regarding the error range in the xz direction in a plan view but also information regarding the error range in the y direction. Specifically, FIG. 12 illustrates that the distance of the error range of the port A2 from the position corresponding to the navel hs on the body surface in the x direction is in a range of 15 to 20 mm. In addition, in FIG. 12, the distance of the error range of the port B2 from the bed BD is in a range of 150 to 160 mm. The display controller 166 may determine and display at least one information (information regarding the error range along the x direction and the error range along the y direction) as a display target. The error range illustrated in FIGS. 11 and 12 may be within or outside the tolerance.
[0195] Next, a method of measuring the distance for determining the port position will be described.
[0196] For example, when the position of a port is measured from a reference position (for example, the navel hs or a port position adjacent thereto) in order to pierce the port, a straight line distance or a curved distance may be measured. That is, the distance between the position of the port and the reference position may be represented by a straight line distance or a curved distance (for example, the distance along the body surface of the subject PS). As a method of measuring these distances, a method of virtually measuring the distance when the port PT is not actually pierced may be used, or a method of actually measuring the distance when the port PT is actually pierced may be used.
[0197] FIG. 13 is a view illustrating a measurement example of a straight line distance. The straight line distance may be a distance L11 along an xz plane (x direction) or a distance L12 (distance from the bed BD) along the y direction. In addition, for example, when measuring the port position using a ruler, the ruler is put on the body surface of the subject PS for the measurement. Therefore, even when a straight line distance is measured, the straight line distance may be a distance that is not parallel to the xyz direction or a distance on a straight line that is parallel to a part of the body surface.
[0198] FIG. 14 is a view illustrating a measurement example of a curved distance. The curved distance may be a surface distance L13 or L14 from the reference position (for example, the navel hs, the port position adjacent thereto, or the bed BD) along the body surface of the subject PS. The curved distance may be a surface distance in a convex hull generated based on the reference position. In addition, for example, when measuring the port position using a tape measure, since the measurement is performed along the body surface of the subject PS for the measurement, measuring the curved distance is convenient. The measured distance may be input to the measuring instrument 400 as distance information via the operation unit of the measuring instrument 400 such that the distance information is transmitted to the robotically-assisted surgical device 100. In addition, the measured distance may be input by the user via the UI 120 of the robotically-assisted surgical device 100.
[0199] Next, the adjustment of the allowable error depending on the amount of pneumoperitoneum will be described.
[0200] FIG. 15 is a view illustrating an adjustment example of the allowable error depending on the amount of pneumoperitoneum.
[0201] The deformation simulator 163 may perform a pneumoperitoneum simulation kn1 using an amount of pneumoperitoneum kr1 to generate volume data v1. A contour of the volume data v1 is a body surface bs1 of the subject PS of the virtual pneumoperitoneum state that is estimated by the pneumoperitoneum simulation kn1. The deformation simulator 163 may perform a pneumoperitoneum simulation kn2 using a larger amount of pneumoperitoneum kr2 (that is kr2>kr1) than the amount of pneumoperitoneum kr1 to generate volume data v2. A contour of the volume data v2 is a body surface bs2 of the subject PS of the virtual pneumoperitoneum state that is estimated by the pneumoperitoneum simulation kn2. The deformation simulator 163 may perform a pneumoperitoneum simulation kn3 using a larger amount of pneumoperitoneum kr3 (that is kr3>kr2) than the amount of pneumoperitoneum kr2 to generate volume data v3. A contour of the volume data v3 is a body surface bs3 of the subject PS of the virtual pneumoperitoneum state that is estimated by the pneumoperitoneum simulation kn3.
[0202] The port position processing unit 164 derives a 3D allow able region PR based on the volume data v2 of the virtual pneumoperitoneum state obtained based on the amount of pneumoperitoneum kr2. In this case, the port position processing unit 164 may derive (for example, calculate) an allowable range PA2 based on an intersection between the allowable region PR and the body surface bs2. In addition, the port position processing unit 164 may derive (for example, calculate) the allowable ranges PA1 and PA3 based on intersections between the allowable region PR and the body surfaces bs1 and bs3 represented by the contours of the volume data v1 and v3 other than the volume data v2 for deriving the allowable region PR. As the amount of pneumoperitoneum increases, the allowable range may increase. As the amount of pneumoperitoneum decreases, the allowable range may decrease.
[0203] The port position processing unit 164 may project the allowable ranges PA1 and PA3 respectively corresponding to the body surfaces bs1 and bs3 to the body surface bs2 to obtain allowable ranges PA1' and PA3' such that a superimposing range of the allowable ranges PA1', PA2, and PA3' is a minimum allowable range MPA. Even when pneumoperitoneum is performed at any of the amounts of pneumoperitoneum kr1 to kr3, the minimum allowable range MPA is included in the allowable region PR. Accordingly, by piercing the port PT in the minimum allowable range MPA, the port position is within the tolerance irrespective of the amount of pneumoperitoneum. Information indicating the minimum allowable range MPA may be displayed on the display 130 or the body surface of the subject PS. The minimum allowable range MPA may be determined using minimum values of diameters of the allowable ranges PA1', PA2, and PA3'.
[0204] This way, the robotically-assisted surgical device 100 may use a plurality of pneumoperitoneum states to acquire, for example, a result of a standard pneumoperitoneum simulation, a result of a pneumoperitoneum simulation in which the abdomen is largely inflated, and a result of a pneumoperitoneum simulation in which the abdomen is not largely inflated. The robotically-assisted surgical device 100 may acquire superimposing ranges (the allowable ranges PA1 to PA3) of the body surfaces bs1 to bs3 of the results of the respective pneumoperitoneum simulations and the allowable region PR to display the allowable ranges PA1 to PA3. In addition, the robotically-assisted surgical device 100 may derive the minimum allowable range MPA including the same region of the subject PS for the allowable ranges PA1 to PA3 to display the minimum allowable range MPA.
[0205] That is, the port position processing unit 164 may adjust the allowable error based on a variation in the degree of pneumoperitoneum (that is, the amount of pneumoperitoneum), and thus may adjust the allowable region PR based on the port position. The adjustment of the allowable error may include the projection of the allowable region PR to the respective body surfaces bs1 to bs3. In addition, the port position processing unit 164 may derive (for example, calculate) the minimum allowable range MPA as the allowable region PR that does not depend on the variation in the degree of pneumoperitoneum (that is, the amount of pneumoperitoneum). The port position processing unit 164 may cause the display controller 166 or the projection controller 167 to display information indicating the derived minimum allowable range MPA (for example, display a figure representing an outer edge of the minimum allowable range MPA or a display manner that can identify the minimum allowable range MPA). In addition, by using the minimum allowable range MPA as one index, the robotically-assisted surgical device 100 can solve a problem that the position to be pierced deviates from the tolerance depending on the degree of pneumoperitoneum.
[0206] In addition, the port position processing unit 164 may project a 3D allowable region PR of the port obtained from spatial coordinates to the body surfaces bs1 to bs3 of the subject PS based on the movement of the subject PS. The movement of the subject PS is, for example, the movement caused by breathing or heartbeat.
[0207] In addition, even when gas is injected into the subject PS under the same conditions, the pneumoperitoneum state may vary depending on the subject PS. For example, there are a person whose body surface portion is likely to extend and a person whose body surface portion is not likely to extend. In addition, depending on a positional relationship with an organ, a part of the body surface of the subject PS is likely to extend, and another part of the body surface is not likely to extend. Even in this case, the robotically-assisted surgical device 100 can derive the allowable error or the allowable region PR in consideration of the plurality of pneumoperitoneum states. Therefore, unexpected allowable error or an unexpected allowable region PR generated due to the actual amount of pneumoperitoneum can be suppressed.
[0208] Next, a variation of a process relating to the allowable error of a port position will be described.
[0209] The port position processing unit 164 may perform the port position simulation or the port position adjustment in consideration of the allowable error. For example, the port position processing unit 164 may newly plan, as a port position to be pierced, any position in the allowable region PR based on the originally acquired or planned port position. Accordingly, the user can pierce the port PT in a wide range such as any position in the allowable region PR without being limited to a narrow range (position) such as the originally acquired or planned port position. Accordingly, the robotically-assisted surgical device 100 can reduce the mental burden of the user during piercing.
[0210] The port position processing unit 164 may separately process the allowable error of the port PT according to the directions in a 3D space. For example, the port position processing unit 164 separately process the allowable error in the xz direction and the allowable error in the y direction. For example, the port position processing unit 164 may distinguish between a port PT for which it is not necessary to pay attention to the thickness direction (y direction) of the subject PS and a port PT for which it is necessary to pay attention to the thickness direction (y direction) of the subject PS.
[0211] In addition, the port position processing unit 164 may set whether or not to consider the allowable error of the port according to the directions in the 3D space. For example, regarding a port position placed at any position in the 3D space, the allowable error in the xy direction is considered, and the allowable error in the y direction is not considered. In this case, for example, when a position in the thickness direction of the subject PS is pierced, the user does not need to pay attention, and a mental burden during piercing can be reduced.
[0212] In addition, the allowable errors in the respective directions in the 3D space may be the same or different. For example, when the allowable errors in the respective directions in the 3D space are the same, an outer edge of the allowable error is a spherical surface. For example, when the allowable errors in the respective directions in the 3D space are different, an outer edge of the allowable error is, for example, a surface of an ellipsoid or other shapes. In addition, the allowable error may be visualized using any coordinate system that is different from the above-described coordinate system including the x direction, the y direction, and the z direction.
[0213] The port position processing unit 164 may cause the display controller 166 or the projection controller 167 to display that a port PT whose allowable error is a threshold th3 or more (a port whose allowable error at be large) can be marked before pneumoperitoneum. In this case, the port position processing unit 164 may cause the display controller 166 or the projection controller 167 to display a port position estimated before pneumoperitoneum. For example, the port position processing unit 164 may perform the port position simulation or the port position adjustment to plan the port position based on volume data of the non-pneumoperitoneum state instead of the volume data of the virtual pneumoperitoneum state. The port position processing unit 164 may cause the display controller 166 or the projection controller 167 to display the planned port position.
[0214] The port position processing unit 164 may cause the display controller 166 or the projection controller 167 to display that a port PT of which allowable error is less than the threshold th3 (a port of which allowable error is small) cannot be marked before pneumoperitoneum.
[0215] In order to display the allowable region PR, the port position processing unit 164 may use a landmark in the subject PS such as a rib or the navel hs. For example, in a predetermined region including a predetermined port position, the allowable region PR may be a region excluding a rib or a region at a predetermined distance from the navel hs.
[0216] This way, as the port PT, there are a port PT in which the piercing accuracy has a high influence on the individual working area WA1 and a port PT in which the piercing accuracy has a low influence on the individual working area WA1. In addition, the influence of the piercing accuracy on the working area (the individual working area WA1 or the entire working area WA2) varies depending on the surgical procedure.
[0217] On the other hand, by determining the allowable error based on the degree of influence of the piercing accuracy on the working area, the robotically-assisted surgical device 100 can adjust the port positions with respect to the port position of the port PT having a small allowable error. Therefore, the robotically-assisted surgical device 100 can improve the usability of the port position simulation or the port position adjustment.
[0218] In addition, the robotically-assisted surgical device 100 can distinguishably display information regarding the port PT that is required to be carefully pierced during robotic surgery and information regarding the port PT that can be carelessly pierced. Accordingly, by checking the display to pierce the port PT, the user can reduce the operative duration. In addition, for the port that can be carelessly pierced, a cooperative work can be easily performed by a plurality of users, which leads to a reduction in the operative duration.
[0219] In addition, a region (difficult-to-use region) where it is difficult to provide a port, for example, due to medical history and adhesion or the like may be present on the body surface of the subject PS. In addition, in the allowable region PR, the difficult-to-use region and a region (usable region) that is not the difficult-to-use region may be present together. The port position processing unit 164 may receive a user input via the UI 120 to designate the difficult-to-use region. Setting information of the difficult-to-use region may be stored in the memory 150 to be appropriately referred to. In this case, even when a port position to be pierced is included in the difficult-to-use region, the port position processing unit 164 may plan, as a new port position, any position in the usable region of the allowable region PR for the port position to be pierced. The port position processing unit 164 may cause the display controller 166 or the projection controller 167 to distinguishably display the newly planned port position or the usable region of the allowable region PR. As a result, even when adhesion or the like is present in the body of the subject PS, the robotically-assisted surgical device 100 can assist the piercing of another position in the tolerance of the port position to be pierced as a new port position.
[0220] FIG. 16 is a view illustrating a first display example of guide information including information indicating the allowable region PR of the port PT to be pierced. FIG. 17 is a view illustrating a second display example of guide information including information indicating the allowable region PR of the port PT to be pierced. FIG. 16 illustrates a coronal section of the subject PS. FIG. 17 illustrates a sagittal section of the subject PS.
[0221] The images of FIGS. 16 and 17 are the examples displayed by the display 130. However, the guide information may be displayed on the body surface using the visible light by projecting visible light from the projection unit 170 to the body surface of the subject PS. Information regarding lengths included in the guide information is merely exemplary and may be other lengths.
[0222] In FIG. 16, the volume rendering image is displayed, and the guide information is also displayed to superimpose the volume rendering image. The guide information may include identification information (for example, a port A, B, C) of the port PT displayed at the port position to be pierced. The identification information of the port PT is not necessarily displayed.
[0223] In addition, FIG. 16 illustrates that an allowable region PRA where the error is allowed for the piercing of the port A has a radius of 15 mm (r15) from the position of the port A. That is, the allowable region PRA of the port A is in a true circle having a radius of 15 mm whose center is the position of the port A. In addition an allowable region PRB where the error is allowed for the piercing of the port B is within a range of 120 mm.+-.10 mm from the navel hs in the body axis direction (x direction) at a position moved from the navel hs by 20 mm in a direction (z direction) along the body axis direction. The allowable region PRB of the port B may be within a range of 0 mm.+-.20 mm from the navel its in the z direction and within a range of 120 mm.+-.10 mm from the navel hs in the x direction. In addition, an allowable region PRC where the error is allowed for the piercing of the port C is within a range of a 10 mm.times.20 rectangle centering on the position of the port C along the body surface at a position moved from a side end portion (end portion in the x direction) of the subject PS by 100 mm in a direction perpendicular to the body axis direction from the navel hs.
[0224] In FIG. 17, the volume rendering image is displayed, and the guide information is also displayed to superimpose the volume rendering image. The guide information may include identification information (for example, a port D or E) of the port PT displayed at the port position to be pierced. The identification information of the port PT is not necessarily displayed.
[0225] In addition, FIG. 17 illustrates that an allowable region PRD where the error is allowed for the piercing of the port D is within a range of an ellipse having a major axis of 20 mm and a minor axis of 10 mm and centering on a position moved from the navel hs along the body surface in a direction (y direction) perpendicular to the body axis. In addition, in FIG. 17, an allowable region PRE where the error is allowed for the piercing of the port E is within a range of a half of an ellipse having a major axis of 30 mm and a minor axis of 10 mm and centering on a position moved from the navel hs along the body surface in a direction alone the y direction and moved from the bed BD by a distance of 100 mm.
[0226] In addition, in the guide information, an arrow shows a distance between head positions of two direction arrows. In FIGS. 16 and 17, the distance is expressed in mm units. In addition, the position of the navel hs is also shown by an arrow. This distance may be a distance having a certain amount of width (for example, 120 mm.+-.10 mm).
[0227] It can be said that the 2D allowable region PDs (PDA is PDE) illustrated in FIGS. 16 and 17 are the above-described allowable ranges projected to the surface represented by the images of FIGS. 16 and 17.
[0228] Next, display examples of port positions according to Comparative Example and the embodiment will be described.
[0229] FIG. 18 is a view illustrating a display example of port positions according to Comparative Example. In FIG. 18, A, B, C, D, and E are examples of the identification information of the ports, and the lengths thereof are expressed in mm units. The respective values illustrated in FIG. 18 are merely exemplary and may be other values.
[0230] In FIG. 18, a port position of a port C is instructed and displayed at a position moved from the navel hs to the head side in the body axis direction such that the distance between the navel hs and the port C is 20 mm. In addition, the ports A, B, C, D and E are instructed and displayed such that the ports A to E are linearly placed in a direction perpendicular to the body axis direction. That is, the ports A, B, C, D and E are instructed and displayed such that the distance between the port A and the port B is 50 mm, the distance between the port B and the port C is 50 mm, the distance between the port C and the port D is 60 mm, and the distance between the port D and the port E is 40 mm. This way, in Comparative Example, the allowable error of each of the ports A to E is not considered. Therefore, the user needs to accurately pierce each of the ports A to E at the designated position.
[0231] FIG. 19 is a view illustrating a display example of port positions and allowable error information according to the embodiment.
[0232] In FIG. 19, the distance between ports adjacent to each other is instructed and displayed to have a certain amount of width (allowable error). That is, the ports A to E are instructed and displayed such that the distance between the navel hs and the port B is 20 mm to 25 mm, the distance between the port A and the port B is 50 mm to 60 mm, the distance between the port B and the port C is 50 mm to 60 mm, the distance between the port C and the port D is 60 mm to 70 mm, and the distance between the port C and the port E is 100 mm to 105 mm. This way, in the embodiment, the allowable error of each of the ports A to E is considered. Therefore, the user can pierce each of the ports A to E with a certain amount of allowance with respect to the designated position, and a mental burden for piercing the port PT can be reduced.
[0233] Hereinbefore, various embodiments have been described with reference to the drawings. However, it is needless to say that the present disclosure is not limited to these examples. It is obvious to those skilled in the art that various changes or modifications can be conceived within the scope of the claims. Of course, it can be understood that these changes or modifications belong to the technical scope of the present disclosure
[0234] In the first embodiment, the volume data as the captured CT images are transmitted from the CT apparatus 200 to the robotically-assisted surgical device 100. Instead, the volume data may be transmitted to a network server to temporarily accumulate the data and then stored in a server or the like. In this case, as necessary, the communication unit 110 of the robotically-assisted surgical device 100 may acquire the volume data from the server or the like via a wired circuit or a wireless circuit, or may acquire the volume data via any storage medium (not illustrated).
[0235] In the first embodiment, the volume data as the captured CT images are transmitted from the CT apparatus 200 to the robotically-assisted surgical device 100 via the communication unit 110. This example also includes a case where the CT apparatus 200 and the robotically-assisted surgical device 100 are substantially integrated into one product. In addition, the example may also include a case where the robotically-assisted surgical device 100 is considered as a console of the CT apparatus 200.
[0236] In the first embodiment, the CT apparatus 200 captures images to generate volume data including information regarding the inside of an organism. However, another device may capture images to generate volume data. Examples of the other device include a Magnetic Resonance Imaging (MRI) device, a Positron Emission Tomography (PET) device, an angiographic device, and other modality devices. In addition, the PET device may be used in combination with other modality devices.
[0237] In the first embodiment, the surgical robot 300 is connected to the robotically-assisted surgical device 100. However, the surgical robot 300 is not necessarily connected to the robotically-assisted surgical device 100. The reason is for this is that this connection is not particularly limited as long as the kinematic information of the surgical robot 300 is acquired in advance. In addition, the surgical robot 300 may be connected after the end of the piercing of the ports. In addition, only a device that is a part of devices constituting the surgical robot 300 may be connected to the robotically-assisted surgical device 100. In addition, the robotically-assisted surgical device 100 itself may be a part of the surgical robot 300.
[0238] In the first embodiment, the surgical robot 300 is a surgical robot for minimal invasion. However, the surgical robot 300 for minimal invasion may be a surgical robot that assists laparoscopic surgery. In addition, the surgical robot 300 may be a surgical robot that assists endoscopic surgery.
[0239] In the first embodiment, the robotically-assisted surgical device 100 plans the port positions based on the volume data of the virtual pneumoperitoneum state of the subject, but the present disclosure is not limited thereto. For example, when the observation target is a respiratory organ, or a cervical part, robotic surgery may be performed without pneumoperitoneum. That is, the robotically-assisted surgical device 100 may plan the port positions based on the volume data of the non-pneumoperitoneum state.
[0240] In the first embodiment, the subject PS is a human body but may be an animal body.
[0241] The present disclosure is also applicable to a program that implements the function of the robotically-assisted surgical device according to the first embodiment, in which the program is supplied to the robotically-assisted surgical device via a network or various storage media and is read and executed by a computer in the robotically-assisted surgical device.
[0242] As described above, the robotically-assisted surgical device 100 according to the embodiment assists minimally invasive robotic surgery by the surgical robot 300. The processing unit 160 may acquire 3D data of the subject PS (for example, the volume data of the non-pneumoperitoneum state or the volume data of the virtual pneumoperitoneum state). The processing unit 160 may acquire operation information (for example, kinematic information) regard to a moving part (for example, the robot arm AR or the end effector EF) of the surgical robot 300 for performing the robotic surgery. The processing unit 160 may acquire information of a surgical procedure for operating the subject PS. The processing unit 160 may acquire information regarding the position of a port that is to be pierced on a body surface of the subject PS. The processing unit 160 may derive a 2D range on the body surface of the subject PS where the error is allowed for the piercing of the port PT based on the 3D data, the operation information (the kinematic information) of the surgical robot 300, the surgical procedure, and the position of the port PT. This 2D range is an example of the allowable region PD (allowable range) displayed on the display 130 or the body surface of the subject PS. The processing unit 160 may cause the display unit (for example, the display 130) to display the information regarding the position of the port PT and information indicating the 2D range.
[0243] As a result, the robotically-assisted surgical device 100 displays the port position and the information indicating the 2D range, and thus, the user can recognize the degree to which the error is allowed during the piercing of the port PT. That is, the piercing accuracy required for piercing the port PT can be recognized. For example, the user can carelessly perform a piercing work on the port PT that does not require high piercing accuracy and thus, the operative duration can be reduced. For example, the user can carefully perform a piercing work on the port PT that requires high piercing accuracy, and thus, the piercing accuracy can be secured. Since the robotically-assisted surgical device 100 visually provides the user with the information regarding the allowable error (required piercing accuracy), a mental burden of the user during piercing can be reduced.
[0244] In addition, distances between the position of the port PT and respective positions on a contour of the 2D range where the error is allowed for the port PT may include a plurality of different distances.
[0245] As a result, the robotically-assisted surgical device 100 can also allow a state where the allowable error of the port position in a 3D space as a real space is large in a first direction and is small in a second direction. That is, the robotically-assisted surgical device 100 can provide the information regarding the allowable error that is more suitable for an actual condition such that the allowable error of the port position in a 3D space as a real space is not necessarily uniform and may have directivity. For example, the user can check a piercing position without being excessively careful in a direction in which the allowable error is large and can carefully check a piercing position in a direction in which the allowable error is small. For example, the user can perform measurement only in the direction in which the allowable error is small, and can visually determine the position in the direction in which the allowable error is large.
[0246] In addition, the processing unit 160 may perform a pneumoperitoneum simulation on volume data of the subject PS to generate the 3D data of a virtual pneumoperitoneum state.
[0247] As a result, the user can check the allowable error in consideration of the 3D data of the virtual pneumoperitoneum state.
[0248] In addition, the processing unit 160 may perform a plurality of pneumoperitoneum simulations on volume data of the subject PS with different amounts of pneumoperitoneum to generate the 3D data of a plurality of virtual pneumoperitoneum states. The processing unit 160 may derive a plurality of 2D ranges based on the 3D data of the plurality of virtual pneumoperitoneum states. The processing unit 160 may display the information regarding the position of the port and information indicating the plurality of 2D ranges.
[0249] As a result, the robotically-assisted surgical device 100 can display the information regarding the plurality of allowable errors corresponding to the pneumoperitoneum state. Since the way of extension of the body surface during pneumoperitoneum or the placement of organs in the subject PS varies, even when gas is injected into the respective subjects PS under the same conditions, the pneumoperitoneum states may vary, respectively. In addition, since the amount of gas during pneumoperitoneum varies depending on patients in consideration of the ventilation capacities of the patients or the risk of complications, the pneumoperitoneum states may vary. Therefore, it is difficult to accurately estimate the pneumoperitoneum state before pneumoperitoneum. On the other hand, the robotically-assisted surgical device 100 can display the respective information regarding the allowable errors corresponding to various pneumoperitoneum states, and the user can easily check the allowable errors corresponding to various pneumoperitoneum states.
[0250] In addition, the processing unit 160 may perform a plurality of pneumoperitoneum simulations on volume data of the subject PS with different amounts of pneumoperitoneum to generate the 3D data of a plurality of virtual pneumoperitoneum states. The processing unit 160 may derive a plurality of 2D ranges based on the 3D data of the plurality of virtual pneumoperitoneum states. The processing unit 160 may derives a minimum allowable range that is a range on the body surface of the subject commonly included in the plurality of 2D ranges. The processing unit 160 may display the information regarding the position of the port and information regarding the minimum allowable range MPA.
[0251] As a result, the robotically-assisted surgical device 100 can display the information regarding the plurality of allowable errors corresponding to the pneumoperitoneum state. Since the way of extension of the body surface during pneumoperitoneum or the placement of organs in the subject PS varies, even when gas is injected into the respective subjects PS under the same conditions, the pneumoperitoneum states may vary, respectively. Therefore, it is difficult to accurately estimate the pneumoperitoneum state before pneumoperitoneum. On the other hand, the robotically-assisted surgical device 100 can display the information regarding the allowable errors in consideration of various pneumoperitoneum states, and the user can easily check the allowable errors corresponding to various pneumoperitoneum states.
[0252] In addition, a shape of the 2D range may include a primitive shape.
[0253] As a result, the robotically-assisted surgical device 100 can visually provide the user with information regarding the allowable error in a primitive shape that can be easily understood by the user.
[0254] In addition, the processing unit 160 may render the 3D data to generate a rendering image. The processing unit 160 may cause the display unit (for example, the display 130) to visualize the 3D data with an annotation of the information regarding the position of the port PT and information regarding a position of the 2D range.
[0255] As a result, the user can check the port position of the port to be pierced on the subject PS and the allowable error on the display 130. In addition, the robotically-assisted surgical device 100 uses the 3D data such that the user can estimate the influence of the piercing of the port on the inside of the subject PS in consideration of the allowable error.
[0256] In addition, the processing unit 160 may causes the projection unit 170 to project visible light representing the information regarding the position of the port PT and information regarding a position of the 2D range to the body surface of the subject such that the information regarding the position of the port PT and information indicating the plurality of 2D ranges are displayed on the body surface of the subject PS.
[0257] As a result, the robotically-assisted surgical device 100 can project the information regarding the port position of the port PT to be pierced and the 2D range directly to the subject PS on which robotic surgery is performed. Therefore, the user can check the information regarding the port position and the 2D range projected to the subject PS to be pierced. Accordingly, the user can recognize the allowable error using the visible light on the subject PS as a mark, and can pierce the port PT with a reduced mental burden.
[0258] The present disclosure is useful for, for example, a robotically-assisted surgical device capable of recognizing a piercing accuracy required for piercing a port, a robotically-assisted surgery method, and a program.
* * * * *
D00000

D00001

D00002

D00003

D00004

D00005

D00006

D00007

D00008

D00009

D00010

D00011

D00012
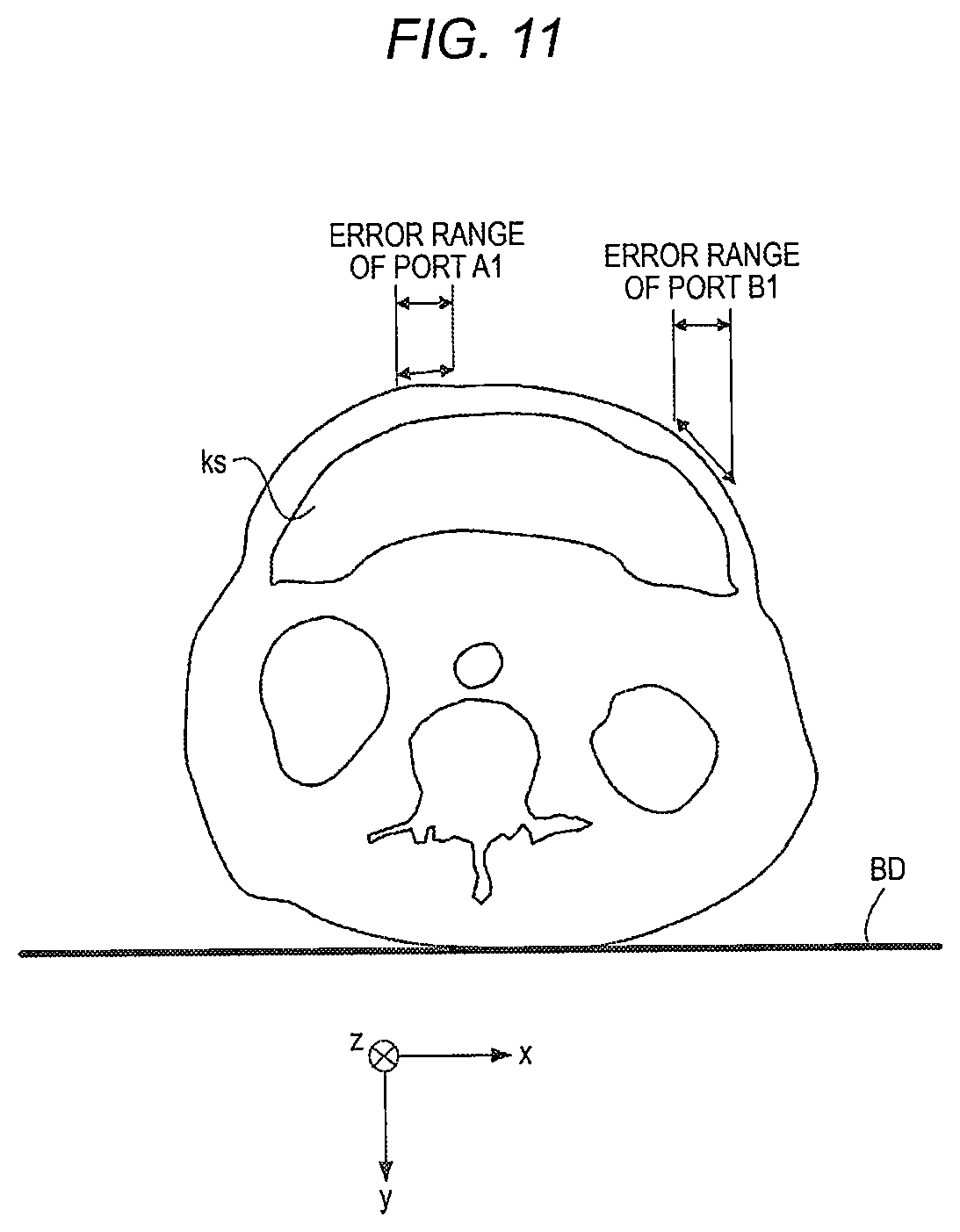
D00013
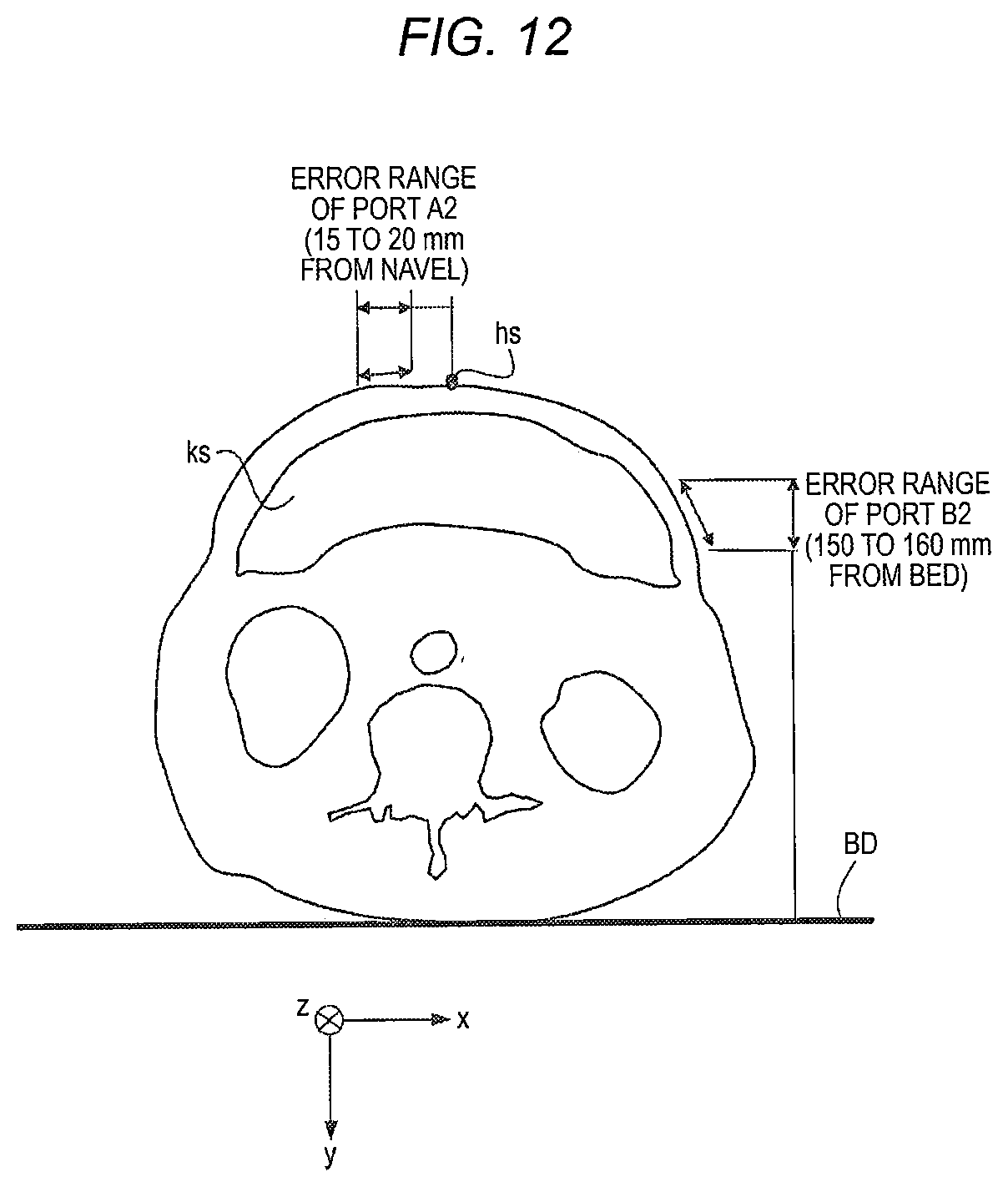
D00014
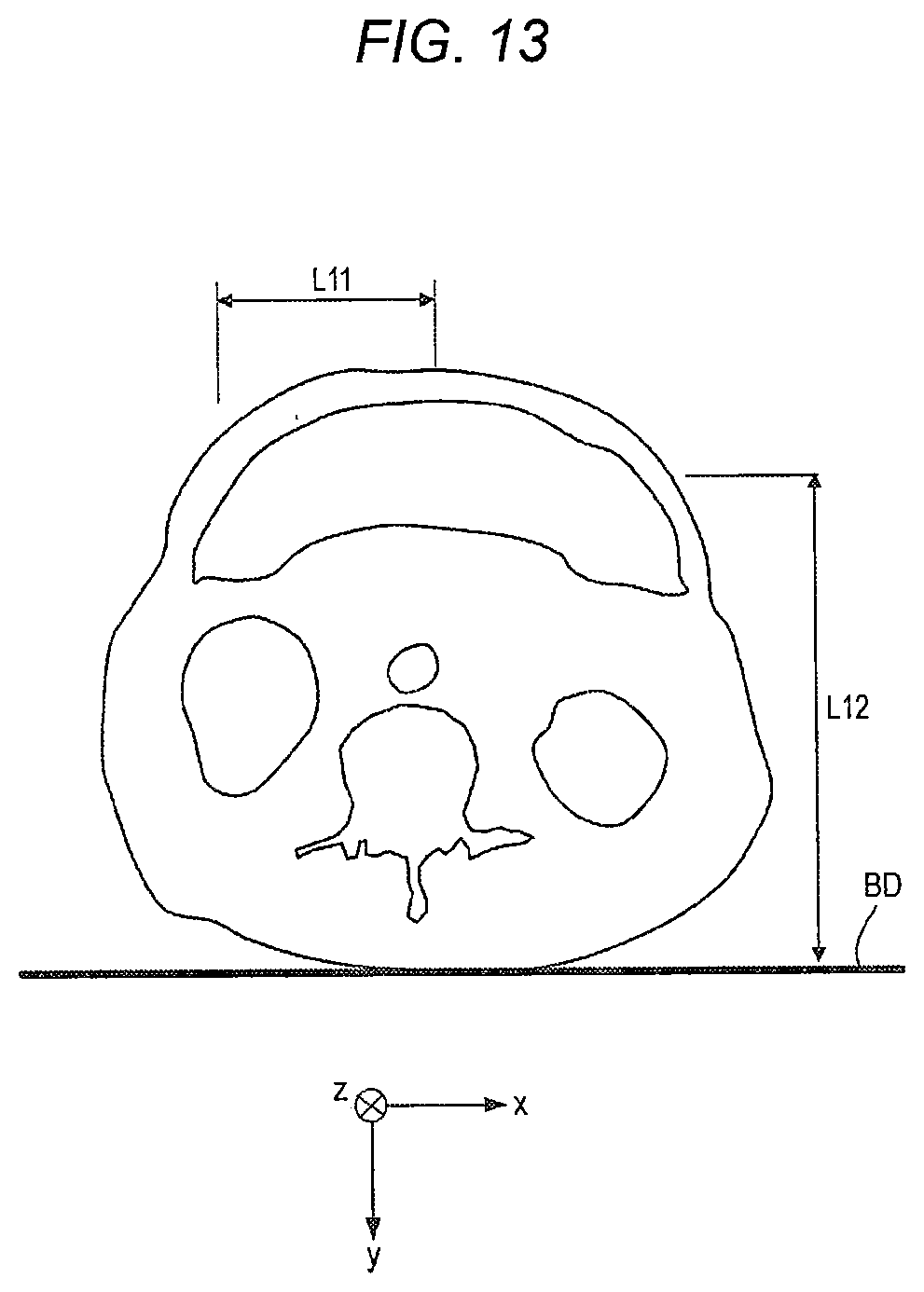
D00015
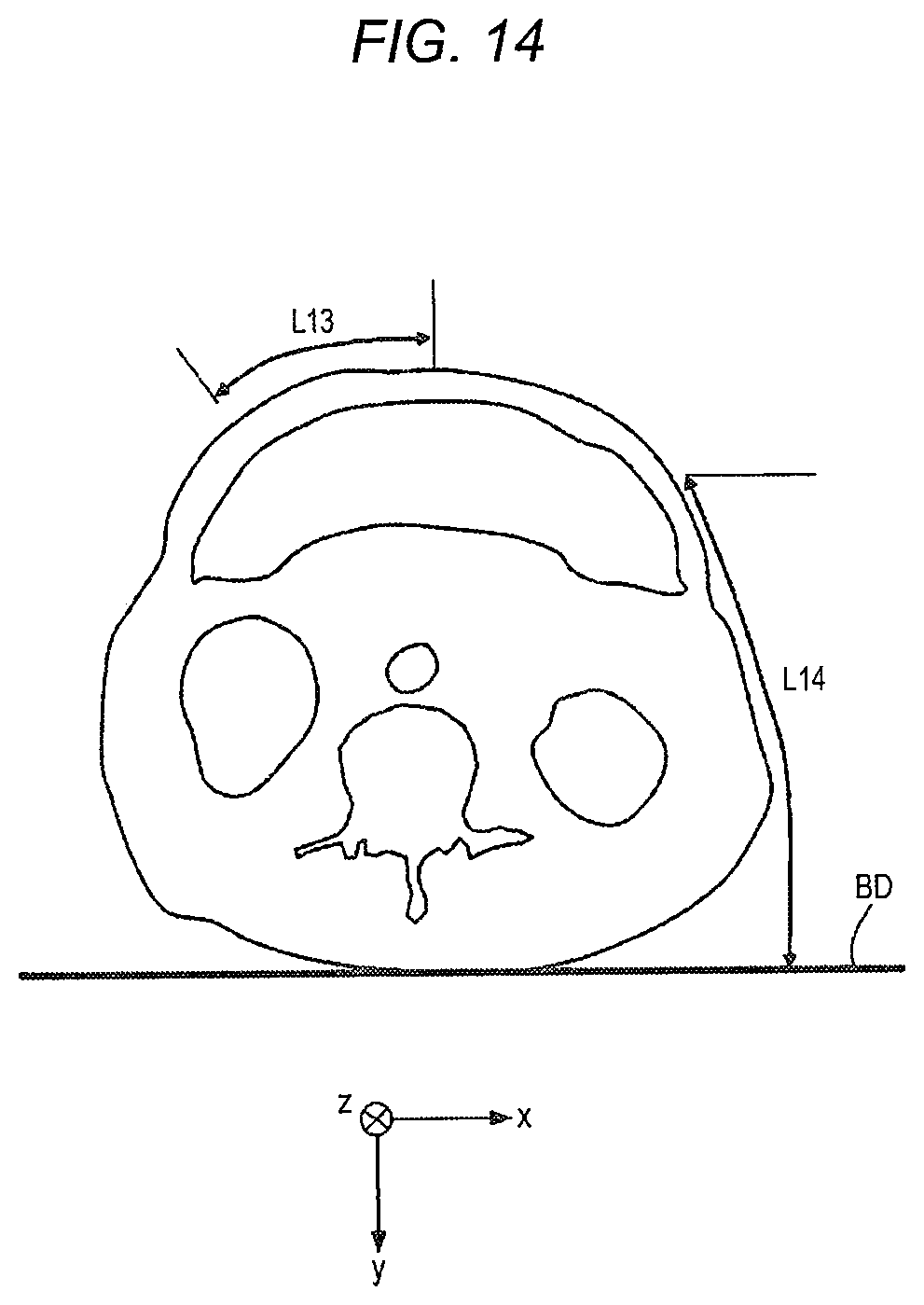
D00016
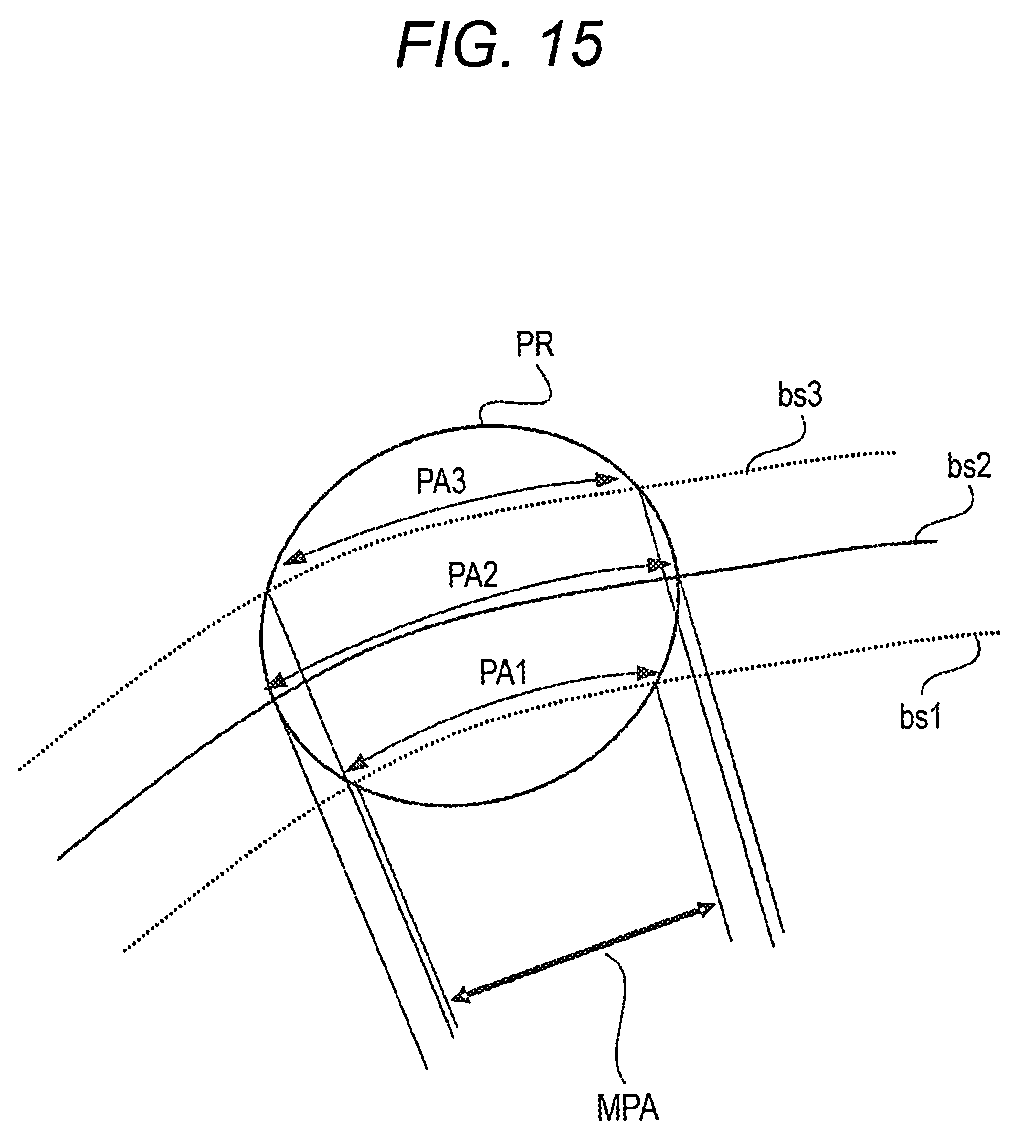
D00017
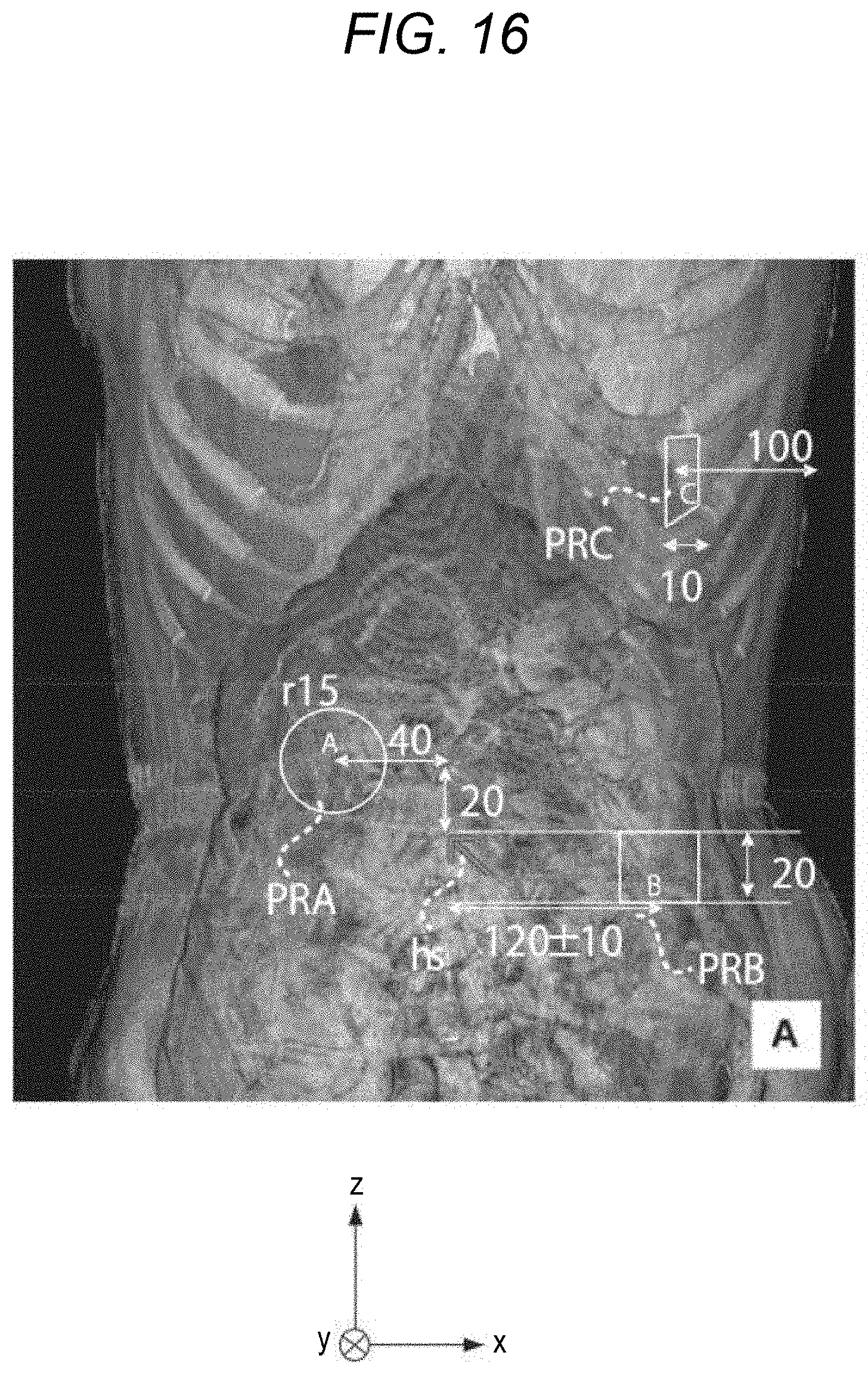
D00018

D00019
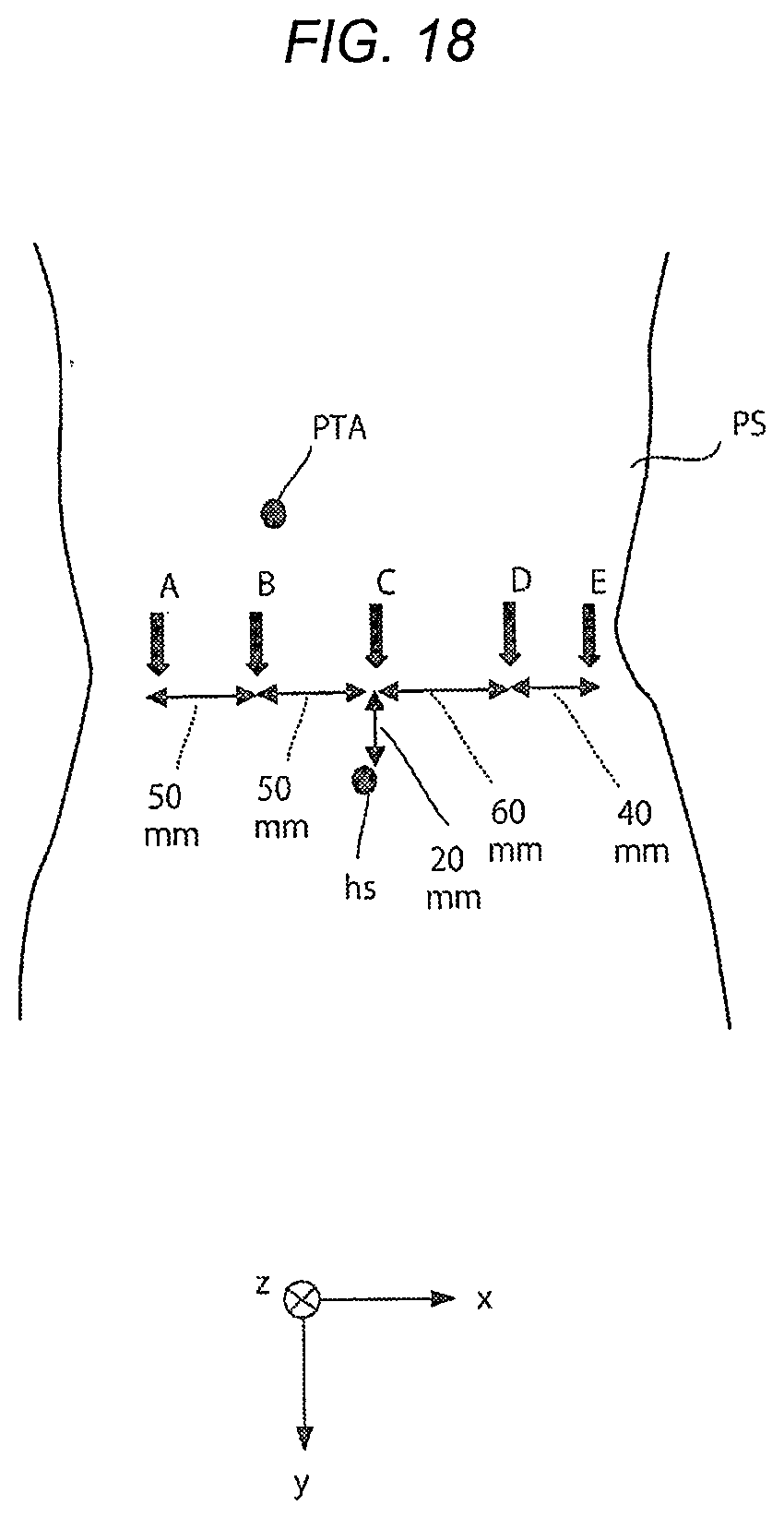
D00020
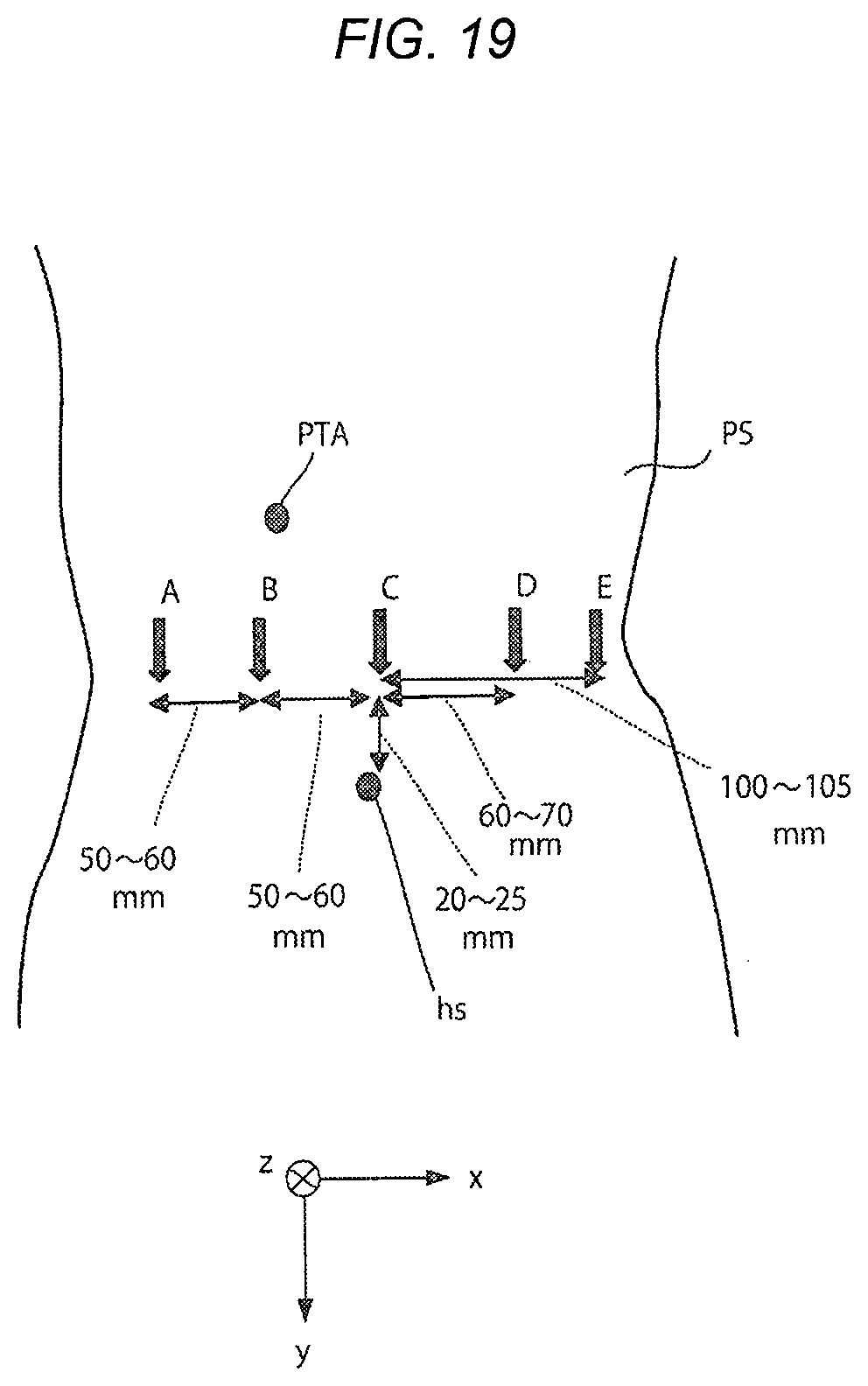
D00021

XML
uspto.report is an independent third-party trademark research tool that is not affiliated, endorsed, or sponsored by the United States Patent and Trademark Office (USPTO) or any other governmental organization. The information provided by uspto.report is based on publicly available data at the time of writing and is intended for informational purposes only.
While we strive to provide accurate and up-to-date information, we do not guarantee the accuracy, completeness, reliability, or suitability of the information displayed on this site. The use of this site is at your own risk. Any reliance you place on such information is therefore strictly at your own risk.
All official trademark data, including owner information, should be verified by visiting the official USPTO website at www.uspto.gov. This site is not intended to replace professional legal advice and should not be used as a substitute for consulting with a legal professional who is knowledgeable about trademark law.