Methods Of Improving Myocardial Performance In Fontan Patients Using Udenafil Compositions
Yeager; James L. ; et al.
U.S. patent application number 16/147153 was filed with the patent office on 2019-01-31 for methods of improving myocardial performance in fontan patients using udenafil compositions. This patent application is currently assigned to Mezzion Pharma Co., Ltd.. The applicant listed for this patent is The Children's Hospital of Philadelphia, Mezzion Pharma Co., Ltd.. Invention is credited to David J. Goldberg, Stephen M. Paridon, James L. Yeager.
| Application Number | 20190030038 16/147153 |
| Document ID | / |
| Family ID | 55301323 |
| Filed Date | 2019-01-31 |



View All Diagrams
| United States Patent Application | 20190030038 |
| Kind Code | A1 |
| Yeager; James L. ; et al. | January 31, 2019 |
METHODS OF IMPROVING MYOCARDIAL PERFORMANCE IN FONTAN PATIENTS USING UDENAFIL COMPOSITIONS
Abstract
The present invention relates generally to the field of using udenafil or a pharmaceutically acceptable salt thereof in patients who have undergone the Fontan operation.
| Inventors: | Yeager; James L.; (Lake Forest, IL) ; Goldberg; David J.; (Philadelphia, PA) ; Paridon; Stephen M.; (Strafford, PA) | ||||||||||
| Applicant: |
|
||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Assignee: | Mezzion Pharma Co., Ltd. Seoul PA The Children's Hospital of Philadelphia Philadelphia PA The Children's Hospital of Philadelphia Philadelphia |
||||||||||
| Family ID: | 55301323 | ||||||||||
| Appl. No.: | 16/147153 | ||||||||||
| Filed: | September 28, 2018 |
Related U.S. Patent Documents
| Application Number | Filing Date | Patent Number | ||
|---|---|---|---|---|
| 14788211 | Jun 30, 2015 | 10137128 | ||
| 16147153 | ||||
| 62036506 | Aug 12, 2014 | |||
| 62186132 | Jun 29, 2015 | |||
| Current U.S. Class: | 1/1 |
| Current CPC Class: | A61P 9/00 20180101; A61K 31/519 20130101; A61K 31/522 20130101; A61K 31/00 20130101; C07D 487/04 20130101 |
| International Class: | A61K 31/522 20060101 A61K031/522; A61K 31/00 20060101 A61K031/00 |
Claims
1-30. (canceled)
31. A pharmaceutical composition for administration to a subject, said pharmaceutical composition comprising: udenafil, or a pharmaceutically acceptable salt thereof, in an amount of about 87.5 mg; and a pharmaceutically acceptable excipient.
32. The pharmaceutical composition of claim 31, wherein said pharmaceutical composition is an oral tablet.
33. The pharmaceutical composition of claim 31, wherein the pharmaceutical composition is a solid or semi-solid oral pharmaceutical composition.
34. The pharmaceutical composition of claim 33, wherein the solid or semi-solid oral pharmaceutical composition is selected from a group of solid or semi-solid oral pharmaceutical compositions consisting of a tablet, a capsule, a gel, a liquid, a liquid dispersion, a pill, a powder and a suspension.
35. The pharmaceutical composition of claim 31, wherein the subject is a human, whose age ranges from about 12 to under about 18 years old.
36. The pharmaceutical composition of claim 35, wherein said pharmaceutical composition is an oral tablet.
37. The pharmaceutical composition of claim 31, wherein the subject is a human, who is under about 18 years.
38. The pharmaceutical composition of claim 37, wherein said pharmaceutical composition is an oral tablet.
39. A pharmaceutical composition for administration to a subject, said pharmaceutical composition comprising: udenafil, or a pharmaceutically acceptable salt thereof, in an amount of about 125 mg; and a pharmaceutically acceptable excipient.
40. The pharmaceutical composition of claim 39, wherein said pharmaceutical composition is an oral tablet.
41. The pharmaceutical composition of claim 39, wherein the pharmaceutical composition is a solid or semi-solid oral pharmaceutical composition.
42. The pharmaceutical composition of claim 41, wherein the solid or semi-solid oral pharmaceutical composition is selected from a group of solid or semi-solid oral pharmaceutical compositions consisting of a tablet, a capsule, a gel, a liquid, a liquid dispersion, a pill, a powder and a suspension.
43. The pharmaceutical composition of claim 39, wherein the subject is a human, whose age ranges from about 12 to under about 18 years old.
44. The pharmaceutical composition of claim 43, wherein said pharmaceutical composition is an oral tablet.
45. The pharmaceutical composition of claim 39, wherein the subject is a human, who is under about 18 years.
46. The pharmaceutical composition of claim 45, wherein said pharmaceutical composition is an oral tablet.
47. A pharmaceutical composition for oral administration to a subject born with single ventricle heart disease who has undergone Fontan surgery for improving, maintaining or reducing the rate of decline in a clinically relevant measurement that is indicative of the subject's health following the Fontan surgery or for increasing the likelihood of improving, maintaining or reducing the rate of decline in the clinically relevant measurement that is indicative of the subject's health following the Fontan surgery, said pharmaceutical composition comprising: udenafil, or a pharmaceutically acceptable salt thereof, in an amount of at least about 125 mg; and a pharmaceutically acceptable excipient; wherein, the subject is a human, whose age ranges between about 12 years old and under about 18 years old; and wherein, the clinically relevant measurement is exercise capacity.
48. The pharmaceutical composition of claim 47, wherein the udenafil, or a pharmaceutically acceptable salt thereof, is in an amount of about 87.5 mg, to be administered twice daily.
49. The pharmaceutical composition of claim 47, wherein the pharmaceutical composition is a solid or semi-solid oral pharmaceutical composition.
50. The pharmaceutical composition of claim 49, wherein the solid or semi-solid oral pharmaceutical composition is selected from a group of solid or semi-solid oral pharmaceutical compositions consisting of a tablet, a capsule, a gel, a liquid, a liquid dispersion, a pill, a powder and a suspension.
51. The pharmaceutical composition of claim 47, wherein the pharmaceutical composition is an oral tablet.
52. A pharmaceutical composition for oral administration to a subject born with single ventricle heart disease who has undergone Fontan surgery for improving, maintaining or reducing the rate of decline in a clinically relevant measurement that is indicative of the subject's health following the Fontan surgery or for increasing the likelihood of improving, maintaining or reducing the rate of decline in the clinically relevant measurement that is indicative of the subject's health following the Fontan surgery, said pharmaceutical composition comprising: udenafil, or a pharmaceutically acceptable salt thereof, in an amount of at least about 125 mg; and a pharmaceutically acceptable excipient; wherein, the subject is a human, whose age ranges between about 12 years old and under about 18 years old; and wherein, the clinically relevant measurement is exercise capacity.
53. The pharmaceutical composition of claim 52, wherein the udenafil, or a pharmaceutically acceptable salt thereof, is in an amount of about 87.5 mg, to be administered twice daily.
54. The pharmaceutical composition of claim 52, wherein the pharmaceutical composition is a solid or semi-solid oral pharmaceutical composition.
55. The pharmaceutical composition of claim 54, wherein the solid or semi-solid oral pharmaceutical composition is selected from a group of solid or semi-solid oral pharmaceutical compositions consisting of a tablet, a capsule, a gel, a pill, a suspension and a powder.
56. The pharmaceutical composition of claim 52, wherein the pharmaceutical composition is an oral tablet.
57. A pharmaceutical composition for oral administration to a subject born with single ventricle heart disease who has undergone Fontan surgery for improving, maintaining or reducing the rate of decline in a clinically relevant measurement that is indicative of the subject's health following the Fontan surgery or for increasing the likelihood of improving, maintaining or reducing the rate of decline in the clinically relevant measurement that is indicative of the subject's health following the Fontan surgery, said pharmaceutical composition comprising: udenafil, or a pharmaceutically acceptable salt thereof, in a therapeutically effective dose; and a pharmaceutically acceptable excipient, for improving, maintaining or reducing the rate of decline in a clinically relevant measurement that is indicative of the subject's health following the Fontan surgery or for increasing the likelihood of improving, maintaining or reducing the rate of decline in the clinically relevant measurement that is indicative of the subject's health following the Fontan surgery in the subject; wherein, the subject is a human, whose age ranges from about 12 to under about 18 years of age or older; wherein, the therapeutically effective dose of udenafil, or a pharmaceutically acceptable salt thereof, is at least about 125 mg; wherein, the pharmaceutical composition is a solid or semi-solid oral pharmaceutical composition; wherein, the solid or semi-solid oral pharmaceutical composition is selected from a group of solid or semi-solid oral pharmaceutical compositions consisting of a tablet, a capsule, a gel, a pill, a suspension and a powder; and wherein, the clinically relevant measurement is exercise capacity.
58. The pharmaceutical composition of claim 57, wherein, the therapeutically effective dose of udenafil, or a pharmaceutically acceptable salt thereof, is about 87.5 mg, to be administered twice daily.
59. An oral pharmaceutical composition for oral administration to a subject born with single ventricle heart disease who has undergone Fontan surgery for improving the subject's exercise capacity or increasing the likelihood of improving the subject's exercise capacity, wherein the subject's exercise capacity is indicative of the subject's health following the Fontan surgery, said oral pharmaceutical composition comprising: a therapeutically effective amount of udenafil, or a pharmaceutically acceptable salt thereof; and a pharmaceutically acceptable excipient, for improving the exercise capacity or increasing the likelihood of improving the subject's exercise capacity; wherein, the therapeutically effective amount of udenafil, or a pharmaceutically acceptable salt thereof, is at least about 125 mg; and wherein, the subject is a human subject.
60. The pharmaceutical composition of claim 59, wherein the therapeutically effective amount of udenafil, or a pharmaceutically acceptable salt thereof, is in an amount of about 87.5 mg, to be administered twice daily.
61. The oral pharmaceutical composition of claim 59, wherein the oral pharmaceutical composition is a tablet.
62. The oral pharmaceutical composition of claim 59, wherein the oral pharmaceutical composition is a solid or semi-solid oral pharmaceutical composition.
63. The oral pharmaceutical composition of claim 62, wherein the solid or semi-solid oral pharmaceutical composition is selected from a group of solid or semi-solid oral pharmaceutical compositions consisting of a tablet, a capsule, a gel, a liquid, a liquid dispersion, a pill, a powder and a suspension.
64. An oral pharmaceutical composition for oral administration to a subject born with single ventricle heart disease who has undergone Fontan surgery for improving the subject's s exercise capacity or increasing the likelihood of improving the subject's exercise capacity, wherein the subject's exercise capacity is indicative of the subject's health following the Fontan surgery, said oral pharmaceutical composition comprising: a therapeutically effective amount of udenafil, or a pharmaceutically acceptable salt thereof; and a pharmaceutically acceptable excipient, for improving the exercise capacity or increasing the likelihood of improving the subject's exercise capacity; wherein, the therapeutically effective amount of udenafil, or a pharmaceutically acceptable salt thereof, is at least about 125 mg; and wherein, the subject is a human subject.
65. The pharmaceutical composition of claim 64, wherein the therapeutically effective amount of udenafil, or a pharmaceutically acceptable salt thereof, is in an amount of about 87.5 mg, to be administered twice daily.
66. The oral pharmaceutical composition of claim 64, wherein the oral pharmaceutical composition is a tablet.
67. The oral pharmaceutical composition of claim 64, wherein the oral pharmaceutical composition is a solid or semi-solid oral pharmaceutical composition.
68. The oral pharmaceutical composition of claim 67, wherein the solid or semi-solid oral pharmaceutical composition is selected from a group of solid or semi-solid oral pharmaceutical compositions consisting of a tablet, a capsule, a gel, a pill, a suspension and a powder.
Description
CROSS REFERENCE TO RELATED APPLICATIONS
[0001] The present invention claims priority to U.S. Provisional Patent Application No. 62/036,506, filed on Aug. 12, 2014, and U.S. Provisional Patent Application No. 62/186,132, filed on Jun. 29, 2015, the disclosures of which are specifically incorporated herein by reference.
FIELD OF THE INVENTION
[0002] The present invention relates generally to the field of using phosphodiesterase E5 (PDE5) inhibitors in patients who have undergone the Fontan operation. In particular, the PDE5 inhibitor is udenafil or a pharmaceutically acceptable salt thereof.
BACKGROUND OF THE INVENTION
1. Background Regarding the Fontan Procedure
[0003] The Fontan procedure, or Fontan/Kreutzer procedure, is a palliative surgical procedure for children born with functional single ventricle congenital heart disease. The Fontan operation was designed to provide blood flow in series to the pulmonary and systemic circulation without the requirement for a right ventricular pumping chamber. The operation allows systemic venous blood to flow directly into the pulmonary circulation on the basis of a single ventricular impetus through the arteries, capillaries, and systemic venous system. This arrangement has improved life expectancy for patients with single-ventricle and pulmonary-outflow obstruction compared with previous arterial shunts.
[0004] The operation, which creates a total cavopulmonary connection, separates the systemic and pulmonary circuits and eliminates both hypoxemia and ventricular volume overload. However, following the Fontan operation there is no ventricular pump to propel blood into the pulmonary arteries. Instead, blood returns to the lungs via passive flow from the systemic veins. This results in a circulation characterized by elevated central venous pressure, abnormal pulmonary vascular resistance, and a chronically low cardiac output. Over time, these inherent characteristics of Fontan physiology result in a predictable, persistent deterioration of cardiovascular efficiency, as marked by a progressive decline in exercise performance that begins after puberty. This decline in exercise capacity correlates with an increase in symptoms from cardiovascular dysfunction and may result in the need for hospitalization, escalation of heart failure management, or transplant.
[0005] Those with the Fontan circulation do not have `normal` heart physiology or functioning. Two major complications that might have many "downstream" effects are the following effects on increasing ("hypertension") and decreasing ("hypotension") blood pressure depending upon its location (veins or arteries). First, with Fontan circulation, there is "systemic venous hypertension", which means that the blood pressure in the veins (blood going back to the heart) in the body is higher than in individuals with normal heart function (not Fontan circulation). There are many negative consequences that may be caused by systemic venous hypertension (congestive heart failure, edema or swelling, dysfunction of the liver, potentially protein-losing enteropathy) that are basically related to the distribution of fluids in the body. A second complication is "pulmonary arterial hypotension" where the blood pressure in arteries going towards or in the lungs (hence pulmonary) is lower than in individuals with normal heart function. There are also a number of negative consequences associated with pulmonary arterial hypotension such as cyanosis (blue lips) or lack of exercise capacity. Many of the subsequent medical conditions and deaths that follow the Fontan procedure (either in the short- or long-term) are thought to originate from this change in systemic and pulmonary blood pressure.
[0006] The long-term effects of marked single-ventricle preload and inefficient oxygenation via an arterial shunt rarely allow survival beyond the second or third decade of life. Uniformly lethal four decades ago, the newborn with single ventricle type congenital heart disease in 2010 is now not only likely--but expected--to survive. However, as these children have grown into adolescence and adulthood, it is clear that there are significant limitations to this strategy. While lifesaving, the Fontan/Kreutzer operation results in profound physiological disturbances with very serious consequences. Pervasive abnormalities of multiple organ systems are affected as time goes on. Realistically, it is unlikely that patients will survive into their third or fourth decades of life untouched by some potentially life-threatening complication. Thus, there is a clear need to identify treatments that may ameliorate the dysfunctional state of the Fontan operation. This is particularly true given the increase in the prevalence of the Fontan procedures: remarkably, the Fontan operation has become the most common procedure performed for congenital heart disease after the age of 2 years. W. M. Gersony, Circulation, 117: 13-15 (2008).
[0007] Multiple studies looking at the results of the Fontan operation demonstrate a decrease in survival beyond 15 years after surgery. An ongoing significant risk of death with continuous attrition is present, regardless of surgical type of cavo-pulmonary connection. In another study looking at morphologically single left ventricle after Fontan surgery, results showed that odds are 1 out 4 that a child after Fontan will be dead by the time he or she reaches their late 20s. J. Rychik, "Forty Years of the Fontan Operation: A Failed Strategy," Pediatric Cardiac Surgery Annual, 96-100(2010).
[0008] Given the increased life span for Fontan patients, researchers have sought out medical therapies to address the side effects of the Fontan surgery. In particular, children and young adults with single-ventricle physiology have abnormal exercise capacity after the Fontan operation. Strategies targeted toward improving cardiac output and reducing central venous pressure will improve their overall well-being and mitigate against the impact of this deleterious physiology.
[0009] In one study, the PDE5 inhibitor sildenafil was found to significantly improve ventilatory efficiency during peak and submaximal exercise. There was also a suggestion of improved oxygen consumption at the anaerobic threshold in 2 subgroups. These findings suggest that sildenafil may be an important agent for improving exercise performance in children and young adults with single-ventricle physiology after the Fontan operation. Goldberg et al., Circulation, 123: 1185-1193 (2011).
[0010] Later studies verified that sildenafil increased ventricular systolic elastance and improved ventriculo-arterial coupling in patients palliated with Fontan circulation. Short-term sildenafil was well tolerated in most of the patients with only minor side effects. Shabanian et al., Pediatr. Cardiol., 34(1): 129-34 (2013). The structure of sildenafil is shown below:
##STR00001##
[0011] In addition, a preliminary study assessed the short-term effects of the PDE5 inhibitor tadalafil on the hemodynamic response to exercise and exercise capacity in patients with Fontan circulation. See http://clinicaltrials.gov/ct2/show/record/NCT01291069. Short term therapy with once daily dosing of tadalafil improved ventilatory efficiency and oxygen saturation, but exercise capacity was unchanged in young Fontan subjects, similar to published sildenafil results. Menon et al., Circulation, 128: A16024 (2013). The chemical structure of tadalafil is shown below:
##STR00002##
[0012] For optimal effectiveness, the PDE5 inhibitors sildenafil or tadalafil would need to be given long term to Fontan patients to delay or prevent the onset of failing Fontan circulation. Fontan surgery produces chronic conditions; short term treatment is unlikely to address mortality associated with children having a Fontan surgery when they are an adolescent or adult. This is particularly true as when Fontan failure sets in, there is an inexorable hemodynamic and functional decline in the patients leading to death or cardiac transplantation. The early experience with transplantation in patients with Fontan circulation was of high operative mortality and morbidity. The assumption that if a patient survives with a Fontan circulation, then the PVR is low enough for the right ventricle of the graft after cardiac transplantation was found to be incorrect in the early experience of Fontan transplants.
[0013] While both sildenafil and tadalafil are known to have undesirable side effects, pulmonary arterial hypertension (PAH) patients switched from sildenafil to tadalafil were found to show significantly different oxygen saturation, significantly different oxygen saturation after a 6-minute walk test, and significantly different distances walked, thus showing that PDE5 inhibitors are not interchangeable when used to treat heart or cardiovascular conditions. Sabri et al., Pediatr Cardiol., 35(4):699-704 (2014).
II. Background Regarding PDE5 Inhibitors and Udenafil
[0014] PDE5 is a cyclic guanosine-3',5'-monophosphate (cGMP)-specific phosphodiesterase belonging to a class of phosphodiesterases which regulate various cell functions by catalyzing the hydrolysis of the second messenger molecules (cGMP) and cyclic adenosine-3',5'-monophosphate (cAMP). Boolell et al., Int'l J. Impot. Res., 8:47 (1996). Because PDE5 is present in the arterial wall smooth muscle within the lungs, PDE5 inhibitors have been explored for the treatment of pulmonary hypertension, a disease in which blood vessels in the lungs become overloaded with fluid, usually as a result of failure of the right ventricle of the heart.
[0015] Udenafil is a drug used in urology to treat erectile dysfunction. It belongs to a class of drugs called PDE5 inhibitors, which also includes sildenafil, tadalafil, and vardenafil. Typical doses are 100 and 200 mg. Udenafil is available in Korea, Russia, and Philippines; in the United States, it is not approved for use by the U.S. Food and Drug Administration.
[0016] The Fontan procedure is palliative, not curative. But in many cases it can result in normal or near-normal growth, development, exercise tolerance, and good quality of life. In 20/30% cases, patients will eventually require heart transplantation.
[0017] Modifications in the Fontan operative model was one of the early steps in improving outcome. Use of fenestration, staging of Fontan completion and better perioperative management have led to a significant drop in mortality rates in the current era. Despite this, there is late attrition of patients with complications such as arrhythmias, ventricular dysfunction, and unusual clinical syndromes of protein-losing enteropathy (PLE) and plastic bronchitis. Management of failing Fontan includes a detailed hemodynamic and imaging assessment to treat any correctable lesions such as obstruction within the Fontan circuit, early control of arrhythmia and maintenance of sinus rhythm, symptomatic treatment for PLE and plastic bronchitis, manipulation of systemic and pulmonary vascular resistance, and Fontan conversion of less favorable atriopulmonary connection to extra-cardiac total cavopulmonary connection with arrythmia surgery. Cardiac transplantation remains the only successful definitive palliation in the failing Fontan patients. However, cardiac transplantation is not a perfect solution because the Fontan circulation has already wreaked havoc in the body such as negatively affecting hepatic or kidney function, thus patients with Fontan circulation may still be in poor shape even after a heart transplant.
[0018] There is a need in the art for improved therapies relating to complications or side effects of the Fontan procedure with the goal of increasing the life span of Fontan patients, and avoiding or delaying the need for cardiac transplantation. There is also a need in the art for improved therapies to delay the onset of cardiac failure or to improve the quality of life for patients who have had the Fontan procedure. The present invention satisfies this need.
SUMMARY OF THE INVENTION
[0019] In one embodiment, the invention is directed to methods of treating, preventing, or minimizing conditions, symptoms, or side effects associated with a subject who has previously had a Fontan procedure. In particular, the methods of the invention are directed the use of udenafil or a pharmaceutically acceptable salt thereof in single ventricle adolescent patients that have undergone the Fontan procedure for the amelioration of associated acute symptoms and chronic symptom development. The method comprises administering a therapeutically effective amount of a PDE5 inhibitor to the patient, where the PDE5 inhibitor is udenafil or a pharmaceutically acceptable salt thereof.
[0020] In one embodiment, the invention is directed to a method of improving cardiac output in a patient who has had a Fontan procedure. The method comprises administering a therapeutically effective amount of a PDE5 inhibitor to the patient, where the PDE5 inhibitor is udenafil or a pharmaceutically acceptable salt thereof.
[0021] In another embodiment, the invention is directed to a method of decreasing pulmonary vascular resistance in a patient who has had a Fontan procedure. The method comprises administering a therapeutically effective amount of a PDE5 inhibitor to the patient, where the PDE5 inhibitor is udenafil or a pharmaceutically acceptable salt thereof.
[0022] In yet another embodiment, the invention is directed to a method of improving exercise capacity in a patient who has had a Fontan procedure. The method comprises administering a therapeutically effective amount of a PDE5 inhibitor to the patient, where the PDE5 inhibitor is udenafil or a pharmaceutically acceptable salt thereof.
[0023] In one embodiment, the invention is directed to a method of improving myocardial performance in a patient who has had a Fontan procedure. The method comprises administering a therapeutically effective amount of a PDE5 inhibitor to the patient, where the PDE5 inhibitor is udenafil or a pharmaceutically acceptable salt thereof.
[0024] In an exemplary embodiment, the methods of the invention comprise administering a therapeutically effective dose of udenafil, or a pharmaceutically acceptable salt thereof, once a day to a patient.
[0025] In another embodiment, the methods of the invention comprise administering a therapeutically effective dose of udenafil, or a pharmaceutically acceptable salt thereof, twice a day to a patient.
[0026] In another embodiment, the patient is a pediatric patient of about 2 to about 18 years of age. Treatment of adult patients are also encompassed by the methods of the invention.
[0027] In yet another embodiment, the invention is directed to improved methods for treating a patient who has had a Fontan procedure, wherein the methods show an improvement in patient compliance with a dosing schedule of udenafil or a pharmaceutically acceptable salt thereof, as compared to patients prescribed a non-udenafil drug.
[0028] In one embodiment, the invention is directed to improved methods for treating a patient who has had a Fontan procedure, wherein the methods of the invention result in fewer or less severe adverse events as compared to conventional, methods of treating such patients. In another embodiment, the methods of the invention result in few, if any, serious adverse events, moderate adverse events, or mild adverse events.
[0029] In another embodiment, the methods of the invention result in improved VO2 at the patient's maximal effort as compared to VO2 at maximal effort in the absence of the methods of the invention (e.g., in the absence of udenafil administration). For example, the improvement can be about 5, about 6, about 7, about 8, about 9, about 10, about 11, about 12, about 13, about 14, about 15, about 16, about 17, about 18, about 19, about 20, about 21, about 22, about 23, about 24, about 25, about 26, about 27, about 28, about 29, or about 30% or greater as compared to VO2 at maximal effort in the absence of the methods of the invention (e.g., in the absence of udenafil administration).
[0030] In another embodiment, the methods of the invention result in improved VO2 at the patient's anaerobic threshold as compared to VO2 at anaerobic threshold in the absence of the methods of the invention (e.g., in the absence of udenafil administration). For example, the improvement can be about 5, about 6, about 7, about 8, about 9, about 10, about 11, about 12, about 13, about 14, about 15, about 16, about 17, about 18, about 19, about 20, about 21, about 22, about 23, about 24, about 25, about 26, about 27, about 28, about 29, or about 30% or greater as compared to VO2 at maximal effort in the absence of the methods of the invention (e.g., in the absence of udenafil administration).
[0031] In another embodiment, the methods of the invention result in the patient's blood pool MPI, or other disclosed measures of ventricular performance, improving as compared to blood pool MPI, or other disclosed measures of ventricular performance in the absence of the methods of the invention (e.g., in the absence of udenafil administration). For example, the improvement can be about 5, about 6, about 7, about 8, about 9, about 10, about 11, about 12, about 13, about 14, about 15, about 16, about 17, about 18, about 19, about 20, about 21, about 22, about 23, about 24, about 25, about 26, about 27, about 28, about 29, or about 30% or greater as compared to blood pool MPI, or other disclosed measures of ventricular performance in the absence of the methods of the invention (e.g., in the absence of udenafil administration).
[0032] In another embodiment, the methods of the invention result in the patient's log of reactive hyperemia index, or another disclosed measure of vascular function, improving as compared to log of reactive hyperemia index, or another disclosed measure of vascular function, in the absence of the methods of the invention (e.g., in the absence of udenafil administration). For example, the improvement can be about 5, about 6, about 7, about 8, about 9, about 10, about 11, about 12, about 13, about 14, about 15, about 16, about 17, about 18, about 19, about 20, about 21, about 22, about 23, about 24, about 25, about 26, about 27, about 28, about 29, or about 30% or greater as compared to log of reactive hyperemia index, or another disclosed measure of vascular function, in the absence of the methods of the invention (e.g., in the absence of udenafil administration).
[0033] Finally, in yet another embodiment, the methods of the invention may result in a characteristic pharmacokinetic profile. The pharmacokinetic profile can comprises a C.sub.max between 300 and 700 ng/ml, or more specifically, about 500 ng/ml; a T.sub.max between 1 and 1.6 hr, or more specifically, about 1.3 hr; an AUC.sub..tau. between 2550 and 4150 nghr/ml, or more specifically, about 3350 nghr/ml; and an AUC.sub.0-24 between 5110 and 8290 nghr/ml, or more specifically, about 6701 nghr/ml.
[0034] The foregoing general description and following detailed description are exemplary and explanatory and are intended to provide further explanation of the invention as claimed. Other objects, advantages, and novel features will be readily apparent to those skilled in the art from the following brief description of the drawings and detailed description of the invention.
BRIEF DESCRIPTION OF THE DRAWINGS
[0035] FIG. 1 shows the percentage of subjects who reported at least one, three, or five adverse events by treatment group.
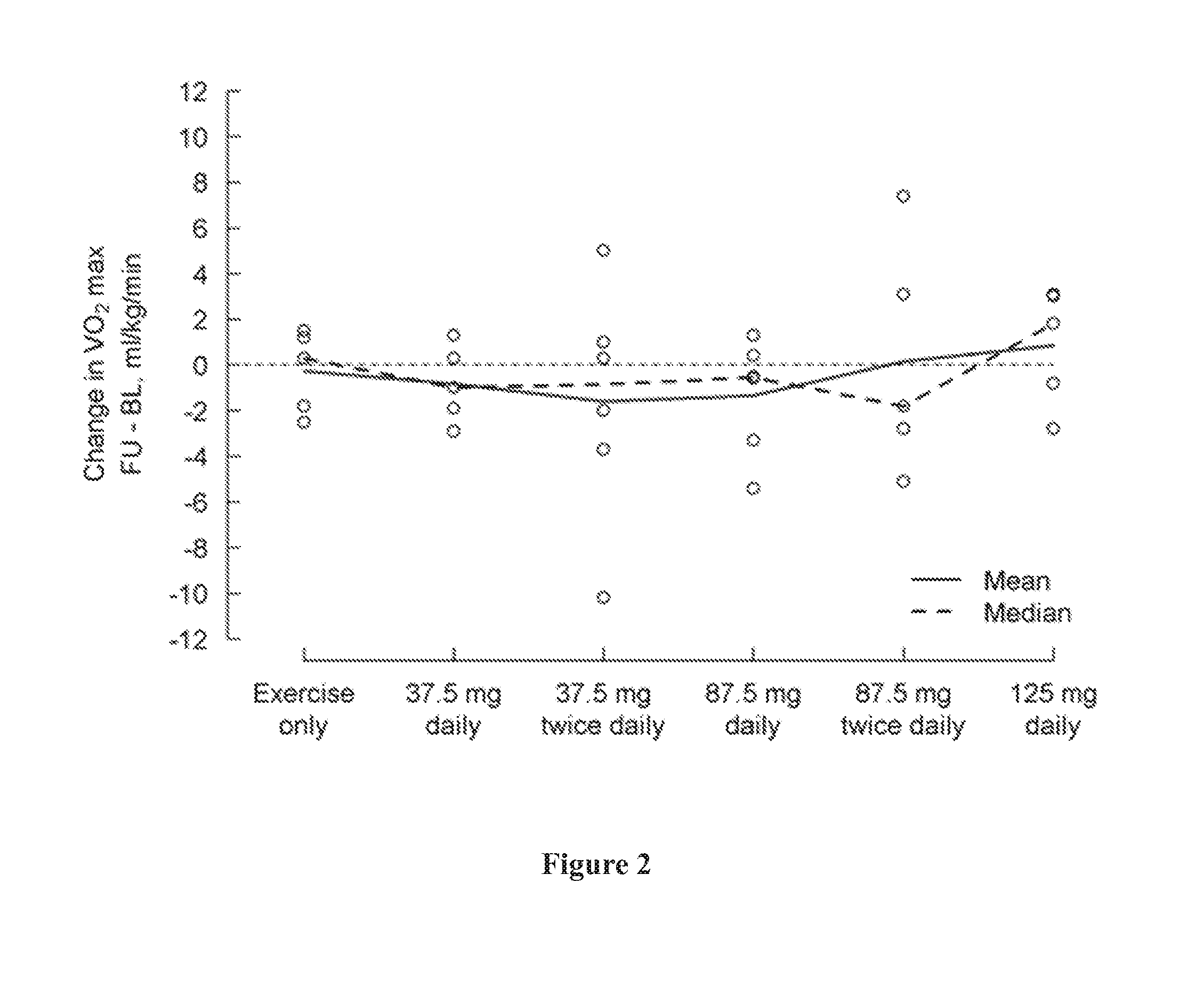
[0036] FIG. 2 shows change in peak VO2 (ml/kg/min) at the maximum effort from baseline (day 1) to the last visit (post-medication, day 5) by treatment group, where a positive change indicates an improvement.
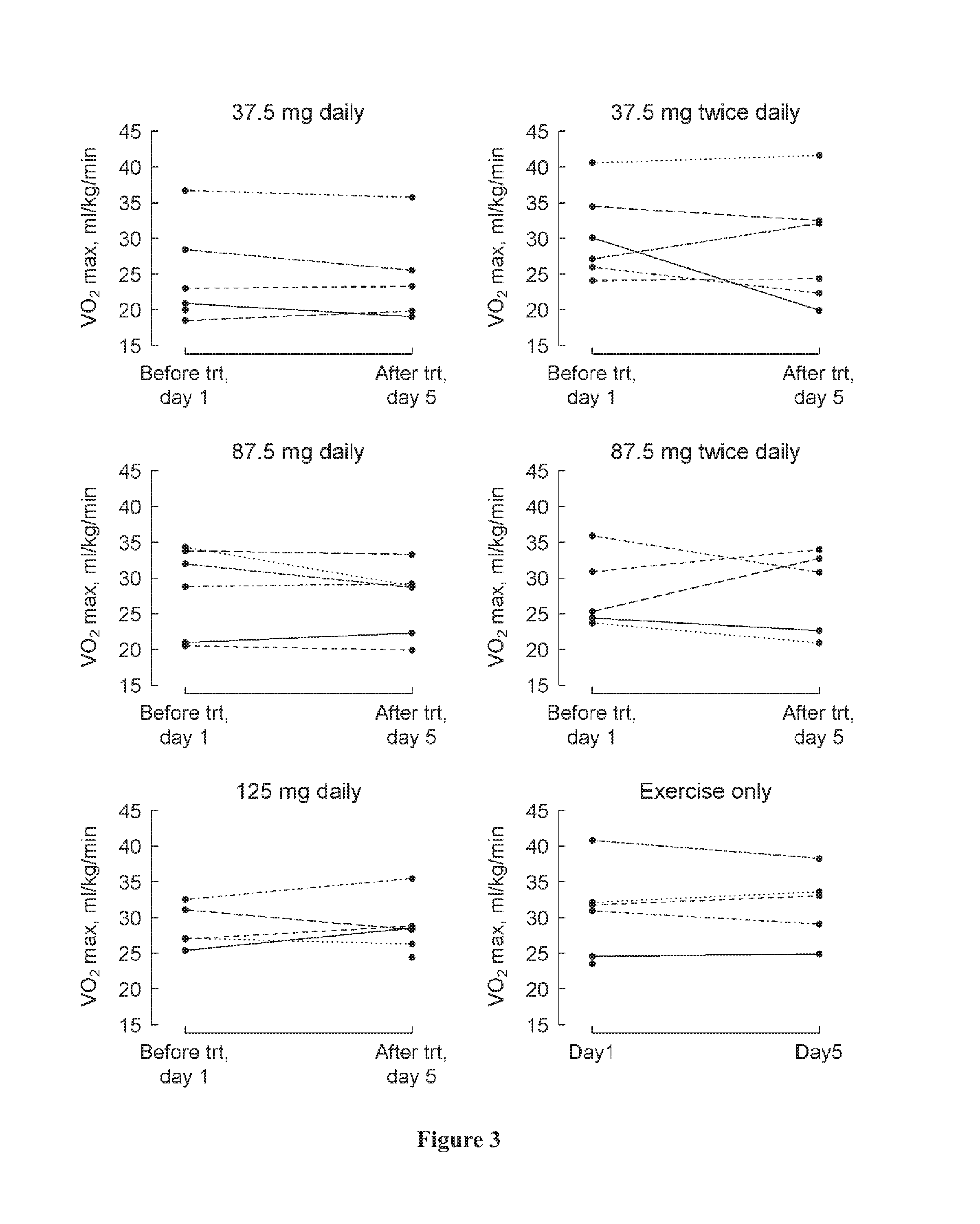
[0037] FIG. 3 shows peak VO2 at the maximum effort at baseline (day 1) and at the last visit (post-medication, day 5) by treatment group, where a positive change indicates an improvement.
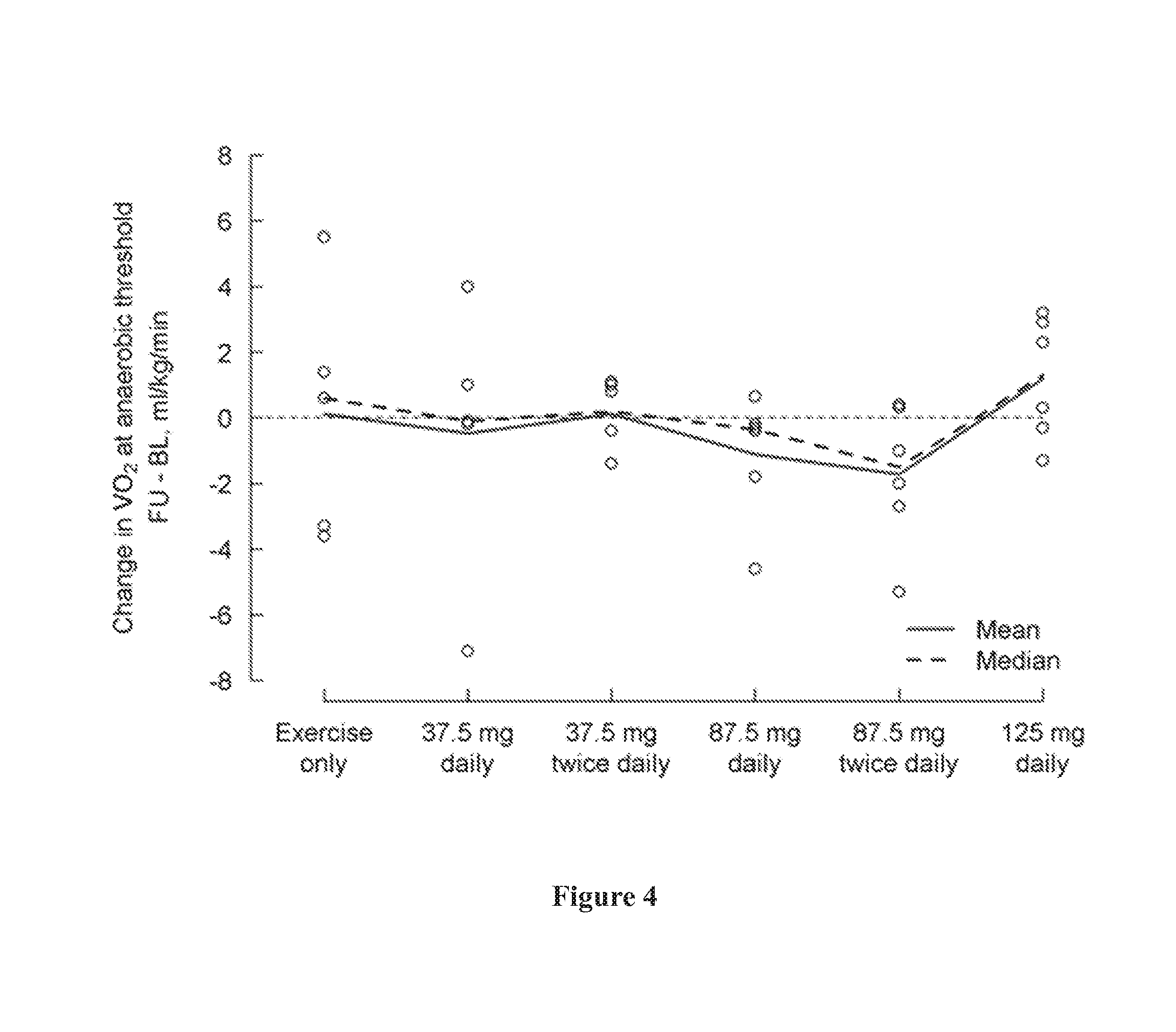
[0038] FIG. 4 shows change in VO2 (ml/kg/min) at anaerobic threshold from baseline (day 1) to the last visit (post-medication, day 5) by treatment group, where a positive change indicates an improvement.
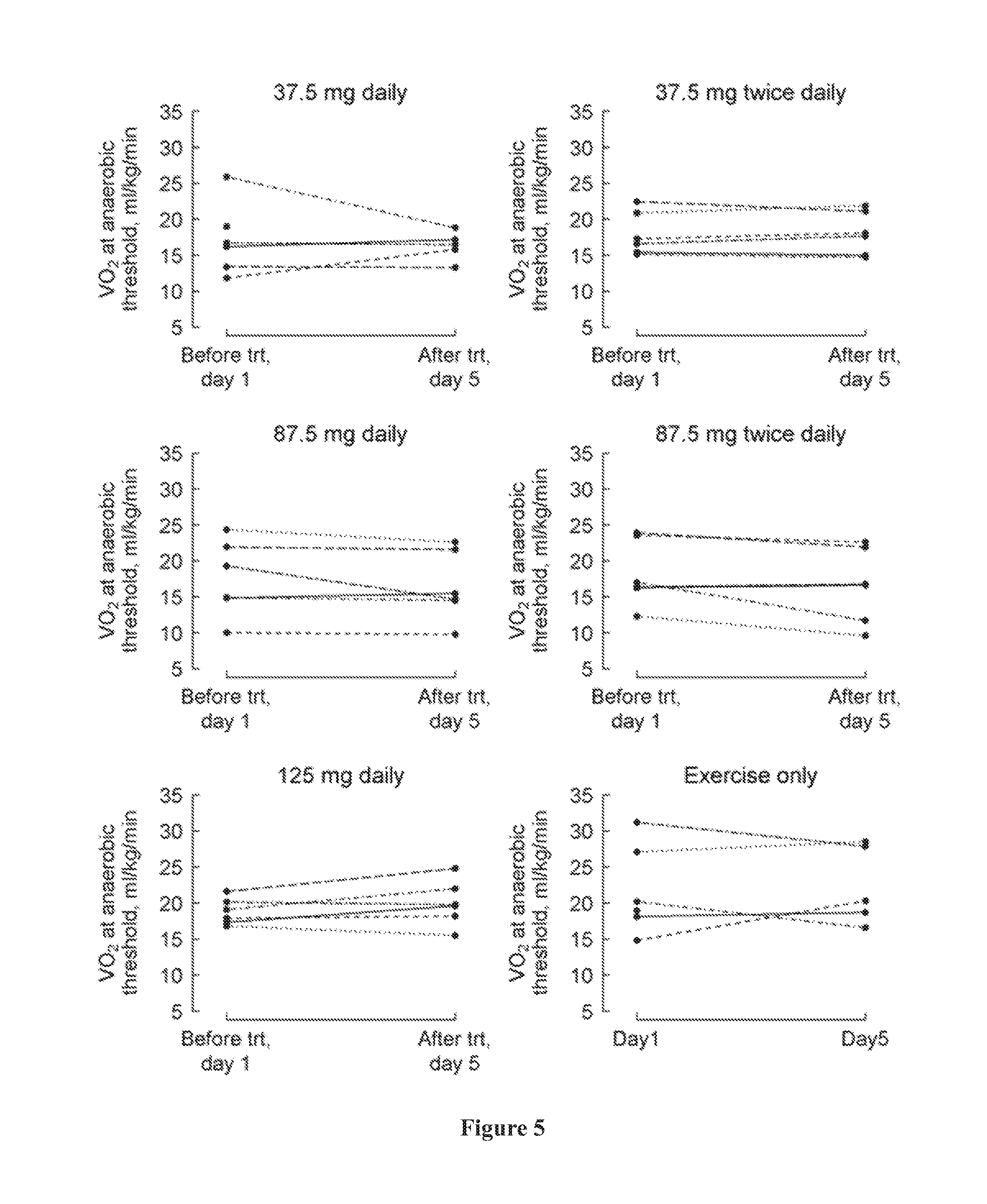
[0039] FIG. 5 shows peak VO2 at anaerobic threshold at baseline (day 1) and at the last visit (post-medication, day 5) by treatment group, where a positive change indicates an improvement.
[0040] FIG. 6 shows change in natural log of Reactive Hyperemia Index from baseline (day 1) to the last visit (post-medication, day 5) by treatment group. A positive change indicates an improvement.
[0041] FIG. 7 shows natural log of Reactive Hyperemia Index (RHI) at baseline (day 1) and at the last visit (post-medication, day 5) by treatment group. A positive change indicates an improvement.
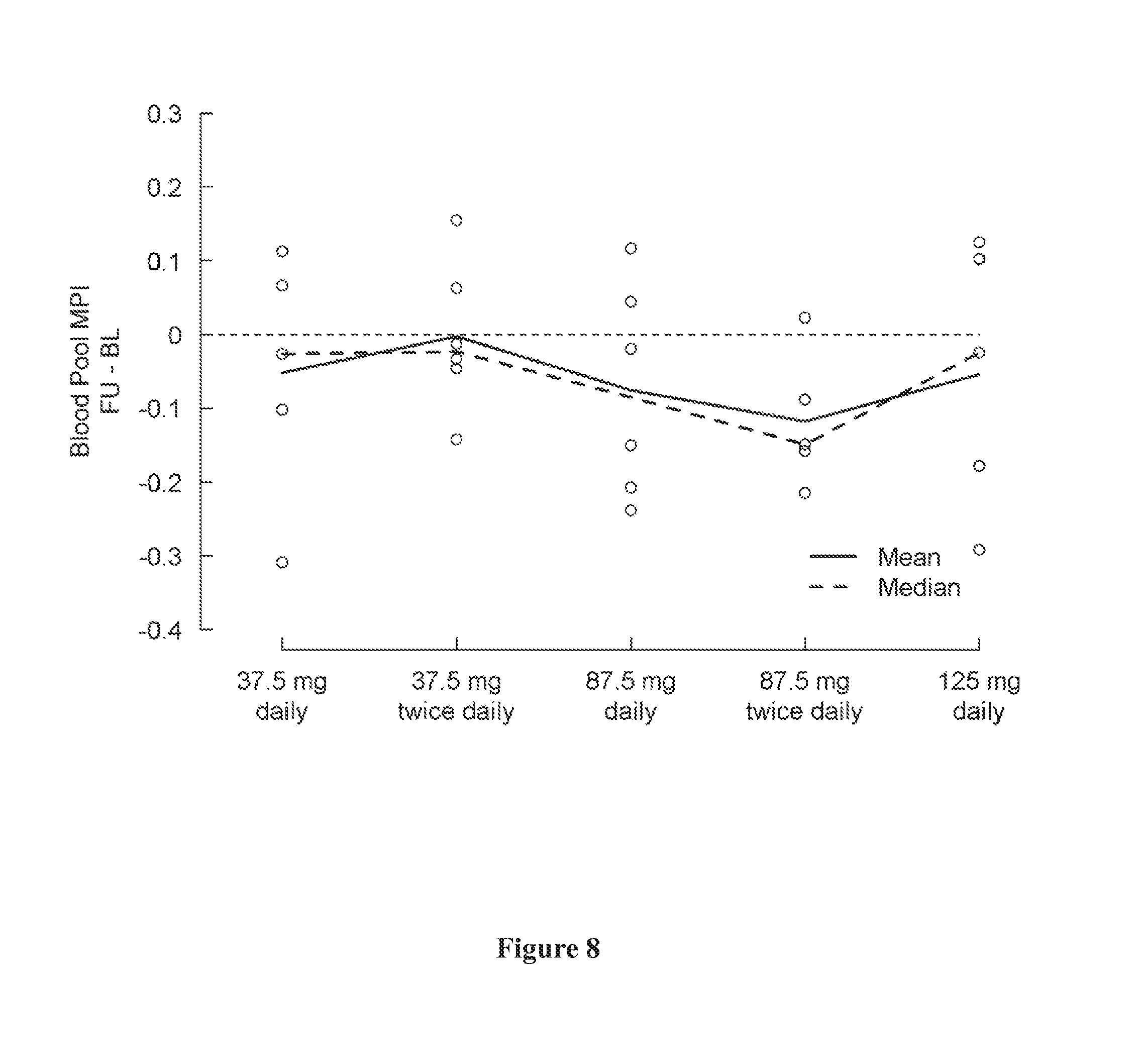
[0042] FIG. 8 shows change in blood pool MPI from baseline (day 1) to the last visit (post-medication, day 5) by treatment group. A negative change indicates an improvement.
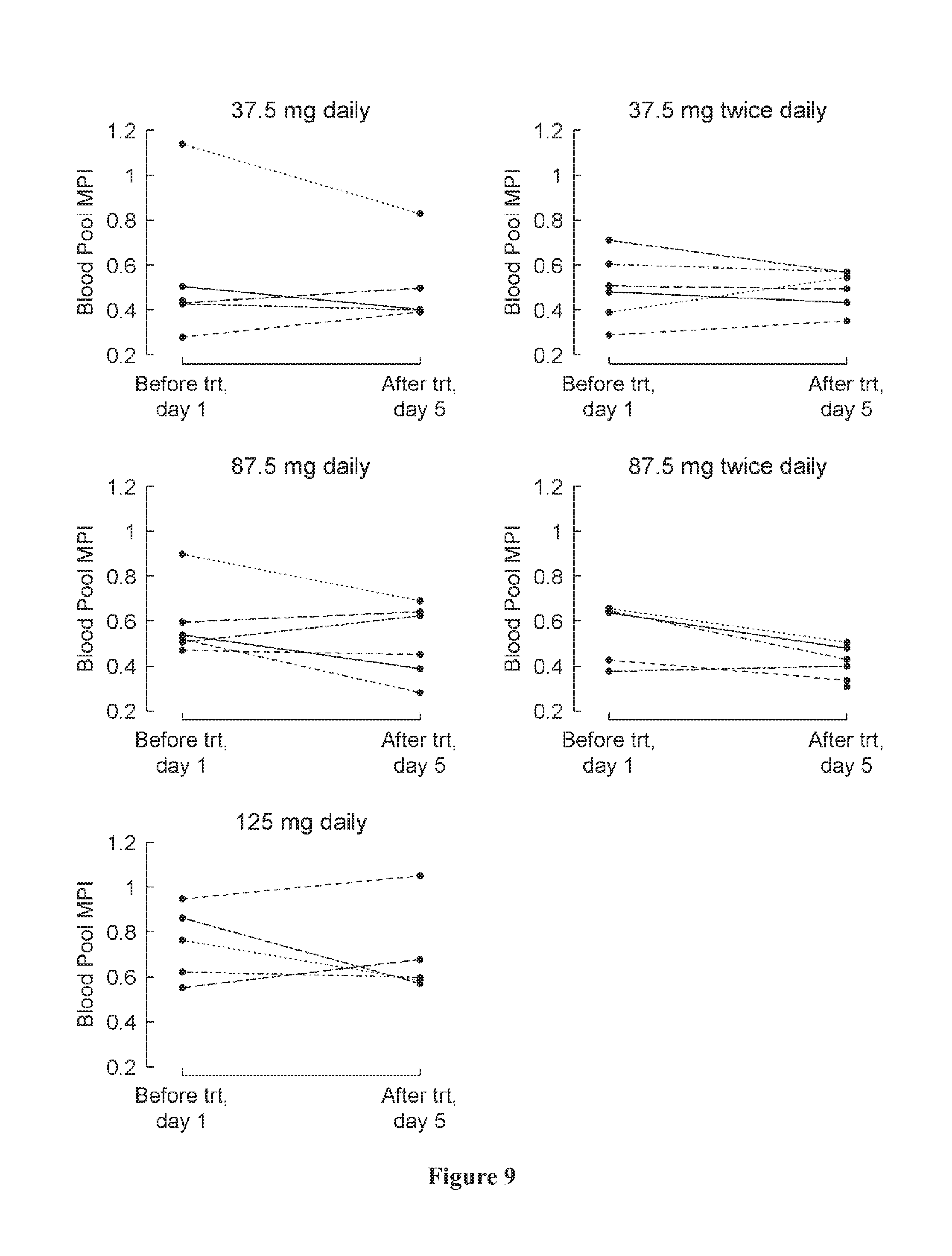
[0043] FIG. 9 shows blood pool MPI at baseline (day 1) and at the last visit (post-medication, day 5) by treatment group. A negative change indicates an improvement.
[0044] FIG. 10 shows change in tissue Doppler MPI from baseline (day 1) to the last visit (post-medication, day 5) by treatment group. A negative change indicates an improvement.
[0045] FIG. 11 shows tissue Doppler MPI at baseline (day 1) and at the last visit (post-medication, day 5) by treatment group. A negative change indicates an improvement.
[0046] FIG. 12 shows change in average isovolumic contraction from baseline (day 1) to the last visit (post-medication, day 5) by treatment group. A negative change indicates an improvement.
[0047] FIG. 13 shows average isovolumic contraction at baseline (day 1) and at the last visit (post-medication, day 5) by treatment group. A negative change indicates an improvement.
[0048] FIG. 14 shows change in average isovolumic relaxation from baseline (day 1) to the last visit (post-medication, day 5) by treatment group. A negative change indicates an improvement.
[0049] FIG. 15 shows average isovolumic relaxation at baseline (day 1) and at the last visit (post-medication, day 5) by treatment group. A negative change indicates an improvement.
[0050] FIG. 16 shows individual concentration time curves stratified by dosing regimens of (A) 37.5 mg q24 h, (B) 37.5 mg q12 h, (C) 87.5 mg q24 h, (D) 87.5 mg q12 h, and (E) 125 mg q24 h.
[0051] FIG. 17 shows concentration time concentration profiles of udenafil in study subjects. The solid line represents the observed data, the dash line stands for the predicted data for the second dose of the day for 12 hour regimens. Data are represented as mean+/-standard deviation.
[0052] FIG. 18 shows a comparison of Cmax among various dosing regimens. The box and whisker plot showed 10-90 percentile and range of observations with middle line representing median value of a dosing regimen. Significant difference: 37.5 mg q24 h vs 87.5 mg q12 h, p<0.001; 37.5 mg q24 h vs 125 mg q24 h, p<0.001; 37.5 mg q12 h vs 87.5 mg q12 h, p<0.001; 37.5 mg q12 h vs 125 mg q24 h, p<0.01; 87.5 mg q24 h vs 87.5 mg q12 h, p<0.05.
[0053] FIG. 19 shows a comparison of (A) AUC.sub..tau. and (B) AUC0-24 among various dosing regimens. The box and whisker plot showed 10-90 percentile and range of observations with middle line representing median value of a dosing regimen. Significant difference: A) 37.5 mg q24 h vs 87.5 mg q12 h, p<0.001; 37.5 mg q24 h vs 125 mg q24 h, p<0.001; 37.5 mg q12 h vs 87.5 mg q12 h, p<0.01; 37.5 mg q12 h vs 125 mg q24 h, p<0.01; B) 37.5 mg q24 h vs 87.5 mg q12 h, p<0.001; 37.5 mg q24 h vs 125 mg q24 h, p<0.01; 37.5 mg q12 h vs 87.5 mg q12 h, p<0.001; 87.5 mg q24 h vs 87.5 mg q12 h, p<0.001; 87.5 mg q12 h vs 125 mg q24 h, p<0.001.
[0054] FIG. 20 shows a comparison of A) CL/F and B) V/F among various dosing regimens. The box and whisker plot showed 10-90 percentile and range of observations with middle line representing median value of a dosing regimen. Significant difference: A) 37.5 mg q24 h vs 87.5 mg q12 h, p<0.05; B) 37.5 mg q24 h vs 87.5 mg q12 h, p<0.01.
[0055] FIG. 21 shows DV (observed concentrations) versus subject ID.
[0056] FIG. 22 shows time (hours) versus subject ID.
[0057] FIG. 23 shows DV (observed concentrations) versus time after dose (TAD).
[0058] FIG. 24 shows DV (observed concentrations) versus time (hours).
[0059] FIG. 25 shows individual visual plots (SID 1-12) with variation between observed concentration (DV) vs predicted concentration (PRED) and individual predicted (IPRED) error vs time (h).
[0060] FIG. 26 shows individual visual plots (SID 13-24) with variation between observed concentration (DV) vs predicted concentration (PRED) and individual predicted (IPRED) error vs time (h).
[0061] FIG. 27 shows individual visual plots (SID 25-30) with variation between observed concentration (DV) vs predicted concentration (PRED) and individual predicted (IPRED) error vs time (h).
[0062] FIG. 28 shows a summary of average plasma concentration per time point from pharmacokinetic studies of udenafil in Fontan's patients. Data are shown as mean+/-standard deviation.
[0063] FIG. 29 shows non-compartmental analysis of udenafil in Fonatn's patients stratified by dosing regimens. Data are shown as mean+/-standard deviation.
[0064] FIG. 30 shows a goodness of fit plot of observed data versus predicted data (DV vs. PRED).
[0065] FIG. 31 shows a goodness of fit plot of observed data versus individual predicted data (DV vs. IPRED).
[0066] FIG. 32 shows a goodness of fit plot of observed data versus predicted data (DV vs. PRED) of the final model.
[0067] FIG. 33 shows a goodness of fit plot of observed data versus individual predicted data (DV vs. IPRED) of the final model.
[0068] FIG. 34 shows characteristic Fontan physiology.
DETAILED DESCRIPTION OF THE PREFERRED EMBODIMENTS
I. Fontan Physiology
[0069] The Fontan physiology is the definitive palliation for those classes of congenital heart defects that share the common feature of a functional single ventricle. They include defects that result in hypoplastic left or right ventricles. Usually through a series of 2 or 3 operations, the systemic and pulmonary circulations are separated to eliminate the mixing of oxygenated and un-oxygenated blood. This is accomplished by directly attaching the superior and inferior vena cavae to the pulmonary arteries. This results in a physiology that works as follows: (1) the single systemic ventricle pumps oxygenated blood out the aorta to the body's systemic vascular bed. (2) Next, the systemic venous blood then returns by the vena cavae and flows passively through the pulmonary vascular bed without the aid of a sub-pulmonary ventricle. (3) Finally, oxygenated blood returns to the common systemic atrium and the cycle is repeated. This anatomy is illustrated in FIG. 34.
[0070] The Fontan operation, which creates a total cavopulmonary connection, separates the systemic and pulmonary circuits and eliminates both hypoxemia and ventricular volume overload. However, following the Fontan operation there is no ventricular pump to propel blood into the pulmonary arteries. Instead blood returns to the lungs via passive flow from the systemic veins. Thus, the major physiologic consequence of this type of palliation is that pulmonary blood flow is completely dependent upon the pressure gradient from the systemic venous bed to the atrium. The normal circulation flow through the pulmonary bed is augmented by the increased pressure generated by the right ventricle. In a healthy adolescent, this results in an increase of about 20 to 25 mm Hg in the pressure present in the pulmonary arteries at rest, which may double with exercise. With the Fontan physiology, there is no sub-pulmonary ventricle and thus no augmentation of pressure as the blood enters the pulmonary arteries. At rest, the pressure gradient across the pulmonary vascular bed is significantly less. The ability to increase this pressure gradient with exercise is extremely limited by the body's ability to tolerate increasingly elevated central venous pressures.
[0071] As a unique consequence of being entirely dependent upon the passive drop in venous pressure to drive pulmonary blood flow, the Fontan physiology is exquisitely sensitive to changes in pulmonary vascular resistance. Even increases that are well within the normal range for pulmonary resistance in normal physiology will have detrimental effects on the Fontan physiology. Likewise any decrease in resistance, even if this value is already normal, has the potential to augment pulmonary blood flow. For this reason, the use of udenafil offers a potential therapy that is unique to this class of palliated congenital heart defects. Unlike other uses for PDE-5 inhibitors, this therapy would be to lower resistance in a population without elevated pulmonary resistances or pressures. This is a distinctly different use of this class of agents as compared to patients with either structurally normal hearts and pulmonary vascular disease or the very rare patient with congenital heart disease palliated with a two ventricle repair (and thus having a sub-pulmonary ventricle) and associated pulmonary vascular disease.
II. Clinical Measurements Relevant to Fontan Patients
[0072] For children born with functional single ventricle congenital heart disease, the Fontan procedure is the current standard of care. The Fontan procedure is palliative, rather than curative, and while it has greatly increased the survival of pediatric subjects with functional single ventricle congenital heart disease, the procedure also results in a series of side effects and complications that can lead to late attrition of patients, with complications such as arrhythmias, ventricular dysfunction, and unusual clinical syndromes of protein-losing enteropathy (PLE) and plastic bronchitis, as well as hepatic and kidney complications.
[0073] In certain embodiments, the disclosed invention relates to improving or preventing the decline of specific clinically relevant measurements that are indicative of a patient's health following a Fontan procedure. Such measurements include, but are not limited to, exercise testing, vascular function testing, and echocardiographic assessment of ventricular performance.
Exercise Testing
[0074] Exercise testing can include assessment of VO2 values during maximal effort or at anaerobic threshold. VO2 max, or maximal oxygen consumption, refers to the maximum amount of oxygen that an individual can utilize during intense exercise. This measurement is generally considered a reliable indicator of cardiovascular fitness and aerobic endurance. Theoretically, the more oxygen a person can use during high level exercise, the more energy that person can produce. This test is the gold standard for cardiorespiratory fitness because muscles need oxygen for prolonged (aerobic) exercise; blood carries oxygen to the muscles and the heart must pump adequate amounts of blood to meet the demands of aerobic exercise.
[0075] VO2 is often measured by putting a mask on a subject, and measuring the volume and gas concentrations of inhaled and expired air. This measurement is often used in both clinical settings and research and is considered the most accurate. Testing commonly involves either exercising on a treadmill or riding a bike at increasing intensity until exhaustion, and is designed to provide readings at a maximal effort of the subject and/or at the subject's anaerobic threshold.
[0076] Patients that have previously undergone a Fontan procedure will generally see a decline in VO2 measurements over time. Treating a patient with a method according to the invention such that the patient's VO2 measurement are either maintained at a similar level, demonstrating that there has been no further decline in VO2 function, or improve with therapy indicates that the treatment is clinically beneficial and may improve or prevent decline in cardiovascular function.
[0077] In one embodiment, the invention is directed to a method of improving or maintaining VO2 measurements of a subject who has previously had a Fontan procedure. The method comprises administering a therapeutically effective amount of a PDE5 inhibitor to the patient, where the PDE5 inhibitor is udenafil or a pharmaceutically acceptable salt thereof. In some embodiments, VO2 is measured at maximal effort, while in other embodiments, VO2 is measured at the subject's anaerobic threshold.
[0078] In some embodiments, the disclosed methods and compositions are administered to a Fontan patient and result in no decrease, or a minimal decrease, in exercise capacity over time. More specifically, the disclosed methods and compositions may result in a decrease in exercise capacity of less than about 40, less than about 35, less than about 30, less than about 35, less than about 20, less than about 15, less than about 10, or less than about 5% over time. The time period between a first and second measurement used to calculate the decrease in exercise capacity can be, for example, about 1, about 2, about 3, about 4, about 5, about 6, about 7, about 8, about 9, about 10, about 11, or about 12 months; about 1, about 2, about 3, about 4, about 5, about 6, about 7, about 8, about 9, about 10, about 11, about 12, about 13, about 14, or about 15 years, or any combination thereof, e.g., 1 year, 3 months; 4 years, 7 months, etc.
[0079] In some embodiments, the disclosed methods and compositions may be administered to a Fontan patient and result in an improvement of exercise capacity. More specifically, the disclosed methods and compositions may result in a 1, 2, 5, 10, 15, 20, 25, 30, 35, 40, 45, or 50% or more improvement in VO2 at maximal effort. Alternatively, the disclosed methods and compositions may result in a 1, 2, 5, 10, 15, 20, 25, 30, 35, 40, 45, or 50% or more improvement in VO2 at the patient's anaerobic threshold.
Vascular Function Testing
[0080] Vascular endothelial dysfunction is an important outcome for assessing vascular health in intervention studies. It is now well established that vascular endothelial dysfunction is positively associated with traditional cardiovascular disease (CVD) risk factors, and independently predicts cardiovascular events over intervals of 1 to 6 years.
[0081] Pulse amplitude tonometry (PAT), a FDA-approved method for assessing vascular function, is increasingly being used as an alternative measure of endothelium-dependent dilation in response to reactive hyperemia and flow-mediated dilation (FMD). The PAT device records digital pulse wave amplitude (PWA) using fingertip plethysmography. PWA can be measured continuously during three phases: a quiet baseline period, 5-min forearm occlusion, and reactive hyperemia following cuff release. Unlike FM D, PAT testing is not dependent upon a highly skilled technician and post-test analysis is largely automated. Most importantly, at least one longitudinal study has shown that PAT measures of endothelial function predict CVD events over a 6-year follow-up period. These significant advantages may make PAT testing suitable for clinical practice if prognostic significance and reliability can be verified.
[0082] Patients that have previously undergone a Fontan procedure will generally see a decline in vascular function over time. Treating a patient such that the patient's vascular function increases or preventing further decline in vascular function would indicate that the treatment is clinically beneficial and may improve patient quality of life or prevent decline in cardiovascular function.
[0083] In one embodiment, the invention is directed to a method of improving or maintaining vascular function of a subject who has previously had a Fontan procedure. The method comprises administering a therapeutically effective amount of a PDE5 inhibitor to the patient, where the PDE5 inhibitor is udenafil or a pharmaceutically acceptable salt thereof. In some embodiments, vascular function is measured using a PAT index.
[0084] In some embodiments, the disclosed methods and compositions are administered to a Fontan patient and result in no decrease, or a minimal decrease, in vascular function over time. Vascular function can be measured using any conventional known technique, including but not limited to pulse amplitude tonometry measurements, the natural log of reactive hyperemia index, Reactive Hyperemia Index, Framingham RHI, area under the curve to max-occlusion/control, average up to max-occlusion/control, and other known EndoPAT indices. In some embodiments, vascular function is measured using a PAT index. More specifically, the disclosed methods and compositions may result in a decrease in vascular function of less than about 40, less than about 35, less than about 30, less than about 35, less than about 20, less than about 15, less than about 10, or less than about 5% over time. The time period between a first and second measurement used to calculate the decrease in vascular function can be, for example, about 1, about 2, about 3, about 4, about 5, about 6, about 7, about 8, about 9, about 10, about 11, or about 12 months; about 1, about 2, about 3, about 4, about 5, about 6, about 7, about 8, about 9, about 10, about 11, about 12, about 13, about 14, or about 15 years, or any combination thereof, e.g., 1 year, 3 months; 4 years, 7 months, etc.
[0085] In some embodiments, the disclosed methods and compositions may be administered to a Fontan patient and result in an improvement of vascular function. Vascular function can be measured using any conventional known technique, including but not limited to pulse amplitude tonometry measurements, the natural log of reactive hyperemia index, Reactive Hyperemia Index, Framingham RHI, area under the curve to max-occlusion/control, average up to max-occlusion/control, and other known EndoPAT indices. In some embodiments, vascular function is measured using a PAT index. More specifically, the disclosed methods and compositions may result in about a 1, about 2, about 5, about 10, about 15, about 20, about 25, about 30, about 35, about 40, about 45, or about 50% or more improvement in one or more measurements of vascular function, including but not limited to pulse amplitude tonometry measurement, the natural log of reactive hyperemia index, Reactive Hyperemia Index, Framingham RHI, area under the curve to max-occlusion/control, average up to max-occlusion/control, and other known EndoPAT indices.
Echocardiographic Assessment of Ventricular Performance
[0086] Ventricular performance and cardiac contractility are important measurements that can reveal impairment of cardiovascular health before overt heart failure is present. Ventricular performance can be assessed using echocardiographic methods and quantified via a myocardial performance index or MPI. MPI is an index that combines systolic and diastolic function. Specifically, MPI is defined as the sum of isovolumic contraction time and isovolumic relaxation time divided by the ejection time.
[0087] Various versions of MPI are known in the art, and each version of MPI may be used to assess ventricular performance. For instance, MPI indices may include but are not limited to blood pool MPI, tissue doppler MPI, average isovolumetric contraction, and average isovolumetric relaxation.
[0088] Patients that have previously undergone a Fontan procedure will generally see a decline in ventricular performance over time. Treating a patient such that the patient's ventricular performance is maintained, exhibits minimal decrease over time, or increases indicates that the treatment is clinically beneficial and may improve patient quality of life or prevent decline in cardiovascular function.
[0089] In one embodiment, the invention is directed to a method of maintaining, producing a minimal decrease in, or increasing ventricular performance of a subject who has previously had a Fontan procedure. The method comprises administering a therapeutically effective amount of a PDE5 inhibitor to the patient, where the PDE5 inhibitor is udenafil or a pharmaceutically acceptable salt thereof. In some embodiments, ventricular performance is measured using a myocardial performance index (MPI). In some embodiments, the MPI may be a blood pool MPI, while in other embodiments the MPI may be a tissue doppler MPI.
[0090] In some embodiments, the disclosed methods and compositions may be administered to a Fontan patient and result in minimal or no decrease in ventricular performance over time. Ventricular performance can be measured using any conventional known technique, including but not limited to myocardial performance index (MPI), blood pool MPI, tissue doppler MPI, average isovolumetric contraction and relaxation, and other known ventricular performance indices. More specifically, the disclosed methods and compositions may result in a decrease in ventricular performance of less than about 40, less than about 35, less than about 30, less than about 35, less than about 20, less than about 15, less than about 10, or less than about 5% over time. The time period between a first and second measurement used to calculate the decrease in ventricular performance can be, for example, about 1, about 2, about 3, about 4, about 5, about 6, about 7, about 8, about 9, about 10, about 11, or about 12 months; about 1, about 2, about 3, about 4, about 5, about 6, about 7, about 8, about 9, about 10, about 11, about 12, about 13, about 14, or about 15 years, or any combination thereof, e.g., 1 year, 3 months; 4 years, 7 months, etc.
[0091] In some embodiments, the disclosed methods and compositions may be administered to a Fontan patient and result in an improvement of ventricular performance over time. Ventricular performance can be measured using any conventional known technique, including but not limited to myocardial performance index (MPI), blood pool MPI, tissue doppler MPI, average isovolumetric contraction and relaxation, and other known ventricular performance indices. For example, the disclosed methods and compositions may result in about a 1, about 2, about 5, about 10, about 15, about 20, about 25, about 30, about 35, about 40, about 45, or about 50% or more improvement in ventricular performance, as measured by any known technique, including but not limited to myocardial performance index (MPI), blood pool MPI, tissue doppler MPI, average isovolumetric contraction and relaxation, and other known ventricular performance indices.
III. Methods According to the Invention
[0092] In one embodiment, the invention is directed to methods of treating, preventing, or minimizing conditions, symptoms, or side effects associated with a subject who has previously had a Fontan procedure. The method comprises administering a therapeutically effective amount of a PDE5 inhibitor to the patient, where the PDE5 inhibitor is udenafil or a pharmaceutically acceptable salt thereof.
[0093] In the Fontan circulation, pulmonary blood flow is passive, driven by the pressure difference between the systemic venous circulation and the ventricular end-diastolic pressure. A medication capable of allowing for more efficient transit of blood through the pulmonary vascular bed can allow for improvement in cardiac preload, and therefore improve cardiac output.
[0094] PDE5 inhibitors are a class of medications that reduce pulmonary vascular resistance and improve ventricular performance in patients with pulmonary hypertension and myocardial dysfunction.
[0095] Some studies have evaluated the single-use or longer-term use of sildenafil in children and young adults who have had the Fontan procedure. However, sildenafil has a short half-life, and is typically administered three to four times per day. Such an administration schedule is not convenient and is likely to reduce patient compliance. In addition, the administration of a short half-life drug results in greater fluctuations of therapeutic levels of drug, increasing the risk that the blood level of the PDE5 inhibitor will drop below the therapeutically effective level for parts of the day. The present inventors hypothesize that administration of a PDE5 inhibitor having a longer half-life to patients who have had the Fontan procedure will prevent or ameliorate the decline in aerobic exercise performance in patients following the Fontan procedure.
[0096] Patient compliance is critical for optimal therapeutic efficacy, particularly for a drug that is to be taken daily for an extended period of time, such as for several years or more. This is particularly true for Fontan patients. In particular, individuals that had the Fontan procedure most often die from heart failure, stroke (thrombosis), or some unexplained sudden death. Of note is the fact that the risk of death from heart failure is quite low within 10 years of the Fontan procedure but increases with time after 10 years post-Fontan. http://bendantzer.wordpress.com/2013/03/13/fontan-circulation-success-or-- failure/.
[0097] Not surprisingly, as time passes from the date of the Fontan procedure, the risk of death or need from a heart transplant increases. This could be from some sudden death or heart failure, but it could also be from a gradual decline in heart function. As the years tick by after the Fontan procedure, heart function gets worse, which is reflected in the decline in the ability to do aerobic exercise. For example, for patients that had the Fontan early in life, they may have exercise capacity that is highly reduced (44%) compared to normal patients and this capacity to do exercise tends to decline in a linear fashion each year (declines 2.6% each year). At thirty years of age, patients with Fontan circulation have much reduced exercise capacity (55% less than normal) and the number of health problems and hospitalization rates increase dramatically. This is probably not surprising since, again, one ventricle is doing the work of two. Thus, methods according to the invention which can diminish or significantly decrease decline in heart function over time, are highly desirable for Fontan patients. Key to the success of such methods is patient compliance with a preferred dosing schedule.
[0098] Patient compliance, or lack thereof, to a prescribed dosing schedule is known to be a critical factor in the success of any therapy. In particular, quality healthcare outcomes depend upon patients' adherence to recommended treatment regimens. Patient nonadherence can be a pervasive threat to health and wellbeing and carry an appreciable economic burden as well. In some disease conditions, more than 40% of patients sustain significant risks by misunderstanding, forgetting, or ignoring healthcare advice. Moreover, when preventive or treatment regimens are very complex and/or require lifestyle changes and the modification of existing habits, nonadherence can be as high as 70%. Martin et al., Ther. Clin. Risk Manag., 1(3): 189-199 (2005) ("A significant barrier to effective medical treatment, however, is the patient's failure to follow the recommendations of his or her physician or other healthcare provider."). Thus, a therapy that can produce the desired results (e.g., improved cardiac output, decreased pulmonary vascular resistance, improved exercise capacity, improved myocardial performance, preventing or ameliorating the decline in aerobic exercise performance), with a preferred once or twice a day dosage, as compared to multiple daily dosages--e.g., 3 to 6.times. daily--required to be taken at least 4 to 6 hours apart, such as with sildenafil, is highly desirable. Such a more simplistic dosing regimen is likely to lead to a significant increase in patient compliance, and concomitant improved therapeutic results.
[0099] In one embodiment, the invention is directed to a method of improving cardiac output in a patient who has had the Fontan procedure, the method comprising administering a therapeutically effective amount of the PDE5 inhibitor udenafil, or a pharmaceutically acceptable salt thereof, to the patient. For example, the method of the invention can result in an improvement in cardiac output, as compared to a subject who is not administered udenafil, of about 5%, about 8%, about 10%, about 15%, about 20%, about 25%, about 30%, about 35%, about 40%, about 45%, or about 50%.
[0100] In another embodiment, the invention is directed to a method of decreasing pulmonary vascular resistance in a patient who has had the Fontan procedure, the method comprising administering a therapeutically effective amount of the PDE5 inhibitor udenafil, or a pharmaceutically acceptable salt thereof, to the patient. For example, the method of the invention can result in an decreased pulmonary vascular resistance, as compared to a subject who is not administered udenafil, of about 5%, about 8%, about 10%, about 15%, about 20%, about 25%, about 30%, about 35%, about 40%, about 45%, or about 50%.
[0101] In yet another embodiment, the invention is directed to a method of improving exercise capacity in a patient who has had the Fontan procedure, the method comprising administering a therapeutically effective amount of the PDE5 inhibitor udenafil, or a pharmaceutically acceptable salt thereof, to the patient. For example, the method of the invention can result in an increase in exercise capacity measured by maximal VO2, as compared to a subject who is not administered udenafil, of about 5%, about 8%, about 10%, about 15%, about 20%, about 25%, about 30%, about 35%, about 40%, about 45%, or about 50%.
[0102] In one embodiment, the invention is directed to a method of improving myocardial performance in a patient who has had the Fontan procedure, the method comprising administering a therapeutically effective amount of a PDE5 inhibitor to the patient. For example, the method of the invention can result in an improvement in myocardial performance, as compared to a subject who is not administered udenafil, of about 5%, about 8%, about 10%, about 15%, about 20%, about 25%, about 30%, about 35%, about 40%, about 45%, or about 50%.
[0103] In one embodiment, the invention is directed to a method of preventing or ameliorating the decline in aerobic exercise performance in a patient who has had the Fontan procedure, the method comprising administering a therapeutically effective amount of the PDE5 inhibitor udenafil, or a pharmaceutically acceptable salt thereof, to the patient. For example, the method of the invention can result in an amelioration of the decline in aerobic exercise performance measured by maximal VO2, as compared to a subject who is not administered udenafil, of about 5%, about 8%, about 10%, about 15%, about 20%, about 25%, about 30%, about 35%, about 40%, about 45%, or about 50%.
[0104] In yet another embodiment, the invention is directed to improved methods for treating a patient who has had a Fontan procedure, wherein the methods show an improvement in patient compliance with a dosing schedule of udenafil or a pharmaceutically acceptable salt thereof, as compared to patients prescribed a non-udenafil drug.
[0105] Udenafil has a half-life of 7.3-12.1 hours, and is believed to possibly have a much better safety profile as compared to sildenafil or tadalafil. Udenafil has unique properties, with a T.sub.max of 1.0-1.5 h and a T.sub.1/2 of 11-13 h (a relatively rapid onset and a long duration of action). Therefore, both on-demand and once-daily use of udenafil have been reported. Udenafil's efficacy and tolerability have been evaluated in several studies, and recent and continuing studies have demonstrated udenafil's promise in both dosing regimens. Presently, tadalafil is the only FDA-approved drug for daily dosing, but udenafil can be used as a once-daily dose for erectile dysfunction patients who cannot tolerate tadalafil due to phosphodiesterase subtype selectivity. Gu Kang et al., Ther. Adv. Urol., 5(2): 101-110 (2013). Once-daily dosing of udenafil was evaluated for the treatment of erectile dysfunction (ED), and the results showed that udenafil significantly improved erectile function among ED patients when administered in doses of 50 mg or 75 mg once daily for 12 wk. Zhao et al., Eur. J. of Urology, 60: 380-387 (2011). While these reports suggest that udenafil may be useful as a once a day therapy for various conditions, other reports show that PDE5 inhibitors show varying efficacy in treating symptoms associated with the Fontan operation. Sabri et al., Pediatr. Cardiol., 35(4):699-704 (2014).
[0106] Thus, it was surprising that the present invention, directed to methods of treating, minimizing, and/or preventing symptoms associated with the Fontan operation comprising administering udenafil or a pharmaceutically acceptable salt thereof, shows desirable results, preferably with a once or twice a day dosage. "Desirable results" include, but are not limited to, improved cardiac output, decreased pulmonary vascular resistance, improved exercise capacity, improved myocardial performance, preventing or ameliorating the decline in aerobic exercise performance, and/or an improvement in patient compliance.
[0107] In one embodiment of the invention, once a day administration of a therapeutically effective dosage of uldenafil, or a pharmaceutically acceptable salt thereof, results in therapeutic levels of uldenafil, present in the patient's blood stream, for up to about 8 hours. In other embodiments of the invention, once a day administration of a therapeutically effective dosage of uldenafil, or a pharmaceutically acceptable salt thereof, results in therapeutic levels of uldenafil, present in the patient's blood stream, for up to about 10, about 11, about 12, about 13, about 14, about 15, about 16, about 17, about 18, about 19, about 20, about 21, about 22, about 23, or about 24 hours.
[0108] In one embodiment of the invention, twice a day administration of a therapeutically effective dosage of udenafil, or a pharmaceutically acceptable salt thereof, results in therapeutic levels of udenafil for at least about 16 hours in a 24 hour dosing period. In other embodiments, twice a day administration of a therapeutically effective dosage of udenafil, or a pharmaceutically acceptable salt thereof, results in therapeutic levels of udenafil for at least about 9 hours, about 10 hours, about 11 hours, about 12 hours, about 13 hours, about 14 hours, about 15 hours, about 16 hours, about 17 hours, about 18 hours, about 19 hours, about 20 hours, about 21 hours, about 22 hours, about 23 hours, or about 24 hours, in a 24 hour dosing period.
[0109] In another embodiment, it was surprising that that the methods of the invention show improved results as compared to prior art treatments using a non-udenafil PDE5 inhibitor, such as sildenafil or tadalafil. In yet another embodiment, it was surprising that the methods of the invention show fewer side effects, and/or less severe side effects, as compared to prior art treatments using a non-udenafil PDE5 inhibitor, such as sildenafil or tadalafil.
[0110] In one embodiment, it is surprising that the administration of twice a day udenafil or a pharmaceutically acceptable salt thereof results in fewer side effects than the administration of once a day udenafil or a pharmaceutically acceptable salt thereof. In another embodiment, it is surprising that twice a day administration of udenafil or a pharmaceutically acceptable salt thereof can achieve therapeutically effective levels of udenafil at a lower total daily dosage than a once a day administration.
[0111] In one embodiment, the patient who has had the Fontan procedure is a human patient. In one embodiment, the patient is an adult human patient over about 18 years of age. In another embodiment, the patient is a pediatric patient of about 2 to about 18 years of age. In another embodiment, the patient is a pediatric patient of about 12 to about 18 years of age, or from about 12 to about 16 years of age.
IV. Pediatric Patients
[0112] Treatment of pediatric patients presents particular challenges, as pediatric physiology is not just a miniature version of an adult. Physical size is just one of the many differences. Children's body surface area, organ and system maturity and function, as well as cognitive and emotional development can result in differences in response to illness, diagnosis, treatment, and medications. Even illnesses that are seen in adults can act differently in children because of their unique anatomy and physiology. Moreover, pediatric patients process drugs differently than adults, and therefore the effects as well as the dosages of drugs may vary widely from those observed with adults. Since children differ from adults in many ways beyond size, simply adjusting the dose of a drug for a smaller size person will not necessarily produce the same response and can lead to adverse drug reactions. Thus, the effectiveness of a drug used in treating an adult condition does not with certainty predict success of treating a pediatric patient with the same drug.
[0113] Thus, the invention is also directed to the surprising discovery that pediatric Fontan patients can be successfully treated with the methods of the invention. The methods comprise administering a therapeutically effective amount of a PDE5 inhibitor to the pediatric patient, where the PDE5 inhibitor is udenafil or a pharmaceutically acceptable salt thereof.
[0114] The structure of udenafil is shown below:
##STR00003##
V. Doses and Dosage Forms
[0115] In one embodiment, the udenafil or a pharmaceutically acceptable salt thereof is administered at total daily dosage amounts of about 0.01 to about 150 mg/kg. In another embodiment, the udenafil or a pharmaceutically acceptable salt thereof is administered at total daily doses of about 0.01 mg/kg up to about 30 mg/kg. In another embodiment, the udenafil or a pharmaceutically acceptable salt thereof is administered at total daily doses of about 5 mg, about 10 mg, about 15 mg, about 20 mg, about 25 mg, about 27.5 mg, about 30 mg, about 32.5, about 35 mg, about 37.5 mg, about 40 mg, about 42.5 mg, about 45 mg, about 47.5 mg, about 50 mg, about 55 mg, about 60 mg, about 65 mg, about 70 mg, about 75 mg, about 80 mg, about 85 mg, about 87.5 mg, about 90 mg, about 95 mg, about 100 mg, about 125 mg, about 150 mg, about 175 mg, about 200 mg, about 225 mg, about 250 mg, or about 275 mg. In one embodiment, the udenafil or a pharmaceutically acceptable salt thereof is administered in total daily doses of about 25 mg, about 37.5 mg, about 50 mg, about 75 mg, about 87.5 mg, 125 mg, about 175 mg, about 200 mg, about 225 mg, about 250 mg, about 275 mg, about 300 mg, about 325 mg, about 350 mg, about 375 mg, about 400 mg, about 425 mg, about 450 mg, about 475 mg, about 500 mg, about 525 mg, about 550 mg, about 575 mg, about 600 mg, about 625 mg, about 650 mg, about 675 mg, or about 700 mg. In another particular embodiment, udenafil or a pharmaceutically acceptable salt thereof is administered at a total daily dose of about 37.5 mg, about 75 mg, about 87.5 mg, 125 mg, or about 175 mg.
[0116] In one embodiment, the udenafil or a pharmaceutically acceptable salt thereof is administered once a day.
[0117] In another embodiment, the udenafil or a pharmaceutically acceptable salt thereof is administered twice a day. In one embodiment, the udenafil or a pharmaceutically acceptable salt thereof is administered twice a day such that therapeutically effective blood levels are maintained for at least about 18, about 19, about 20, about 21, about 22, about 23 or about 24 hours of a 24 hour dosing period. In some embodiments, the total daily dosage amount of udenafil or a pharmaceutically acceptable salt administered twice a day is less than the total daily dosage amount of udenafil or a pharmaceutically acceptable salt thereof administered once a day. In some embodiments, the total daily dosage amount of udenafil or a pharmaceutically acceptable salt thereof administered twice a day, maintains therapeutically effective blood levels for the same number of hours in a 24 hour period as a higher dosage of udenafil or a pharmaceutically acceptable salt thereof when administered once a day. In other embodiments, the total daily dosage amount of udenafil or a pharmaceutically acceptable salt thereof administered twice a day, maintains therapeutically effective blood levels for a higher number of hours in a 24 hour period as the same dosage of udenafil or a pharmaceutically acceptable salt thereof when administered once a day.
[0118] In some embodiments, the udenafil or a pharmaceutically acceptable salt thereof administered twice a day produces a greater reduction in the conditions, symptoms, or side effects associated with a subject who has previously had a Fontan procedure, when compared to udenafil or a pharmaceutically acceptable salt thereof administered once a day.
[0119] In some embodiments, the pharmaceutically acceptable salt of udenafil is an acid addition salt. In one embodiment, the acid addition salt of udenafil is an inorganic acid addition salt such as, hydrochloric, hydrobromic, sulfuric, or phosphoric acid addition salt. In another embodiment, the acid addition salt is an organic acid addition salt such as citrate, tartarate, acetate, lactate, maleate, fumarate, gluconate, methanesulfonate (mesylate), glycolate, succinate, p-toluenesulfonate (tosylate), galacturonate, embonate, glutamate, aspartate, oxalate, benzensulfonate, camphorsulfonate, cinnamate, adipate, or cyclamate. In a particular embodiment, the pharmaceutically acceptable salt of udenafil is an oxalate, benzensulfonate, camphorsulfonate, cinnamate, adipate, or cyclamate salt.
[0120] In one embodiment the udenafil or a pharmaceutically acceptable salt thereof is administered as a pharmaceutical composition. In one embodiment, the pharmaceutical composition comprising udenafil or a pharmaceutically acceptable salt thereof can be formulated in a wide variety of oral or parenteral dosage forms on clinical application. Each of the dosage forms can contain various disintegrating agents, surfactants, fillers, thickeners, binders, diluents such as wetting agents or other pharmaceutically acceptable excipients.
[0121] The udenafil composition can be administered using any pharmaceutically acceptable method, such as intranasal, buccal, sublingual, oral, rectal, ocular, parenteral (intravenously, intradermally, intramuscularly, subcutaneously, intracisternally, intraperitoneally), pulmonary, intravaginal, locally administered, topically administered, topically administered after scarification, mucosally administered, via an aerosol, or via a buccal or nasal spray formulation.
[0122] Further, the udenafil composition can be formulated into any pharmaceutically acceptable dosage form, such as a solid dosage form, tablet, pill, lozenge, capsule, liquid dispersion, gel, aerosol, pulmonary aerosol, nasal aerosol, ointment, cream, semi-solid dosage form, and a suspension. Further, the composition may be a controlled release formulation, sustained release formulation, immediate release formulation, or any combination thereof. Further, the composition may be a transdermal delivery system.
[0123] In another embodiment, the pharmaceutical composition comprising udenafil or a pharmaceutically acceptable salt thereof can be formulated in a solid dosage form for oral administration, and the solid dosage form can be powders, granules, capsules, tablets or pills. In yet another embodiment, the solid dosage form can include one or more excipients such as calcium carbonate, starch, sucrose, lactose, microcrystalline cellulose or gelatin. In addition, the solid dosage form can include, in addition to the excipients, a lubricant such as talc or magnesium stearate. In some embodiments, the oral dosage form can be immediate release, or a modified release form. Modified release dosage forms include controlled or extended release, enteric release, and the like. The excipients used in the modified release dosage forms are commonly known to a person of ordinary skill in the art.
[0124] In a further embodiment, the pharmaceutical composition comprising udenafil or a pharmaceutically acceptable salt thereof can be formulated as a sublingual or buccal dosage form. Such dosage forms comprise sublingual tablets or solution compositions that are administered under the tongue and buccal tablets that are placed between the cheek and gum.
[0125] In yet a further embodiment, the pharmaceutical composition comprising udenafil or a pharmaceutically acceptable salt thereof can be formulated as a nasal dosage form. Such dosage forms of the present invention comprise solution, suspension, and gel compositions for nasal delivery.
[0126] In one embodiment, the pharmaceutical composition can be formulated in a liquid dosage form for oral administration, such as suspensions, emulsions or syrups. In other embodiments, the liquid dosage form can include, in addition to commonly used simple diluents such as water and liquid paraffin, various excipients such as humectants, sweeteners, aromatics or preservatives. In particular embodiments, the composition comprising udenafil or a pharmaceutically acceptable salt thereof can be formulated to be suitable for administration to a pediatric patient.
[0127] In one embodiment, the pharmaceutical composition can be formulated in a dosage form for parenteral administration, such as sterile aqueous solutions, suspensions, emulsions, non-aqueous solutions or suppositories. In other embodiments, the non-aqueous solutions or suspensions can include propyleneglycol, polyethyleneglycol, vegetable oils such as olive oil or injectable esters such as ethyl oleate. As a base for suppositories, witepsol, macrogol, tween 61, cacao oil, laurin oil or glycerinated gelatin can be used.
[0128] The dosage of the pharmaceutical composition can vary depending on the patient's weight, age, gender, administration time and mode, excretion rate, and the severity of disease.
VI. Adverse Events
[0129] Adverse events are an important consideration, particularly when treating a susceptible population such as pediatric patients with Fontan physiology. PDE-5 inhibitors may produce adverse events including eye and/or hearing issues. Therefore, developing methods in which PDE-5 inhibitors such as udenafil or a pharmaceutically acceptable salt thereof can safely be administered to pediatric patients is one aspect of the invention.
[0130] In some embodiments, a pediatric patient with Fontan physiology may be administered a PDE-5 inhibitor to treat, minimize, and/or prevent the deleterious effects of Fontan physiology.
[0131] In some embodiments, administering the PDE-5 inhibitor, specifically udenafil or a pharmaceutically acceptable salt thereof, results in minimal if any serious adverse events. In other embodiments, administering the PDE-5 inhibitor, specifically udenafil or a pharmaceutically acceptable salt thereof, results in minimal if any unexpected adverse events.
[0132] In some embodiments, a pediatric patient with Fontan physiology being administered udenafil or a pharmaceutically acceptable salt thereof may experience only mild adverse events related to the medication, and in other embodiments, the patient may experience only moderate adverse events related to the medication. In some embodiments, a pediatric patient with Fontan physiology being administered udenafil or a pharmaceutically acceptable salt thereof may experience fewer, less frequent, or less severe adverse events compared to a Fontan patient receiving another PDE-5 inhibitor.
VII. Pharmacokinetic Parameters
[0133] Pharmacokinetics refers to the absorption, distribution, metabolism, and excretion of a drug once it has been administered to a subject. The kinetics of a drug have an impact on the drug's efficacy and toxicity. A given drug's kinetic profile can depend not only on the compound itself, but also on the size of the dose and the dosing regimen as well as how the drug is formulated and administered. Pharmacokinetic parameters that may be useful in determining clinical utility include but are not limited to plasma concentration, plasma concentration over time, maximum plasma concentration (C.sub.max), time to reach maximum concentration (T.sub.max), area under concentration time curve within the dosing interval (AUC.sub..tau.), daily area under concentration time curve at steady state (AUC.sub.0-24); CL/F, apparent clearance; V/F, apparent volume of distribution; ke, elimination rate constant; T1/2, terminal half-life.
[0134] In some embodiments, the disclosed invention is directed to methods of administering udenafil or a pharmaceutically acceptable salt thereof to a patient with Fontan physiology, wherein the administration results in a unique pharmacokinetic profile. For instance, in some embodiments the disclosed methods can produce plasma concentrations of udenafil ranging from about 10 to about 700 ng/ml, about 50 to about 650 ng/ml, about 100 to about 600 ng/ml, about 150 to about 550 ng/ml, or about 200 to about 500 ng/ml. In other words, dosing regimens of the disclosed methods may result in sustained plasma concentrations of udenafil above 25, 50, 75, 100, 125, 150, 175, 200, 225, 250, 275, 300, 325, 350, 375, 400, 425, 450, 475, 500, 525, 550, 575, 600, 625, 650, 675, or 700 ng/ml. In some embodiments, the plasma concentration is maintained above about 140 ng/ml.
[0135] In some embodiments, the disclosed methods include a characteristic pharmacokinetic profile in which the C.sub.max is about 25, about 50, about 75, about 100, about 125, about 150, about 175, about 200, about 225, about 250, about 275, about 300, about 325, about 350, about 375, about 400, about 425, about 450, about 475, about 500, about 525, about 550, about 575, about 600, about 625, about 650, about 675, or about 700 ng/ml. In some embodiments, the C.sub.m, is about 506.
[0136] In some embodiments, the disclosed methods include a characteristic pharmacokinetic profile in which the T.sub.m, is about 0.1, 0.2, 0.3, 0.4, 0.5, 0.6, 0.7, 0.8, 0.9, 1.0, 1.1, 1.2, 1.3, 1.4, 1.5, 1.6, 1.7, 1.8, 1.9, 2.0, 2.1, 2.2, 2.3, 2.4, 2.5, 2.6, 2.7, 2.8, 2.9, or 3.0 hours (hr). In some embodiments, the T.sub.max is about 1.3 hr.
[0137] In some embodiments, the disclosed methods include a characteristic pharmacokinetic profile in which the area under the curve (AUC) is unique to a therapeutically effective dose of udenafil in a Fontan's patient. For instance AUC.tau. is between 750 and 4500 nghr/ml, 800-4000 nghr/ml, or 850-3500 nghr/ml. More specifically AUC.tau. is about 750, about 800, about 850, about 900, about 950, about 1000, about 1050, about 1100, about 1150, about 1200, about 1250, about 1300, about 1400, about 1500, about 1600, about 1700, about 1800, about 1900, about 2000, about 2100, about 2200, about 2300, about 2400, about 2500, about 2600, about 2700, about 2800, about 2900, about 3000, about 3100, about 3200, about 3300, about 3400, about 3500, about 3600, about 3700, about 3800, about 3900, about 4000, about 4100, about 4200, about 4300, about 4400, or about 4500 nghr/ml. In some embodiments, the AUC.sub..tau. is about 3350.
[0138] In some embodiments, AUC.sub.0-24 is between 750 and 8500 nghr/ml, 800-8000 nghr/ml, or 850-7500 nghr/ml. More specifically AUC.sub.0-24 is about 750, about 800, about 850, about 900, about 950, about 1000, about 1050, about 1100, about 1150, about 1200, about 1250, about 1300, about 1400, about 1500, about 1600, about 1700, about 1800, about 1900, about 2000, about 2100, about 2200, about 2300, about 2400, about 2500, about 2600, about 2700, about 2800, about 2900, about 3000, about 3100, about 3200, about 3300, about 3400, about 3500, about 3600, about 3700, about 3800, about 3900, about 4000, about 4100, about 4200, about 4300, about 4400, about 4500, about 4600, about 4700, about 4800, about 4900, about 5000, about 5100, about 5200, about 5300, about 5400, about 5500, about 5600, about 5700, about 5800, about 5900, about 6000, about 6100, about 6200, about 6300, about 6400, about 6500, about 6600, about 6700, about 6800, about 6900, about 7000, about 7100, about 7200, about 7300, about 7400, about 7500, about 7600, about 7700, about 7800, about 7900, about 8000, about 8100, about 8200, about 8300, about 8400, or about 8500 nghr/ml. In some embodiments, the AUC.sub.0-24 is about 6700.
[0139] In some embodiments, the pharmacodynamics results of administering udenafil to a patient with Fontan's physiology can be attributed to the characteristic pharmacokinetic profile of the drug administration or regimen.
VIII. Definitions
[0140] As used herein, the term "about" will be understood by persons of ordinary skill in the art and will vary to some extent depending upon the context in which it is used. If there are uses of the term which are not clear to persons of ordinary skill in the art given the context in which it is used, "about" will mean up to plus or minus 10% of the particular term.
[0141] "A treatment" is intended to target the disease state and combat it, i.e., ameliorate or prevent the disease state. The particular treatment thus will depend on the disease state to be targeted and the current or future state of medicinal therapies and therapeutic approaches. A treatment may have associated toxicities.
[0142] The terms "administration of" or "administering" an active agent should be understood to mean providing an active agent of the invention to the subject in need of treatment in a form that can be introduced into that individual's body in a therapeutically useful form and therapeutically effective amount.
[0143] The term "therapeutically effective amount" refers to a sufficient quantity of the active agents of the present invention, in a suitable composition, and in a suitable dosage form to treat or prevent the symptoms, progression, or onset of the complications seen in patients who have had the Fontan procedure. The therapeutically effective amount will vary depending on the state of the patient's condition or its severity, and the age, weight, etc., of the subject to be treated. A therapeutically effective amount can vary, depending on any of a number of factors, including, e.g., the route of administration, the condition of the subject, as well as other factors understood by those in the art.
[0144] The term "treatment" or "treating" generally refers to an intervention in an attempt to alter the natural course of the subject being treated, and can be performed either for prophylaxis or during the course of clinical pathology. Desirable effects include, but are not limited to, preventing occurrence or recurrence of disease, alleviating symptoms, suppressing, diminishing or inhibiting any direct or indirect pathological consequences of the disease, ameliorating or palliating the disease state, and causing remission or improved prognosis.
[0145] The terms "individual," "host." "subject," and "patient" are used interchangeably herein.
[0146] As used herein, "improving cardiac output" means an increase in the volume of blood pumped by the heart. The cardiac output is commonly measured as a function of the oxygen consumption.
[0147] As used herein, the term "exercise capacity" refers to the maximum amount of physical exertion that a patient can sustain. Exercise capacity can be measured by a number of different clinical methods, including by interview or by direct measurement. The present methods include different methods of measuring exercise capacity, including but not limited to, riding a cycle ergometer or walking on a treadmill. Thus, the term "improving exercise capacity" means increasing the ability of the patient to perform any level of physical exertion or exercise.
[0148] As used herein, the term "decreasing pulmonary vascular resistance" refers to decreasing or reducing the resistance offered by lung vasculature to blood flow.
[0149] As used herein, "improving myocardial performance" refers to an increase or decrease, as the case can be, in specific heart function measurements, including but not limited to, specific electrocardiographic readings, echocardiographic readings, cardiac output measures, heart rate, systolic or diastolic pressure, forced vital capacity, oxygen saturation, and respiratory rate.
[0150] As used herein, "aerobic exercise performance" refers to the ability of a patient to perform a specified aerobic exercise.
[0151] As used herein, "pediatric" refers to a population of subjects ranging between a newborn and about 18 years of age. A pediatric subject can include a subject that begins a course of treatment with the disclosed compositions or according to the disclosed methods prior to turning about 18 years of age, even if the subject continues treatment beyond 18 years of age. More specifically, within the population of "pediatric" subjects, neonates may be defined as 1 week to 1 month in age, infants may be 1 to less than 2 years of age, toddlers may be 2 to less than 6 years of age, and school age may refer to subjects 6-18 years of age.
[0152] The following examples are given to illustrate the present invention. It should be understood, however, that the invention is not to be limited to the specific conditions or details described in these examples. All printed publications referenced herein are specifically incorporated by reference.
EXAMPLES
Example 1--Phase I/II Pharmacokinetic and Pharmacodynamic Study
[0153] A Phase I/II dose escalation trial of Udenafil in adolescents with single ventricle physiology after Fontan palliation was conducted.
[0154] The trial was conducted over a 5 month period, with an additional 3 month follow-up period for adverse events (AE). The 36 subjects enrolled in the trial were comprised of 6 cohorts, as described in Table 1.
TABLE-US-00001 TABLE 1 Dose escalation design Cohort 1 Cohort 2 Cohort 3 Cohort 4 Cohort 5 Cohort 6 Dose 37.5 mg 37.5 mg 87.5 mg 87.5 mg 125 mg Control daily twice daily daily twice daily daily (no drug) N 6 6 6 6 6 6
[0155] The goals for this trial were to assess the safety of udenafil at multiple dose levels over a five-day period, the pharmacokinetic profile of udenafil in adolescents with Fontan physiology, and the short-term effect of udenafil on pharmacodynamic measures of exercise capacity, ventricular performance, and vascular function.
[0156] Multiple doses of udenafil or a pharmaceutically acceptable salt thereof were administered to male and female Fontan patients who are 14-18 years of age.
[0157] Inclusion Criteria for the trial were: [0158] Males and females with Fontan physiology who are 14-18 years of age. [0159] Willingness to return to center to complete blood draws and exercise tests as described in the study protocol. [0160] Patients must agree to abstain from alcohol, caffeinated beverages, and grapefruit juice for the duration of the trial. [0161] Informed assent from subject and informed consent from parent/legal guardian as appropriate.
[0162] Exclusion Criteria for the study include: [0163] Non-cardiac medical, psychiatric, and/or social disorder that would prevent successful completion of planned study testing or would invalidate its results. [0164] Height <132 cm (minimum height requirement for exercise stress testing). [0165] Known Fontan baffle obstruction, branch pulmonary artery stenosis, or pulmonary vein stenosis resulting in a mean gradient of >4 mmHg between the regions proximal and distal to the obstruction. [0166] Single lung physiology. [0167] Severe ventricular dysfunction or valvular regurgitation (systemic atrioventricular or semilunar valve) determined from review of the echocardiogram performed in closest proximity to study enrollment. [0168] Significant renal (serum creatinine >2.0), hepatic (serum AST and/or ALT >3 times upper limit of normal), gastrointestinal or biliary disorders that could impair absorption, metabolism or excretion of orally administered medications, based on laboratory assessment at the time of screening visit. [0169] Hospitalization for acute decompensated heart failure within the 12 months preceding study screening. [0170] A diagnosis of active protein-losing enteropathy or plastic bronchitis. [0171] Active evaluation or listing for heart transplant. [0172] History of use of a PDE5 inhibitor within three months of study screening. [0173] Concurrent illness that, in the opinion of the investigator, precludes participation. [0174] Current therapy with alpha-blockers or nitrates. [0175] Pregnancy at the time of enrollment. [0176] Latex allergy.
[0177] Table 2 presents baseline characteristics of 36 enrolled subjects--in aggregate (2nd column) and for each of the 6 individual cohorts. Median age of enrolled subjects is 16 years (with the range from 14 to 18 years), 58% were male, 78% were white and 6% were Hispanic. There were no significant differences in baseline characteristics among the cohorts (right column).
TABLE-US-00002 TABLE 2 Baseline Characteristics for Enrolled Subjects Exercise 37.5 mg 87.5 mg 87.5 mg 125 mg testing P- Overall 37.5 mg twice daily daily twice daily daily only value Characteristic (N = 36) daily (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) * Age, year 15.8 .+-. 1.3 15.5 .+-. 1.0 16.2 .+-. 0.8 15.0 .+-. 0.9 15.5 .+-. 1.8 16.5 .+-. 1.5 16.2 .+-. 1.2 0.319 Median 16 (15, 17) 16 (15, 16) 16 (16, 17) 15 (14, 16) 15 (14, 17) 17 (16, 18) 16 (15, 17) 0.309 (Interquartile Range) Range, Min- 14-18 14-17 15-17 14-16 14-18 14-18 15-18 Max Male 21 (58.3%) 4 (66.7%) 3 (50.0%) 3 (50.0%) 3 (50.0%) 4 (66.7%) 4 (66.7%) 1.000 Hispanic or 2 (5.7%) 1 (16.7%) 1 (16.7%) 0 (0.0%) 0 (0.0%) 0 (0.0%) 0 (0.0%) 1.000 Latino/Latina Race 0.453 White/Caucasian 28 (77.8%) 3 (50.0%) 4 (66.7%) 6 (100.0%) 6 (100.0%) 4 (66.7%) 5 (83.3%) Black/African 3 (8.3%) 2 (33.3%) 1 (16.7%) 0 (0.0%) 0 (0.0%) 0 (0.0%) 0 (0.0%) American Other/Unknown 4 (11.1%) 1 (16.7%) 1 (16.7%) 0 (0.0%) 0 (0.0%) 1 (16.7%) 1 (16.7%) Weight, cm 165.7 .+-. 10.1 161.0 .+-. 12.9 164.9 .+-. 10.9 168.6 .+-. 7.8 164.7 .+-. 14.2 171.3 .+-. 7.8 163.6 .+-. 5.6 0.585 Weight, kg 62.4 .+-. 15.9 72.5 .+-. 27.1 56.3 .+-. 7.7 66.8 .+-. 11.0 62.0 .+-. 15.5 61.9 .+-. 9.0 54.9 .+-. 16.8 0.425 Body mass 22.6 .+-. 5.0 27.2 .+-. 8.1 20.8 .+-. 3.2 23.4 .+-. 3.2 22.6 .+-. 4.8 21.0 .+-. 2.0 20.3 .+-. 4.8 0.157 index, kg/m.sup.2 *P-values for continuous variables were calculated by ANOVA for parametric analysis or Kruskal-Wallis test for non-parametric analysis. P-values for categorical variables were calculated by Fisher's exact test.
Example 2--Safety and Adverse Events
[0178] The purpose of this example was to describe and evaluate the safety of the udenafil compositions administered in the study described in Example 1.
[0179] Tables 3-6 present numbers of subjects reporting at least one AE; data are presented by treatment group. The counts are presented by AE category (Table 3) and by preferred term (Table 6). Tables 3-6 report all AEs by category (Table 3), serious AEs (Table 4), non-serious AEs (Table 5), and all AEs by preferred term (Table 6). No serious AEs were reported.
TABLE-US-00003 TABLE 3 Adverse Events by Category Exercise 37.5 mg 37.5 mg 87.5 mg 87.5 mg 125 mg testing daily twice daily daily twice daily daily only AE Category (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) Subjects Reporting at Least One 5 (83%) 6 (100%) 6 (100%) 5 (83%) 6 (100%) 1 (17%) Adverse Event Allergy/Immunology 1 (17%) 0 (0%) 1 (17%) 0 (0%) 0 (0%) 0 (0%) Auditory/ocula 0 (0%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) Cardiovascular 0 (0%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) 1 (17%) Endocrine/metabolic 0 (0%) 0 (0%) 0 (0%) 0 (0%) 1 (17%) 0 (0%) Gastrointestinal 2 (33%) 1 (17%) 1 (17%) 1 (17%) 3 (50%) 0 (0%) Hematological 0 (0%) 1 (17%) 0 (0%) 0 (0%) 1 (17%) 0 (0%) Hepatobiliary/pancreas 0 (0%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) Infection 0 (0%) 0 (0%) 0 (0%) 1 (17%) 0 (0%) 0 (0%) Musculoskeletal/skin 1 (17%) 1 (17%) 1 (17%) 2 (33%) 2 (33%) 0 (0%) Neurological/psychiatric 3 (50%) 3 (50%) 5 (83%) 2 (33%) 5 (83%) 0 (0%) Pulmonary/upper respiratory 2 (33%) 3 (50%) 1 (17%) 1 (17%) 1 (17%) 0 (0%) Renal/genitourinary 0 (0%) 2 (33%) 1 (17%) 0 (0%) 0 (0%) 0 (0%) Sexual/reproductive function 0 (0%) 0 (0%) 0 (0%) 2 (33%) 2 (33%) 0 (0%) Vascular 1 (17%) 2 (33%) 4 (67%) 1 (17%) 1 (17%) 0 (0%) Other 0 (0%) 2 (33%) 4 (67%) 3 (50%) 2 (33%) 0 (0%) At each level of summation, subjects reporting more than one adverse event are counted only once. N = number of subjects in each cohort. n (%) = number and percentage of subjects in category and cohort (n/N .times. 100)
TABLE-US-00004 TABLE 4 Serious Adverse Events 37.5 mg 37.5 mg 87.5 mg 87.5 mg 125 mg Exercise daily twice daily daily twice daily daily testing only AE Category (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) Subjects Reporting at Least One 0 (0%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) Adverse Event Serious adverse events were not reported for this trial. At each level of summation, subjects reporting more than one adverse event are counted only once. N = number of subjects in each cohort. n(%) = number and percentage of subjects in category and cohort (n/N .times. 100)
TABLE-US-00005 TABLE 5 Non-Serious Adverse Events 37.5 mg 37.5 mg 87.5 mg 87.5 mg 125 mg Exercise daily twice daily daily twice daily daily testing only AE Category (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) Subjects Reporting at Least One 5 (83%) 6 (100%) 6 (100%) 5 (83%) 6 (100%) 1 (17%) Adverse Event At each level of summation, subjects reporting more than one adverse event are counted only once. N = number of subjects in each cohort. n(%) = number and percentage of subjects in category and cohort (n/N .times. 100)
TABLE-US-00006 TABLE 6 Adverse Events by Preferred Term 37.5 mg 87.5 mg Exercise 37.5 mg twice 87.5 mg twice 125 mg testing daily daily daily daily daily only Preferred Term (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) Subjects Reporting, at Least 5 (83%) 6 (100%) 6 (100%) 5 (83%) 6 (100%) 1 (17%) One Adverse Event Abdominal discomfort 1 (17%) 0 (0%) 0 (0%) 1 (17%) 1 (17%) 0 (0%) Abdominal pain upper 0 (0%) 0 (0%) 0 (0%) 0 (0%) 1 (17%) 0 (0%) Back pain 0 (0%) 0 (0%) 0 (0%) 1 (17%) 0 (0%) 0 (0%) Chest pain 0 (0%) 0 (0%) 0 (0%) 0 (0%) 1 (17%) 0 (0%) Diarrhoea 0 (0%) 0 (0%) 0 (0%) 0 (0%) 1 (17%) 0 (0%) Dizziness 0 (0%) 0 (0%) 0 (0%) 1 (17%) 1 (17%) 0 (0%) Dry mouth 0 (0%) 0 (0%) 1 (17%) 0 (0%) 0 (0%) 0 (0%) Dysmenorrhoea 0 (0%) 1 (17%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) Dyspnoea 1 (17%) 1 (17%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) Epistaxis 0 (0%) 1 (17%) 0 (0%) 0 (0%) 2 (33%) 0 (0%) Face oedema 0 (0%) 0 (0%) 0 (0%) 0 (0%) 1 (17%) 0 (0%) Fatigue 0 (0%) 1 (17%) 0 (0%) 1 (17%) 0 (0%) 0 (0%) Flushing 1 (17%) 2 (33%) 4 (67%) 2 (33%) 1 (17%) 0 (0%) Head injury 0 (0%) 0 (0%) 1 (17%) 0 (0%) 0 (0%) 0 (0%) Headache 3 (50%) 4 (67%) 4 (67%) 4 (67%) 5 (83%) 0 (0%) Injection site pain 1 (17%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) Lacrimation increased 0 (0%) 0 (0%) 1 (17%) 0 (0%) 0 (0%) 0 (0%) Migraine 0 (0%) 0 (0%) 0 (0%) 0 (0%) 1 (17%) 0 (0%) Motion sickness 0 (0%) 0 (0%) 1 (17%) 0 (0%) 0 (0%) 0 (0%) Myalgia 0 (0%) 1 (17%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) Nasal congestion 3 (50%) 2 (33%) 2 (33%) 1 (17%) 1 (17%) 0 (0%) Nasopharyngitis 0 (0%) 1 (17%) 0 (0%) 0 (0%) 0 (0%) 0 (0%) At each level of summation, subjects reporting more than one adverse event are counted only once. N = number of subjects in each cohort. n(%) = number and percentage of subjects in category and cohort (n/N .times. 100)
[0180] Table 7 presents narratives for all adverse events (limited to non-serious at the moment of writing) classified by cohort, subject, AE term, and preferred term.
TABLE-US-00007 TABLE 7 Related Subject Adverse Event Term// Onset Resolution to Study Cohort ID* Preferred Term Date Date Severity Drug Outcome Med..sup.1 Disc..sup.2 37.5 mg T12 Nausea//Nausea Aug. 5, 2014 Aug. 5, 2014 Moderate Possibly Resolved without sequelae No No daily Nausea//Nausea Mild None Resolved without sequelae No NA Headache//Headache Aug. 2, 2014 Aug. 2, 2014 Mild Possibly Resolved without sequelae No No Headache//Headache Aug. 5, 2014 Aug. 5, 2014 Moderate Possibly Resolved without sequelae No No headache//Headache Aug. 6, 2014 Aug. 7, 2014 Moderate Possibly Resolved without sequelae No NA Headache//Headache Aug. 4, 2014 Aug. 4, 2014 Moderate Possibly Resolved without sequelae No No headache//Headache Aug. 7, 2014 Aug. 7, 2014 Moderate Possibly Resolved without sequelae No NA Stuffy nose//Nasal congestion Aug. 22, 2014 Aug. 29, 2014 Mild None Resolved without sequelae No NA T13 Stomach discomfort//Abdominal Aug. 1, 2014 Aug. 1, 2014 Moderate None Resolved without sequelae No No discomfort Headache//Headache Aug. 2, 2014 Aug. 5, 2014 Moderate Possibly Resolved without sequelae No No Headache//Headache Aug. 7, 2014 Moderate Possibly Resolved without sequelae No No Headache//Headache Mild Possibly Ongoing Yes NA Shortness of breath//Dyspnoea Aug. 1, 2014 Aug. 1, 2014 Severe None Resolved without sequelae No No Congestion (Nose)//Nasal Aug. 5, 2014 Moderate Possibly Resolved without sequelae No No congestion T14 Flushing//Flushing Aug. 1, 2014 Aug. 1, 2014 Mild Probably Resolved without sequelae No No Flushing//Flushing Aug. 2, 2014 Aug. 3, 2014 Mild Probably Resolved without sequelae No No Headache//Headache Aug. 1, 2014 Aug. 1, 2014 Moderate Possibly Resolved without sequelae Yes No T15 Pain/other//Injection site pain Aug. 5, 2014 Aug. 8, 2014 Moderate None Resolved without sequelae Yes No T16 nasal congestion//Nasal Aug. 4, 2014 Aug. 5, 2014 Mild None Resolved without sequelae No No congestion 37.5 mg T21 Nose bleed//Epistaxis Moderate None Resolved without sequelae Yes NA twice daily 37.5 mg T22 Shortness of breath//Dyspnoea Nov. 5, 2014 Nov. 5, 2014 Moderate None Resolved without sequelae Yes NA twice daily upper respiratory infection// Nov. 2, 2014 Mild None Resolved without sequelae No NA Upper respiratory tract infection Facial flushing//Flushing Aug. 9, 2014 Aug. 9, 2014 Mild Possibly Resolved without sequelae No No T23 Headache//Headache Aug. 8, 2014 Aug. 9, 2014 Mild Possibly Resolved without sequelae No No congestion (stuffy nose)//Nasal Aug. 8, 2014 Aug. 8, 2014 Mild Possibly Resolved without sequelae No No congestion cold/congestion// Sep. 14, 2014 Sep. 19, 2014 Mild None Resolved without sequelae No NA Nasopharyngitis Menstrual Cramps// Aug. 11, 2014 Aug. 16, 2014 Mild None Resolved without sequelae Yes No Dysmenorrhoea Facial flushing//Flushing Aug. 10, 2014 Aug. 10, 2014 Mild Possibly Resolved without sequelae No No T24 Nausea//Nausea Aug. 10, 2014 Aug. 10, 2014 Mild Possibly Resolved without sequelae No No Nausea//Nausea Aug. 11, 2014 Aug. 11, 2014 Mild Possibly Resolved without sequelae No No Soreness in chest and arms// Aug. 10, 2014 Aug. 11, 2014 Mild Possibly Resolved without sequelae No No Myalgia Headache//Headache Aug. 8, 2014 Aug. 8, 2014 Mild Possibly Resolved without sequelae No No Headache//Headache Mild Possibly Resolved without sequelae Yes NA Congestion (stuffy nose)//Nasal Aug. 10, 2014 Aug. 10, 2014 Mild Possibly Resolved without sequelae No No congestion Sponatenous penile erection// Aug. 11, 2014 Aug. 11, 2014 Mild Possibly Resolved without sequelae No No Sponatenous penile erection Sponatenous penile erection// Aug. 14, 2014 Aug. 14, 2014 Mild Possibly Resolved without sequelae No NA Sponatenous penile erection T25 Headache//Headache Aug. 8, 2014 Aug. 8, 2014 Mild Possibly Resolved without sequelae No No T26 Headache//Headache Aug. 9, 2014 Aug. 9, 2014 Mild Possibly Resolved without sequelae Yes No Sinus pain//Sinus headache Aug. 9, 2014 Nov. 18, 2014 Mild Probably Resolved without sequelae No No Headache//Headache Aug. 10, 2014 Sep. 22, 2014 Moderate Probably Resolved without sequelae Yes No Fatigue//Fatigue Aug. 9, 2014 Aug. 10, 2014 Mild Possibly Resolved without sequelae No No 87.5 mg T31 headache//Headache Aug. 15, 2014 Aug. 15, 2014 Mild Probably Resolved without sequelae No No daily headache//Headache Aug. 17, 2014 Aug. 17, 2014 Mild Probably Resolved without sequelae No No headache//Headache Aug. 18, 2014 Aug. 18, 2014 Moderate Probably Resolved without sequelae No No congestion (stuffy nose)//Sinus Aug. 15, 2014 Aug. 21, 2014 Mild Probably Resolved without sequelae No No congestion Facial flushing//Flushing Aug. 18, 2014 Aug. 18, 2014 Mild Probably Resolved without sequelae No No spotty vision//Vision blurred Aug. 15, 2014 Aug. 15, 2014 Mild None Resolved without sequelae No No T32 motion sickness//Motion Aug. 15, 2014 Aug. 15, 2014 Mild Possibly Resolved without sequelae No No sickness headache//Headache Aug. 15, 2014 Aug. 15, 2014 Mild Probably Resolved without sequelae Yes No headache//Headache Aug. 16, 2014 Aug. 16, 2014 Mild Probably Resolved without sequelae No No headache//Headache Aug. 17, 2014 Aug. 17, 2014 Mild Probably Resolved without sequelae No No dry mouth//Dry mouth Aug. 16, 2014 Aug. 16, 2014 Mild Possibly Resolved without sequelae No No T33 Head Injury//Head injury Aug. 21, 2014 Aug. 22, 2014 Mild None Resolved without sequelae Yes NA facial flushing//Flushing Aug. 16, 2014 Aug. 22, 2014 Mild Probably Resolved without sequelae No No tearing//Lacrimation increased Aug. 16, 2014 Aug. 22, 2014 Mild None Resolved without sequelae No No T34 Sleepiness//Somnolence Aug. 16, 2014 Aug. 25, 2014 Mild Possibly Resolved without sequelae No No Sponatenous penile erection// Aug. 20, 2014 Aug. 20, 2014 Mild Possibly Resolved without sequelae No No Sponatenous penile erection Facial flushing//Flushing Aug. 16, 2014 Aug. 21, 2014 Mild Possibly Resolved with sequelae No No T35 headache//Headache Aug. 15, 2014 Aug. 15, 2014 Mild Probably Resolved without sequelae No No 87.5 mg headache//Headache Aug. 16, 2014 Aug. 16, 2014 Mild Probably Resolved without sequelae No No daily stuffy nose//Nasal congestion Sep. 20, 2014 Sep. 23, 2014 Moderate None Resolved without sequelae No NA T36 Nasal congestion//Nasal Aug. 19, 2014 Aug. 21, 2014 Mild Possibly Resolved without sequelae Yes No congestion Flushing//Flushing Aug. 15, 2014 Aug. 15, 2014 Mild Probably Resolved without sequelae No No Headache//Headache Aug. 15, 2014 Aug. 15, 2014 Mild Possibly Resolved without sequelae No No 87.5 mg T42 Nausea/vomiting//Nausea Aug. 26, 2014 Aug. 26, 2014 Mild Possibly Resolved without sequelae No No twice daily Stomach discomfort//Abdominal Aug. 22, 2014 Aug. 22, 2014 Mild Possibly Resolved with sequelae No No discomfort Facial flushing//Flushing Aug. 26, 2014 Aug. 26, 2014 Mild Probably Resolved without sequelae No No Headache//Headache Aug. 23, 2014 Aug. 23, 2014 Mild Probably Resolved without sequelae No No Headache//Headache Aug. 25, 2014 Aug. 25, 2014 Mild Probably Resolved without sequelae No No Headache//Headache Aug. 24, 2014 Aug. 24, 2014 Mild Probably Resolved without sequelae No No Headache//Headache Aug. 26, 2014 Aug. 26, 2014 Mild Probably Resolved without sequelae No No T43 headache//Headache Aug. 22, 2014 Aug. 22, 2014 Moderate Possibly Resolved without sequelae No No headache//Headache Aug. 23, 2014 Aug. 23, 2014 Mild Possibly Resolved without sequelae No No headache//Headache Aug. 24, 2014 Aug. 24, 2014 Mild Possibly Resolved without sequelae No No T44 Stuffy nose//Nasal congestion Aug. 22, 2014 Aug. 22, 2014 Mild Possibly Resolved without sequelae No No Stuffy nose//Nasal congestion Aug. 25, 2014 Aug. 25, 2014 Mild Possibly Resolved without sequelae No No Stuffy nose//Nasal congestion Aug. 25, 2014 Aug. 25, 2014 Mild Possibly Resolved without sequelae No No sponatenous penile erection// Aug. 21, 2014 Aug. 21, 2014 Mild Possibly Resolved without sequelae No No Sponatenous penile erection 87.5 mg Sponatenous penile erection// Aug. 21, 2014 Aug. 21, 2014 Mild Possibly Resolved without sequelae No No twice Sponatenous penile erection daily Sponatenous penile erection// Aug. 22, 2014 Aug. 22, 2014 Mild Possibly Resolved without sequelae No No Sponatenous penile erection sponatenous penile erection// Aug. 25, 2014 Aug. 25, 2014 Mild Possibly Resolved without sequelae No No Sponatenous penile erection Sponatenous penile erection// Aug. 26, 2014 Aug. 26, 2014 Mild Possibly Resolved without sequelae No No Sponatenous penile erection Headache//Headache Aug. 21, 2014 Aug. 21, 2014 Mild Possibly Resolved without sequelae No No Headache//Headache Aug. 22, 2014 Aug. 22, 2014 Mild Possibly Resolved without sequelae No No headache//Headache Aug. 23, 2014 Aug. 23, 2014 Mild Possibly Resolved without sequelae No No headache//Headache Aug. 24, 2014 Aug. 24, 2014 Mild Possibly Resolved without sequelae No No T45 sponatenous penile erection// Aug. 31, 2014 Aug. 31, 2014 Mild Possibly Resolved without sequelae No No Sponatenous penile erection T46 sinusitis//Sinusitis Aug. 26, 2014 Moderate None Ongoing No No back pain//Back pain Aug. 31, 2014 Sep. 5, 2014 Mild Possibly Resolved without sequelae No No flushing//Flushing Aug. 30, 2014 Aug. 31, 2014 Mild Possibly Resolved without sequelae No No flushing//Flushing Sep. 1, 2014 Sep. 1, 2014 Mild Possibly Resolved without sequelae No No flushing//Flushing Sep. 2, 2014 Sep. 2, 2014 Mild Possibly Resolved without sequelae No No flushing//Flushing Sep. 2, 2014 Sep. 3, 2014 Mild Possibly Resolved without sequelae No No Headache//Headache Aug. 29, 2014 Sep. 5, 2014 Mild Possibly Resolved without sequelae Yes No Dizziness//Dizziness Aug. 30, 2014 Aug. 30, 2014 Mild Possibly Resolved with sequelae No No flushing//Flushing Aug. 31, 2014 Aug. 31, 2014 Mild Possibly Resolved without sequelae No No 87.5 mg Fatigue//Fatigue Aug. 30, 2014 Sep. 1, 2014 Mild Possibly Resolved without sequelae No No twice daily edema//Oedema Sep. 2, 2014 Mild Possibly Ongoing No No 125 mg T51 headache//Headache Feb. 9, 2015 Mild None Resolved without sequelae Yes NA daily T52 Increased frequency of Nov. 7, 2014 Nov. 8, 2014 Mild Possibly Resolved without sequelae No No sponatenous penile erections// Sponatenous penile erection T53 Diarrhea//Diarrhoea Dec. 6, 2014 Dec. 6, 2014 Mild Possibly Resolved without sequelae No No Epistaxis//Epistaxis Dec. 7, 2014 Dec. 7, 2014 Mild None Resolved without sequelae No No Headache//Headache Dec. 3, 2014 Dec. 3, 2014 Mild Possibly Resolved without sequelae No No Sponatenous penile erection// Dec. 4, 2014 Dec. 4, 2014 Mild Possibly Resolved without sequelae No No Sponatenous penile erection Flushing//Flushing Dec. 4, 2014 Dec. 8, 2014 Mild Probably Resolved without sequelae No No
T54 Headache//Headache Oct. 10, 2014 Oct. 10, 2014 Moderate Possibly Resolved without sequelae No No headache//Headache Oct. 12, 2014 Oct. 13, 2014 Mild Possibly Resolved without sequelae Yes No headaches//Headache Oct. 13, 2014 Moderate Possibly Ongoing Yes No Dizziness//Dizziness Oct. 13, 2014 Oct. 13, 2014 Moderate Possibly Resolved without sequelae Yes No Stuffy nose (congestion)//Nasal Oct. 11, 2014 Mild Possibly Ongoing No No congestion Nose bleed//Epitaxis Oct. 13, 2014 Oct. 13, 2014 Mild Possibly Resolved without sequelae No No itchy throat//Throat irritation Oct. 30, 2014 Oct. 30, 2014 Moderate None Resolved without sequelae Yes NA T55 Nausea//Nausea Jan. 13, 2015 Jan. 14, 2015 Moderate None Resolved without sequelae Yes NA Swollen/puffy cheeks//Face Nov. 29, 2014 Nov. 29, 2014 Mild None Resolved without sequelae No No oedema headaches//Headache Nov. 25, 2014 Nov. 25, 2014 Mild Possibly Resolved without sequelae No No 125 mg Headache//Headache Nov. 27, 2014 Nov. 27, 2014 Mild Possibly Resolved without sequelae No No daily Headache//Headache Nov. 28, 2014 Nov. 28, 2014 Mild Possibly Resolved without sequelae No No Headache//Headache Nov. 30, 2014 Nov. 30, 2014 Mild Possibly Resolved without sequelae No NA Migraine Headache//Migraine Jan. 12, 2015 Jan, 14, 2015 Moderate None Resolved without sequelae Yes NA T56 Stomach discomfort//Abdominal Sep. 8, 2014 Sep. 8, 2014 Mild Possibly Resolved without sequelae No No discomfort Stomach discomfort//Abdominal Sep. 6, 2014 Sep. 10, 2014 Mild Possibly Resolved with sequelae No No discomfort Stomach discomfort//Abdominal Sep. 7, 2014 Sep. 7, 2014 Mild Possibly Resolved without sequelae No No discomfort Stomach discomfort//Abdominal Sep. 9, 2014 Sep. 9, 2014 Mild Possibly Resolved without sequelae No No discomfort Chest pain//Chest pain Sep. 6, 2014 Sep. 7, 2014 Mild Possibly Resolved with sequelae No No Rash//Rash Sep. 7, 2014 Sep. 10, 2014 Mild Possibly Resolved without sequelae No No Chest pain//Chest pain Sep. 6, 2014 Sep. 6, 2014 Mild None Resolved without sequelae No No Rash//Rash Sep. 8, 2014 Sep. 8, 2014 Mild None Resolved without sequelae No No Rash//Rash Sep. 9, 2014 Sep. 9, 2014 Mild None Resolved without sequelae No No Rash//Rash Sep. 11, 2014 Sep. 11, 2014 Mild None Resolved without sequelae No No Rash//Rash Sep. 12, 2014 Sep. 12, 2014 Mild None Resolved without sequelae No No Headache//Headache Sep. 6, 2014 Sep. 6, 2014 Mild Probably Resolved with sequelae Yes No Headache//Headache Sep. 7, 2014 Sep. 7, 2014 Mild Possibly Resolved without sequelae Yes No Headache//Headache Sep. 8, 2014 Sep. 8, 2014 Mild Possibly Resolved without sequelae No No Headache//Headache Sep. 9, 2014 Sep. 9, 2014 Mild Probably Resolved without sequelae Yes No Headache//Headache Sep. 10, 2014 Sep. 10, 2014 Mild Probably Resolved without sequelae Yes No Exercise C2 Ventricular arrhythmia// Dec. 11, 2014 Dec. 11, 2014 Mild None Resolved without sequelae No NA testing Ventricular arrhythmia// only Ventricular Tachycardia// Dec. 15, 2014 Dec. 15, 2014 Mild None Resolved without sequelae No NA Ventricular tachycardia//
[0181] Table 8 presents numbers of subjects with number of AEs.gtoreq.n, where n=1, 2, . . . , 6, by treatment group.
TABLE-US-00008 TABLE 8 Adverse Events by Treatment Group N (%) of Subjects 37.5 mg 87.5 mg 87.5 mg Exercise Reporting 37.5 mg daily twice daily daily twice daily 125 mg daily testing only at Least: (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) 1 event 5 (83%) 6 (100%) 6 (100%) 5 (83%) 6 (100%) 1 (17%) 2 events 3 (50%) 4 (67%) 6 (100%) 4 (67%) 4 (67%) 1 (17%) 3 events 3 (50%) 4 (67%) 6 (100%) 4 (67%) 4 (67%) 0 (0%) 4 events 2 (33%) 3 (50%) 2 (33%) 3 (50%) 4 (67%) 0 (0%) 5 events 2 (33%) 2 (33%) 2 (33%) 3 (50%) 4 (67%) 0 (0%) 6 events 2 (33%) 1 (17%) 1 (17%) 3 (50%) 3 (50%) 0 (0%)
[0182] Tables 9-12 present AEs by preferred term (similar to Table 6), but additionally report the number of subjects with an AE and the number of AEs (Table 9), the number of AE events/subjects grouped by treatment group and by related (including possibly or probably) vs. not related to the study drug (Table 10), mild vs. moderate/severe (Table 11), and expected vs. unexpected AEs (Table 12).
TABLE-US-00009 TABLE 9 Adverse Events by Preferred Term Preferred 37.5 37.5 mg 87.5 87.5 mg 125 Exercise Term mg twice mg twice mg testing #Events daily daily daily daily daily only (#Subjects) (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) Abdominal 1 (1) 0 (0) 0 (0) 1 (1) 3 (1) 0 (0) discomfort Abdominal 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) pain upper Back pain 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Chest pain 0 (0) 0 (0) 0 (0) 0 (0) 2 (1) 0 (0) Diarrhoea 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) Dizziness 0 (0) 0 (0) 0 (0) 1 (1) 1 (1) 0 (0) Dry mouth 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) Dysmenorrhoea 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) Dyspnoea 1 (1) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) Epistaxis 0 (0) 1 (1) 0 (0) 0 (0) 2 (2) 0 (0) Face oedema 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) Fatigue 0 (0) 1 (1) 0 (0) 1 (1) 0 (0) 0 (0) Flushing 2 (1) 2 (2) 4 (4) 6 (2) 1 (1) 0 (0) Head injury 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) Headache 9 (3) 6 (4) 9 (4) 12 (4) 14 (5) 0 (0) Injection site 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) pain Lacrimation 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) increased Migraine 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) Motion sickness 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) Myalgia 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) Nasal 3 (3) 2 (2) 2 (2) 3 (1) 1 (1) 0 (0) congestion Nasopharyngitis 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) Nausea 2 (1) 2 (1) 0 (0) 1 (1) 1 (1) 0 (0) Oedema 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) Rash 0 (0) 0 (0) 0 (0) 0 (0) 5 (1) 0 (0) Sinus 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) congestion Sinus headache 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) Sinusitis 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) Somnolence 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) Spontaneous 0 (0) 2 (1) 1 (1) 6 (2) 2 (2) 0 (0) penile erection Throat irritation 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) Upper 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) respiratory tract infection Ventricular 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) arrhythmia Ventricular 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) tachycardia Vision blurred 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0)
TABLE-US-00010 TABLE 10 Related and Unrelated AEs 37.5 mg twice 87.5 mg twice Preferred 37.5 mg daily daily 87.5 mg daily daily 125 mg daily Exercise only Term, (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) #Events Drug Not Drug Not Drug Not Drug Not Drug Not Drug Not (#Subjects) related* related related* related related* related related* related related* related related* related Abdominal 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 3 (1) 0 (0) 0 (0) 0 (0) discomfort Abdominal 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) pain upper Back pain 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Chest pain 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 1 (1) 0 (0) 0 (0) Diarrhoea 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) Dizziness 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) Dry mouth 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Dys- 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) menorrhoea Dyspnoea 0 (0) 1 (1) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Epistaxis 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 1 (1) 0 (0) 0 (0) Face oedema 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) Fatigue 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Flushing 2 (1) 0 (0) 2 (2) 0 (0) 4 (4) 0 (0) 6 (2) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) Head injury 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Headache 9 (3) 0 (0) 6 (4) 0 (0) 9 (4) 0 (0) 12 (4) 0 (0) 13 (4) 1 (1) 0 (0) 0 (0) Injection site 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) pain Lacrimation 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) increased Migraine 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) Motion 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) sickness Myalgia 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Nasal 1 (1) 2 (2) 2 (2) 0 (0) 1 (1) 1 (1) 3 (1) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) congestion Naso- 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) pharyngitis Nausea 1 (1) 1 (1) 2 (1) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) Oedema 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Rash 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 4 (1) 0 (0) 0 (0) Sinus 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) congestion Sinus 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) headache Sinusitis 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) Somnolence 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Spontaneous 0 (0) 0 (0) 2 (1) 0 (0) 1 (1) 0 (0) 6 (2) 0 (0) 2 (2) 0 (0) 0 (0) 0 (0) penile erection Throat 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) irritation Upper 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) respiratory tract infection Ventricular 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) arrhythmia Ventricular 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) tachycardia Vision 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) blurred Total 13 (3) 6 (4) 17 (5) 5 (3) 19 (6) 4 (3) 33 (5) 1 (1) 26 (5) 11 (5) 0 (0) 2 (1) *Drug related = possibly related, probably related or related to study drug Out of all 36 study subjects, none had adverse events related to the study drug, and 11, 21 and 17 subjects had adverse events that were probably related, possibly related and unrelated to the study drug, respectively.
TABLE-US-00011 TABLE 11 AEs by Severity 37.5 mg twice 87.5 mg twice Preferred 37.5 mg daily daily 87.5 mg daily daily 125 mg daily Exercise only Term, (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) #Events Moderate/ Moderate/ Moderate/ Moderate/ Moderate/ Moderate/ (#Subjects) Mild severe Mild severe Mild severe Mild severe Mild severe Mild severe Abdominal 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 3(1) 0 (0) 0 (0) 0 (0) discomfort Abdominal 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) pain upper Back pain 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Chest pain 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 2 (1) 0 (0) 0 (0) 0 (0) Diarrhoea 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) Dizziness 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) Dry mouth 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Dys- 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) menorrhoea Dyspnoea 0 (0) 1 (1) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Epistaxis 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 2 (2) 0 (0) 0 (0) 0 (0) Face oedema 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) Fatigue 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Flushing 2 (1) 0 (0) 2 (2) 0 (0) 4 (4) 0 (0) 6 (2) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) Head injury 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Headache 2 (2) 7 (3) 5 (4) 1 (1) 8 (4) 1 (1) 11 (4) 1 (1) 12 (5) 2 (1) 0 (0) 0 (0) Injection site 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) pain Lacrimation 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) increased Migraine 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) Motion 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) sickness Myalgia 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Nasal 2 (2) 1 (1) 2 (2) 0 (0) 1 (1) 1 (1) 3 (1) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) congestion Naso- 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) pharyngitis Nausea 1 (1) 1 (1) 2 (1) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) Oedema 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Rash 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 5 (1) 0 (0) 0 (0) 0 (0) Sinus 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) congestion Sinus 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) headache Sinusitis 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) Somnolence 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Spontaneous 0 (0) 0 (0) 2 (1) 0 (0) 1 (I) 0 (0) 6 (2) 0 (0) 2 (2) 0 (0) 0 (0) 0 (0) penile erection Throat 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) irritation Upper 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) respiratory tract infection Ventricular 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) arrhythmia Ventricular 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) tachycardia Vision 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) blurred Total 7 (4) 12 (4) 19 (5) 3 (3) 21 (6) 2 (2) 32 (5) 2 (2) 31 (6) 6 (2) 2 (1) 0 (0) Out of all 36 study subjects, 27 had mild adverse events, 13 had moderate and 1 subject had a severe adverse event.
TABLE-US-00012 TABLE 12 AEs by Expectedness 37.5 mg twice 87.5 mg twice 37.5 mg daily daily 87.5 mg daily daily 125 mg daily Exercise only Preferred (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) Term, Not Not Not Not Not Not #Events Ex- Ex- Ex- Ex- Ex- Ex- Ex- Ex- Ex- Ex- Ex- Ex- (#Subjects) pected pected pected pected pected pected pected pected pected pected pected pected Abdominal 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 3 (1) 0 (0) 0 (0) 0 (0) discomfort Abdominal 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) pain upper Back pain 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 2 (1) 0 (0) 0 (0) Chest pain 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) Diarrhoea 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) Dizziness 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) Dry mouth 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Dys- 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) menorrhoea Dyspnoea 0 (0) 1 (1) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Epistaxis 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 2 (2) 0 (0) 0 (0) Face oedema 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) Fatigue 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) Flushing 2 (1) 0 (0) 2 (2) 0 (0) 4 (4) 0 (0) 5 (2) 1 (1) 1 (1) 0 (0) 0 (0) 0 (0) Head injury 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Headache 8 (3) 1 (1) 5 (4) 1 (1) 9 (4) 0 (0) 11 (3) 1 (1) 13 (5) 1 (1) 0 (0) 0 (0) Injection site 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) pain Lacrimation 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) increased Migraine 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) Motion 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) sickness Myalgia 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Nasal 2 (2) 1 (1) 2 (2) 0 (0) 2 (2) 0 (0) 3 (1) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) congestion Naso- 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) pharyngitis Nausea 2 (1) 0 (0) 2 (1) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 1 (1) 0 (0) 0 (0) Oedema 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) Rash 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 5 (1) 0 (0) 0 (0) Sinus 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) congestion Sinus 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) headache Sinusitis 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) Somnolence 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Spontaneous 0 (0) 0 (0) 2 (1) 0 (0) 1 (1) 0 (0) 6 (2) 0 (0) 2 (2) 0 (0) 0 (0) 0 (0) penile erection Throat 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) irritation Upper 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) respiratory tract infection Ventricular 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) arrhythmia Ventricular 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) tachycardia Vision 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 1 (1) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) blurred Total 14 (4) 5 (3) 15 (5) 7 (5) 18 (6) 5 (4) 26 (5) 8 (2) 22 (6) 15 (4) 2 (1) 0 (0) Out of all 36 study subjects, 27 subjects had expected and 18 had unexpected adverse events
[0183] Table 13 focuses on a subset of Table 7 limited to preferred terms for which AEs happened more than once (either >2 AEs for one subject, or >2 subjects with at least one AE) in at least one cohort.
TABLE-US-00013 TABLE 13 Events That Occurred More Than Once in One Subject or in More Than One Subject 37.5 mg 37.5 mg 87.5 mg 87.5 mg 125 mg Exercise Preferred Term, daily twice daily daily twice daily daily testing only #Events (#Subjects) (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) (N = 6) Abdominal discomfort 1 (1) 0 (0) 0 (0) 1 (1) 3 (1) 0 (0) Chest pain 0 (0) 0 (0) 0 (0) 0 (0) 2 (1) 0 (0) Epistaxis 0 (0) 1 (1) 0 (0) 0 (0) 2 (2) 0 (0) Flushing 2 (1) 2 (2) 4 (4) 6 (2) 1 (1) 0 (0) Headache 9 (3) 6 (4) 9 (4) 12 (4) 14 (5) 0 (0) Nasal congestion 3 (3) 2 (2) 2 (2) 3 (1) 1 (1) 0 (0) Nausea 2 (1) 2 (1) 0 (0) 1 (1) 1 (1) 0 (0) Rash 0 (0) 0 (0) 0 (0) 0 (0) 5 (1) 0 (0) Spontaneous penile 0 (0) 2 (1) 1 (1) 6 (2) 2 (2) 0 (0) erection
[0184] FIG. 1 displays the percent of subjects reporting at least one, three or five adverse events by treatment group (the numbers are taken from Table 6). The cohorts at horizontal axis are sorted from the lowest daily dose at the left (exercise only group; zero dose, though not a placebo) to the highest one-time dose (125 mg) at the right. The percentages vary from 100% to 0% (exercise only group). As expected, the exercise only group features the lowest percentage. The plot doesn't suggest a clear association between the dose and percent of subjects reporting AEs.
Example 3--Exercise Testing
[0185] The purpose of this example was to evaluate the efficacy of the treatment protocol described in Example 1 using various exercise testing parameters.
[0186] The primary outcome of this arm of the study was maximal VO2 as determined by exercise testing. Table 14 summarizes results for the key outcome from the exercise testing--peak VO2 (limited to the subjects who achieved maximum effort) by treatment group. Out of the 36 subjects enrolled in the trial, 33 reached max effort in the exercise testing at each of the time points, and 31 subjects at both time points. The first two lines present data for baseline and follow-up measurements, while the third line presents differences between the two measurements (change scores, the outcome for this aim). Analysis of variances suggests lack of differences between the change scores (p=0.85).
TABLE-US-00014 TABLE 14 Peak VO2 at Maximum Effort, ml/kg/min 87.5 37.5 37.5 mg 87.5 mg All mg twice mg twice 125 mg Exercise P- N subjects N daily N daily N daily N daily N daily N only value Baseline 34 28.5 .+-. 5.8 6 24.6 .+-. 6.9 6 30.4 .+-. 6.2 6 28.4 .+-. 6.2 5 28.0 .+-. 5.2 5 28.6 .+-. 3.0 6 30.6 .+-. 6.2 0.542 measurement Follow-up 33 28.2 .+-. 5.8 5 24.7 .+-. 6.7 6 28.8 .+-. 8.1 6 27.1 .+-. 5.0 5 28.2 .+-. 6.0 6 28.6 .+-. 3.8 5 31.8 .+-. 5.0 0.570 measurement Difference, 32 -0.6 .+-. 3.3 5 -0.8 .+-. 1.7 6 -1.6 .+-. 5.1 6 -1.4 .+-. 2.5 5 0.2 .+-. 5.0 5 0.9 .+-. 2.6 5 -0.3 .+-. 1.8 0.851 FU - BL P-values were calculated by ANOVA. The maximum effort was achieved when the respiratory quotient at peak .gtoreq. 1.1.
[0187] FIGS. 2 and 3 present the findings for change scores in a visual way (with a positive change indicating an improvement). FIG. 2 displays individual change score for each subject with paired measurements (circles) and two lines with mean and median values. The plots don't suggest that change scores increase with the dose. FIG. 3 displays maximal VO2 values before and after the treatment for each subject and in each cohort.
[0188] As expected, baseline and follow-up measurements are strongly correlated, with the correlation coefficient >0.8.
[0189] An additional outcome, VO2 at anaerobic threshold, was also measured. Similar analyses were performed for this outcome. Results are presented in Table 15 and FIGS. 4 and 5. Overall results are similar to those for maximal VO2.
TABLE-US-00015 TABLE 15 Peak VO2 at Anaerobic Threshold, ml/kg/min 37.5 37.5 mg 87.5 87.5 mg All mg twice mg twice 125 mg Exercise P- N subjects N daily N daily N daily N daily N daily N only value Baseline 36 18.6 .+-. 6 17.2 .+-. 6 18.0 .+-. 6 17.6 .+-. 6 18.3 .+-. 6 18.8 .+-. 6 21.7 .+-. 0.570 measurement 4.5 5.0 3.0 5.3 4.6 1.8 6.2 Follow-up 34 18.2 .+-. 5 16.3 .+-. 6 18.1 .+-. 6 16.5 .+-. 6 16.5 .+-. 6 20.0 .+-. 5 22.4 .+-. 0.135 measurement 4.4 2.0 3.0 4.8 5.2 3.2 5.5 Difference 34 -0.3 .+-. 5 -0.5 .+-. 6 0.1 .+-. 6 -1.1 .+-. 6 -1.7 .+-. 6 1.2 .+-. 5 0.1 .+-. 0.469 FU - BL 2.6 4.1 1.0 1.9 2.1 1.9 3.8 P-values were calculated by ANOVA.
[0190] Of note, both exercise outcomes (peak VO2 and VO2 at anaerobic threshold) are highly correlated (with the correlation coefficient at each visit above 0.7), which may explain similarities in the trend lines in FIGS. 2 and 4.
Example 4--Vascular Function Testing
[0191] The primary outcome of vascular function was determined according to an endothelial pulse amplitude tonometry (PAT) index as determined by the EndoPAT.RTM. device (Itamar Medical, Caesarea, Israel).
[0192] Table 16 summarizes the results for the key outcome from the vascular function testing--natural log of Reactive Hyperemia Index (InRHI) by treatment group. Out of the 30 subjects enrolled in the treatment arms of the trial, 27 subjects had paired measurements with an acceptable quality (with QC score equal to 3 (the best) or 2). The structure of the table is similar to the one for exercise variables.
TABLE-US-00016 TABLE 16 Natural Log of Reactive Hyperemia Index 37.5 37.5 mg 87.5 87.5 mg All mg twice mg twice 125 mg N subjects N daily N daily N daily N daily N daily P-value Baseline 28 0.52 .+-. 6 0.48 .+-. 6 0.60 .+-. 6 0.41 .+-. 4 0.49 .+-. 6 0.63 .+-. 0.704 measurement 0.28 0.31 0.30 0.25 0.12 0.37 Follow-up 28 0.49 .+-. 6 0.51 .+-. 6 0.53 .+-. 5 0.45 .+-. 5 0.40 .+-. 6 0.52 .+-. 0.945 measurement 0.28 0.26 0.29 0.31 0.29 0.34 Difference, 27 -0.02 .+-. 6 0.03 .+-. 6 -0.07 .+-. 5 0.07 .+-. 4 -0.03 .+-. 6 -0.10 .+-. 0.902 FU - BL 0.30 0.47 0.17 0.22 0.20 0.38
[0193] FIGS. 6 and 7 present the findings for change scores in a visual way (with a positive change indicating an improvement). FIG. 6 displays the individual change score for each subject with paired measurements (circles) and two lines with mean and median values. The plots do not suggest that change scores increase with the dose. FIG. 7 displays InRHI values before and after the treatment for each subject and in each cohort.
[0194] Baseline and follow-up measurements are moderately correlated, with an overall correlation coefficient of 0.4.
[0195] Of note, both mean baseline and follow-up measurements are close to the cut-off value of 0.51 suggested by the EndoPAT documentation as a threshold between the normal (defined as InRHI>0.51) and abnormal (InRHI <0.51) values. Analysis of the data indicates that some patients showed as much as a 9.75% improvement in this measure.
[0196] Table 17 reports change scores only for secondary EndoPAT outcomes (RHI, Framingham RHI etc; top panel) and other EndoPAT indices. In all cases a positive change suggests a possible improvement.
TABLE-US-00017 TABLE 17 Secondary and Other EndoPAT Outcomes, FU - BL 37.5 mg 87.5 mg All 37.5 mg twice 87.5 mg twice 125 mg P- N subjects N daily N daily N daily N daily N daily value Secondary EndoPAT outcomes Reactive 27 -0.04 .+-. 6 0.03 .+-. 6 -0.12 .+-. 5 0.12 .+-. 4 0.01 .+-. 6 -0.21 .+-. 0.895 Hyperemia 0.56 0.84 0.30 0.34 0.38 0.78 Index Framingham 27 -0.06 .+-. 6 -0.00 .+-. 6 -0.17 .+-. 5 0.04 .+-. 4 0.00 .+-. 6 -0.13 .+-. 0.901 RHI 0.39 0.58 0.19 0.36 0.20 0.51 AUC2max_oc: 27 0.51 .+-. 6 -0.93 .+-. 6 -1.19 .+-. 5 3.03 .+-. 4 0.16 .+-. 6 1.80 .+-. 0.058 Area under the 2.91 4.37 1.84 2.49 1.08 1.18 curve to Max- Occlusion/ Control Avg2Max_oc: 27 -0.16 .+-. 6 -0.35 .+-. 6 -0.33 .+-. 5 0.17 .+-. 4 0.24 .+-. 6 -0.32 .+-. 0.626 average up to 0.79 1.01 0.26 0.43 0.73 1.28 max- Occlusion, Control Other EndoPAT indices AUC2max_o: 27 -0.26 .+-. 6 -0.23 .+-. 6 0.09 .+-. 5 -1.26 .+-. 4 -0.51 .+-. 6 0.37 .+-. 0.910 Area under the 2.75 2.74 1.45 4.89 1.64 2.71 curve to Max- Occlusion (ratio to baseline) AUCall_o: 27 0.18 .+-. 6 -0.01 .+-. 6 -0.69 .+-. 5 1.66 .+-. 4 0.60 .+-. 6 -0.28 .+-. 0.864 Area under the 3.54 2.73 2.17 5.96 2.95 3.98 curve all- Occlusion (ratio to baseline) AUCall_oc: 27 -0.60 .+-. 6 -1.34 .+-. 6 -1.19 .+-. 5 1.88 .+-. 4 0.17 .+-. 6 -1.84 .+-. 0.772 Area under the 4.93 6.42 2.00 3.25 4.30 7.21 curve all- Occlusion/ Control Avg2Max-o: 27 0.04 .+-. 6 -0.12 .+-. 6 0.15 .+-. 5 0.10 .+-. 4 0.03 .+-. 6 0.07 .+-. 0.930 average upto 0.51 0.28 0.19 0.69 0.36 0.86 max- Occlusion** Avgall_o: 27 0.02 .+-. 6 0.02 .+-. 6 -0.08 .+-. 5 0.14 .+-. 4 0.09 .+-. 6 -0.03 .+-. 0.927 average all- 0.40 0.27 0.24 0.67 0.33 0.49 Occlusion** Avgall_oc: 27 -0.06 .+-. 6 -0.10 .+-. 6 -0.13 .+-. 5 0.16 .+-. 4 0.05 .+-. 6 -0.20 .+-. 0.848 average all- 0.54 0.66 0.22 0.36 0.45 0.84 Occlusion/ Control P-values were calculated by ANOVA. **ratio to baseline
Example 5--Echocardiographic Assessment of Ventricular Performance
[0197] The primary outcome of ventricular performance with assessed using echocardiographic methods and measured according to a myocardial performance Index (MPI). The MPI is a ventricular geometry-independent measure of combined systolic and diastolic ventricular performance (Charles S. Kleinman et al, 2008--Health and Fitness). It is obtained by indexing the sum of isovolumetric contraction and relaxation time to ejection time.
[0198] Table 18 summarizes results for the key outcome from the Echocardiographic Assessment of Ventricular Performance--Blood Pool MPI. Out of the 30 subjects enrolled in the treatment arms of the trial, 27 subjects had paired measurements. The structure of the table is similar to the one for exercise variables. Analysis of the data indicates that some patients showed as much as a 21.5% improvement in this measure.
TABLE-US-00018 TABLE 18 Blood Pool MPI All 37.5 mg 37.5 mg 87.5 mg 87.5 mg 125 mg P- N subjects N daily N twice daily N daily N twice daily N daily value Baseline 29 0.581 .+-. 6 0.537 .+-. 6 0.496 .+-. 6 0.588 .+-. 5 0.548 .+-. 6 0.728 .+-. 0.305 measurement 0.197 0.304 0.150 0.158 0.136 0.155 Follow-up 28 0.517 .+-. 5 0.504 .+-. 6 0.494 .+-. 6 0.512 .+-. 6 0.410 .+-. 5 0.696 .+-. 0.058 measurement 0.165 0.187 0.087 0.163 0.078 0.202 Difference, 27 -0.059 .+-. 5 -0.052 .+-. 6 -0.003 .+-. 6 -0.076 .+-. 5 -0.118 .+-. 5 -0.054 .+-. 0.744 FU - BL 0.134 0.166 0.102 0.144 0.090 0.180
[0199] FIGS. 8 and 9 present the findings for change scores in a visual way (with a negative change indicating an improvement). FIG. 8 displays individual change score for each subject with paired measurements (circles) and two lines with mean and median values. The plots don't suggest that change scores increase with the dose. FIG. 9 displays blood pool MPI index values before and after the treatment for each subject and in each cohort.
[0200] Baseline and follow-up measurements are strongly correlated, with the overall correlation coefficient of 0.7 (last 2 lines). Of note, both mean baseline and follow-up measurements are in the elevated area (>0.4).
[0201] Tables 19-21 and FIGS. 9-15 report similar results for three other versions of MPI: Tissue Doppler MPI, and Average Isovolumetric Contraction and Relaxation.
TABLE-US-00019 TABLE 19 Tissue Doppler MPI All 37.5 mg 37.5 mg 87.5 mg 87.5 mg 125 mg P- N subjects N daily N twice daily N daily N twice daily N daily value Baseline 28 0.760 .+-. 6 0.701 .+-. 6 0.818 .+-. 6 0.804 .+-. 4 0.540 .+-. 6 0.861 .+-. 0.517 measurement 0.299 0.417 0.361 0.118 0.019 0.323 Follow-up 28 0.707 .+-. 5 0.637 .+-. 6 0.729 .+-. 6 0.716 .+-. 6 0.638 .+-. 5 0.822 .+-. 0.579 measureulent 0.201 0.206 0.230 0.142 0.168 0.271 Difference, 26 -0.056 .+-. 5 -0.052 .+-. 6 -0.089 .+-. 6 -0.089 .+-. 4 0.060 .+-. 5 -0.074 .+-. 0.813 FL - BL 0.198 0.398 0.142 0.131 0.068 0.141
TABLE-US-00020 TABLE 20 Average Isovolumic Contraction All 37.5 mg 37.5 mg 87.5 mg 87.5 mg 125 mg P- N subjects N daily N twice daily N daily N twice daily N daily value Baseline 28 115.6 .+-. 6 99.2 .+-. 6 109.4 .+-. 6 122.4 .+-. 4 84.1 .+-. 6 152.4 .+-. 0.236 measurement 50.5 50.7 51.1 36.7 20.3 64.4 Follow-up 28 107.1 .+-. 5 86.4 .+-. 6 103.6 .+-. 6 115.0 .+-. 6 83.8 .+-. 5 150.5 .+-. 0.047 measurement 41.3 22.7 32.4 32.9 26.4 60.5 Difference, 26 -4.6 .+-. 5 -3.5 .+-. 6 -5.8 .+-. 6 -7.4 .+-. 4 4.1 .+-. 5 -8.0 .+-. 0.977 FU - BL 28.3 50.0 25.7 26.5 12.1 24.6
TABLE-US-00021 TABLE 21 Average Isovolumetrie Relaxation 87.5 mg 125 All 37.5 mg 37.5 mg 87.5 mg twice mg P- N subjects N daily N twice daily N daily N daily N daily value Baseline 28 91.2 .+-. 6 83.8 .+-. 6 100.8 .+-. 6 93.4 .+-. 4 72.3 .+-. 6 99.5 .+-. 0.236 measurement 22.2 16.1 32.3 11.0 10.5 25.0 Follow-up 28 92.0 .+-. 5 94.0 .+-. 6 101.6 .+-. 6 86.4 .+-. 6 82.4 .+-. 5 96.8 .+-. 0.674 measurement 23.8 26.7 40.0 15.3 11.4 17.4 Difference, 26 0.1 .+-. 5 9.0 .+-. 6 0.8 .+-. 6 -6.9 .+-. 4 5.2 .+-. 5 -5.4 .+-. 0.354 FU - BL 14.4 11.5 21.2 10.1 12.6 11.1
[0202] For these three additional versions of MPI, a negative change also suggests a possible improvement and the overall conclusions are similar to those for Blood Pool MPI.
[0203] Additionally, because positive outcomes were seen during the short duration of the studies described in Examples 1-5, administering udenafil or a pharmaceutically acceptable salt thereof to a Fontan patient for a longer period of time could produce even more beneficial pharmacodynamic outcomes.
Example 6--Pharmacokinetic Testing
[0204] NONMEM version 7.2, R, PDxPOP.RTM. 5, Xpose, and Phoenix WinNonlin was used for the pharmacokinetic analysis.
[0205] Pharmacokinetic analysis was performed on Fontan patients receiving udenafil. FIG. 16 show the results of data evaluation for individual subjects by dosing cohort, and FIG. 17 shows the concentration profiles of udenafil in the study subjects. Plasma concentrations were determined at various time points and non-compartmental analysis was performed in patients and stratified by dosing regimens.
[0206] FIGS. 18-20 demonstrate various comparisons among the dosing cohorts. Based on the non-compartment analysis, C.sub.max was significantly increased in 87.5 mg q12 h cohort and 125 mg q24 h cohort compared to the 37.5 mg q12 h or q24 h cohorts (FIG. 18).
[0207] The 87.5 mg q12 h cohort exhibited increased C.sub.max compared to its q24 h counterpart (FIG. 18). AUC.sub..tau. was significantly increased in 87.5 mg q12 h cohort and 125 mg q24 h cohort compared to the 37.5 mg q12 h or q24 h cohorts (FIG. 19). AUC.sub.0-24 was significantly increased in 125 mg q24 h cohort compared to the 37.5 mg q24 h cohorts. The 87.5 mg q12 h cohort showed increased highest AUC.sub.0-24 among all the regimens tested (FIG. 19). No significant difference was observed in CL/F or V/F among dosing regimens, expect the significant differences between 37.5 mg q24 h and 87.5 mg q12 h (FIG. 20). There was no statistically significant difference in k.sub.e, T.sub.1/2, or T.sub.max among all 5 tested dosing regimens.
[0208] Population PK Model Development
[0209] The population PK analysis was performed using a non-linear mixed effects modeling approach. This approach estimates the typical value of parameters and their variances. It was assumed subjects were at steady state (SS): at a time (t) after dose (D) given at time tD after repeated administration of dose D given at interval .tau. (t.gtoreq.t.sub.D) as PK samples/udenafil concentrations were taken on study day 6.
[0210] As only the drug administration at Day 6 was supplied, it is expected that the subjects have taken the drug at regular intervals at home; due to this a steady state flag will be tested to account for the doses which are not available. As stated, it is assumed steady state has been reached by Day 6, as previous studies of udenafil have stated that during multiple dosing, steady state is reached in 5 days, with apparently little additional accumulation occurring after dosing for 7 days. If there were missed doses during the study period prior to the PK sampling, this can affect the ability to determine whether steady state could be assumed or not for the PK profile. If two or more additional drug administration dates and times were available prior to the visit where the PK samples were taken, then a much better dosing profile could be used for analysis.
[0211] Structural Model
[0212] One- and two-compartment models were explored (based on literature and available data). The equation for the Input model for the drug described oral absorption. For the one-compartment model, the following equation may apply to the model:
dA dt = Input - ( k 10 * A ) ##EQU00001##
[0213] And considering that CL=k10*V, the following equation may also apply:
dC dt = Input - ( CL * C ) V ##EQU00002##
[0214] The two-compartment model can be described by the following differential equation:
dX 1 dt = ka Xg + k 21 X 2 - ( k 12 + kel ) X 1 ##EQU00003##
[0215] Drug Amount in the body after oral administration may be described by the following differential equation:
Cp=Ae.sup.-.alpha.t+Be.sup.-.beta.t+Ce.sup.-k.alpha.t
[0216] The robustness of the final model was assessed in PDxPOP.RTM. 5 by bootstrap re-sampling (n=1000). Values obtained with the bootstrap (based on all runs with successful minimization) were compared to the parameter estimates from the final model. To evaluate the accuracy of the model predictions, normalized prediction distribution errors (NPDE) was performed.
[0217] Certain a priori information was used in guiding the development of the models.
[0218] One- and two-compartment models with oral absorption input were evaluated using initial estimates obtained from the literature as described above, and were explored to determine the potential structure of the model. The models were evaluated during the model building process by using objective function value, level of statistical significance, goodness of fit plots, and standard error.
[0219] The only covariate available for analysis was current body weight. Weight was tested as a fixed effect on typical values for clearance and volume of distribution (e.g., weight has a "fixed effect" on clearance). Median weight in the dataset was 65.3 kg.
[0220] The "typical value" for clearance is predicted per 70 kg patient using weight (WT) in the data set. The estimated THETA(1) and THETA(2) for subjects of known WT can be directly compared with CL and V values in subjects of "standard" weight, e.g. WTs=70 kg.
[0221] Concern is sometimes expressed that scaling parameter values estimated in children in terms of an adult size standard of 70 kg may bias the estimates, or affect the precision of estimation. There is no basis for this concern. This can be seen by inspection of the allometric scaled covariate model which may be re-arranged and is simply a constant that is determined by whatever weight is chosen for standardization. The precision of a parameter estimate will not be changed by multiplying the parameter value by an ad hoc constant. The criteria for covariate equation selection for weight in the model was statistical significance.
[0222] FIGS. 21-29 show the results of the pharmacokinetic data analysis.
[0223] During the model building process, a number of residual error models were evaluated. Proportional and exponential error models were unable to run, these terminated every time. Additive error models were able to run, but the GOF plots showed a poor fit for one-compartment models with a better fit in the two compartment model. The choice was made to use a combined error model for the base model, despite the high CV % in the residual variability, as this model gave good estimates for other parameters, 95% CIs and showed a good fit on visual inspection of GOF plots (FIGS. 30-31). It may be possible to control for the high CV % if all of the doses from days 1-5 were included from each subject in the dataset before the day 6 dose, around which the sampling occurred. It is not be necessary to do this as the model fit is good as presently described, but this may further reduce the % CVs.
[0224] After comparing observed data and predicted data, a final model was produced. GOF plots for the final model are found in FIGS. 32 and 33.
[0225] Bootstrap re-sampling was undertaken to compare the parameter estimates from the final model with those determined following 1000 bootstrap runs. In addition: visual predictive checks (plot comparing 95% prediction interval with observed data) and normalized prediction distribution errors (NPDE) techniques were applied for final model evaluation. Additionally a visual predictive check was performed.
[0226] Udenafil pharmacokinctics were well described by a two-compartment model with combined additive and proportional error. Apparent clearance (CL/F) were scaled using current body weight standardized to adult weight, 70 kg. Absorption rate constant was estimated as 0.28 h-1 (95% CI 0.16-0.39), apparent clearance (CL/F/70 kg) 36 L/h (95% CI 28.5-43.1), central volume of distribution (V2/F) 74 L (95% CI 36.2-112), inter-compartmental clearance (Q/F) 21.1 L (95% CI 10.4-31.8) and peripheral volume of distribution (V3/F) 181 L (95% CI 141-221). The final model was evaluated by bootstrap re-sampling, normalized prediction distribution errors, and visual predictive check techniques. These techniques demonstrated a good fit of the final covariate model to the data.
[0227] A two-compartment model with absorption rate constant successfully described the pharmacokinetics of udenafil in adolescents with single ventricle physiology after Fontan palliation. There was a statistically significantly influence on apparent clearance (CL/F) when subject body weight was standardized to adult weight, 70 kg included in the final model, CL/F L/hr/70 kg.
Example 7--Phase III Study of Udenafil in Fontan Patients
[0228] A Phase III study of udenafil in Fontan patients will determine the safety of udenafil (87.5 mg, twice daily) in an adolescent population with single ventrile congenital heart disease palliated with the Fontan procedure. The study will also evaluate the pharmacodynamics profile of udenafil over a period of time ranging from at least six months and up to one year. Pharmacodynamic outcomes will include exercise capacity, echocardiographic measures of ventricular function, endothelial function, and serum biomarkers, as well as measures of functional health status/quality of life. It is expected that udenafil (87.5 mg, twice daily) will be safe, and effective for improving exercise capacity and other endpoints of cardiovascular health, as well as improving quality of life.
[0229] Methodology--Randomized, double-blind, placebo-controlled clinical trial of a six month to one-year treatment with an 87.5 mg/twice a day dose in 300 subjects between 12 and 19 years of age who have had the Fontan surgery before 5 years of age.
[0230] Inclusion Criteria for the study include: [0231] Males or females age 12-19. [0232] Fontan surgery before 5 years of age.
[0233] Exclusion Criteria for the study include: [0234] Height <132 cm. [0235] Hospitalization for acute decompensated heart failure within the last 12 months. [0236] Current intravenous inotropic drugs. [0237] Undergoing evaluation for heart transplantation or listed for transplantation. [0238] Diagnosis of protein losing enteropathy, plastic bronchitis, liver cirrhosis. [0239] Known Fontan baffle obstruction, branch pulmonary artery stenosis, or pulmonary vein stenosis resulting in a mean gradient of >4 mm Hg between the regions proximal and distal to the obstruction as measured by either catheterization or echocardiography. [0240] Single lung physiology. [0241] Severe ventricular dysfunction assessed qualitatively by clinical echocardiography within 6 months prior to enrollment. [0242] Severe valvar regurgitation, ventricular outflow obstruction, or aortic arch obstruction assessed by clinical echocardiography within 6 months prior to enrollment. [0243] Significant renal, hepatic, gastrointestinal or biliary disorders that could impair absorption, metabolism or excretion of orally administered medications. [0244] Inability to complete exercise testing at baseline screening. [0245] History of PDE-5 inhibitor use within 3 months before study onset. [0246] Use of any other drug to treat pulmonary hypertension within 3 months before study onset. [0247] Known intolerance to oral udenafil. [0248] Frequent use of medications or other substances that inhibit or induce CYP3A4. [0249] Current use of alpha-blockers or nitrates. [0250] Ongoing or planned participation in another research protocol that would either prevent successful completion of planned study testing or invalidate its results. [0251] Noncardiac medical, psychiatric, and/or social disorder that would prevent successful completion of planned study testing or would invalidate its results. [0252] Cardiac care, ongoing or planned, at a non-study center that would impede study completion. [0253] For females: Pregnancy at the time of screening, pregnancy planned before study completion, or refusal to use an acceptable method of contraception for study duration. [0254] Unable to abstain or limit intake of grapefruit juice during the duration of the trial. [0255] Refusal to provide written informed consent/assent. [0256] In the opinion of the primary care physician, the subject is likely to be non-compliant with the study protocol.
[0257] The study will include baseline measures of the proposed pharmacodynamics (PD) endpoints as well as quality of life surveys. For example, EndoPAT vascular assessment will be completed as the first PD test following consent. This must be performed in a fasting (from midnight until after the test), non-caffeinated state. After the vascular assessment, subjects will have a targeted echocardiogram to assess ventricular function. A short break will be given, either after the vascular assessment or after the echocardiogram, and a light snack will be provided. Safety labs will be performed following the vascular assessment, echocardiogram, and break. These will include collection of blood to evaluate serum creatinine and liver enzyme (aspartate transaminase and alanine transaminase) levels for all participants, and a urine pregnancy test for female participants. If the pregnancy test is positive all further testing will be stopped, the patient will not be enrolled into the trial and the result will be conveyed to the subject and/or guardians by the site-principal investigator in accordance with local IRB procedures. After the safety labs, an exercise test will be administered using a braked cycle ergometer following a ramp protocol previously published in the PHN Fontan Cross-Sectional Study. After exercise testing, subjects will have completed the baseline testing. Additionally, The Peds QL, cardiac specific Peds QL, and PCQLI will be administered during the baseline testing visit.
[0258] A study coordinator will call each subject weekly for four weeks and then monthly thereafter to collect adverse events and answer questions related to the study.
[0259] At the end of the study, subjects will arrive in a fasting, non-caffeinated state, and first undergo vascular function assessment including repeating the baseline tests as well as the quality of life surveys. Follow up with subjects may occur at 30 and 90 days following end-of-study testing to record any additional adverse events possibly or probably related to the study drug that may have occurred in the 90 days following completion of the study protocol.
[0260] It is expected that udenafil (87.5 mg bid) in adolescents with Fontan physiology over a 6-12 month period will be safe and well tolerated, with few, if any, serious adverse events related to udenafil. The severity of adverse events is determined according to the Common Terminology Criteria for Adverse Events (CTCAE) Version 4.0 MedDRA 12.1 (http://ctep.cancer.gov). Likewise, the effect of udenafil on pharmacodynamic outcomes including exercise capacity, echocardiographic measures of ventricular function, endothelial function, and biomarkers associated with heart failure is expected to improve over the course of treatment. The outcomes to be measured to determine the efficacy of udenafil in this patient population will include: [0261] Exercise: Change in maximal oxygen consumption from baseline to end-of-study testing measured using a standardized exercise test; [0262] Echo: Change in myocardial performance index as measured by pulse wave Doppler echocardiography from baseline to end-of-study testing; [0263] Endothelial Function: Change in log-transformed Reactive Hyperemia Index derived from the EndoPAT.RTM. device; and [0264] Biomarkers: Change in serum BNP level from baseline to end-of-study.
[0265] As well as: [0266] Exercise: Submaximal measures of exercise capacity will be collected and evaluated. [0267] Echo: Measure of systolic and diastolic function will be collected from a targeted echocardiogram.
[0268] The study may also look at outcomes related to ventricular cavity size, eccentricity, and mass; systolic function as estimated using mean dP/dt during isovolumetric contraction (dP/dtic) and peak systolic annular velocity (S') on tissue Doppler; tissue Doppler based estimates of diastolic function and MPI; and qualitative and quantitative estimate of AV valve insufficiency.
[0269] It is also expected that functional health status will improve following administration of udenafil. The change in functional health status from baseline to the end of the study may be measured by the full scale Peds QL, Peds QL physical functioning score, Peds QL psychosocial functioning score, Peds QL cardiac-specific module quality of life score, and/or the pediatric cardiac quality of life inventory (PCQLI) score.
[0270] Furthermore, genetic material may be collected during the study to identify genetic determinants of response to udenafil after the Fontan procedure in persons with single-ventricle lesions. This will provide an indication of whether specific sub-populations of patients will have a more positive response to udenafil than others. For instance, the response to udenafil may be influenced by variants related to the vascular response to udenafil. Variants in the endothelial nitric oxide synthase gene have been reported to influence the response to sildenafil in patients with erectile dysfunction, although this has not been studied for udenafil. Variation in genes that regulate the vascular, inotropic and chronotropic response to exercise may influence the exercise capacity of patients after the Fontan procedure as well as the response to udenafil. DNA will be stored to perform future genotyping studies to analyze the genetic contribution to the response to udenafil.
[0271] Additional covariate measures will include, but may not be limited to, age, gender, race/ethnicity, height/weight, ventricular morphology, resting oxygen saturation, baseline pharmacodynamics test results, and current medication use. Observance of these variables will allow for the identification of associations between a variety of clinical factors and both safety and PD outcomes.
[0272] Data collection will include recording demographic information including age, gender, race, ethnicity, cardiac anatomy, date of Fontan procedure, presence of a fenestration, degree of atrioventricular valve regurgitation, grade of ventricular function, concomitant medications, and significant co-morbidities. Safety data will reviewed with each subject at each study visit and during telephone encounters. These events will be recorded and graded by severity and relationship to the study drug based upon established criteria. Two additional telephone encounters will take place 30 days and 90 days following end-of-study testing to assess for any adverse events possibly or probably related to the study drug in the period following the completion of study procedures.
[0273] Other data collection will include: [0274] Exercise stress test--Data from the braked cycle ergometry exercise stress tests will be collected according to protocol established in the PHN Fontan Cross-Sectional Study3. [0275] Assessment of ventricular performance--Each study echocardiogram will be stored in a de-identified manner and sent to a core laboratory, which will perform the data analysis and submit the measurements to the PHN Data Coordinating Center (DCC). [0276] Vascular function testing--De-identified data from EndoPAT.RTM. testing will be collected according to a standardized protocol. These data will be sent to a vascular core lab, which will perform the analysis and submit the measurements to the PHN DCC. [0277] Biomarkers--Serum for measurement of BNP level will be sent to a core clinical lab. Results will be sent directly to the PHN DCC. [0278] Quality of life survey--Results of the Quality of life surveys will be submitted to the PHN DCC. [0279] Samples for the biorepository--Samples collected for the biorepository will be shipped directly to the biorepository for future analysis.
[0280] Subjects will be treated with other medications at the discretion of their physicians. At the study visits, current medications will be recorded on the study forms. If a subject begins open-label use of any other PDE-5 inhibitor at any time during the study, withdrawal from the study drug is required.
[0281] When an individual subject completes the study, the subject's primary cardiologist will be notified, and the study drug will be stopped; there is no need to wean subjects off of the study drugs. The decision of whether to continue the use of an off label PDE-5 inhibitor for individual subjects will be decided by the subjects and their primary cardiologist.
[0282] While certain of the preferred embodiments of the present invention have been described and specifically exemplified above, it is not intended that the invention be limited to such embodiments. Various modifications may be made thereto without departing from the scope and spirit of the present invention.
* * * * *
References



D00001

D00002

D00003

D00004

D00005

D00006

D00007

D00008

D00009

D00010
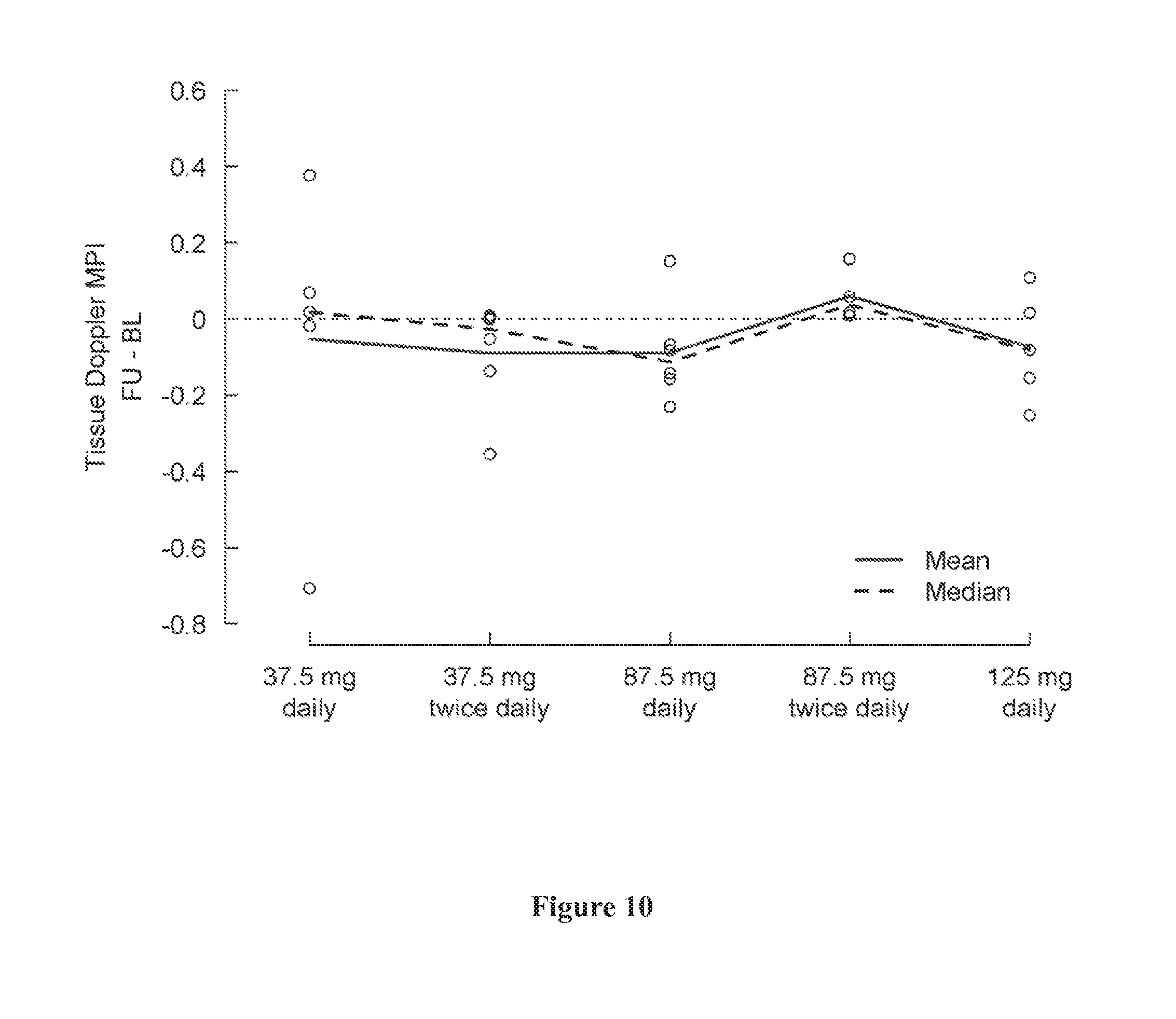
D00011
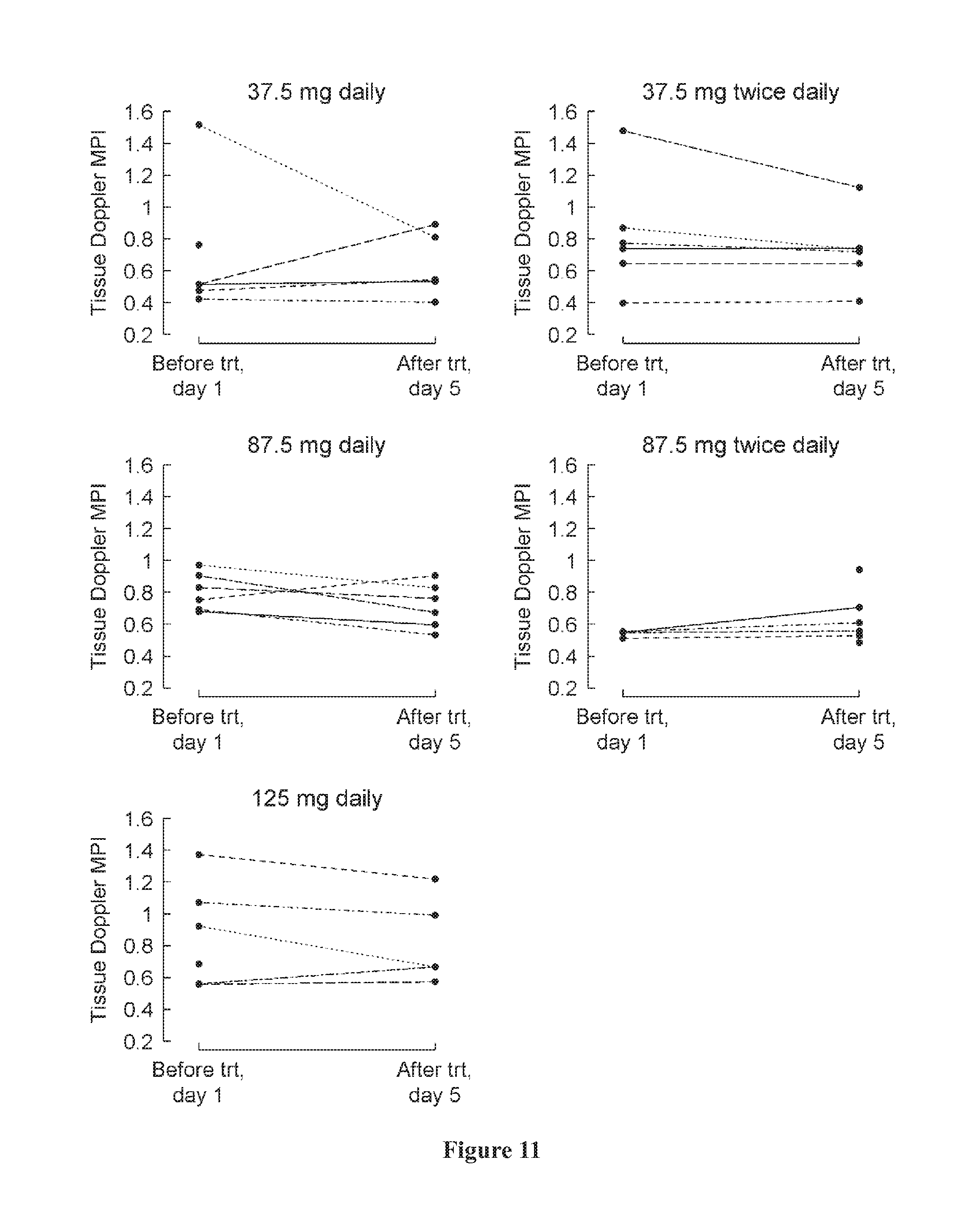
D00012
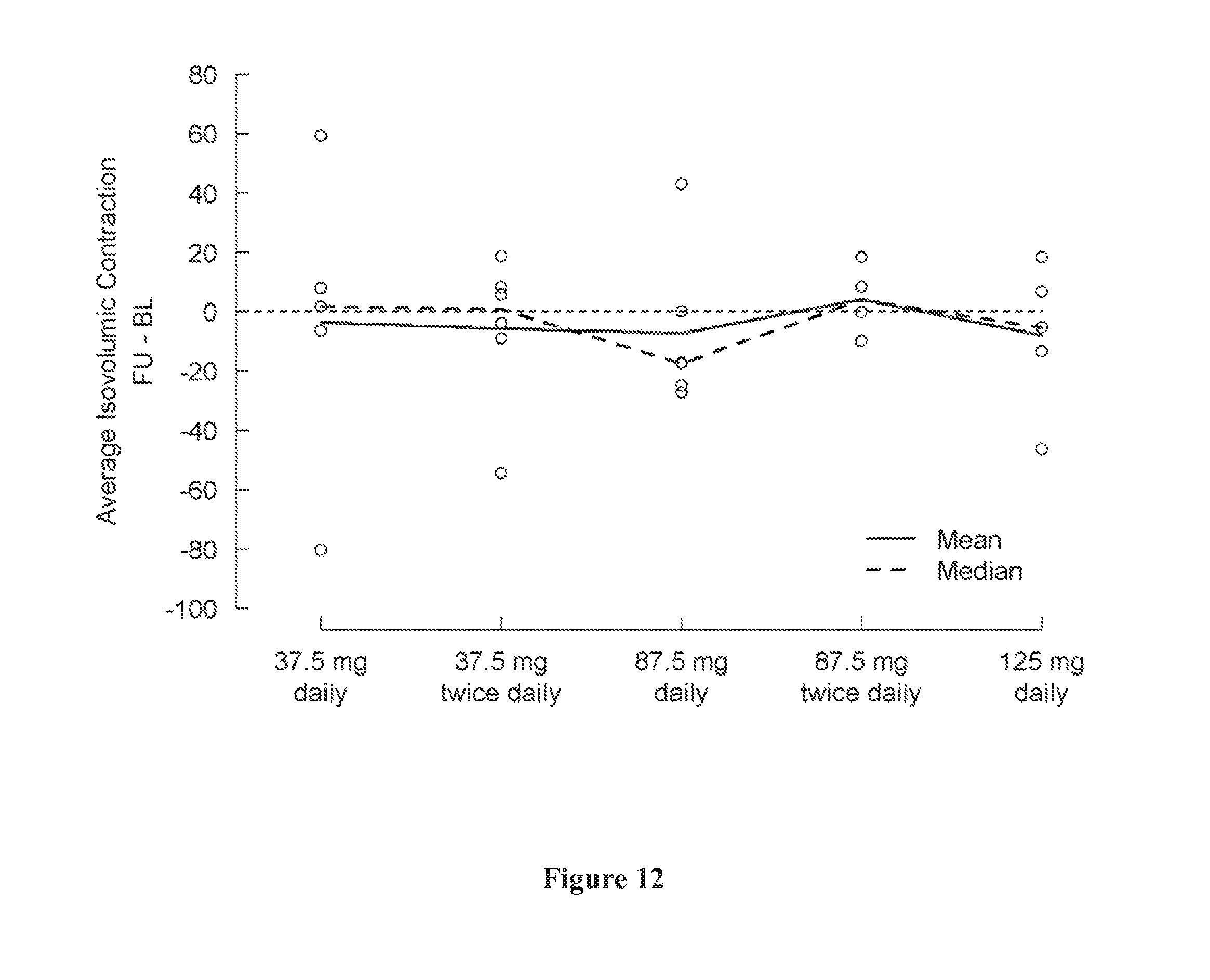
D00013
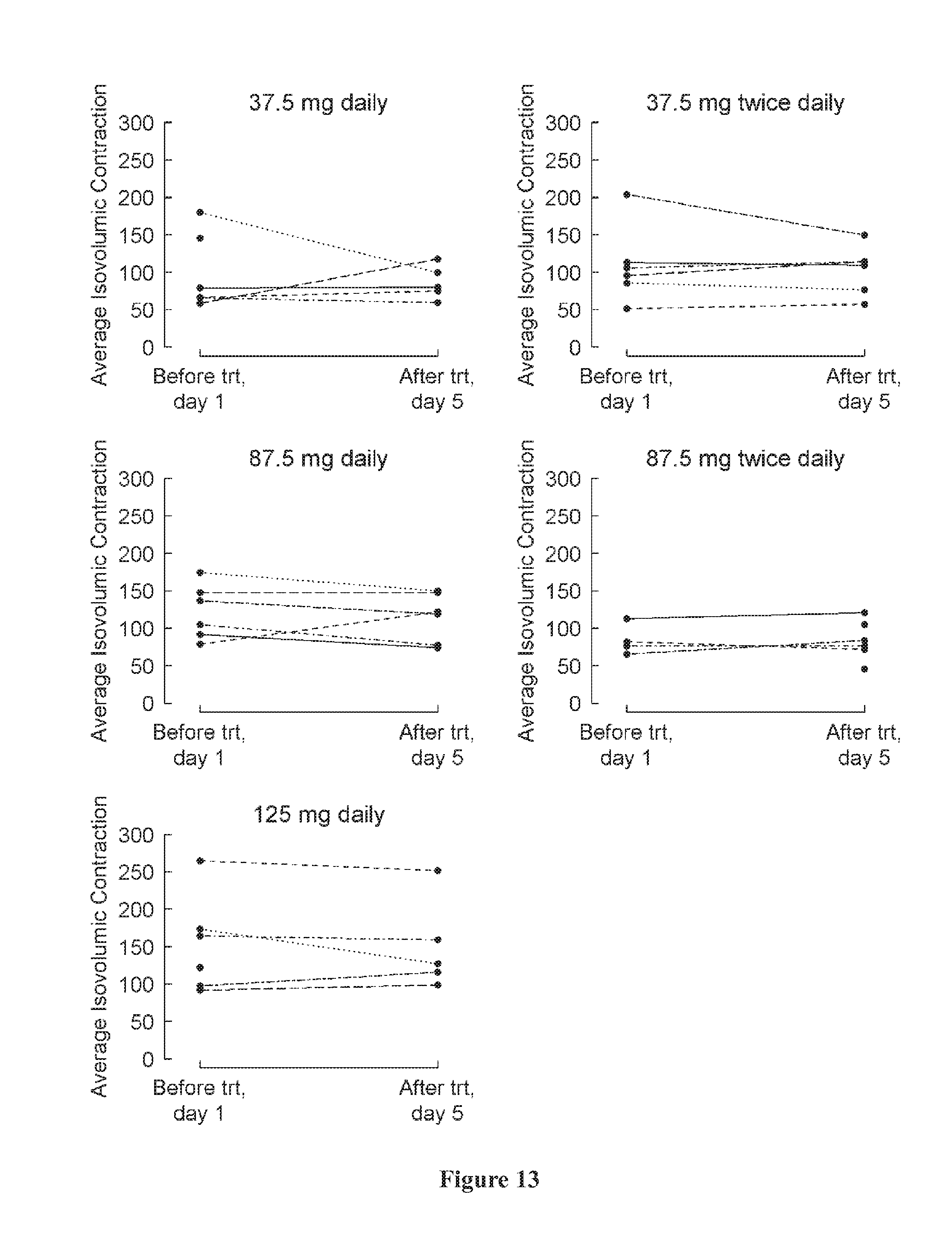
D00014
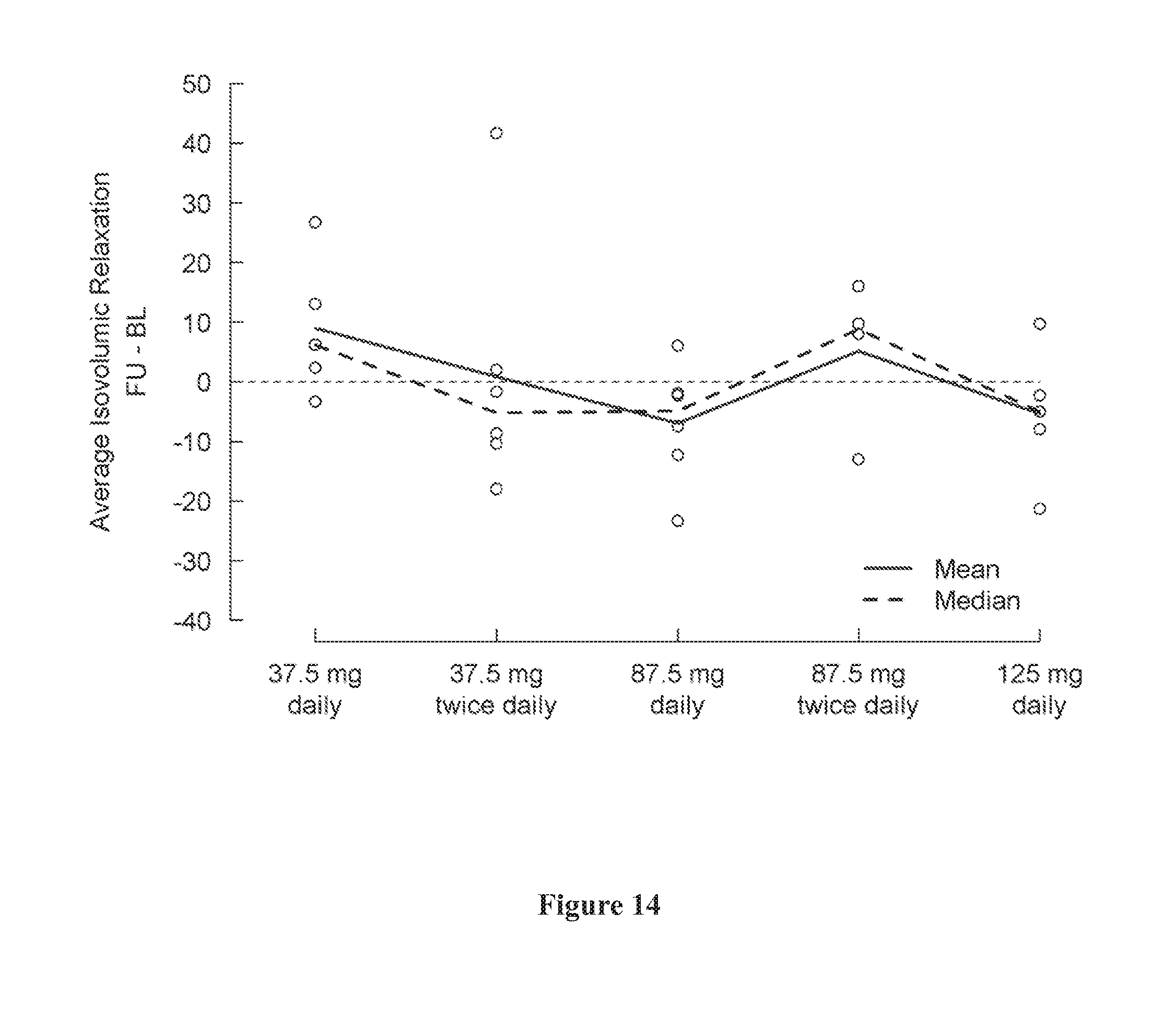
D00015

D00016

D00017

D00018
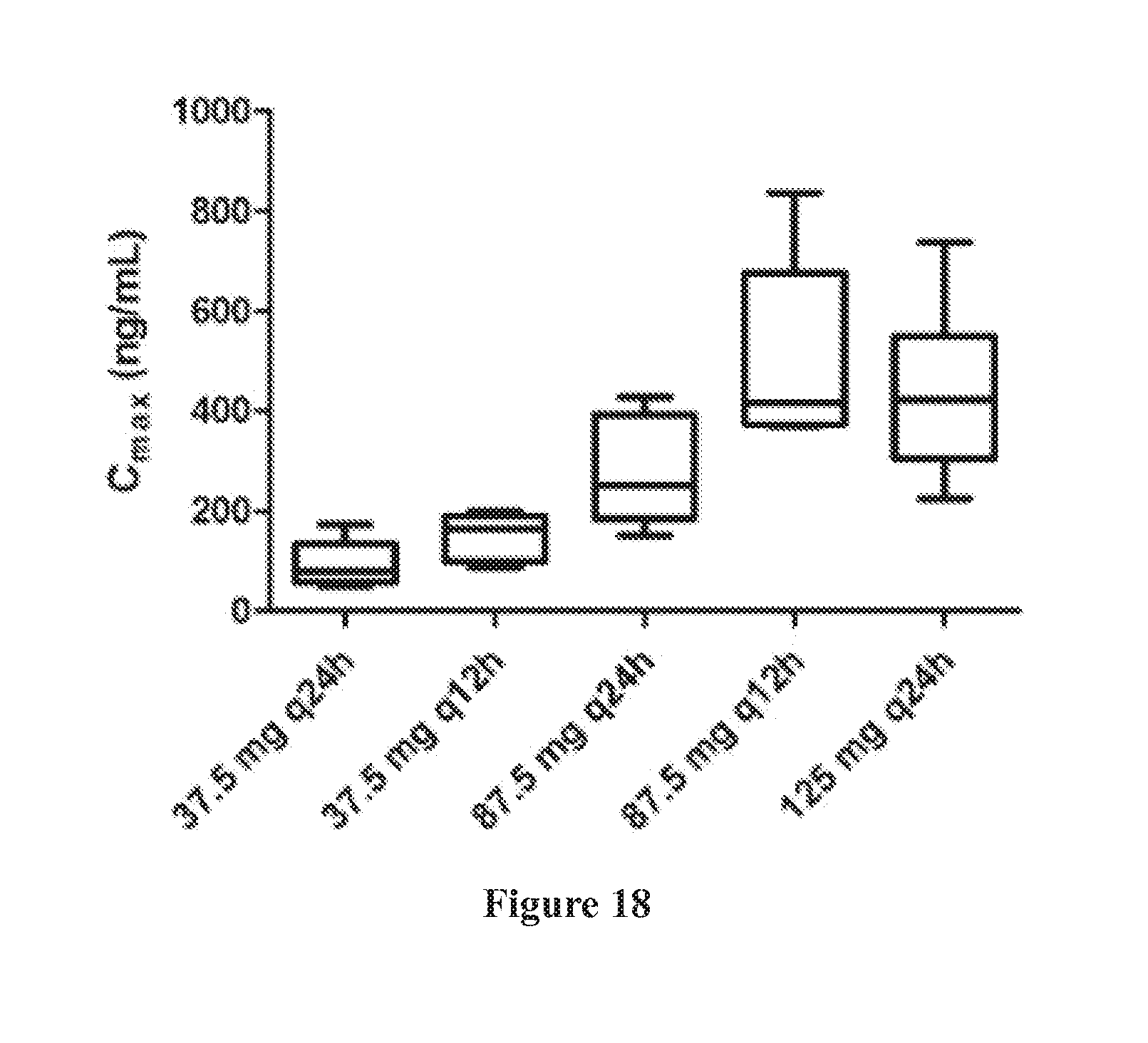
D00019
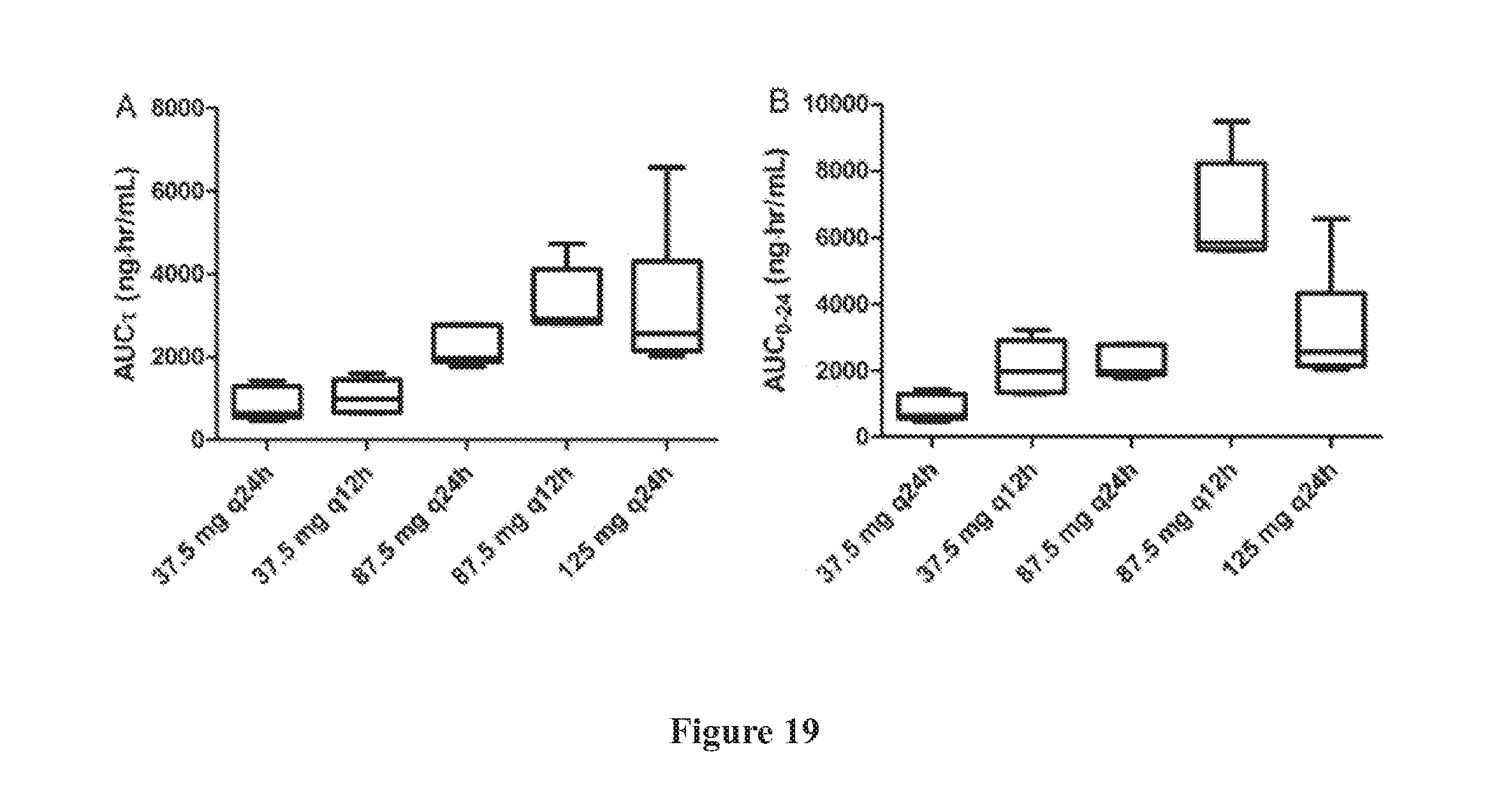
D00020

D00021
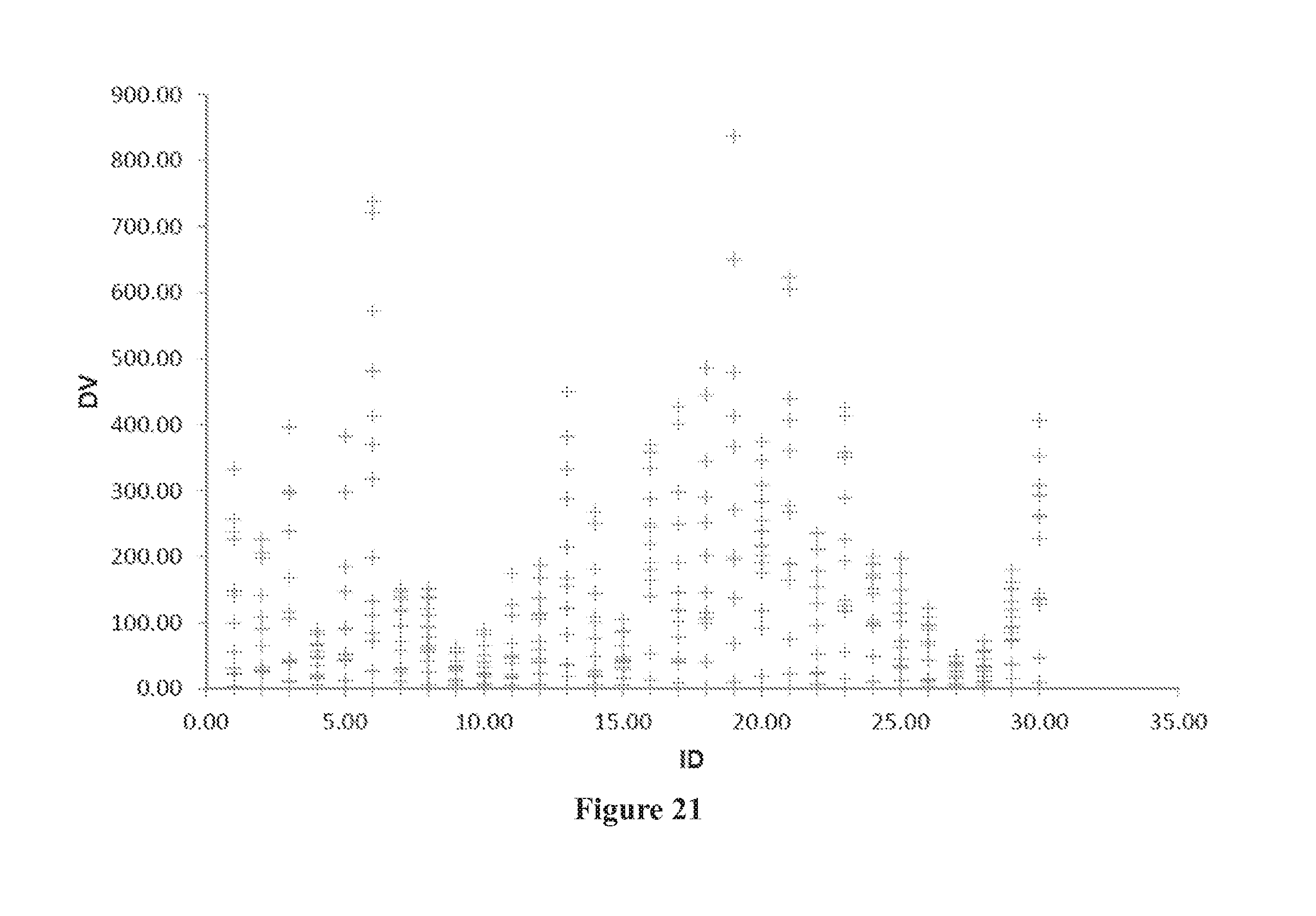
D00022
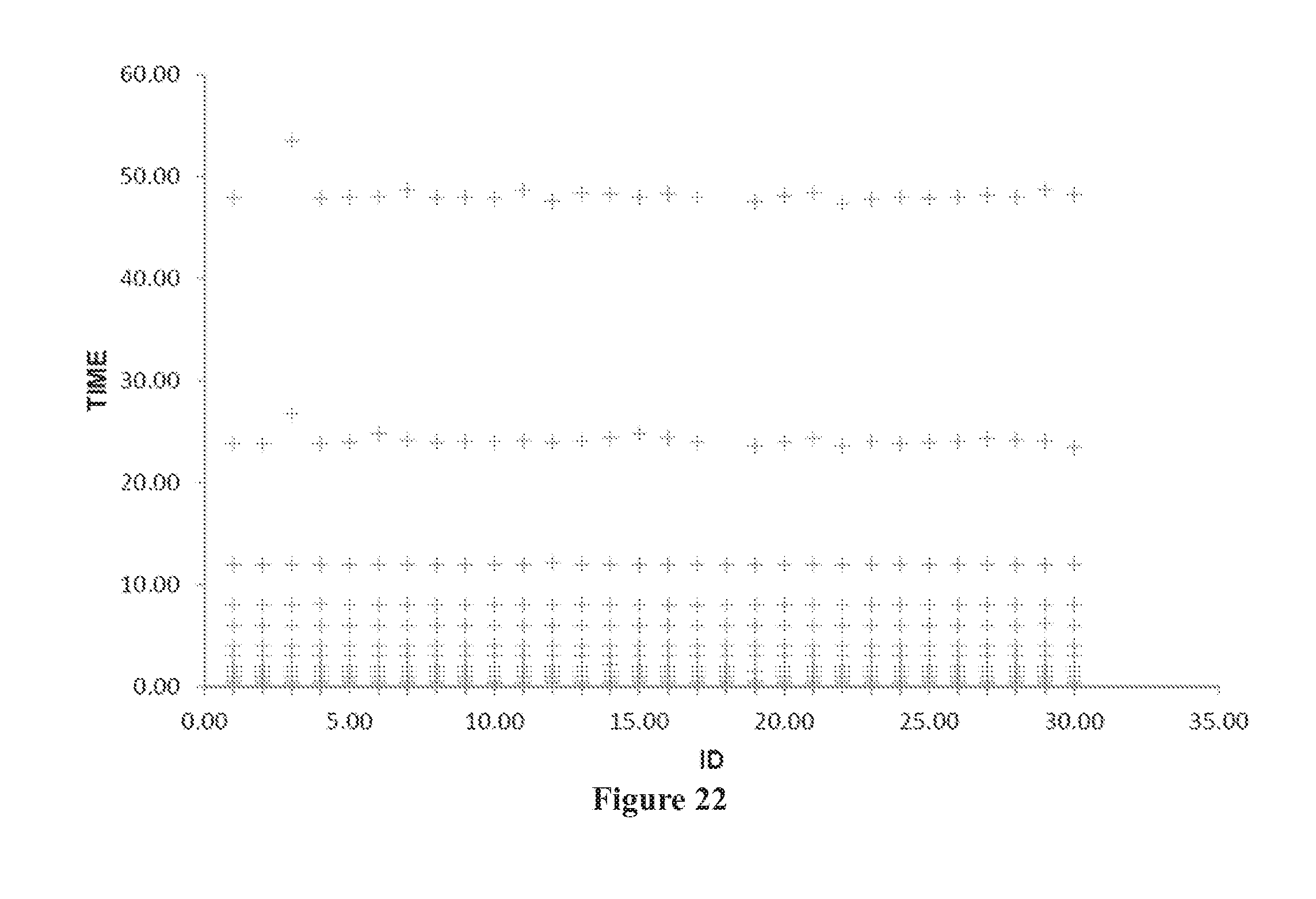
D00023
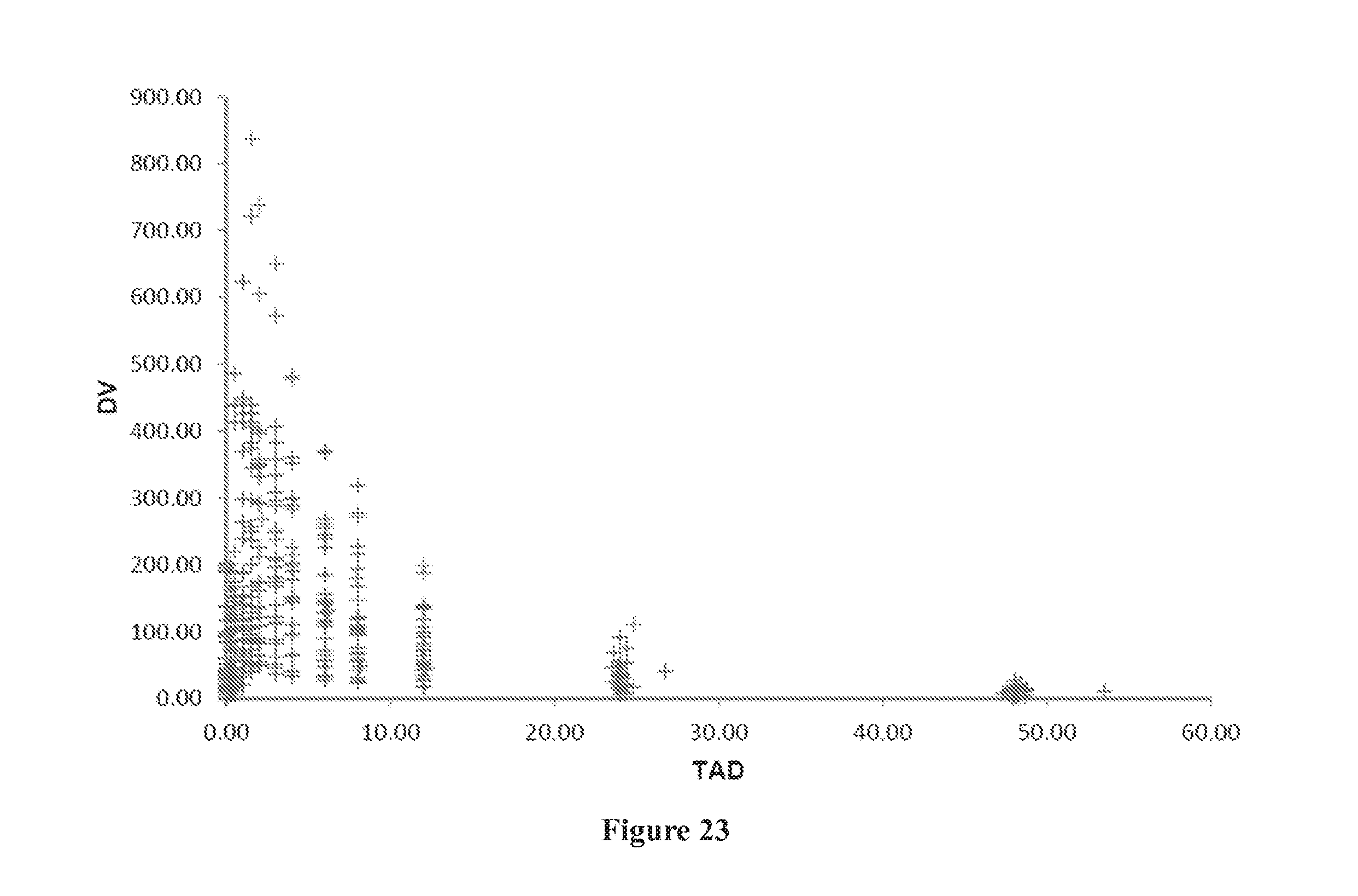
D00024
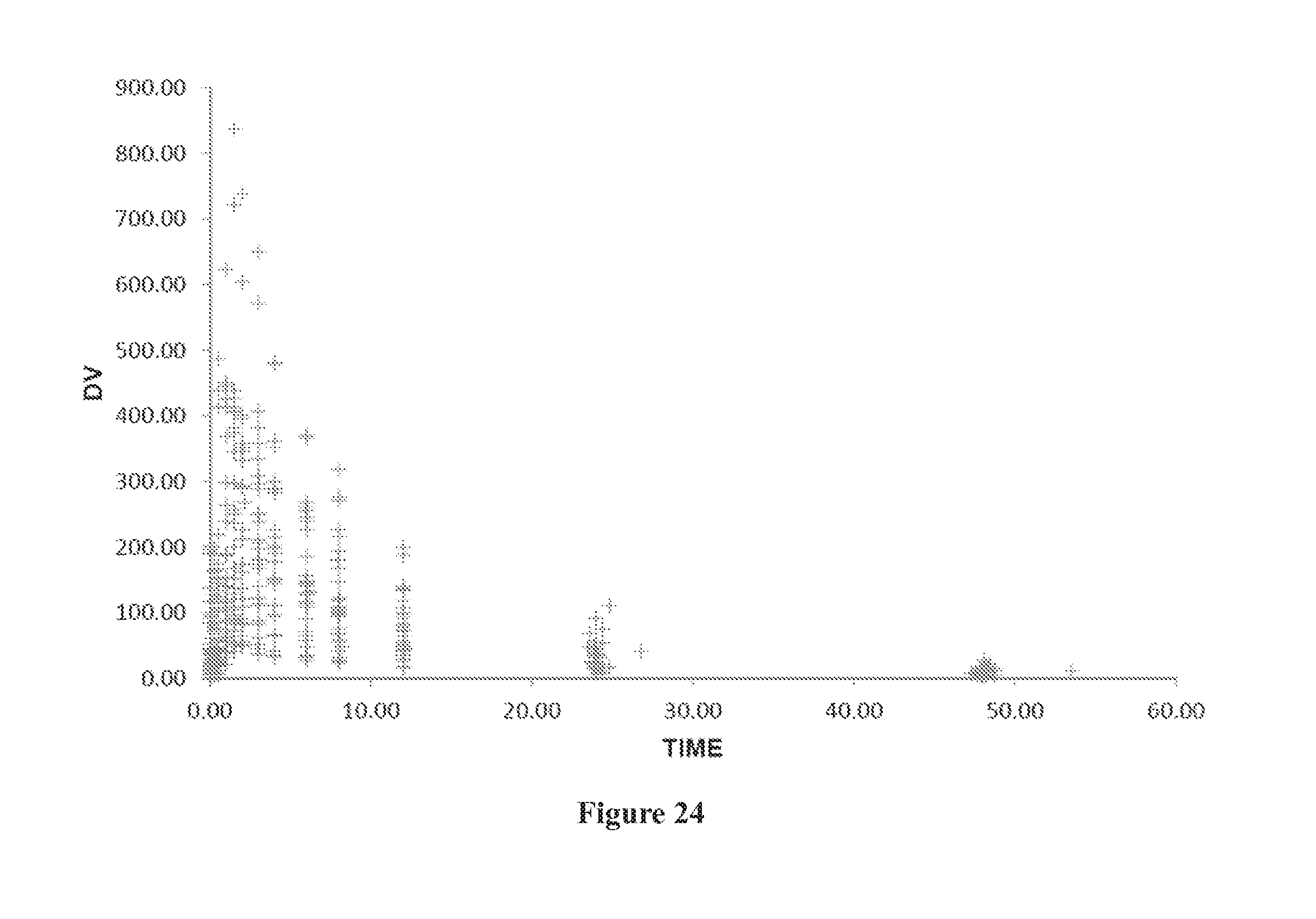
D00025

D00026
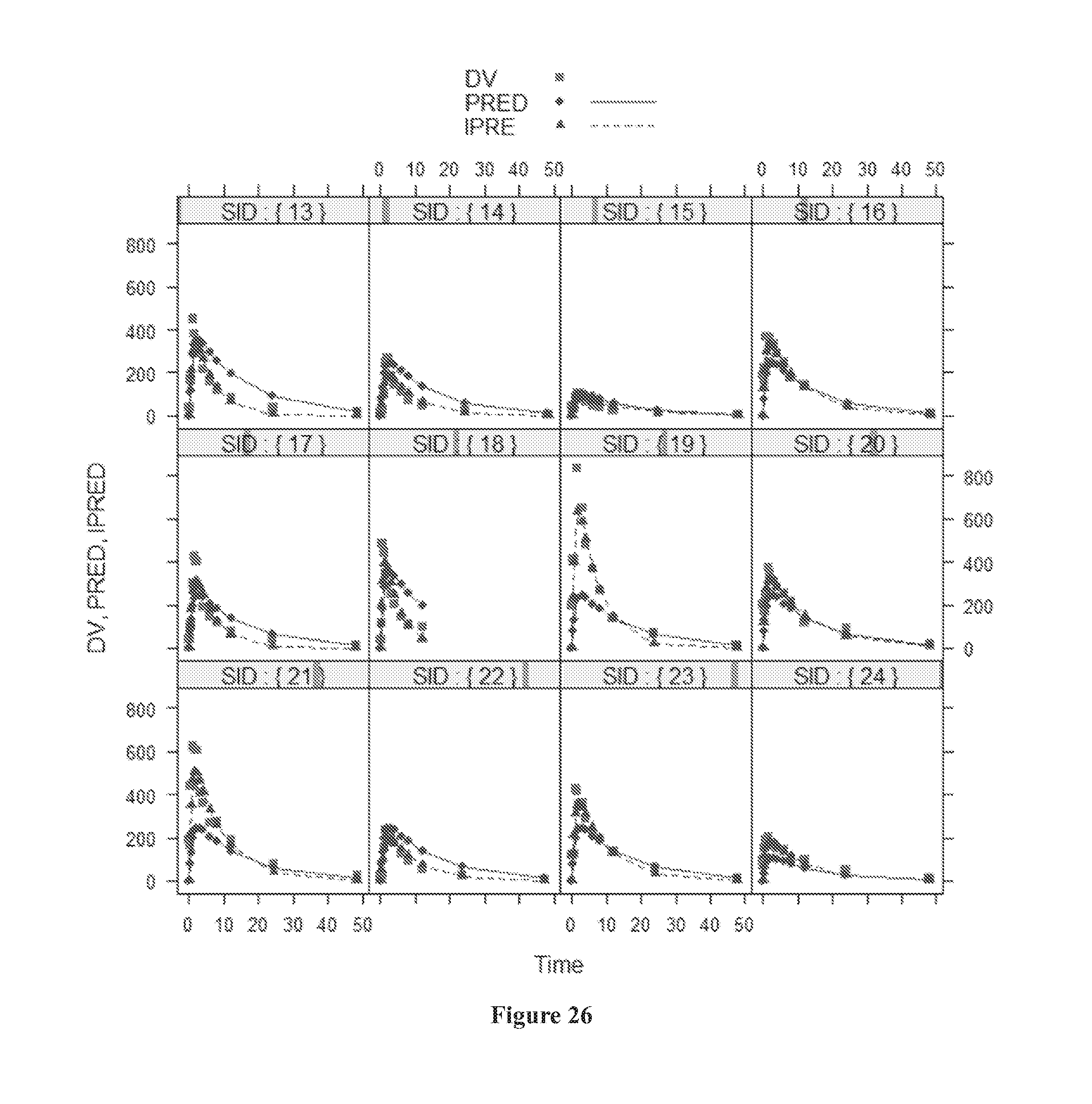
D00027
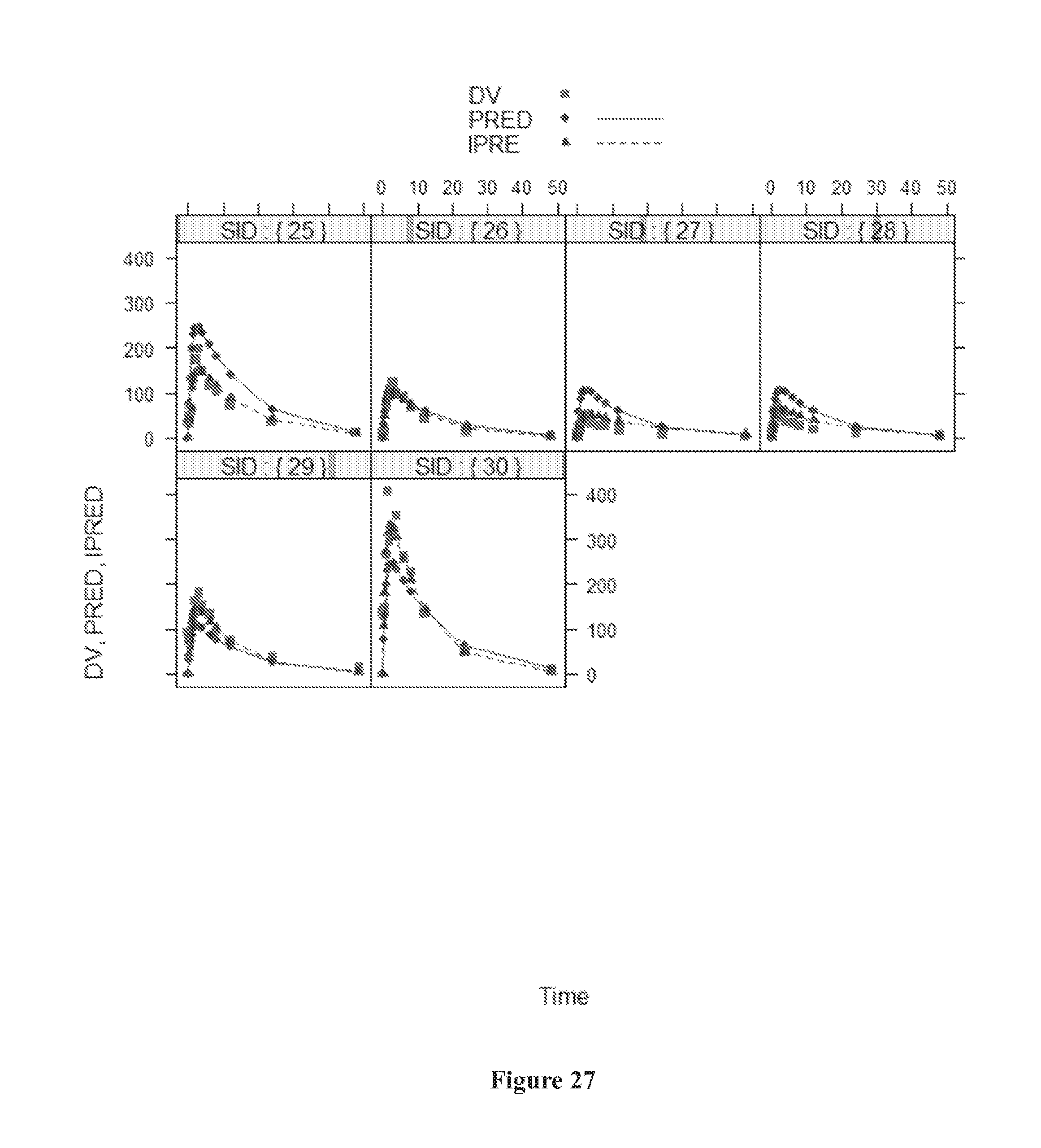
D00028

D00029

D00030
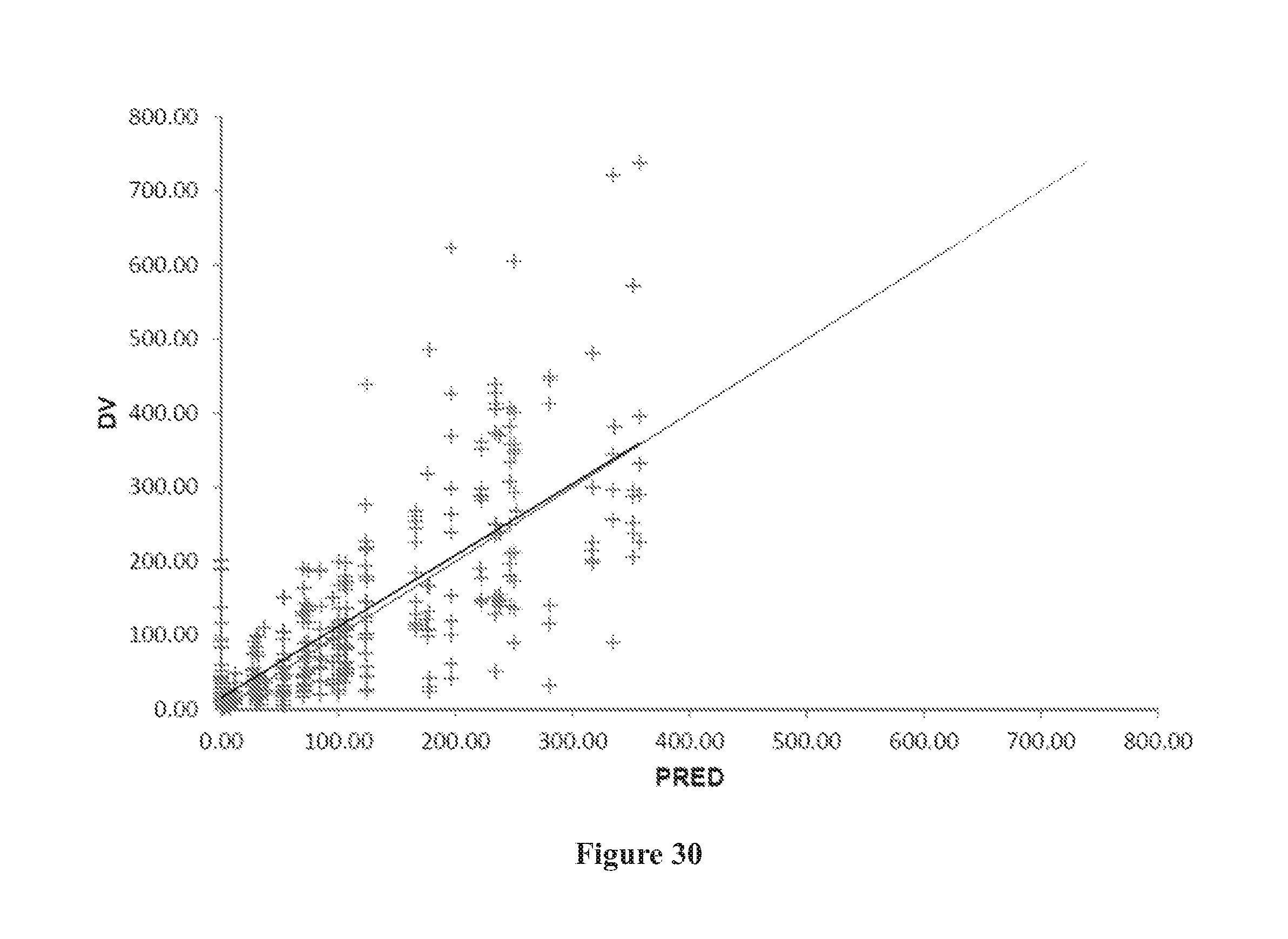
D00031
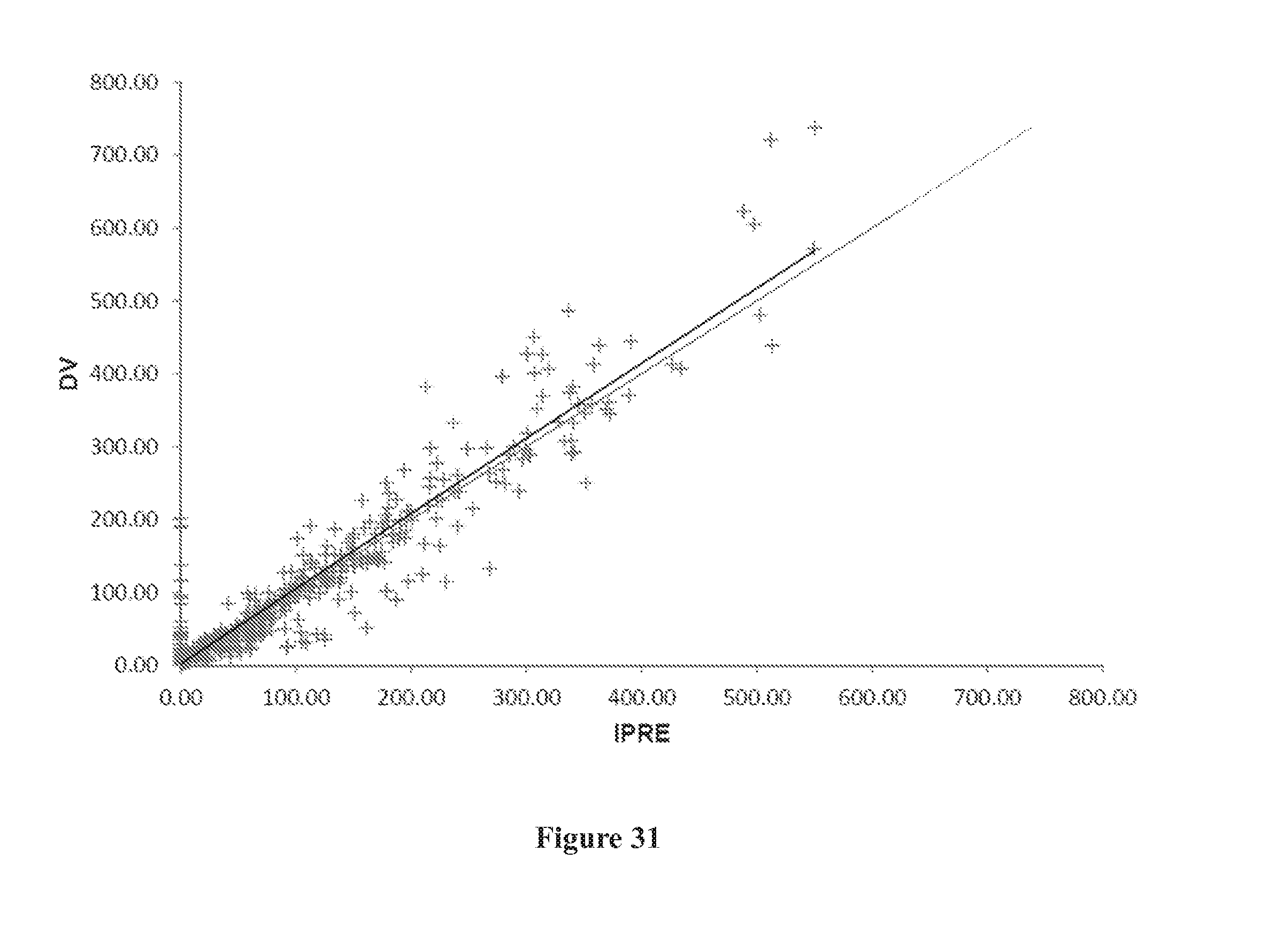
D00032
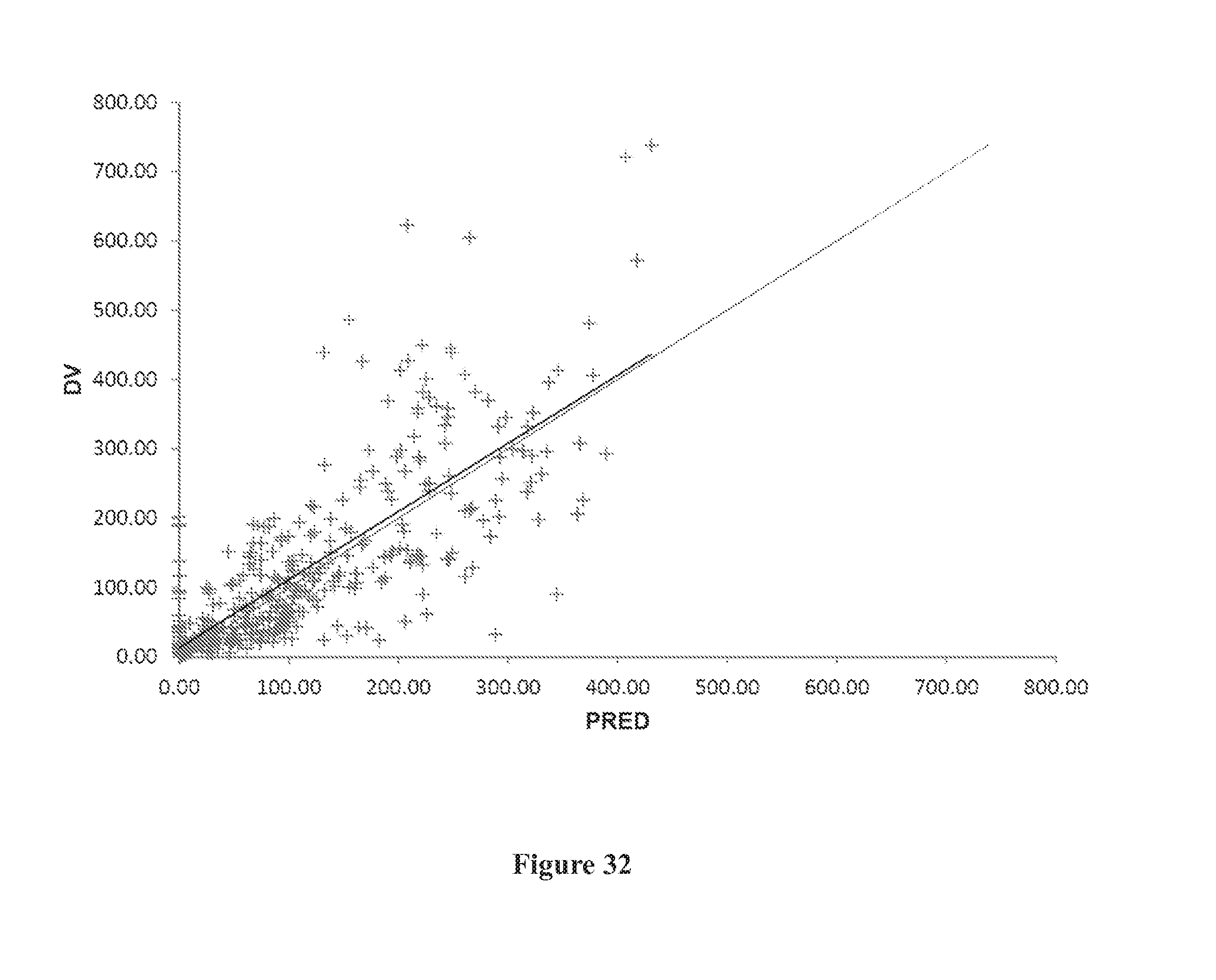
D00033
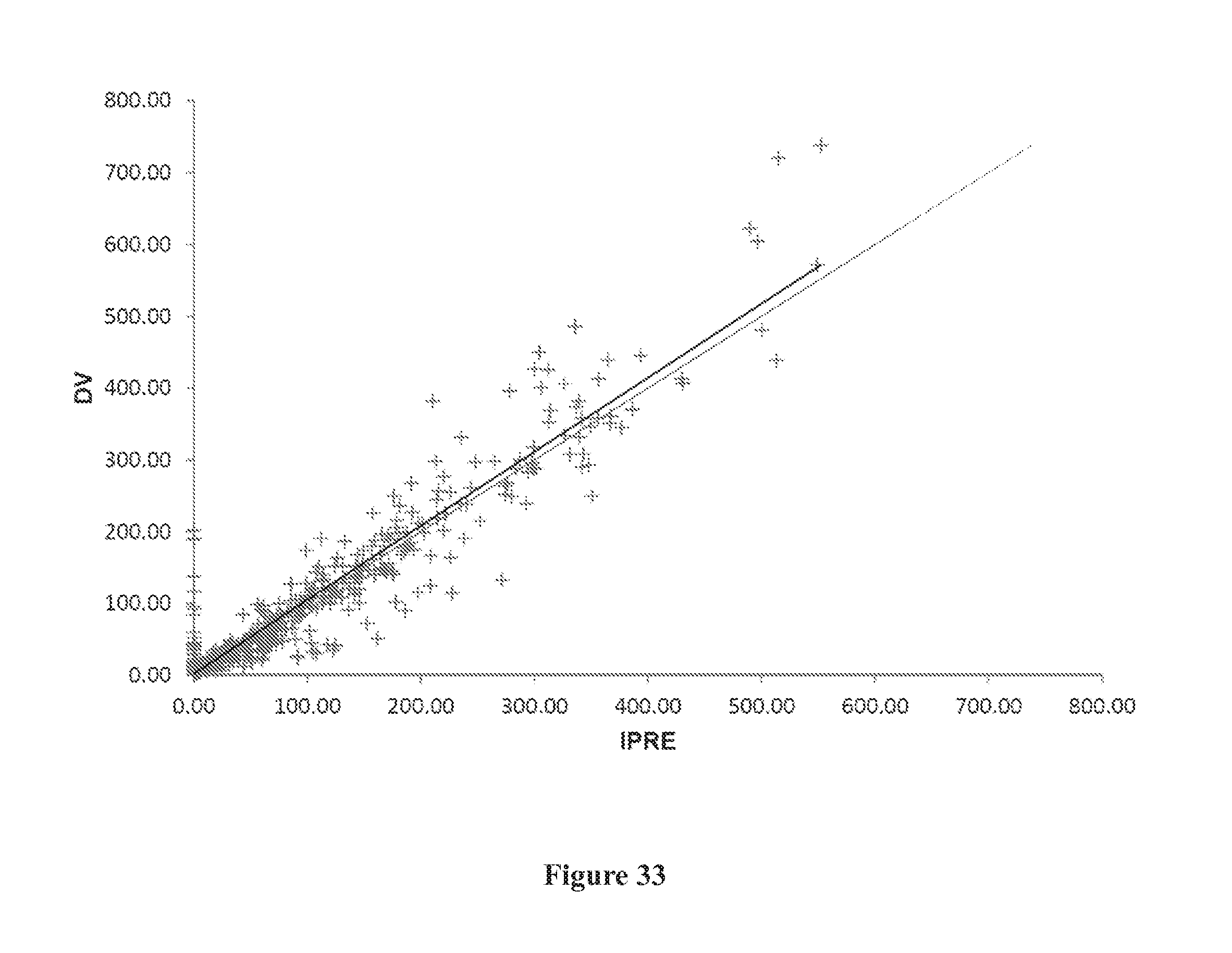
D00034



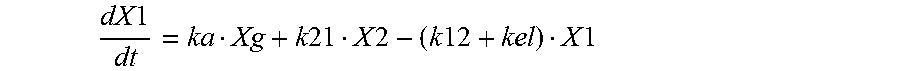
XML
uspto.report is an independent third-party trademark research tool that is not affiliated, endorsed, or sponsored by the United States Patent and Trademark Office (USPTO) or any other governmental organization. The information provided by uspto.report is based on publicly available data at the time of writing and is intended for informational purposes only.
While we strive to provide accurate and up-to-date information, we do not guarantee the accuracy, completeness, reliability, or suitability of the information displayed on this site. The use of this site is at your own risk. Any reliance you place on such information is therefore strictly at your own risk.
All official trademark data, including owner information, should be verified by visiting the official USPTO website at www.uspto.gov. This site is not intended to replace professional legal advice and should not be used as a substitute for consulting with a legal professional who is knowledgeable about trademark law.