Wound Care Method And System With One Or Both Of Vacuum-light Therapy And Thermally Augmented Oxygenation
QUISENBERRY; Tony
U.S. patent application number 16/659814 was filed with the patent office on 2020-02-13 for wound care method and system with one or both of vacuum-light therapy and thermally augmented oxygenation. This patent application is currently assigned to ThermoTek, Inc.. The applicant listed for this patent is ThermoTek, Inc.. Invention is credited to Tony QUISENBERRY.
| Application Number | 20200046569 16/659814 |
| Document ID | / |
| Family ID | 46966651 |
| Filed Date | 2020-02-13 |





View All Diagrams
| United States Patent Application | 20200046569 |
| Kind Code | A1 |
| QUISENBERRY; Tony | February 13, 2020 |
WOUND CARE METHOD AND SYSTEM WITH ONE OR BOTH OF VACUUM-LIGHT THERAPY AND THERMALLY AUGMENTED OXYGENATION
Abstract
A combination therapy pad that includes a first layer and a second layer operatively coupled to the first layer. A fiber-optic array is disposed between the first layer and the second layer. A third layer is operatively coupled to the first layer. The third layer includes a vacuum tube in fluid communication with a vacuum source and a therapeutic fluid tube in fluid communication with a therapeutic fluid source. The third layer provides at least one of vacuum therapy and therapeutic fluid treatment to a wound area.
| Inventors: | QUISENBERRY; Tony; (Highland Village, TX) | ||||||||||
| Applicant: |
|
||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Assignee: | ThermoTek, Inc. Flower Mound TX |
||||||||||
| Family ID: | 46966651 | ||||||||||
| Appl. No.: | 16/659814 | ||||||||||
| Filed: | October 22, 2019 |
Related U.S. Patent Documents
| Application Number | Filing Date | Patent Number | ||
|---|---|---|---|---|
| 15456147 | Mar 10, 2017 | 10507140 | ||
| 16659814 | ||||
| 14330449 | Jul 14, 2014 | 9616210 | ||
| 15456147 | ||||
| 13962994 | Aug 9, 2013 | 8940034 | ||
| 14330449 | ||||
| 13456410 | Apr 26, 2012 | 8574278 | ||
| 13962994 | ||||
| 13359210 | Jan 26, 2012 | 8632576 | ||
| 13456410 | ||||
| 11975047 | Oct 17, 2007 | 8128672 | ||
| 13359210 | ||||
| 11801662 | May 9, 2007 | 8100956 | ||
| 11975047 | ||||
| 61479156 | Apr 26, 2011 | |||
| 60852803 | Oct 19, 2006 | |||
| 60798982 | May 9, 2006 | |||
| Current U.S. Class: | 1/1 |
| Current CPC Class: | A61N 5/0616 20130101; A61F 7/0085 20130101; A61F 13/00068 20130101; A61N 2005/0661 20130101; A61F 13/00029 20130101; A61F 2007/0295 20130101; A61F 7/02 20130101; A61F 2013/00195 20130101; A61M 1/0023 20130101; A61F 2007/0296 20130101; A61N 2005/0651 20130101; A61N 2005/063 20130101; A61M 37/00 20130101; A61N 2005/0645 20130101; A61F 2013/0017 20130101; A61N 5/0613 20130101; A61N 2005/0652 20130101; A61M 2205/05 20130101; A61F 2007/0054 20130101; A61N 5/04 20130101; A61M 2205/051 20130101; A61N 2005/0649 20130101 |
| International Class: | A61F 13/00 20060101 A61F013/00; A61M 1/00 20060101 A61M001/00; A61N 5/06 20060101 A61N005/06; A61M 37/00 20060101 A61M037/00; A61F 7/00 20060101 A61F007/00; A61N 5/04 20060101 A61N005/04; A61F 7/02 20060101 A61F007/02 |
Claims
1. A method of treating a wound area, the method comprising: covering the wound area with a therapy pad, the therapy pad comprising: a first layer; a second layer operatively coupled to the first layer; a third layer operatively coupled to the first layer, the third layer having a vacuum tube in fluid communication with a vacuum source and a therapeutic fluid tube in fluid communication with a therapeutic fluid source, wherein the third layer provides at least one of vacuum therapy and therapeutic fluid treatment to a wound area; and administering at least one of oxygenation therapy and vacuum therapy to the wound area via the therapy pad.
2. The method of claim 1, wherein the administering of oxygenation therapy comprises delivering oxygen from an oxygen source to the wound area via the therapy pad.
3. The method of claim 2, wherein the administering oxygenation therapy comprises at least one of warming or cooling the oxygen via a thermoelectric element.
4. The method of claim 1, comprising administering a pulsed radio frequency signal to the wound area via a radio frequency antenna disposed within the therapy pad.
5. The method of claim 4, wherein the radio frequency antenna is disposed substantially around a perimeter of the wound area.
6. The method of claim 1, wherein the vacuum therapy and the oxygenation therapy are administered via a common port in the therapy pad.
Description
CROSS-REFERENCE TO RELATED APPLICATIONS
[0001] This patent application is a continuation of U.S. patent application Ser. No. 15/456,147, filed on Mar. 10, 2017. U.S. patent application Ser. No. 15/456,147 is a continuation of U.S. patent application Ser. No. 14/330,449, filed on Jul. 14, 2014. U.S. patent application Ser. No. 14/330,449 is a continuation of U.S. patent application Ser. No. 13/962,994, filed Aug. 9, 2013. U.S. patent application Ser. No. 13/962,994 is a continuation of U.S. patent application Ser. No. 13/456,410, filed on Apr. 26, 2012 (now U.S. Pat. No. 8,574,278). U.S. patent application Ser. No. 13/456,410 is a Continuation-in-Part of U.S. patent application Ser. No. 13/359,210, filed on Jan. 26, 2012 (now U.S. Pat. No. 8,632,576). U.S. patent application Ser. No. 13/359,210 is a Continuation-in-Part of U.S. patent application Ser. No. 11/975,047 (now U.S. Pat. No. 8,128,672), filed on Oct. 17, 2007. U.S. patent application Ser. No. 11/975,047 is a Continuation-in-Part of U.S. patent application Ser. No. 11/801,662 (now U.S. Pat. No. 8,100,956), filed on May 9, 2007. U.S. patent application Ser. No. 11/975,047 claims priority to, and incorporates by reference the entire disclosure of, U.S. Provisional Patent Application No. 60/852,803, filed on Oct. 19, 2006. U.S. patent application Ser. No. 11/801,662 (now U.S. Pat. No. 8,100,956) claims priority to, and incorporates by reference the entire disclosure of, U.S. Provisional Patent Application No. 60/798,982, filed on May 9, 2006. U.S. patent application Ser. No. 13/456,410 claims priority to, and incorporates by reference for any purpose, the entire disclosure of U.S. Provisional Patent Application No. 61/479,156, filed on Apr. 26, 2011. of U.S. patent application Ser. No. 15/456,147, U.S. patent application Ser. No. 13/456,410, U.S. patent application Ser. No. 13/359,210, U.S. patent application Ser. No. 11/975,047, U.S. patent application Ser. No. 11/801,662, U.S. Provisional Patent Application No. 60/852,803, U.S. Provisional Patent Application No. 60/798,982, and U.S. Provisional Patent Application No. 61/479,156 are each incorporated herein by reference.
[0002] This patent application is related to and incorporates by reference U.S. Provisional Patent Application No. 60/488,709, filed on Jul. 18, 2003; U.S. Provisional Patent Application No. 60/550,658 filed on Mar. 5, 2004; and U.S. patent application Ser. No. 10/894,369, filed on Jul. 19, 2004. This patent application incorporates by reference commonly assigned U.S. Pat. Nos. 5,097,829; 5,989,285, and 6,935,409.
BACKGROUND OF THE INVENTION
Technical Field
[0003] The present invention relates to a wound care method and system with one or both of vacuum-light therapy, pulsed radio frequency ("RF"), and thermally augmented oxygenation, and more particularly, but not by way of limitation, to a programmable wound care control unit configured to generate a negative pressure for wound cleaning with light therapy, and, in one embodiment, pulsed RF or oxygenation of a wound area for healing in conjunction with high thermal contrast modalities generated by the control unit.
Description of the Related Art
[0004] An important aspect of patient treatment is wound care. Medical facilities are constantly in need of advanced technology for the cleaning and treatment of skin wounds. The larger the skin wound, the more serious the issues are of wound closure and infection prevention. The rapidity of the migration over the wound of epithelial and subcutaneous tissue adjacent the wound is thus critical. Devices have been developed and/or technically described which address certain aspects of such wound healing. For example, U.S. Pat. No. 6,695,823 to Lina et al. ("Lina") describes a wound therapy device that facilitates wound closure. A vacuum pump is taught for collecting fluids from the wound. WO 93/09727 discloses a solution for wound drainage by utilizing negative pressure over the wound to promote the above references migration of epithelial and subcutaneous tissue over the wound.
[0005] In other embodiments, wound treatment is performed using light therapy. For example, U.S. Pat. No. 7,081,128 to Hart et al. ("Hart") describes a method of treating various medical conditions such as, for example, joint inflammation, edema, etc., utilizing an array of Light Emitting Diodes contained on a flexible substrate that may be wrapped around an anatomical feature of the human body. U.S. Pat. No. 6,596,016 to Vreman et al. ("Vreman") discloses a phototherapy garment for an infant having a flexible backing material, a transparent liner, and a flexible printed circuit sheet containing surface-mounted LEDs. The LEDs preferably emit high-intensity blue light, suitable for the treatment of neonatal hyperbilirubinemia. The device may include a portable power supply.
[0006] In other embodiments, wound treatment is performed using oxygen. The use of oxygen for the treatment of skin wounds has been determined to be very beneficial in certain medical instances. The advantages are multitudinous and include rapidity in healing. For this reason, systems have been designed for supplying high concentration of oxygen to wound sites to facilitate the healing process. For example, U.S. Pat. No. 5,578,022 to Scherson et al. ("Scherson") teaches an oxygen producing bandage and method. One of the benefits cited in Scherson is the ability to modulate a supply of concentrated hyperbaric oxygen to skin wounds. Although oxygen is beneficial in direct application of predetermined dosages to skin wounds, too much oxygen can be problematic. Oxygen applied to a wound site can induce the growth of blood vessels for stimulating the growth of new skin. Too much oxygen, however, can lead to toxic effects and the cessation of healing of the wound. It would be an advantage, therefore, to maximize the effectiveness of oxygen applied to a wound area by enhancing the absorption rate of oxygen into the skin and tissue fluids. By enhancing the absorption rate of the oxygen in the wound, less exposure time and concomitantly fewer toxic side effects to the endothelial cells surrounding the wound, such as devasculation, occurs. It would be a further advantage, therefore, to utilize existing medical treatment modalities directed toward other aspects of patient therapy to augment oxygenation for wound care.
[0007] It has been accepted for many years by medical care providers that patient thermal therapy can be very advantageous for certain injuries and/or post operative recovery. For this reason, thermal therapy has been advanced and many reliable and efficient systems exist today which provide localized thermal therapy to patients in both pre and post surgical environments. In particular, absorption of oxygen by cells is enhanced by contrast thermal therapy wherein the wound area is heated prior to being saturated with oxygen and subsequently cooled.
[0008] Addressing first thermal therapy systems, several devices have been engineered to deliver temperature controlled fluids through pads or convective thermal blankets to achieve the above purpose. Typically, these devices have a heating or a cooling element, a source for the fluid, a pump for forcing the fluid through the pad or blanket, and a thermal interface between the patient and the temperature controlled fluid. U.S. Pat. No. 4,884,304 to Elkins ("Elkins") is, for example, directed to a mattress cover device which contains liquid flow channels which provide the selective heating or cooling by conduction.
[0009] Devices have also been developed for simply providing heat or cooling to a person in bed. Electric blankets containing electric heating elements have been used, for example, to provide heat to people in bed. Likewise, cooling blankets, such as the blanket disclosed in U.S. Pat. No. 4,660,388 to Greene ("Greene"), have also been proposed. Greene discloses a cooling cover having an inflatable pad with plenum chambers at opposite ends thereof. Cool air is generated in a separate unit and directed to the pad and out to a number of apertures on the underside of the pad and against the body of the person using the cover.
[0010] A disposable heating or cooling blanket is disclosed in U.S. Pat. No. 5,125,238 to Ragan et al. ("Ragan"), which has three layers of flexible sheeting. Two of the layers form an air chamber while a third layer includes a comfortable layer for contact with the patient. Conditioned air is directed toward the covered person through a multiplicity of orifices in the bottom layers of the blanket.
[0011] A temperature controlled blanket and bedding assembly is also disclosed in U.S. Pat. No. 5,989,285 to DeVilbiss et al. ("DeVilbiss"), assigned to the assignee of the present invention. DeVilbiss discloses a temperature controlled blanket and temperature control bedding system having the provision of both recirculating temperature controlled fluid and temperature controlled gas to enhance performance for convectively heating or cooling a patient. Counter-flow or co-flow heat exchanging principles between the temperature controlled liquid and the temperature controlled gas achieve temperature uniformity across different sections of the blanket and the bedding system. Drapes and the temperature controlled bedding system provide a temperature controlled envelope around a person using the bedding system. In one embodiment of the bedding system, the air portion of the bedding system is provided for use with a patient that supplies the fluid portion of the overall bedding system. In another embodiment of the bedding system, the fluid portion of the bedding system is provided for use with a patient bed which supplies the air portion of the overall bedding system.
[0012] U.S. Pat. No. 5,097,829 to Quisenberry ("Quisenberry") describes an improved temperature controlled fluid circulating system for automatically cooling a temperature controlled fluid in a thermal blanket with a thermoelectric cooling device having a cold side and a hot side when powered by electricity. The temperature controlled fluid is cooled by the cold side of the cooling device and pumped through, to, and from the blanket through first and second conduits.
[0013] Finally, co-pending U.S. patent application Ser. No. 10/894,369, assigned to the assignee of the present invention, teaches a sequential compression blanket for use with heating or cooling therapy. In this particular embodiment, the utilization of thermal therapy with sequential compression in a programmable format which further has the option of the introduction of oxygenation through a perforated membrane disposed between the patient and the thermal therapy pad is taught. These advances in the medical industry have been recognized as advantageous to both the medical care providers as well as the patients. The precise manner of oxygenation application is, however, still in the process of development.
[0014] The present invention provides improvements in wound care by providing multiple wound healing approaches such as, for example, the application of negative pressure over the wound area along with light therapy of the wound area, and oxygenation of the wound area in conjunction with thermal therapy. By combining an oxygenation modality that is utilized in conjunction with light and thermal therapy and/or sequential compression in association therewith, the individual benefits of negative wound pressure, light therapy, and oxygenation treatments can be synergistically enhanced.
SUMMARY
[0015] In one aspect, the present invention relates to a therapy system. The therapy system includes a therapy pad having a plurality of fiber-optic strands and a port. A pressure switch is fluidly coupled to the port. An oxygen source is fluidly coupled to the pressure switch. A vacuum pump is fluidly coupled to the pressure switch. A plurality of light emitting diodes is operationally coupled to the plurality of fiber-optic strands. The pressure switch adjusts the therapy pad between vacuum and oxygenation therapy.
[0016] In another aspect, the present invention relates to a therapy pad. The therapy pad includes an outer surface and an inner surface. A bladder is disposed between the outer surface and the inner surface. An array of fiber optic strands is disposed on the inner surface. An inlet is disposed on the outer surface. The inlet is fluidly coupled to a plurality of ports disposed on the inner surface. A radio frequency antenna is disposed on the inner surface.
[0017] In another aspect, the present invention relates to a method of treating a wound area. The method includes dressing the wound area with a therapy pad and administering at least one of ultra-violet light and vacuum therapy to the wound area via the therapy pad. In various embodiments, the method may also include administering oxygenation therapy to a wound area via the therapy pad, administering thermal therapy to the wound area via the therapy pad, and administering a pulsed radio frequency signal to the wound area via a radio frequency antenna disposed within the therapy pad.
[0018] A combination therapy pad that includes a first layer and a second layer operatively coupled to the first layer. A fiber-optic array is disposed between the first layer and the second layer. A third layer is operatively coupled to the first layer. The third layer includes a vacuum tube in fluid communication with a vacuum source and a therapeutic fluid tube in fluid communication with a therapeutic fluid source. The third layer provides at least one of vacuum therapy and therapeutic fluid treatment to a wound area.
[0019] A therapy system that includes a combination therapy pad having a plurality of fiber-optic strands and a port. A pressure switch is fluidly coupled to the port. An oxygen source and a vacuum pump are fluidly coupled to the pressure switch. A plurality of light emitting diodes are optically coupled to the plurality of fiber-optic strands. A thermoelectric element is thermally exposed to the oxygen source. The combination therapy pad administers at least one of vacuum therapy and oxygenation therapy via the pressure switch.
[0020] A method of treating a wound area. The method includes covering the wound area with a therapy pad, the therapy pad having a first layer, a second layer operatively coupled to the first layer, a fiber-optic array disposed between the first layer and the second layer, and a third layer operatively coupled to the first layer. The third layer includes a vacuum tube in fluid communication with a vacuum source and a therapeutic fluid tube in fluid communication with a therapeutic fluid source. The third layer provides at least one of vacuum therapy and therapeutic fluid treatment to a wound area. The method further includes administering at least one of ultra-violet light therapy and vacuum therapy to the wound area via the therapy pad and administering at least one of oxygenation therapy and thermal therapy to the wound area via the therapy pad.
BRIEF DESCRIPTION OF THE DRAWINGS
[0021] A more complete understanding of the method and apparatus of the present invention may be obtained by reference to the following Detailed Description when taken in conjunction with the accompanying Drawings wherein:
[0022] FIG. 1 is an illustration of the wound care system according to an exemplary embodiment;
[0023] FIG. 2 is a block diagram according to an exemplary embodiment;
[0024] FIG. 3 is a flow diagram of a process according to an exemplary embodiment;
[0025] FIG. 4 illustrates a side elevational cross sectional view of a therapy blanket/pad according to an exemplary embodiment;
[0026] FIG. 5 illustrates a side elevational cross sectional view of a therapy blanket/pad according to an exemplary embodiment;
[0027] FIG. 6 is a diagrammatic illustration of a therapy blanket/pad according to an exemplary embodiment;
[0028] FIG. 7 is a diagrammatic illustration of a wound evacuation and UV LED treatment pad according to an exemplary embodiment;
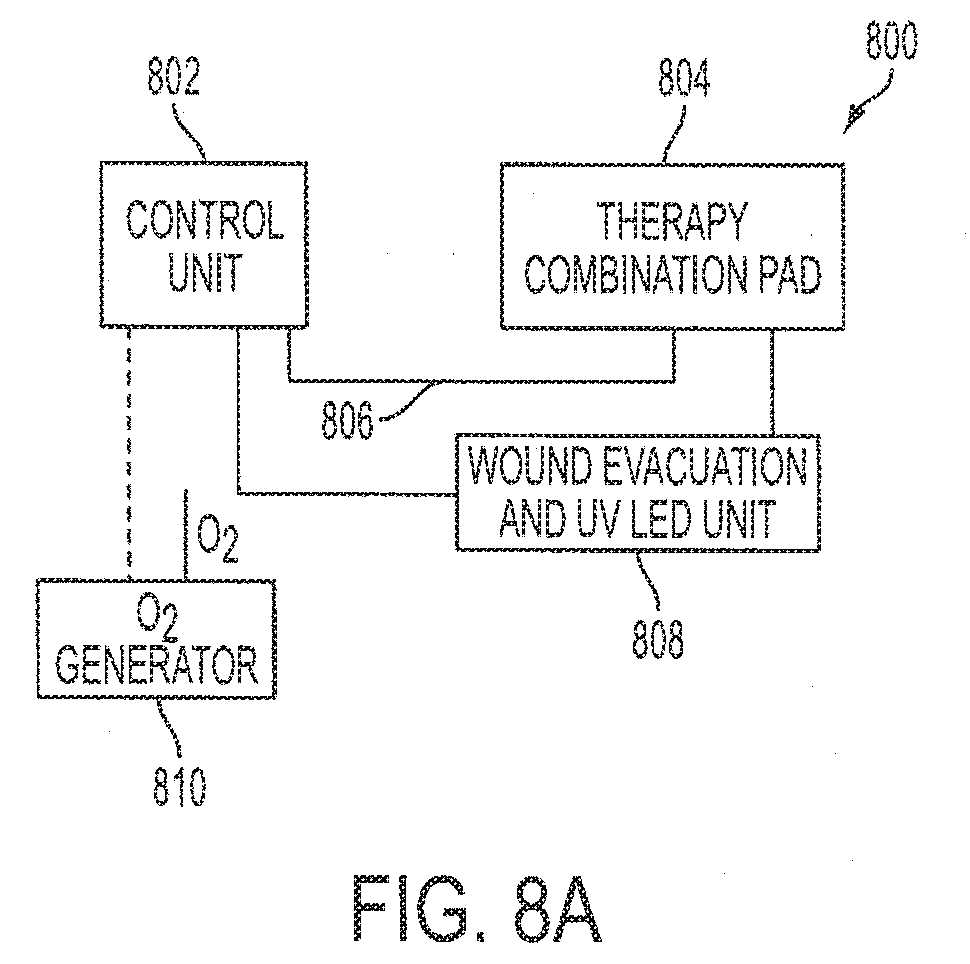
[0029] FIG. 8A is a schematic diagram of a wound care system according to an exemplary embodiment;
[0030] FIG. 8B is a front perspective view of a wound care system according to an exemplary embodiment;
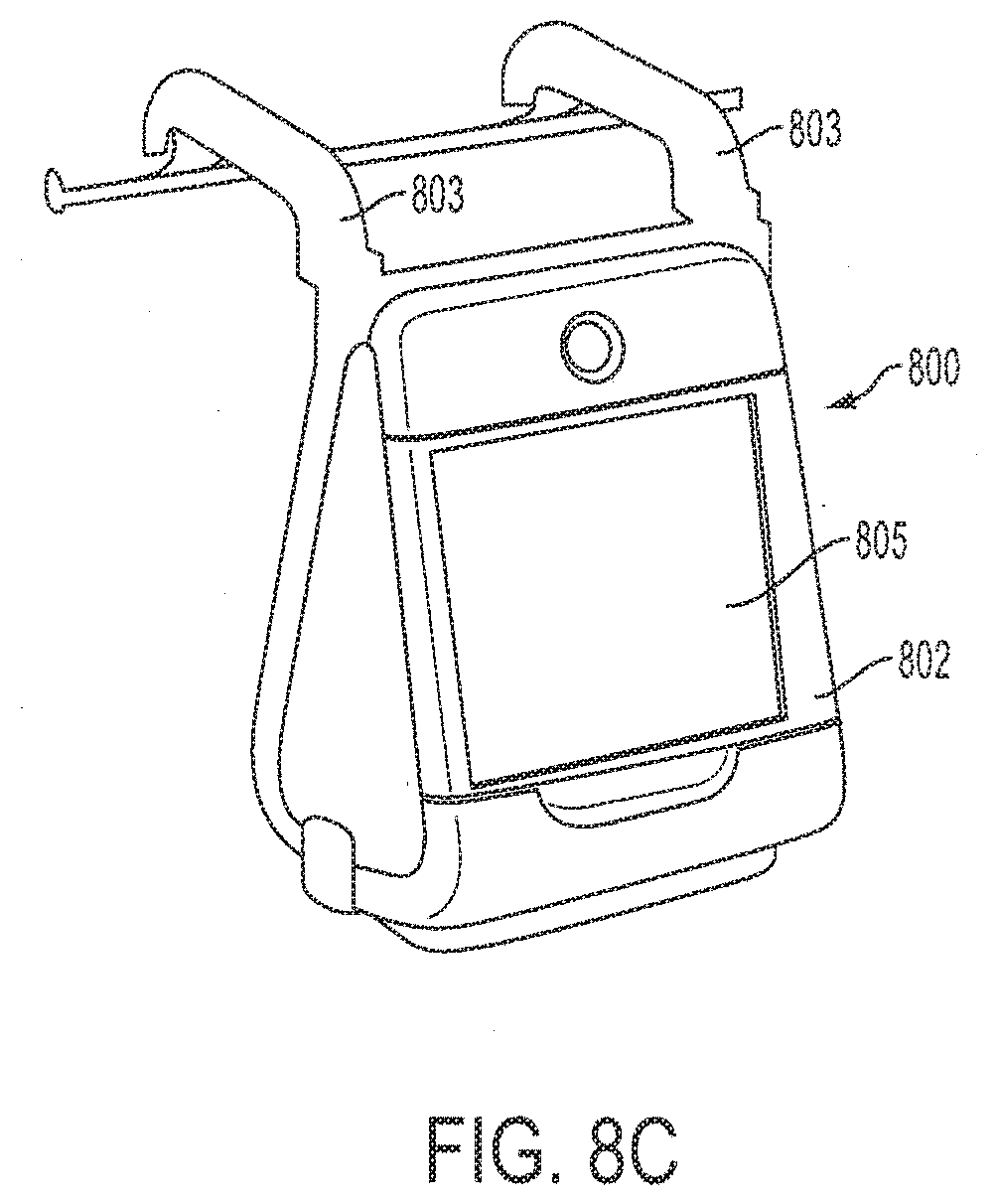
[0031] FIG. 8C is a front perspective view of a wound care system illustrating a plurality of hooks according to an exemplary embodiment;
[0032] FIG. 9 is a is a block diagram of a wound care system according to an exemplary embodiment;
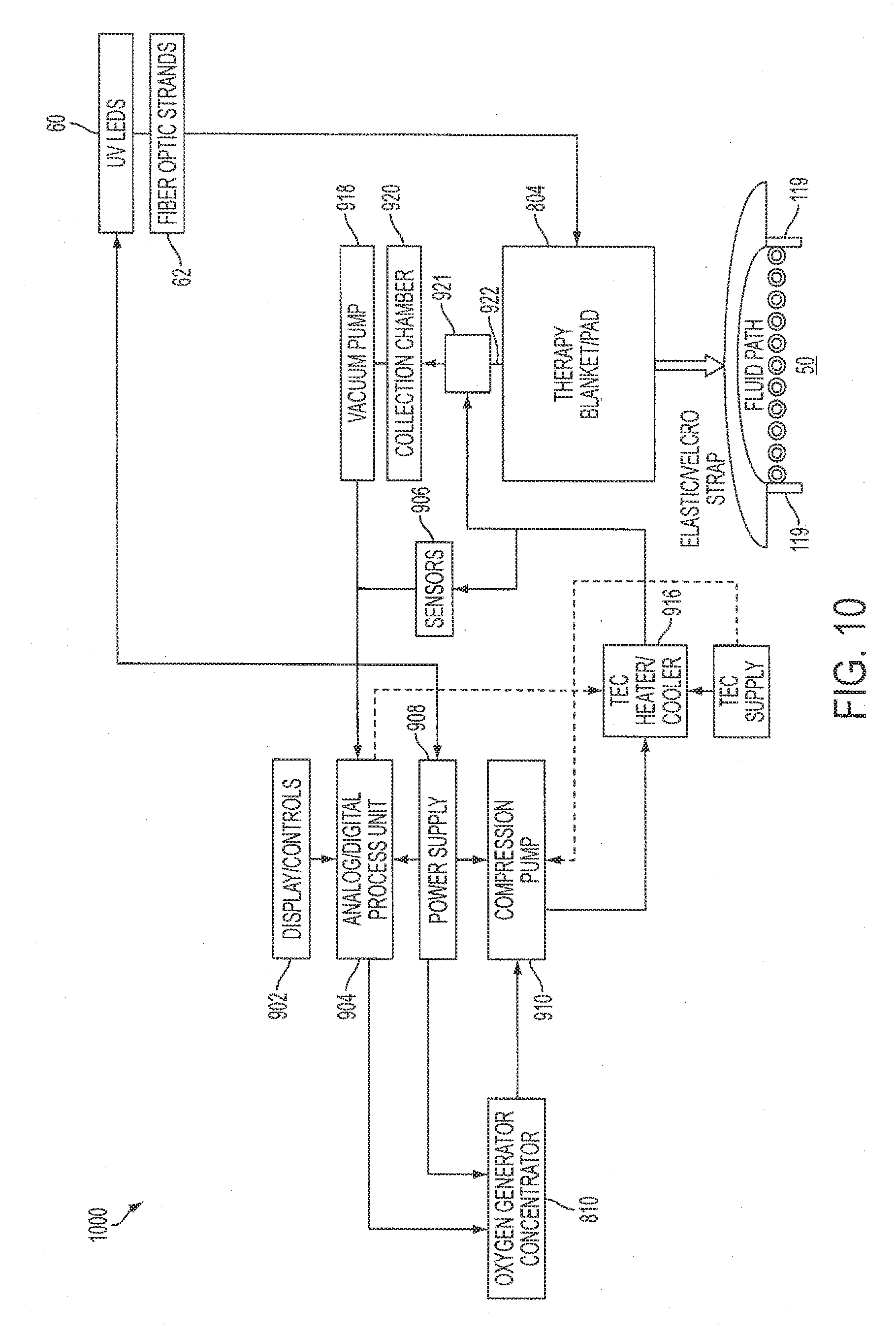
[0033] FIG. 10 is a block diagram of a wound care system according to an exemplary embodiment;
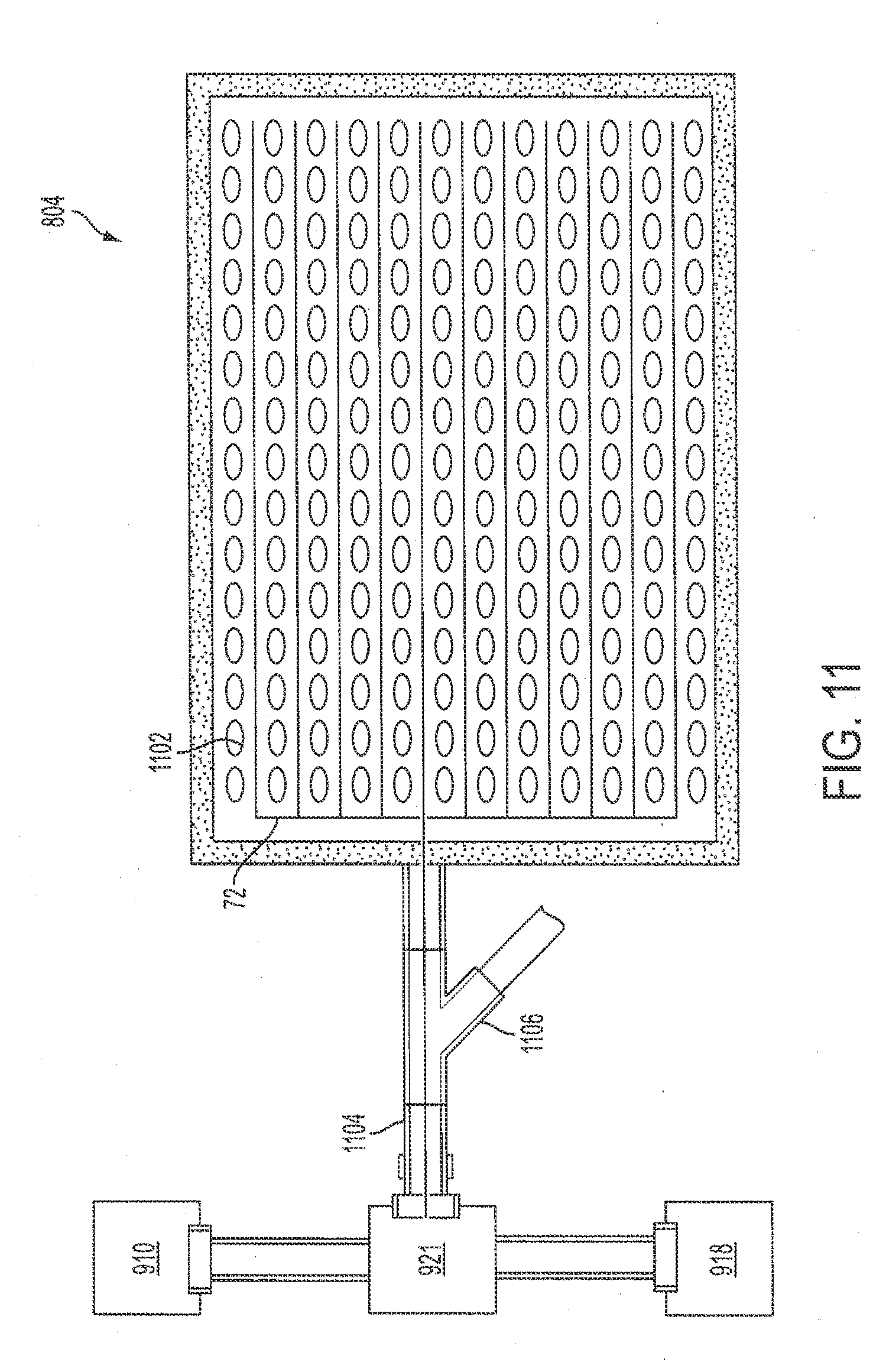
[0034] FIG. 11 is a diagrammatic illustration of a combination therapy pad according to an exemplary embodiment;
[0035] FIG. 12 is a diagrammatic illustration of a combination therapy pad according to an exemplary embodiment; and
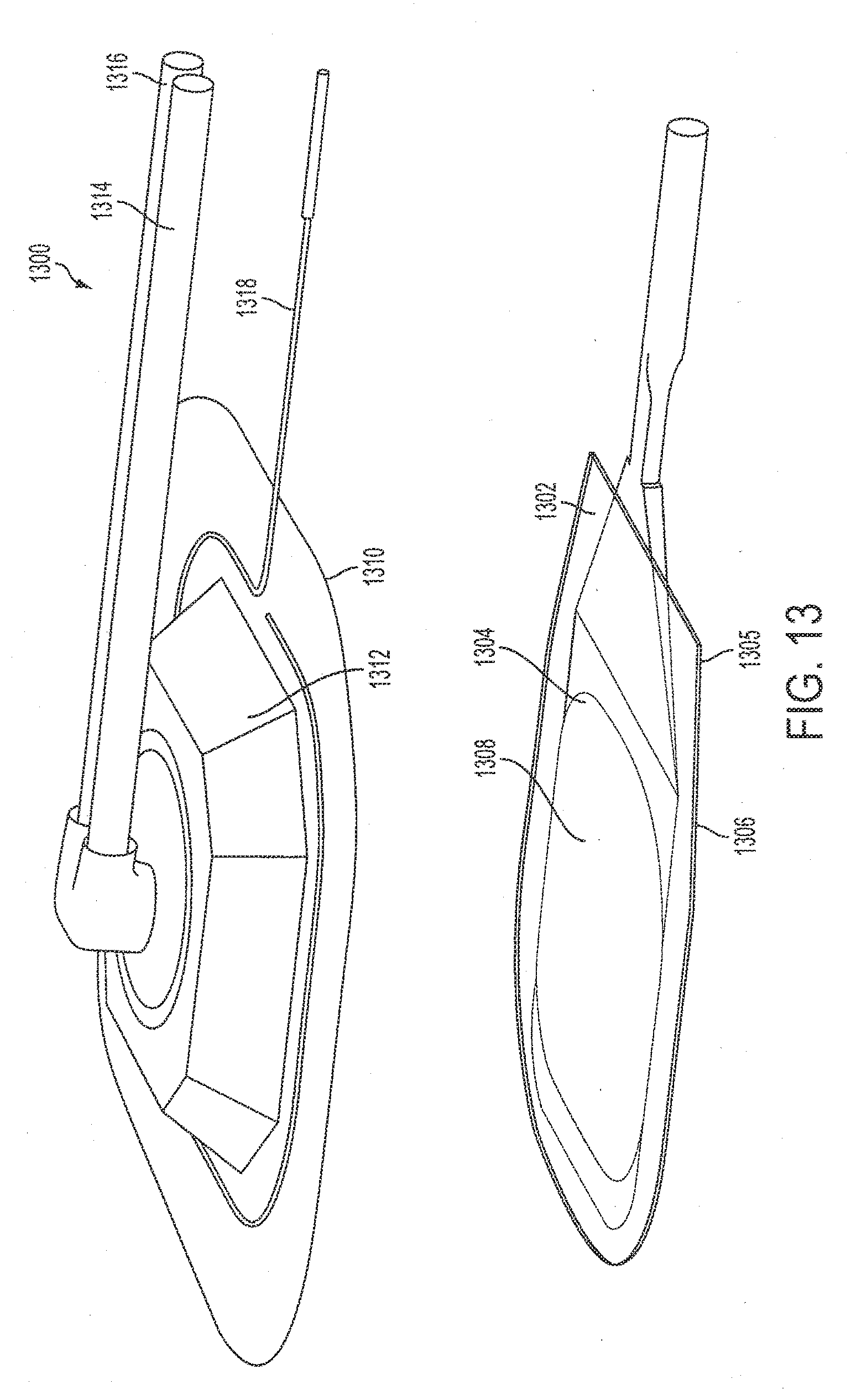
[0036] FIG. 13 is an exploded view of a combination therapy pad according to an exemplary embodiment.
DETAILED DESCRIPTION
[0037] Various embodiments of the present invention will now be described more fully with reference to the accompanying drawings. The invention may, however, be embodied in many different forms and should not be construed as limited to the embodiments set forth herein; rather, the embodiments are provided so that this disclosure will be thorough and complete, and will fully convey the scope of the invention to those skilled in the art.
[0038] Referring first to FIG. 1, there is shown an illustration of one embodiment of a wound care system 10 in accordance with principles of the present invention. The system 10 comprises a control unit 12, a therapy blanket/pad 14 and a plurality of tubular members 16 (to be defined below) connecting the control unit 12 to the therapy blanket/pad 14. The system 10 further includes a wound evacuation and ultra violet light emitting diode (UV LED) unit 28 and a wound evacuation and UV LED treatment pad 58. The wound evacuation and UV LED unit 28 is connected to the control unit 12 while the wound evacuation and UV LED treatment pad 58 is connected to the wound evacuation and UV LED unit 28. A system for providing both oxygenation therapy in conjunction with certain aspects of thermal therapy and fully describing the thermal operation and sequence compression aspects of one embodiment of the present invention is set forth and shown in U.S. patent application Ser. No. 10/894,369, assigned to the assignee of the present invention and incorporated herein in its entirety by reference. For that reason, thermal detail relative to the interaction between the control unit 12 and the therapy blanket/pad 14 relative to the thermal fluid flow and pressurization for sequenced compression therapy is not further defined herein. What is defined, is the added aspect of wound care provided by wound evacuation and light therapy. Light therapy is the application of light energy to the skin for therapeutic benefits. LED light therapy promotes wound healing and human tissue growth. Energy delivered by the LEDs enhances cellular metabolism, accelerates the repair and replenishment of damaged skin cells, as well as stimulates the production of collagen which is the foundation of a healthy and smooth skin. Light therapy is non-ablative, non-invasive, and painless.
[0039] Still referring to FIG. 1, the use of the therapy blanket/pad 14 to the wound site of the patient may be, in one embodiment, subsequent to the cleaning of the wound area of dead tissue by the wound evacuation and UV LED treatment pad 58. In one embodiment, Velcro cross straps may be utilized to secure the therapy blanket/pad 14. A 93% concentration of oxygen has been suggested to be advantageous when applied to a wound site as described herein with one or two atmospheres of pressure. In accordance with one aspect of the present invention, an oxygen generator/concentrator 20 may be utilized within the control unit 12 or may be separate therefrom. In FIG. 1, an oxygen generator/concentrator 20 is shown in association with the control unit 12 by dotted line 22 and an oxygenation gas line 24 shown extending between the control unit 12 and the therapy blanket/pad 14 as a diagrammatic illustration according to an embodiment of the present invention.
[0040] In FIG. 1, fiber optic strands (not explicitly shown) direct ultraviolet light from a plurality of LEDs (not explicitly shown) to an array of fiber optic strand ends (not explicitly shown) located on the undersurface of wound evacuation and UV LED treatment pad 58. The control unit 12 may be used to modulate the ultraviolet light to create various patterns of light, different intensities of light, and different durations of light. For example, the control unit 12 may be used to generate pulsed emission of ultraviolet light. The ultraviolet light is capable of penetrating through several layers of skin to destroy infectious bacteria. In one embodiment, not specifically shown herein, the UV LED treatment pad 58 may be provided on the therapy blanket/pad 14. According to exemplary embodiments, the ultraviolet light from the plurality of LEDs located on the undersurface of wound evacuation and UV LED treatment pad 58 destroys a wide variety of microorganisms such as, for example, bacteria which causes skin infections. In addition, the ultraviolet light from the plurality of LEDs improves wound healing along with cell and bone growth. Furthermore, the use of LEDs in light therapy is safe, non-invasive, drug-free and therapeutic.
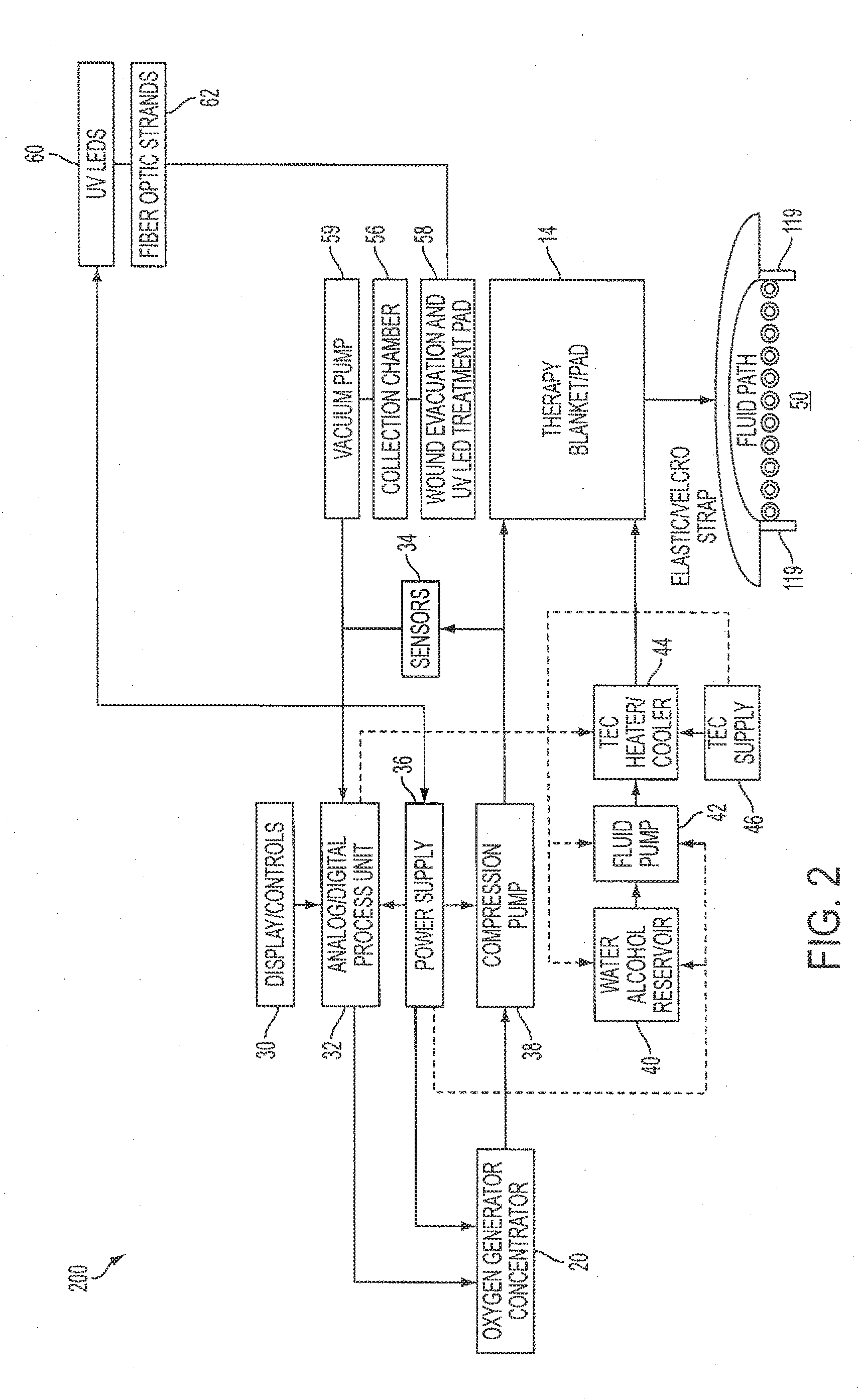
[0041] Referring now to FIG. 2, there is a block diagram 200 illustrating the flow of oxygenation gas as a transfer fluid according to an embodiment of the present invention. As set forth in the block diagram 200, a control unit display 30 is provided in conjunction with an analog/digital processing unit 32. A plurality of sensors 34 are utilized in conjunction with the processing unit 32 for control of heat transfer fluids to the therapy blanket/pad 14 as well as the oxygen delivery thereto. The oxygen generator/concentrator 20 is connected to a power supply 36, which power supply 36, also powers the processing unit 32. The oxygen generated from the oxygen generator/concentrator 20 is then pumped through compression pump 38 before delivery to the therapy blanket/pad 14. It should be noted that an oxygen supply may also be used.
[0042] Referring still to FIG. 2, a water/alcohol reservoir 40 is shown in fluid flow communication with fluid pump 42 and Thermo Electric Cooler (TEC) heater/cooler 44. The TEC heater/cooler 44 is controlled by the processing unit 32 and a TEC supply 46 is likewise shown. Adjacent the TEC supply 46 is illustrated a diagrammatical schematic of a treatment chamber 50 defined beneath the therapy blanket/pad 14 wherein the treatment chamber 50 is thermally exposed to the thermal fluid by the fluid path therein illustrated. The adhesive attachment edges 52 therein shown likewise define the treatment chamber space 50 between the therapy blanket/pad 14 and the wound site to allow for the flow of the oxygenation gas therein.
[0043] Referring still to FIG. 2, there is shown a vacuum pump 59 powered by the power supply 36. A collection chamber 56 is connected to the vacuum pump 59 and to a wound evacuation and UV LED treatment pad 58. The wound evacuation and UV LED treatment pad 58 is used prior to the therapy blanket/pad 14, in one embodiment of the present invention, for cleaning the wound area in preparation for oxygenation in conjunction with thermal therapy in accordance with the present invention.
[0044] Referring still to FIG. 2, there is shown a plurality of ultraviolet LEDs 60 and fiber optic strands 62, which are interoperably connected to the wound evacuation and UV LED treatment pad 58. The wound evacuation and UV LED treatment pad 58 is used prior to the therapy blanket/pad 14, in one embodiment of the present invention, for removing bacteria from the wound area in preparation for oxygenation in conjunction with thermal therapy in accordance with an embodiment. According to exemplary embodiments, ultraviolet light from the plurality of LEDs 60 destroys a wide variety of microorganisms such as, for example, bacteria which causes skin infections. In addition, the ultraviolet light from the plurality of LEDs 60 improves wound healing along with cell and bone growth. Furthermore, the use of the plurality of LEDs 60 in light therapy is safe, non-invasive, drug-free and therapeutic.
[0045] According to exemplary embodiments, the ultraviolet light from the plurality of LEDs 60 is in the range of approximately 200 to 450 nanometers and higher, and energy levels of up to 35,000 microwatt seconds/cm.sup.2, which are necessary to eliminate or destroy most microorganisms such as bacteria, spores, algae and viruses. Most bacteria can be destroyed at ultra violet energies of from about 3,000 to about 5,000 microwatt-seconds/cm.sup.2 while mold spores may require energies in the 20,000 to 35,000 mW-seconds/cm.sup.2.
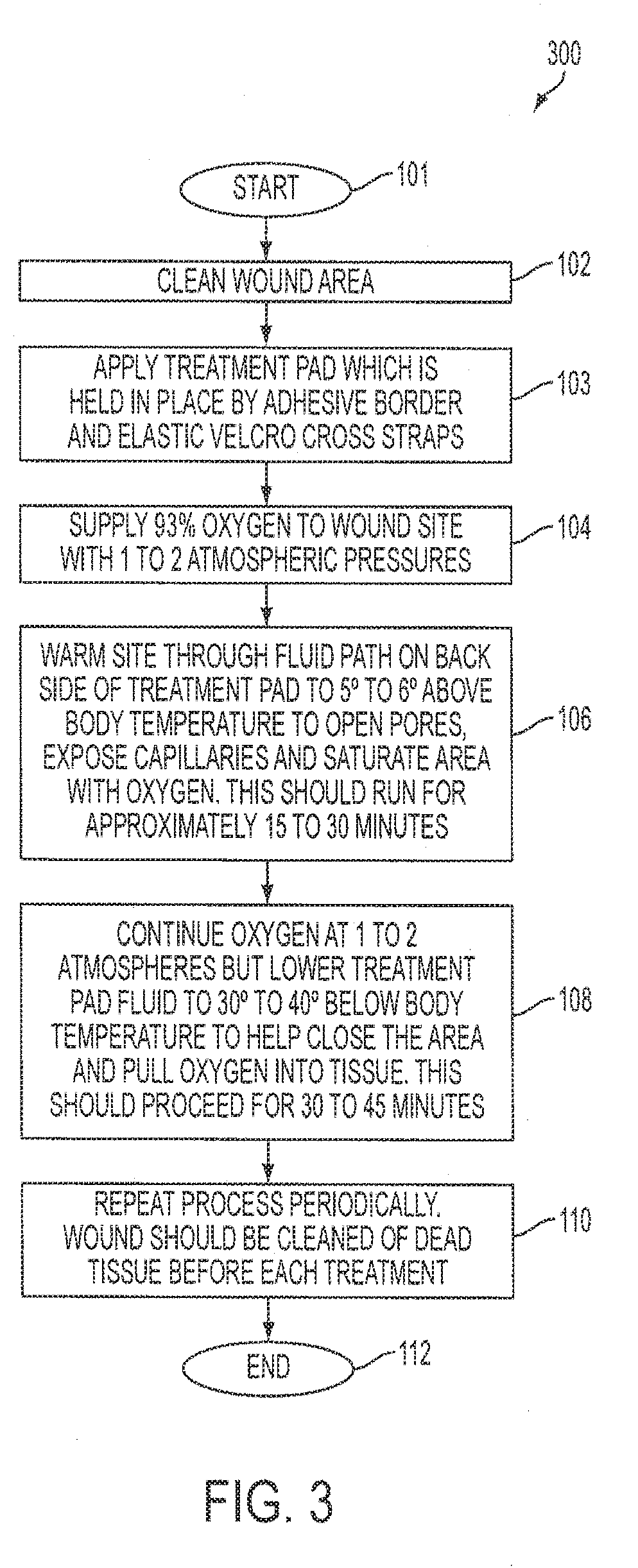
[0046] Referring now to FIG. 3 there is shown a flow diagram of a process 300 according to an embodiment. The process 300 starts at step 101. At step 102, the wound area is cleaned of dead tissue, any undesirable fluids, and bacteria by applying the wound evacuation and UV LED treatment pad 58. The wound evacuation and UV LED treatment pad 58 is used prior to the therapy blanket/pad 14 for removing bacteria from the wound area in preparation for oxygenation in conjunction with thermal therapy in accordance with the present invention. According to exemplary embodiments, the ultraviolet light from the plurality of LEDs located on the undersurface of wound evacuation and UV LED treatment pad 58 destroys a wide variety of microorganisms such as, for example, bacteria which causes skin infections. In addition, the ultraviolet light from the plurality of LEDs improves wound healing along with cell and bone growth. Furthermore, the use of LEDs in light therapy is safe, non-invasive, drug-free and therapeutic.
[0047] At step 103, the therapy blanket/pad 14 is applied to the wound area. The therapy blanket/pad 14 is held in position by an adhesive border and, in one embodiment, elastic Velcro cross straps. At step 104, according to an embodiment, an oxygenation gas comprising on the order of 93% concentration of oxygen gas is delivered to the wound site with one to two atmospheric pressures. The numbers as set forth and shown are exemplary and other oxygenation concentrations as well as pressures are contemplated in various embodiments. Consistent therewith, however, is the concept of, and teachings for, thermal treatment of the wound site in conjunction with oxygenation. In step 106, the site is warmed through the fluid path herein shown on the back side of the therapy blanket/pad 14 up to approximately 5 to approximately 6 degrees above the body temperature of the patient. Warming allows the pores of the patient's skin to open, exposing capillaries therein. The capillaries of the skin are then saturated with oxygen. In one period of time herein described, a warming period of approximately 15 to approximately 30 minutes is recommended. At step 108, oxygenation is continued at one to two atmospheres and the therapy blanket/pad fluid is lowered to approximately 30 to approximately 40 degrees below body temperatures. Cooling closes the pores of the wound area and pulls oxygen into the underlying tissue. Cooling then proceeds for approximately 30 to approximately 45 minutes in accordance with an embodiment. At step 110, the process 300 may be repeated periodically and the wound area may be cleaned of dead tissue before each treatment. At step 112, the process 300 ends.
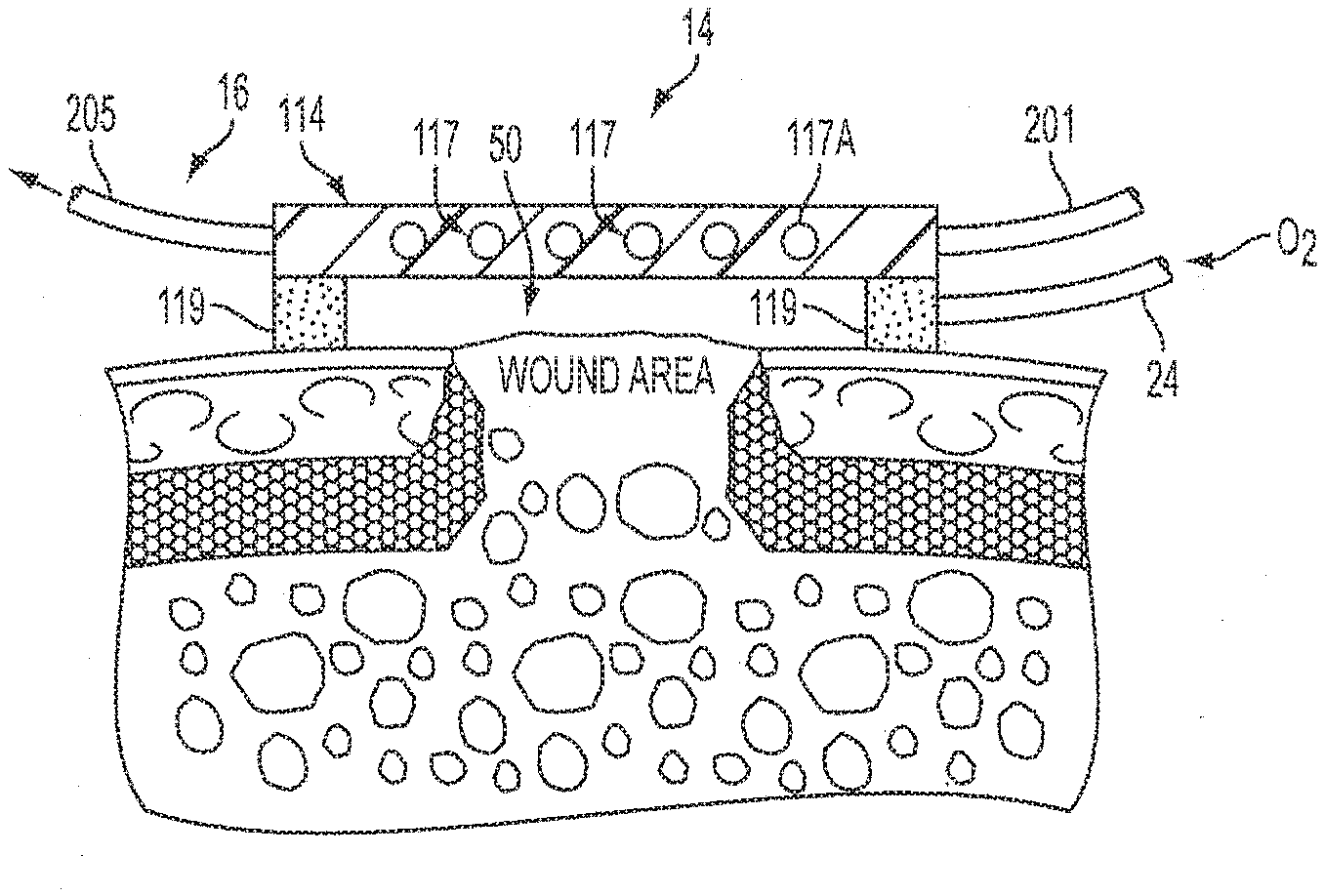
[0048] FIG. 4 is a side elevational, cross sectional view of one embodiment of the therapy blanket/pad 14. In an embodiment, the therapy blanket/pad 14 is constructed with a single bladder 114 where thermal fluid flow may be provided. The tubular members 16 are coupled to the therapy blanket/pad 14. The therapy blanket/pad is fabricated with a circuitous flow path therein for thermal fluid flow. The circuitous flow path may be tubular in form, or simply a path within therapy blanket/pad 14 defined by flow channels. What is shown is a path 117 within therapy blanket/pad 14. The path 117 is shown with tubular ends 117A, for example, illustrating that thermal fluid flows therein for thermal treatment of the underlying wound area. Again, the path 117 may not be of tubular form and may have a variety of shapes and fabrication techniques well know in the art of thermal pads.
[0049] According to an exemplary embodiment, the therapy blanket/pad 14 is separated from the patient's skin by adhesive strips 119 having a thickness of, for example, 1/8 inch. The therapy blanket/pad 14 (not drawn to scale) exposes the wound to both heat and cold via the path 117 while oxygen is injected into the treatment chamber 50. The injection of oxygen in conjunction with the aforesaid heating and cooling via the path 117 helps treat the wound area and any stasis zones therein where tissue swelling has restricted flow of blood to tissues within the wound area. It is well known that, without sufficient blood flow, the epithelial and subcutaneous tissues referenced above receive less oxygen and are less able to migrate over the wound area to promote healing. By utilizing the embodiments disclosed herein, oxygenation is enhanced and the problems associated with such conditions are mitigated.
[0050] FIG. 5 illustrates an exemplary embodiment of the thermal therapy and oxygenation treatment pad of FIG. 4. A dual bladder 214 is thus provided where air may be applied to second bladder 207 atop the path 117, also represented by the "tubular" ends 117A shown for purposes of example only. In this manner, select compression therapy may be afforded in conjunction with the thermal and oxygenation treatment. In that regard, air inlet tube 201 is connected to the second bladder 207. Both FIGS. 4 and 5 show oxygen tube 24 for feeding oxygen to the treatment chamber 50, with tube 203 allowing thermal fluid into conduits 117 with tube 205 allowing thermal fluid return to control unit 12 of FIG. 1. FIG. 5 further illustrates the advantages of FIG. 4 with the ability for either compression or sequenced compression as referenced above.
[0051] Referring now to FIG. 6, there is shown a diagrammatic illustration of the therapy blanket/pad 14 of FIGS. 1 and 4. The tubular members 16 for thermal fluid flow and the tube 24 for oxygen flow are clearly seen. The adhesive border 119 is likewise shown.
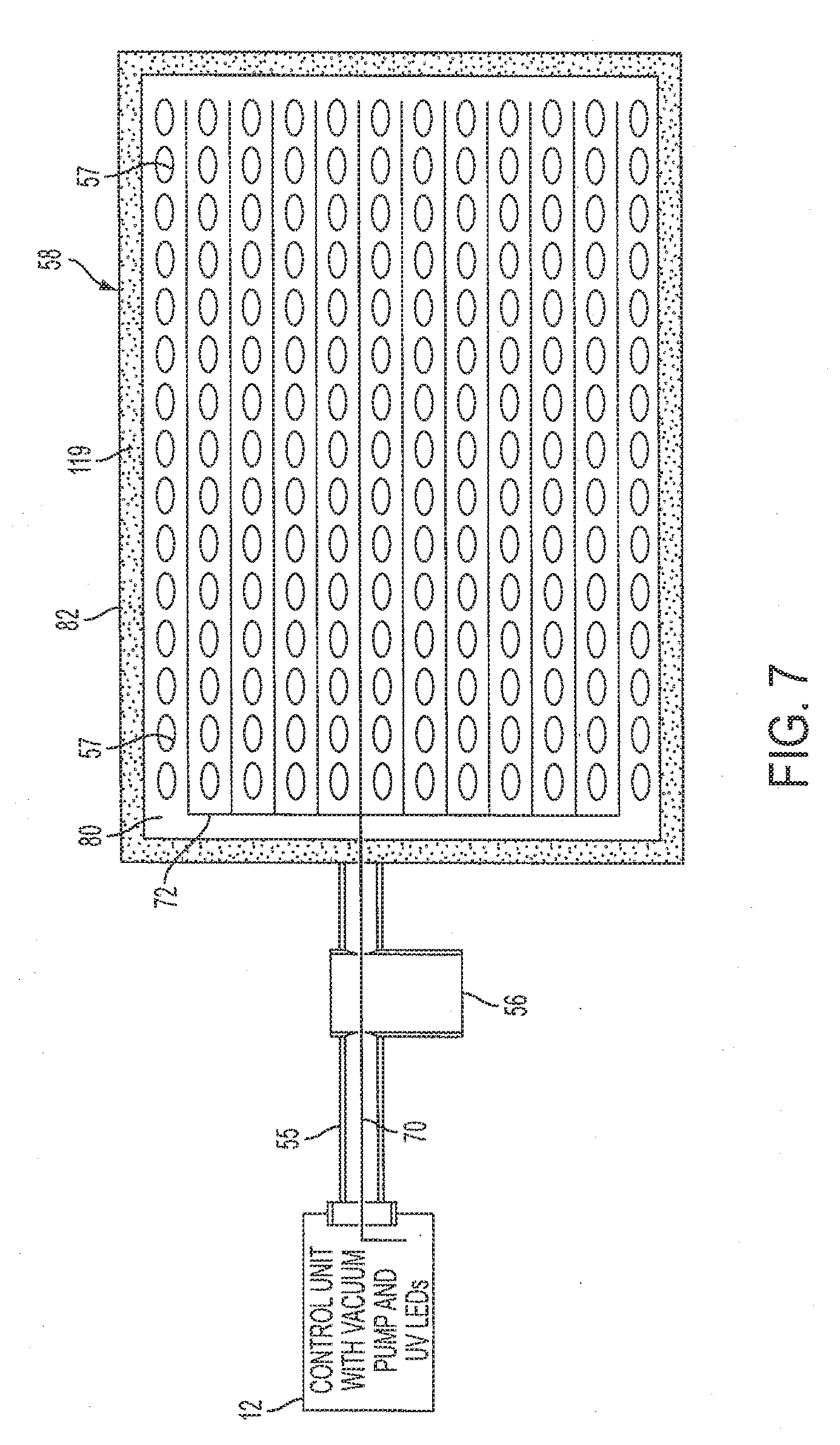
[0052] FIG. 7 is diagrammatic illustration of a wound evacuation and UV LED treatment pad 58 according to an embodiment of the present invention. In this embodiment, the wound evacuation and UV LED treatment pad 58 contains an array of fiber optic strand 72 to project ultraviolet light onto a wound area (not explicitly shown). In a typical embodiment, the fiber optic strands 72 may be cleaved side emitting fibers. The wound evacuation and UV LED treatment pad 58 also contains an array of unique removal ports 57 that may be used to remove any undesirable fluid from the wound area. The wound evacuation and UV LED treatment pad 58 further contains a non-tissue adhesive service 80 which contains both the fiber optic strand array 72 and the unique removal ports 57. An adhesive circumference 82 is located around the periphery of the wound evacuation and UV LED treatment pad 58 to allow for a seal to be formed around the wound area. The seal, in conjunction with the removal ports 57, allows a negative pressure to form over the wound area. Negative pressure facilitates removal undesirable tissues from the wound area. The wound evacuation and UV LED treatment pad 58 is connected to a control unit 12. The control unit 12 contains a vacuum pump (not shown) and a plurality of ultraviolet LEDs (not explicitly shown). The vacuum pump is connected to the wound evacuation and UV LED treatment pad 58 via a vacuum line 55. A collection chamber 56 is positioned between the vacuum pump and the wound evacuation and UV LED treatment pad 58 to intercept and store undesirable fluids, tissues, and the like that are removed from the wound area as a result of negative pressure applied to the wound area with the vacuum pump. The plurality of ultraviolet LEDs transmit ultraviolet light through the fiber optic strands 70 to the wound evacuation and UV LED treatment pad 58, where the fiber optic strands 70 are then dispersed throughout the wound evacuation and UV LED treatment pad 58 to project ultraviolet light onto the wound area. Energy delivered by the plurality of LEDs enhances cellular metabolism, accelerates repair and replenishment of damaged skin cells, as well as stimulates production of collagen which is the foundation of a healthy and smooth skin. Light therapy is non-ablative, non-invasive, and painless.
[0053] FIG. 8A is a schematic diagram of a wound care system according to an exemplary embodiment. A wound care system 800 includes a control unit 802, a combination therapy pad 804, and a plurality of tubular members 806 connecting the combination therapy pad 804 to the control unit 802. A wound evacuation and UV-LED unit 808 is associated with the control unit 802 and connected to the combination therapy pad 804. In various embodiments, the wound evacuation and UV-LED unit 808 and the control unit 802 are contained in a single housing; however, in various alternative embodiments, the wound evacuation and UV-LED unit 808 and the control unit 802 may not be in a single housing and are independent devices.
[0054] Still referring to FIG. 8A, use of the combination therapy pad 804 incorporates ultraviolet light and evacuation therapy for wound cleaning with thermal and oxygenation therapy known to promote healing. In various embodiments, Velcro cross straps are used to secure the combination therapy pad 804. An oxygen generator/concentrator 810 is utilized to provide, for example, a 93% concentration of oxygen to a wound site via the combination therapy pad 804. In a typical embodiment, the oxygen generator/concentrator 810 and the control unit 802 are separate devices; however, in other embodiments, the oxygen generator/concentrator 810 and the control unit 802 are contained in a single housing.
[0055] Still referring to FIG. 8A, fiber optic strands (not explicitly shown) direct ultraviolet light from a plurality of LEDs (not explicitly shown) located in the wound evacuation and UV-LED unit 808 to an array of fiber optic strands (not explicitly shown) located on an undersurface of the combination therapy pad 804. The control unit 802 may be used to modulate the ultraviolet light to create, for example, various patterns of light, different intensities of light, and different durations of light. For example, in various embodiments, the control unit 802 is used to produce pulsed emission of the ultraviolet light.
[0056] FIG. 8B is a front perspective view of a wound care system according to an exemplary embodiment. The wound care system 800 includes the control unit 802, the combination therapy pad 804, and the plurality of tubular members 806 connecting the combination therapy pad 804 to the control unit 802. A user interface 805 is disposed on a front surface of the control unit 802. In a typical embodiment, the user interface 805 allows a user to control various parameters of wound care-treatment including, for example, oxygen concentration, oxygen pressure, temperature, and ultra-violet light intensity. The user interface 805 may be pivoted relative to the control unit 802 to provide a favorable viewing angle. In a typical embodiment, the user interface 805 may be, for example a touch screen interface; however, in other embodiments, the user interface 805 may be, for example, a plurality of controls or any other user interface. Use of the combination therapy pad 804 incorporates ultraviolet light and evacuation therapies for wound cleaning with thermal and oxygenation therapy known to promote healing. In various embodiments, Velcro cross straps (not shown) may be used to secure the combination therapy pad 804.
[0057] FIG. 8C is a front perspective view of the wound care system of FIG. 8A illustrating a plurality of foldable hooks. The wound care system 800 includes a plurality of foldable hooks 803 disposed, for example, along a top of the control unit 802. In a typical embodiment, the plurality of foldable hooks 803 may be utilized to hang the control unit 802 from, for example, a hospital bed.
[0058] FIG. 9 is a block diagram of a wound care system according to an exemplary embodiment. In a wound-care system 900, a control unit display 902 is provided in conjunction with a processing unit 904. In a typical embodiment, the processing unit 904 is an analog/digital processing unit. A plurality of sensors 906 are utilized in conjunction with the processing unit 904 for control of heat transfer fluids to a combination therapy pad 804. In various embodiments, the oxygen generator/concentrator 810 is connected to a power supply 908. The power supply 908 also powers the processing unit 904. Oxygen generated by the oxygen generator/concentrator 810 is pumped through a compression pump 910 and a pressure switch 921 before being delivered to the combination therapy pad 804.
[0059] Still referring to FIG. 9, in a typical embodiment, a water/alcohol reservoir 912 is in fluid communication with a fluid pump 914 and a thermoelectric cooler 916. The thermoelectric cooler 916 is controlled by the processing unit 904. In a typical embodiment, a vacuum pump 918 is powered by the power supply 908. A collection chamber 920 is fluidly connected to the vacuum pump 918 and the pressure switch 921. The pressure switch 921 is fluidly coupled to the combination therapy pad 804. In a typical embodiment, oxygen therapy and vacuum therapy are each administered to the combination therapy pad 804 through a common port 922. In a typical embodiment, the pressure switch 921 is capable of adjusting the combination therapy pad 804 between vacuum treatment and oxygenation therapy.
[0060] FIG. 10 is a block diagram of a wound care system according to an exemplary embodiment. In a typical embodiment, a wound care system 1000 is similar in construction to the arrangement described above with respect to FIG. 9. However, the wound care system 1000 does not include a water/alcohol reservoir or a fluid pump as shown in FIG. 9. In a typical embodiment, the thermoelectric cooler 916 is in fluid communication with the compression pump 910. Thus, thermal therapy is supplied to the combination therapy pad 804 through heating and cooling of the oxygen supplied by the oxygen generator/concentrator 810.
[0061] FIG. 11 is a diagrammatic illustration of a combination therapy pad according to an exemplary embodiment. In a typical embodiment, the combination therapy pad 804 includes a plurality of fiber optic strands 72 to project ultraviolet light onto a wound area (not explicitly shown). In various embodiments, the fiber optic strands 72 may be cleaved or side-emitting fibers; however, one skilled in the art will recognize that any type of fiber-optic strand could be used. In a typical embodiment, the combination therapy pad 804 also includes a plurality of oxygenation/removal ports 1102. In a typical embodiment, the oxygenation/removal ports 1102 alternate between providing oxygen therapy and vacuum therapy to the wound area.
[0062] Still referring to FIG. 11, in a typical embodiment, oxygen therapy and vacuum therapy is administered to the combination therapy pad 804 via an evacuation/oxygenation line 1104. The evacuation/oxygenation line 1104 is fluidly coupled to the pressure switch 921. The pressure switch 921 is fluidly connected to the compression pump 910 and the vacuum pump 918. Thus, in a typical embodiment, the pressure switch 921 is capable of adjusting the combination therapy pad 804 between vacuum treatment and oxygenation therapy.
[0063] Still referring to FIG. 11, in various embodiments, a luer lock 1106 is fluidly coupled to the combination therapy pad 804. During treatment, it is often necessary to administer various medications to a wound site. Such administration often requires removal of a wound dressing such as, for example, the combination therapy pad 804. Frequent removal of the wound dressing can increase risk of further damage to tissue immediately surrounding the wound site. In a typical embodiment, the luer lock 1106 allows for administration of medications and other therapeutic compounds directly to a wound site without the need to remove the combination therapy pad 804.
[0064] FIG. 12 is a diagrammatic illustration of a combination therapy pad according to an exemplary embodiment. In a typical embodiment, the combination therapy pad 1200 includes the plurality of fiber optic strands 72 to project ultraviolet light onto a wound area (not explicitly shown). In a typical embodiment, a combination therapy pad 1200 also includes a radio frequency ("RF") antenna 1202. In a typical embodiment, the RF antenna 1202 comprises a wire 1204. The wire 1204 extends along a length of the combination therapy pad 1204. In a typical embodiment, the wire 1204 is disposed within the combination therapy pad 1200 so that, during use, the wire is in close proximity to a wound area. In various embodiments, the wire 1204 is insulated to reduce risk of electric shock to a patient.
[0065] FIG. 13 is an exploded view of a combination therapy pad according to an exemplary embodiment. A combination therapy pad 1300 includes a first layer 1302 having a first central gap 1304 formed therein. In a typical embodiment, the first layer 1302 is constructed of, for example, urethane. A second layer 1305 is disposed below the first layer 1302 and includes an adhesive bottom surface 1306. A second central gap (not explicitly shown) is formed in the second layer 1305 In a typical embodiment, the second layer 1305 is constructed of, for example, urethane. The first layer 1302 and the second layer 1305 are coupled to each other around a perimeter of the first layer 1302 and the second layer 1305 so that the second central gap aligns with the first central gap 1304. A fiber-optic array 1308 is disposed between the first layer 1302 and the second layer 1305 so as to fill a space defined by the first central gap 1304 and the second central gap.
[0066] Still referring to FIG. 13, a third layer 1310 is disposed above the first layer 1302. The third layer 1310 includes a recessed central area 1312. The recessed central area 1312 is fluidly coupled to a vacuum tube 1314 via a first port and a therapeutic fluid tube 1316 via a second port. An antenna 1318 is coupled to the third layer 1310. The antenna 1318 is formed into a loop and is generally arranged around a perimeter of the recessed central area 1312. In a typical embodiment, the first layer 1302, the second layer 1305, and the third layer 1310 are coupled to each other via a process such as, for example, adhesive bonding or welding.
[0067] Still referring to FIG. 13, during operation, the adhesive bottom surface 1306 is placed on a bodily region of a patient proximate a wound area. In a typical embodiment, the adhesive bottom surface 1306 is oriented such that the second central gap is positioned over the wound area. Thus, the adhesive bottom surface 1306 is not in direct contact with the wound area. The fiber-optic array 1308 is disposed over the wound area and, in various embodiments, may contact the wound area. The fiber-optic array 1308 delivers UV lighting to the wound area thereby promoting cleaning and disinfection of the wound area. The vacuum tube 1314 applies negative pressure to the wound area thereby removing undesirable fluids, tissues, and the like from the wound area. The therapeutic fluid tube 1316 provides a therapeutic fluid such as, for example, oxygen to the wound area. In various embodiments, the therapeutic fluid may be heated or cooled prior to delivery to the wound area. Heating or cooling of the therapeutic fluid allows delivery of thermal therapy to the wound area.
[0068] Still referring to FIG. 13, during operation, a pulsed radio-frequency ("RF") signal having a pulse frequency on the order of, for example 27 MHz, is transmitted to the antenna 1318. In a typical embodiment, an amplitude of the pulsed RF signal is on the order of, for example, a fraction of a Watt. Such an amplitude is below a threshold where federal licensing is typically required. The antenna 1318 receives the pulsed RF signal from a radio-frequency source and transmits the pulsed RF signal to a region in close proximity to the wound area. Exposing the wound area to the pulsed RF signal has been shown to be beneficial to healing by encouraging intracellular communication. In particular, pulsed RF signals have been shown to stimulate cellular bonding, and metabolism.
[0069] The previous Detailed Description is of embodiment(s) of the invention. The scope of the invention should not necessarily be limited by this Description. The scope of the invention is instead defined by the following claims and the equivalents thereof.
* * * * *
D00000

D00001

D00002

D00003

D00004

D00005

D00006

D00007

D00008

D00009

D00010

D00011

D00012
D00013

D00014
XML
uspto.report is an independent third-party trademark research tool that is not affiliated, endorsed, or sponsored by the United States Patent and Trademark Office (USPTO) or any other governmental organization. The information provided by uspto.report is based on publicly available data at the time of writing and is intended for informational purposes only.
While we strive to provide accurate and up-to-date information, we do not guarantee the accuracy, completeness, reliability, or suitability of the information displayed on this site. The use of this site is at your own risk. Any reliance you place on such information is therefore strictly at your own risk.
All official trademark data, including owner information, should be verified by visiting the official USPTO website at www.uspto.gov. This site is not intended to replace professional legal advice and should not be used as a substitute for consulting with a legal professional who is knowledgeable about trademark law.