Method And Device For Detecting Heart Rhythm Irregularities
LIN; Shiming
U.S. patent application number 16/465508 was filed with the patent office on 2020-02-27 for method and device for detecting heart rhythm irregularities. The applicant listed for this patent is BIV MEDICAL, LTD., Shiming LIN. Invention is credited to Shiming LIN.
| Application Number | 20200060562 16/465508 |
| Document ID | / |
| Family ID | 62241240 |
| Filed Date | 2020-02-27 |






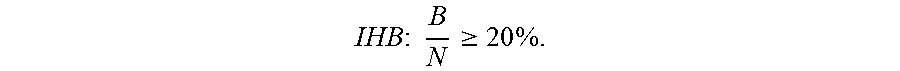
| United States Patent Application | 20200060562 |
| Kind Code | A1 |
| LIN; Shiming | February 27, 2020 |
METHOD AND DEVICE FOR DETECTING HEART RHYTHM IRREGULARITIES
Abstract
A method for detecting heart rhythm irregularities, including the steps of: measuring pulse peaks continuously over a period of time to obtain pulse peak sequence and pulse peak time interval sequence corresponding to the pulse peak sequence; and calculating the absolute value of a difference between a single pulse peak time interval in the pulse peak time interval sequence and an average value of the pulse peak time interval sequence, and determining that an irregular pulse peak (IPP) has occurred if the absolute value is larger than or equal to 15% to 25% of the average value of the pulse peak time interval sequence. A detection device using the method is also provided. This uses a non-invasive approach to detect heart rhythm irregularities such as sick sinus syndrome, irregular pulse peaks, irregular heartbeat, and atrial fibrillation, and can be applied to a sphygmomanometer or a wearable device.
| Inventors: | LIN; Shiming; (Taipei, TW) | ||||||||||
| Applicant: |
|
||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Family ID: | 62241240 | ||||||||||
| Appl. No.: | 16/465508 | ||||||||||
| Filed: | November 29, 2017 | ||||||||||
| PCT Filed: | November 29, 2017 | ||||||||||
| PCT NO: | PCT/CN2017/113528 | ||||||||||
| 371 Date: | May 30, 2019 |
Related U.S. Patent Documents
| Application Number | Filing Date | Patent Number | ||
|---|---|---|---|---|
| 62497740 | Dec 1, 2016 | |||
| 62497747 | Dec 1, 2016 | |||
| 62601843 | Apr 4, 2017 | |||
| Current U.S. Class: | 1/1 |
| Current CPC Class: | A61B 5/046 20130101; A61B 5/0235 20130101; F04B 39/123 20130101; F04B 43/02 20130101; A61B 5/02141 20130101; A61B 5/0225 20130101; A61B 5/02208 20130101; F04B 45/047 20130101; F04B 39/121 20130101; F04B 53/10 20130101; A61B 5/681 20130101; A61B 5/02 20130101; A61B 5/021 20130101 |
| International Class: | A61B 5/046 20060101 A61B005/046; A61B 5/022 20060101 A61B005/022; A61B 5/00 20060101 A61B005/00 |
Claims
1. A method for detecting heart rhythm irregularities, comprising the steps of: a) measuring pulse peaks continuously over a period of time to obtain a pulse peak sequence and a pulse peak time interval sequence corresponding to the pulse peak sequence; and b) calculating the absolute value of a difference between a single pulse peak time interval in the pulse peak time interval sequence and an average value of the pulse peak time interval sequence, and determining that an irregular pulse peak (IPP) has occurred if the absolute value is larger than or equal to 15% to 25% of the average value of the pulse peak time interval sequence.
2. The method for detecting heart rhythm irregularities of claim 1, wherein the method further comprises the step of: c) performing the determination of the occurrence (or absence) of an irregular pulse peak on each pulse peak time interval in the pulse peak time interval sequence, calculating the ratio of the number of the identified irregular pulse peaks to the total number of the time intervals in the pulse peak time interval sequence, and determining that irregular heartbeat (IHB) has occurred if the ratio is larger than or equal to a threshold value.
3. The method for detecting heart rhythm irregularities of claim 1, wherein the method further comprises the steps of: d) pausing for a period of time, then measuring pulse peaks continuously over another period of time to obtain a second pulse peak sequence and a second pulse peak time interval sequence corresponding to the second pulse peak sequence, and performing the foregoing determination of the occurrence (or absence) of irregular heartbeat; e) pausing for a period of time, then measuring pulse peaks continuously over another period of time to obtain a third pulse peak sequence and a third pulse peak time interval sequence corresponding to the third pulse peak sequence, and performing the foregoing determination of the occurrence (or absence) of irregular heartbeat; and f) determining that atrial fibrillation (AF) has occurred if at least two occurrences of irregular heartbeat are identified in the three consecutive performances of the determination of the occurrence (or absence) of irregular heartbeat.
4. The method for detecting heart rhythm irregularities of claim 1, wherein the determination of the occurrence of an irregular pulse peak includes grading an irregular pulse peak according to the percentage of the average value of the pulse peak time interval sequence that the absolute value is larger than or equal to.
5. The method for detecting heart rhythm irregularities of claim 4, wherein an irregular pulse peak is graded as a 15% irregular pulse peak (IPP 15%) if the absolute value is larger than or equal to 15% of the average value of the pulse peak time interval sequence, as a 20% irregular pulse peak (IPP 20%) if the absolute value is larger than or equal to 20% of the average value of the pulse peak time interval sequence, or as a 25% irregular pulse peak (IPP 25%) if the absolute value is larger than or equal to 25% of the average value of the pulse peak time interval sequence.
6. The method for detecting heart rhythm irregularities of claim 1, wherein the method for detecting heart rhythm irregularities determines that sick sinus syndrome (SSS) has occurred if a single pulse peak time interval in the pulse peak time interval sequence is longer than or equal to 3 seconds or if the pulse peak frequency of the pulse peak time interval sequence is lower than or equal to 50 times per minute.
7. The method for detecting heart rhythm irregularities of claim 6, wherein the detection is carried out with a sphygmomanometer that measures blood pressure by the oscillometric method.
8. A detection device, comprising: a detecting portion for measuring pulse peaks continuously over a period of time; a recording portion for receiving and recording measurement data obtained by the detecting portion; a processor for performing computation on the measurement data in the recording portion and for determining the occurrence of heart rhythm irregularities by the method of claim 1; and a display device for displaying a determination result of the processor.
9. The detection device of claim 8, wherein the detection device is a sphygmomanometer that measures blood pressure by the oscillometric method or the auscultatory method, or a smartwatch that measures blood pressure/heart rhythm through an inflatable bladder.
10. The detection device of claim 8, wherein the detecting portion includes: a bladder adapted to be wrapped around a user's limb at a position corresponding to an artery; an air pressure pump for inflating the bladder; at least one pressure sensor for measuring the pressure in the bladder; a pressure relief valve through which air is discharged from the bladder; and a microcontroller unit for controlling the operation of the air pressure pump and the pressure relief valve.
Description
BACKGROUND OF THE INVENTION
1. Technical Field
[0001] The present invention relates to a method and device for detecting heart rhythm irregularities. More particularly, the invention relates to a method and device that measure pulse peaks in order to detect an irregular pulse peak (IPP), irregular heartbeat (IHB), atrial fibrillation (AF), and sick sinus syndrome (SSS).
2. Description of Related Art
[0002] The human circulatory system is composed of the heart, blood vessels, and blood, and is driven by contraction of the heart. Each time the heart contracts, the blood in the left ventricle is squeezed into the aorta and then into the other arteries in the body. As the diameter of an artery increases with the pressure therein when a large amount of blood enters the artery, the contraction and relaxation of the ventricles in a cardiac cycle causes arteries to expand and recoil (i.e., to pulsate) in a cyclic manner. The pulsation of arteries that are relatively close to the skin can be felt by hand and is known as the pulse.
[0003] Generally, a normal pulse is synchronous with heartbeat, and an irregular pulse may arise from a clinical disease, especially one related to the heart. Pulse measurement, therefore, is an important physical examination item for those with, or prone to, cardiovascular disease. A physician may also diagnose diseases according to variation in the pulse.
[0004] Heart rhythm irregularities may take many forms, including an abnormal pulsation frequency or rhythm of the heart, an abnormal origin of cardiac impulse, an abnormal conduction velocity in the heart, an abnormal sequence of excitation of the heart, and so on. The mechanisms by which heart rhythm irregularities are formed can be divided into two major categories: abnormal impulse formation and abnormal impulse conduction. Heart rhythm irregularities caused by abnormal impulse formation include those associated with the sinus node such as sinus tachycardia, sinus bradycardia, sinus arrhythmia, and sinus arrest; other examples include an escape beat, paroxysmal tachycardia, atrial fibrillation, ventricular fibrillation, and other ectopic rhythms. Heart rhythm irregularities caused by abnormal impulse conduction include sinoatrial block, sick sinus syndrome, atrioventricular block, and so on. Of all the heart rhythm irregularities, atrial fibrillation is the one that requires medical attention the most often because it may increase the risk of heart failure, dementia, and stroke.
[0005] To discover a heart rhythm irregularity as early as possible, the first step is to monitor heart rate and heart rhythm and determine whether they are regular, and to note the starting time, ending time, and duration of any irregularity. Nowadays, heart rate is generally monitored by measuring the electrical potential of the heart or by photoplethysmography. The former method is commonly known as electrocardiography (ECG), in which electrodes are placed on the skin of a person's chest to record the electrophysiological activities of the heart, or more particularly to record the electrical potential difference of the cardiac cells between the polarization and depolarization processes of each heartbeat so that the rhythm of pulsation of the heart can be derived accordingly. The latter method is currently in common use in smart bracelets and works on the principle that blood absorbs light of certain wavelengths. More specifically, a device projects light to a user's skin, and the user's heartbeat is measured by detecting variation of the light reflected from the skin. While the ECG method provides the more accurate measurement result, the operation and determination skills required are also more sophisticated, not to mention the costly ECG equipment. As to photoplethysmography, it is subject to interference from the environment (e.g., the sweat on a user's skin and the degree of contact between the sensor and the user's skin) and therefore has relatively large measurement errors. Apart from the above, sphygmomanometers can also be used to measure the pulse in the following manner. A manually or automatically inflatable cuff is wrapped around the arm, and the pulse is observed by means of a resonance device or stethoscope while determining the systolic pressure and diastolic pressure.
[0006] Today, monitoring devices that can take relatively accurate measurement of the pulse or heart rate are generally bulky and hence do not allow monitoring wherever and whenever desired. Smart bracelets that claim to be capable of measuring or monitoring heart rate in real time (based on measurement of the pulse) are indeed available, but despite their portability, huge measurement errors tend to result from the environment, which poses a tremendous risk of health to those who have cardiovascular disease and require their heart rates to be accurately monitored. Besides, while heart rhythm irregularities may be accompanied by a pulse deficit, directly identifying an irregular pulse as a heart rhythm irregularity could be erroneous. It is therefore imperative to have an algorithm that can preclude misjudgment of heart rhythm irregularities. Moreover, there has never been a method or device that not only can measure heart rate, but also can determine the occurrence of sick sinus syndrome and detect such heart rhythm irregularities as irregular pulse peaks, irregular heartbeat, and atrial fibrillation.
BRIEF SUMMARY OF THE INVENTION
[0007] In order to solve the above problems, the primary objective of the present invention is to provide a method for detecting heart rhythm irregularities, comprising the steps of: a) measuring pulse peaks continuously over a period of time to obtain a pulse peak sequence and a pulse peak time interval sequence corresponding to the pulse peak sequence; and b) calculating the absolute value of a difference between a single pulse peak time interval in the pulse peak time interval sequence and an average value of the pulse peak time interval sequence, and determining that an irregular pulse peak (IPP) has occurred if the absolute value is larger than or equal to 15% to 25% of the average value of the pulse peak time interval sequence.
[0008] In one preferred embodiment, the method for detecting heart rhythm irregularities further comprises the step of: c) performing the determination of the occurrence (or absence) of an irregular pulse peak on each pulse peak time interval in the pulse peak time interval sequence, calculating the ratio of the number of the identified irregular pulse peaks to the total number of the time intervals in the pulse peak time interval sequence, and determining that irregular heartbeat (IHB) has occurred if the ratio is larger than or equal to a threshold value.
[0009] In one preferred embodiment, the method for detecting heart rhythm irregularities further comprises the steps of: d) pausing for a period of time, then measuring pulse peaks continuously over another period of time to obtain a second pulse peak sequence and a second pulse peak time interval sequence corresponding to the second pulse peak sequence, and performing the foregoing determination of the occurrence (or absence) of irregular heartbeat; e) pausing for a period of time, then measuring pulse peaks continuously over another period of time to obtain a third pulse peak sequence and a third pulse peak time interval sequence corresponding to the third pulse peak sequence, and performing the foregoing determination of the occurrence (or absence) of irregular heartbeat; and f) determining that atrial fibrillation (AF) has occurred if at least two occurrences of irregular heartbeat are identified in the three consecutive performances of the determination of the occurrence (or absence) of irregular heartbeat.
[0010] In one preferred embodiment, the determination of the occurrence of an irregular pulse peak includes grading an irregular pulse peak according to the percentage of the average value of the pulse peak time interval sequence that the absolute value is larger than or equal to.
[0011] In one preferred embodiment, an irregular pulse peak is graded as a 15% irregular pulse peak (IPP 15%) if the absolute value is larger than or equal to 15% of the average value of the pulse peak time interval sequence, as a 20% irregular pulse peak (IPP 20%) if the absolute value is larger than or equal to 20% of the average value of the pulse peak time interval sequence, or as a 25% irregular pulse peak (IPP 25%) if the absolute value is larger than or equal to 25% of the average value of the pulse peak time interval sequence.
[0012] In one preferred embodiment, the method for detecting heart rhythm irregularities determines that sick sinus syndrome (SSS) has occurred if a single pulse peak time interval in the pulse peak time interval sequence is longer than or equal to 3 seconds or if the pulse peak frequency of the pulse peak time interval sequence is lower than or equal to 50 times per minute.
[0013] In one preferred embodiment, the detection is carried out with a sphygmomanometer that measures blood pressure by the oscillometric method.
[0014] Another objective of the present invention is to provide a detection device, comprising: a detecting portion for measuring pulse peaks continuously over a period of time; a recording portion for receiving and recording measurement data obtained by the detecting portion; a processor for performing computation on the measurement data in the recording portion and for determining the occurrence of heart rhythm irregularities by the foregoing method; and a display device for displaying a determination result of the processor.
[0015] In one preferred embodiment, the detection device is a sphygmomanometer that measures blood pressure by the oscillometric method or the auscultatory method, or a smartwatch that measures blood pressure/heart rhythm through an inflatable bladder.
[0016] In one preferred embodiment, the detecting portion includes: a bladder adapted to be wrapped around a user's limb at a position corresponding to an artery; an air pressure pump for inflating the bladder; at least one pressure sensor for measuring the pressure in the bladder; a pressure relief valve through which air is discharged from the bladder; and a microcontroller unit for controlling the operation of the air pressure pump and the pressure relief valve.
[0017] The present invention provides a method and device that use a non-invasive approach to detecting heart rhythm irregularities. In addition to monitoring a person's heart rate continuously, the method and device disclosed herein can determine the occurrence of such heart rhythm irregularities as sick sinus syndrome, irregular pulse peaks, irregular heartbeat, and atrial fibrillation by means of a special algorithm. The method and device of the invention can be applied to a sphygmomanometer or a wearable device (e.g., a smartwatch) in order to detect, for example, the radial artery in a user's arm and measure the user's pulse and its rhythm, thereby adding to the convenience of self-measurement. The invention is advantageous in that it reduces errors associated with the use of a photoplethysmographic detection device (e.g., errors resulting from the way the detection device is worn or from the sweat on a user's skin) and is suitable for personal or household daily health care. A sphygmomanometer capable of detecting heart rhythm irregularities as disclosed herein can be used in emergency rooms, intensive care units, hospital wards, clinics, and other medical institutions and therefore has high utility value in the medical industry.
BRIEF DESCRIPTION OF THE SEVERAL VIEWS OF THE DRAWINGS
[0018] FIG. 1 shows the steps of the method for detecting heart rhythm irregularities according to a preferred embodiment of the present invention.
[0019] FIG. 2 is an assembled perspective view of the detection device according to a preferred embodiment of the present invention.
[0020] FIG. 3 is a side view of the detection device according to a preferred embodiment of the present invention.
[0021] FIG. 4 is a perspective view of the bladder of the detection device according to a preferred embodiment of the present invention.
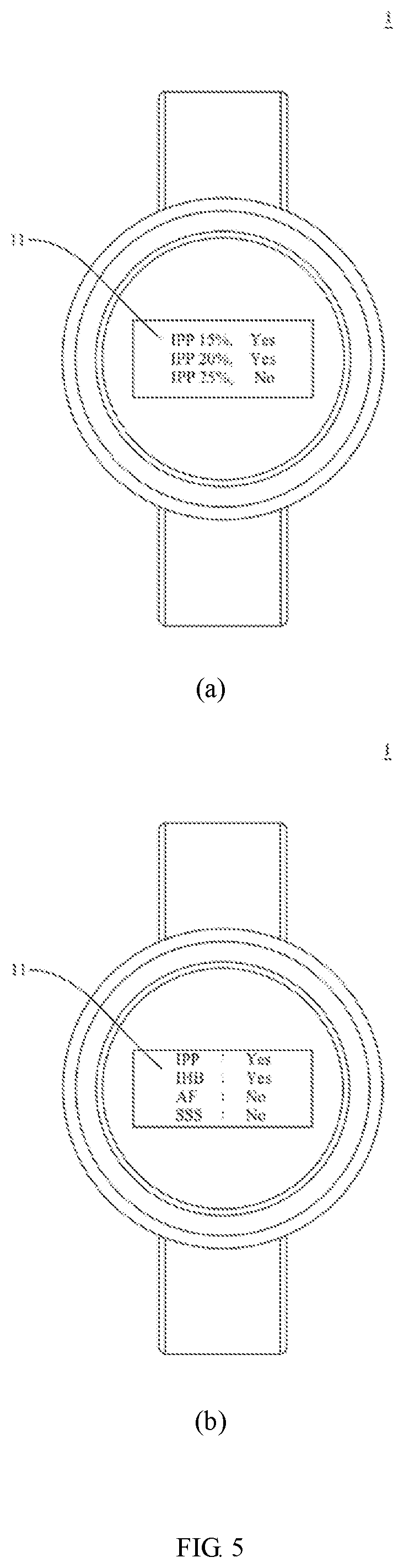
[0022] FIG. 5 shows the display screen diagrams (a) and (b) of the detection device according to a preferred embodiment of the present invention.
[0023] FIG. 6 shows the pulse signals of the method for detecting heart rhythm irregularities according to a preferred embodiment of the present invention.
DETAILED DESCRIPTION OF THE INVENTION
[0024] The details and technical solution of the present invention are hereunder described with reference to accompanying drawings. For illustrative sake, the accompanying drawings are not drawn to scale. The accompanying drawings and the scale thereof are not restrictive of the present invention.
[0025] Throughout the whole document, the terms "comprises or includes" and/or "comprising or including" used in the document mean that one or more other components, steps, operations, and/or the existence or addition of elements are not excluded in addition to the described components, steps, operations and/or elements. The terms "about or close to" or "substantially" mean a value or range that is close to the allowable specified error to avoid any unreasonable use by third parties, illegal or unfair use, to understand the precise or absolute value disclosed herein. The terms "a" and "an" refer to one or to more than one (i.e., to at least one) of the grammatical object of the article.
[0026] Referring to FIG. 1, the present invention provides a method for detecting heart rhythm irregularities, and the method includes the steps of: a) measuring pulse peaks continuously over a period of time to obtain a pulse peak sequence and a pulse peak time interval sequence corresponding to the pulse peak sequence; and b) calculating the absolute value of the difference between a single pulse peak time interval in the pulse peak time interval sequence and the average value of the pulse peak time interval sequence, and determining that an irregular pulse peak (IPP) has occurred if the absolute value is larger than or equal to 15% to 25% of the average value of the pulse peak time interval sequence.
[0027] As used herein, the term "heart rhythm irregularity" refers to an abnormal pulsation frequency or rhythm of the heart, an abnormal origin of cardiac impulse, an abnormal conduction velocity in the heart, an abnormal sequence of excitation of the heart, or the like, whose clinical characteristics may include an exceedingly fast, exceedingly slow, or irregular rhythm of the heart. In one preferred embodiment, the present invention can identify heart rhythm irregularities by detecting one or (in a separate manner) a combination of heart rhythm irregularities selected from the group consisting of irregular pulse peaks, irregular heartbeat, atrial fibrillation, and sick sinus syndrome. In a more preferred embodiment, the present invention can identify heart rhythm irregularities by detecting irregular pulse peaks, irregular heartbeat, atrial fibrillation, and sick sinus syndrome simultaneously.
[0028] As used herein, the term "pulse peak" refers to a waveform of the pulsation of an artery, or more particularly a curve representing the rise and fall of the pressure in an artery when blood flows therethrough during a cardiac cycle. Pulse peaks reflect how an artery pulsates and serve as a means by which to locate a lesion and identify the corresponding symptom.
[0029] As used herein, the term "irregular pulse peak" (IPP) refers to a condition in which an irregular rhythm of the heart can be inferred from pulse peaks measured continuously over a period of time. In one embodiment of the present invention, the method for detecting heart rhythm irregularities includes the steps of: a) measuring pulse peaks continuously over a period of time to obtain a pulse peak sequence and a pulse peak time interval sequence corresponding to the pulse peak sequence; and b) calculating the absolute value of the difference between a single pulse peak time interval in the pulse peak time interval sequence and the average value of the pulse peak time interval sequence, and determining that an irregular pulse peak has occurred if the absolute value is larger than or equal to 15% to 25% of the average value of the pulse peak time interval sequence. In one preferred embodiment, the determination of the occurrence of an irregular pulse peak further includes grading an irregular pulse peak according to the percentage of the average value of the pulse peak time interval sequence that the absolute value is larger than or equal to, wherein the percentage includes but is not limited to 5%, 10%, 15%, 20%, and 25%. In a more preferred embodiment, an irregular pulse peak is graded as a 15% irregular pulse peak (IPP 15%) if the absolute value is larger than or equal to 15% of the average value of the pulse peak time interval sequence, as a 20% irregular pulse peak (IPP 20%) if the absolute value is larger than or equal to 20% of the average value of the pulse peak time interval sequence, or as a 25% irregular pulse peak (IPP 25%) if the absolute value is larger than or equal to 25% of the average value of the pulse peak time interval sequence.
[0030] As used herein, the term "irregular heartbeat" (also known as cardiac arrhythmia or cardiac dysrhythmia) refers to a condition in which a heart rhythm irregularity exceeding a normal range (i.e., exceeding a threshold value) can be inferred from pulse peaks measured continuously over a period of time. In one embodiment of the present invention, the method for detecting heart rhythm irregularities includes the steps of: a) measuring pulse peaks continuously over a period of time to obtain a pulse peak sequence and a pulse peak time interval sequence corresponding to the pulse peak sequence; b) calculating the absolute value of the difference between a single pulse peak time interval in the pulse peak time interval sequence and the average value of the pulse peak time interval sequence, and determining that an irregular pulse peak has occurred if the absolute value is larger than or equal to 15% to 25% of the average value of the pulse peak time interval sequence; and c) performing the determination of the occurrence (or absence) of an irregular pulse peak on each pulse peak time interval in the pulse peak time interval sequence, calculating the ratio of the number of the identified irregular pulse peaks to the total number of the time intervals in the pulse peak time interval sequence, and determining that irregular heartbeat has occurred if the ratio is larger than or equal to a threshold value. The threshold value may be 5%, 10%, 15%, 20%, 25%, 30%, 35%, or 40%; the present invention has no limitation in this regard. In one preferred embodiment, irregular heartbeat is determined to have occurred if the ratio of the number of the identified irregular pulse peaks to the total number of the time intervals in the pulse peak time interval sequence is larger than or equal to 20%.
[0031] As used herein, the term "atrial fibrillation" refers to a condition in which a heart rhythm irregularity exceeding a normal range and having an increasing duration or frequency can be inferred from pulse peaks measured continuously over a period of time. Clinically, atrial fibrillation is the most common of all heart rhythm irregularities. In one embodiment of the present invention, the method for detecting heart rhythm irregularities includes the steps of: a) measuring pulse peaks continuously over a period of time to obtain a pulse peak sequence and a pulse peak time interval sequence corresponding to the pulse peak sequence; b) calculating the absolute value of the difference between a single pulse peak time interval in the pulse peak time interval sequence and the average value of the pulse peak time interval sequence, and determining that an irregular pulse peak has occurred if the absolute value is larger than or equal to 15% to 25% of the average value of the pulse peak time interval sequence; c) performing the determination of the occurrence (or absence) of an irregular pulse peak on each pulse peak time interval in the pulse peak time interval sequence, calculating the ratio of the number of the identified irregular pulse peaks to the total number of the time intervals in the pulse peak time interval sequence, and determining that irregular heartbeat has occurred if the ratio is larger than or equal to a threshold value; d) pausing for a period of time, then measuring pulse peaks continuously over another period of time to obtain a second pulse peak sequence and a second pulse peak time interval sequence corresponding to the second pulse peak sequence, and performing the foregoing determination of the occurrence (or absence) of irregular heartbeat; e) pausing for a period of time, then measuring pulse peaks continuously over another period of time to obtain a third pulse peak sequence and a third pulse peak time interval sequence corresponding to the third pulse peak sequence, and performing the foregoing determination of the occurrence (or absence) of irregular heartbeat; and f) determining that atrial fibrillation has occurred if at least two occurrences of irregular heartbeat are identified in the three consecutive performances of the determination of the occurrence (or absence) of irregular heartbeat. In another embodiment of the present invention, atrial fibrillation is determined to have occurred if at least three occurrences of irregular heartbeat are identified in five consecutive performances of the determination of the occurrence (or absence) of irregular heartbeat.
[0032] As used herein, the term "sick sinus syndrome" refers to a condition in which there is at least one incidence of the heart pausing for at least 3 seconds or the heart beats slower and slower (typically with a heart rate/pulse rate lower than 40 to 50 times per minute). Sick sinus syndrome may have such symptoms as dizziness and physical weakness. In one embodiment of the present invention, the method for detecting heart rhythm irregularities determines that sick sinus syndrome has occurred if a single pulse peak time interval in the pulse peak time interval sequence is longer than or equal to 3 seconds or if the pulse peak frequency (also known as pulse frequency) of the pulse peak time interval sequence is lower than or equal to 50 times per minute.
[0033] As used herein, the term "period of time" refers to either a time span of continuous measurement or an intermission, the former of which may be 5 seconds, 10 seconds, 15 seconds, 20 seconds, 25 seconds, 30 seconds, 40 seconds, 50 seconds, 60 seconds, and so on without limitation, and the latter of which may be 5 seconds, 10 seconds, 15 seconds, 20 seconds, 25 seconds, 30 seconds, and so on without limitation. In one preferred embodiment of the present invention, the method for detecting heart rhythm irregularities uses a 25-second time span of continuous measurement and a 10-second intermission.
[0034] As used herein, the term "intermission" refers to a period of time over which measurement and/or recording and/or computation (the present invention has no limitation in this regard) is temporarily stopped.
[0035] The present invention also provides a detection device that includes: a detecting portion for measuring pulse peaks continuously over a period of time; a recording portion for receiving and recording the measurement data obtained by the detecting portion; a processor for performing computation on the measurement data in the recording portion and for determining the occurrence (or absence) of heart rhythm irregularities by the foregoing method for detecting heart rhythm irregularities; and a display device for displaying the determination result of the processor.
[0036] As used herein, the term "detection device" refers to a device for determining the occurrence (or absence) of heart rhythm irregularities by the foregoing method for detecting heart rhythm irregularities, and the device may be a sphygmomanometer, a smart bracelet, a smartwatch, or the like, without limitation. In one preferred embodiment of the present invention, the detection device is a sphygmomanometer that measures blood pressure by the oscillometric method or the auscultatory method. In another preferred embodiment of the present invention, the detection device is a smartwatch that measures blood pressure/heart rhythm through an inflatable bladder (see FIG. 3).
[0037] As used herein, the term "detecting portion" refers to the portion of the detection device that is configured to measure pulse peaks continuously over a period of time, and the detecting portion may use either the resonance method or the low-pressure method as its detection method, without limitation. In one preferred embodiment, the detecting portion includes: a bladder adapted to be wrapped around a user's limb at a position corresponding to an artery, wherein the artery may be, but is not limited to, a brachial artery or a radial artery; an air pressure pump for inflating the bladder so that, once inflated, the bladder occludes the artery temporarily; at least one pressure sensor for measuring the pressure in the bladder; a pressure relief valve through which air is discharged from the bladder; and a microcontroller unit for controlling the operation of the air pressure pump and the pressure relief valve. In one preferred embodiment, the detecting portion detects pressure variation by the oscillometric method or the auscultatory method in order to obtain pulse signals.
[0038] As used herein, the term "recording portion" refers to the portion of the detection device that is configured to receive and record the measurement data obtained by the detecting portion, wherein the measurement data at least includes data or graphs that show the correspondence between pulse peaks and time (or time points), among other information. The recording portion may be any stationary or movable random access memory (RAM), read-only memory (ROM), flash memory, other similar devices, or a combination of the above.
[0039] As used herein, the term "processor" refers to the portion of the detection device that is configured to perform computation on the measurement data in the recording portion and to determine the occurrence (or absence) of heart rhythm irregularities by the foregoing method for detecting heart rhythm irregularities. More specifically, the processor may be coupled to the recording portion, where the measurement data is stored, in order to perform the predetermined steps by accessing the program(s) or data in the recording portion. The processor may be a central processing unit (CPU), a programmable general-purpose or special-purpose microprocessor, a digital signal processor (DSP), a programmable controller, an application-specific integrated circuit (ASIC), a programmable logic device (PLD), other similar devices, or a combination of the above. In another preferred embodiment, the processor and the recording portion form a co-constructed processor for loading the prestored program(s) in the recording portion and executing the corresponding commands and algorithms.
[0040] As used herein, the term "display device" refers to the portion of the detection device that is configured to display the determination result of the processor. For example, in cases where the detection device of the present invention is implemented as a desktop device, such as a sphygmomanometer, the display device may be an externally connected display screen, and in cases where the detection device of the present invention is implemented as a wearable device, such as a smartwatch, the display device may be the screen of the smartwatch (see FIG. 5); the present invention has no limitation in this regard.
[0041] The detection device of the present invention may be further connected to a communication module for transmitting the determination result or the recorded data to an external device or for enabling remote control. The communication module may communicate with a remote processor or other device in a wired or wireless manner. Wired communication can be carried out, for example, via a physical transmission interface configured for electrical or optical signal transmission, and wireless communication, via one or a combination of at least two of the following protocols/techniques: Bluetooth, infrared (IR) transmission, near-field communication (NFC), ultra-wideband (UWB), wireless local area networks (WLAN), Wireless Gigabit Alliance (WiGig Alliance) communications technology, ZigBee, wireless universal serial bus (wireless USB), and Wi-Fi. The present invention has no limitation on the type of the communication module or the communication protocol or encryption method used thereby.
[0042] The present invention will be described in more detail below with reference to some illustrative embodiments. It should be understood, however, that the embodiments serve only to facilitate understanding, but not to restrict the scope, of the invention.
[0043] I. Embodiment 1--Determining the Occurrence (Absence) of an Irregular Pulse Peak
[0044] Referring to steps a and b in FIG. 1, the method of the present invention for detecting heart rhythm irregularities can be used to detect an irregular pulse peak, and the determination steps are as follows:
[0045] [Step a]:
[0046] Pulse peaks are measured continuously for 25 seconds to obtain a pulse peak sequence and a pulse peak time interval sequence P.sub.(i) corresponding to the pulse peak sequence, where i is an integer ranging from 1 to N.
[0047] Referring to the pulse signal graph in FIG. 6, pulse signals are detected while the bladder is gradually pressurized (i.e., inflated). Pulse peaks are measured continuously for 25 seconds such that a pulse peak sequence and a pulse peak time interval sequence P.sub.(i) corresponding to the pulse peak sequence are obtained, where i is an integer ranging from 1 to 15. During the 25-second period, the first pulse peak detected (indicated by the letter a in FIG. 6) and the second pulse peak detected (indicated by the letter b in FIG. 6) are spaced apart by the first time interval (indicated by the notation P.sub.(i) in FIG. 6).
[0048] [Step b]:
[0049] The average value M of the pulse peak time interval sequence P.sub.(i) is calculated, and then the absolute value of the difference between a single pulse peak time interval and the average value M is calculated. If the absolute value is larger than or equal to any value between 15% and 25% of the average value M inclusive, it is determined that an irregular pulse peak (IPP) has occurred. Mathematically, the determination of the occurrence of IPP can be expressed by the following inequality: [0050] IPP: |P.sub.(i)-M|.gtoreq.M.times.(15%-25%), where i is an integer ranging from 1 to N.
[0051] [Step b-1]: Determining the Degree of Irregularity of the Irregular Pulse Peak Identified
[0052] In embodiment 1, the irregularity of the irregular pulse peak identified can be graded as follows according to the percentage of the average value M of the pulse peak time interval sequence that the absolute value is larger than or equal to: [0053] IPP 15%: |P.sub.(i)-M|.gtoreq.M.times.15%, where i is an integer ranging from 1 to N; [0054] IPP 20%: |P.sub.(i)-M|.gtoreq.M.times.20%, where i is an integer ranging from 1 to N; or [0055] IPP 25%: |P.sub.(i)-M|.gtoreq.M.times.25%, where i is an integer ranging from 1 to N.
[0056] [Repeated Detection Mode]
[0057] The determination of the occurrence (or absence) of an irregular pulse peak can be performed repeatedly and consecutively for a plurality of times, e.g., three times as detailed below. Pulse peaks are measured continuously over the first 25-second time span of continuous measurement, and the first set of IPP-related computation is carried out accordingly. Then, measurement is stopped for a 10-second intermission, before the second 25-second time span of continuous measurement begins and gives rise to the second set of IPP-related computation. After that, measurement is stopped for another 10-second intermission, before the third 25-second time span of continuous measurement begins and gives rise to the third set of IPP-related computation. Thus, three IPP determination results are obtained to avoid errors attributable to a single measurement.
[0058] The present invention has no limitation on the number of times for which detection should be repeated, the time span of continuous measurement, or the duration of the intermission.
[0059] II. Embodiment 2-Determining the Occurrence (or Absence) of Irregular Heartbeat
[0060] Referring to step c in FIG. 1, the method of the present invention for detecting heart rhythm irregularities can be used to detect irregular heartbeat, and the determination step is as follows:
[0061] [Step c]:
[0062] Following step b, IPP determination is performed on each pulse peak time interval in the pulse peak time interval sequence P.sub.(i), i.e., on the first through the N.sup.th pulse peak time intervals. The number B of the irregular pulse peaks identified in the sequence P.sub.(i) is counted. Then, the ratio of the number B of the identified irregular pulse peaks to the total number N of the time intervals in the sequence P.sub.(i) is calculated. If the ratio is larger than or equal to a threshold value, it is determined that irregular heartbeat (IHB) has occurred. The threshold value in this embodiment is 20%, but the present invention has no limitation on this value. Mathematically, the determination of the occurrence of IHB can be expressed by the following inequality:
IHB : B N .gtoreq. 20 % . ##EQU00001##
[0063] [Repeated Detection Mode]
[0064] The determination of the occurrence (or absence) of irregular heartbeat can be performed repeatedly and consecutively for a plurality of times, e.g., three times as detailed below. Pulse peaks are measured continuously over the first 25-second time span of continuous measurement, and the first set of IHB-related computation is carried out accordingly. Then, measurement is stopped for a 10-second intermission, before the second 25-second time span of continuous measurement begins and gives rise to the second set of IHB-related computation. After that, measurement is stopped for another 10-second intermission, before the third 25-second time span of continuous measurement begins and gives rise to the third set of IHB-related computation. Thus, three IHB determination results (i.e., the IHB determination results 1, 2, and 3 in FIG. 1) are obtained to avoid errors attributable to a single measurement.
[0065] The present invention has no limitation on the number of times for which detection should be repeated, the time span of continuous measurement, or the duration of the intermission.
[0066] III. Embodiment 3-Determining the Occurrence (or Absence) of Atrial Fibrillation
[0067] Referring to steps d to f in FIG. 1, the method of the present invention for detecting heart rhythm irregularities can be used to detect atrial fibrillation, and the determination steps are as follows:
[0068] [Step d]:
[0069] After step c (i.e., after determining the occurrence or absence of IHB in the sequence P.sub.(i)), measurement is stopped for 10 seconds. Then, pulse peaks are measured continuously for 25 seconds to obtain another pulse peak sequence and a pulse peak time interval sequence Q.sub.(i) corresponding to this pulse peak sequence, where i is an integer ranging from 1 to N. The occurrence (or absence) of IHB in the sequence Q.sub.(i) is determined as in step c.
[0070] [Step e]:
[0071] Measurement is stopped for 10 seconds, and then pulse peaks are measured continuously for 25 seconds to obtain yet another pulse peak sequence and a pulse peak time interval sequence R.sub.(i) corresponding to this pulse peak sequence, where i is an integer ranging from 1 to N. The occurrence (or absence) of IHB in the sequence R.sub.(i) is determined as in step c.
[0072] [Step f]:
[0073] If at least two occurrences of irregular heartbeat are found in steps c to e (i.e., if IHB is determined to have occurred in at least two of the sequences P.sub.(i), Q.sub.(i), and R.sub.(i)), it is determined that atrial fibrillation (AF) has occurred.
[0074] IV. Embodiment 4-Determining the Occurrence (or Absence) of Sick Sinus Syndrome
[0075] The method of the present invention for detecting heart rhythm irregularities can also be used to derive the pulse frequency or the pulsation frequency of the heart (i.e., heart rate) from pulse peaks measured continuously over a period of time.
[0076] [Step g]:
[0077] Referring to step g in FIG. 1, sick sinus syndrome is determined to have occurred if a single pulse peak time interval in the pulse peak time interval sequence is longer than or equal to 3 seconds or if the detected pulse peak frequency of the pulse peak time interval sequence (i.e., the pulse frequency or heart rate) is lower than or equal to 50 times per minute.
[0078] The method of the present invention for detecting heart rhythm irregularities can be applied to and implemented by means of a detection device. Two preferred embodiments of such a detection device are disclosed below. The detection device of the present invention can be used in emergency rooms, intensive care units, hospital wards, and clinics, or as a personal or household daily health care device, to monitor a patient's or user's heart rhythm in real time.
[0079] V. Embodiment 5-Detection Device in the Form of a Smartwatch
[0080] Referring to FIG. 2 to FIG. 5, this embodiment discloses a smartwatch that doubles as a detection device 1 for implementing a method for detecting heart rhythm irregularities as disclosed in the foregoing embodiments 1 to 4.
[0081] The detection device 1 includes a detecting portion (not shown), a recording portion (not shown), a processor (not shown), and a display device 11. The detecting portion includes an inflatable bladder 12 as shown in FIG. 4), an air pressure pump 13, a pressure sensor 122, a pressure relief valve (not shown), and a microcontroller unit (not shown). The microcontroller unit is configured to control the operation of the motor in the air pressure pump 13 and of the pressure relief valve so that the bladder 12 can be inflated and deflated by the air pressure pump 13 through the air inlet 121 of the bladder 12. In this embodiment, the pressure sensor 122 is provided on the bladder 12.
[0082] The detection device 1 can be worn on a user's wrist, with the bladder 12 wrapped around the wrist, preferably with the bladder 12 lying compliantly on the inner side of the wrist (see FIG. 4) to provide higher sensitivity in measuring pressure variation in the radial artery.
[0083] The user may choose between an ambulatory monitoring mode, in which monitoring is carried out constantly, and a measure-as-you-need mode, in which monitoring begins as soon as the mode is chosen. FIG. 6 shows the pressure of the bladder 12 and the pulse signals detected by the detection device 1 (using the oscillometric method), both plotted against time. The graph in FIG. 6 shows how pulse peaks vary while the bladder is being slowly pressurized. When the detection device 1 starts monitoring, the detecting portion is gradually inflated (pressurized) to a fixed pressure such as 175 mmHg (or the value 500 in FIG. 6). Once the pressure is stable enough for the detection of pressure wave variation, the varying pressure pulse peaks are measured continuously over a predetermined period of time (e.g., 25 seconds).
[0084] That is to say, referring back to FIG. 1, the detection device 1 performs step a in embodiment 1, followed by step b, which determines whether an irregular pulse peak has occurred. If it is determined that an irregular pulse peak has occurred, step b-1 is performed to determine the degree of irregularity of the irregular pulse peak (e.g., IPP 15%, IPP 20%, or IPP 25%). The determination results of steps b and b-1 are displayed on the display device 11 (see FIG. 5(a)).
[0085] Then, with continued reference to FIG. 1, the detection device 1 performs: step c in embodiment 2 regardless of the results of steps b and b-1 in order to determine whether irregular heartbeat (IHB) has occurred; steps d to fin embodiment 3 regardless of the results of steps b, b-1, and c in order to determine whether atrial fibrillation (AF) has occurred; and step g in embodiment 4 regardless of results of steps b to f and b-1 in order to determine whether sick sinus syndrome has occurred. The determination results of steps c to g are displayed on the display device 11(see FIG. 5(b)).
[0086] When all the measurements are completed, the microcontroller unit opens the pressure relief valve to deflate the bladder 12. The inflation speed and deflation speed of the bladder 12 are controlled by the microcontroller unit.
[0087] According to the above, the method and device of the present invention for detecting heart rhythm irregularities can be used to detect irregular pulse peaks (IPP), irregular heartbeat (IHB), atrial fibrillation (AF), and sick sinus syndrome (SSS). Moreover, the method of the present invention can be applied to a sphygmomanometer that measures blood pressure by the oscillometric method or the auscultatory method, or a wearable device (e.g., a smartwatch) that measures blood pressure through an inflatable bladder, making it easier for one to measure their own blood pressure and thereby prevent medical conditions that may accompany heart rhythm irregularities, such as myocardial infarction (heart attack), hypertension, and angina. The present invention can be used in emergency rooms, intensive care units, hospital wards, and clinics or as a personal or household daily health care device and therefore has high utility value in the medical industry.
[0088] The above is the detailed description of the present invention. However, the above is merely the preferred embodiment of the present invention and cannot be the limitation to the implement scope of the present invention, which means the variation and modification according to the present invention may still fall into the scope of the invention.
* * * * *
uspto.report is an independent third-party trademark research tool that is not affiliated, endorsed, or sponsored by the United States Patent and Trademark Office (USPTO) or any other governmental organization. The information provided by uspto.report is based on publicly available data at the time of writing and is intended for informational purposes only.
While we strive to provide accurate and up-to-date information, we do not guarantee the accuracy, completeness, reliability, or suitability of the information displayed on this site. The use of this site is at your own risk. Any reliance you place on such information is therefore strictly at your own risk.
All official trademark data, including owner information, should be verified by visiting the official USPTO website at www.uspto.gov. This site is not intended to replace professional legal advice and should not be used as a substitute for consulting with a legal professional who is knowledgeable about trademark law.