Hierarchical Condition Categories Program
THESMAN; DEBRA
U.S. patent application number 13/167976 was filed with the patent office on 2012-12-27 for hierarchical condition categories program. Invention is credited to DEBRA THESMAN.
| Application Number | 20120329015 13/167976 |
| Document ID | / |
| Family ID | 47362176 |
| Filed Date | 2012-12-27 |
| United States Patent Application | 20120329015 |
| Kind Code | A1 |
| THESMAN; DEBRA | December 27, 2012 |
HIERARCHICAL CONDITION CATEGORIES PROGRAM
Abstract
Systems and methods of recording patient's medical documents and training programs for improving medical document recordation. The system includes a computer readable medium capable of storing medical data obtained from patients, including disease codes, a computer with software capable of evaluating the data stored on the computer readable medium for completeness, and a notification system capable of presenting to the user of the system a warning if any of the data is found to be incomplete or incorrect. The training includes evaluating the healthcare provider's current medical documentation process, training the healthcare provider in methods of recording medical documents, providing a system for recording medical documents, and training the healthcare provider in use of the system.
| Inventors: | THESMAN; DEBRA; (Garden City, NY) |
| Family ID: | 47362176 |
| Appl. No.: | 13/167976 |
| Filed: | June 24, 2011 |
| Current U.S. Class: | 434/219 ; 707/812; 707/E17.005 |
| Current CPC Class: | G09B 19/00 20130101; G06Q 10/101 20130101; G16H 10/60 20180101; G16H 15/00 20180101 |
| Class at Publication: | 434/219 ; 707/812; 707/E17.005 |
| International Class: | G09B 19/00 20060101 G09B019/00; G06F 17/30 20060101 G06F017/30 |
Claims
1. A method of recording a patient's medical documents comprising: a. obtaining medical data from the patient, wherein the data comprises disease codes; b. storing such data obtained in step (a) in electronic medical records embodied on a computer readable medium; c. evaluating said data stored in step (b) via a computer capable of interpreting said electronic medical records to ensure that the data entry is complete; and d. presenting a notification if any of the data evaluated in step (c) is found to be incomplete or incorrect.
2. The method of claim 1, wherein the disease codes are ICD-9 codes.
3. The method of claim 1, wherein the evaluation in step (c) comprises evaluating whether for each disease code there is recorded a corresponding diagnosis of the disease, status of the disease, and plan of action for the disease.
4. The method of claim 1, wherein the evaluation in step (c) comprises evaluating the obtained disease code to determine whether an improper code has been entered.
5. The method of claim 4, wherein the obtained disease code is evaluated to determine whether a more specific code should be used.
6. The method of claim 4, wherein the evaluation of the obtained disease code is determining whether a current disease has been improperly coded as a history of the disease.
7. The method of claim 1, wherein the evaluation in step (c) comprises evaluating whether there are likely disease codes that have not been obtained in step (a).
8. The method of claim 7, wherein if a diabetes code is obtained in step (a), a notification in step (d) is presented to the user that complications of diabetes should be properly coded.
9. The method of claim 1, wherein the data obtained in step (a) further comprises medication prescriptions of the patient.
10. The method of claim 9, wherein the evaluation of step (c) determines whether there is a linking disease code for each medication prescription.
11. The method of claim 1 further comprising presenting a notification to the user of the system to review the medical records for commonly unreported or miscoded diseases within a population of patients.
12. The method of claim 11, wherein the commonly unreported or miscoded diseases are selected from the group consisting of chronic kidney disease, neuropathy, peripheral vascular disease, and malnutrition.
13. A method of training healthcare providers to properly record medical documents, said method comprising the steps: a. evaluating the healthcare provider's current medical documentation process; b. training the healthcare provider in methods of recording medical documents; c. providing a system for recording medical documents, wherein the system comprises: i. a computer readable medium capable of storing medical data obtained from patients, wherein the data comprises disease codes; ii. a computer with software capable of evaluating the data stored on the computer readable medium for completeness; and iii. a notification system capable of presenting to the user of the system a warning if any of the data is found to be incomplete or incorrect; and d. training the healthcare provider in use of said system.
14. The method of claim 13, wherein the training provided in step (b) comprises instructing the healthcare provider to ensure the medical documents are sufficiently detailed and coded to achieve the correct RAF score.
15. A system for recording medical documents comprising: a. a computer readable medium capable of storing medical data obtained from patients, wherein the data comprises disease codes; b. a computer with software capable of evaluating the data stored on the computer readable medium for completeness; and c. a notification system capable of presenting to the user of the system a warning if any of the data is found to be incomplete or incorrect.
16. The system of claim 15, wherein the notification system presents a warning if a disease code does not have a corresponding recorded diagnosis of disease, status of disease, and plan of action for the disease.
17. The system of claim 15, wherein the notification system presents a warning if an improper disease code has been entered.
18. The system of claim 15, wherein the notification system presents a warning if there are likely disease codes that have not been recorded.
19. The system of claim 15, wherein the notification system presents a warning if a medical prescription is recorded without a linking disease code for the medication.
Description
CROSS-REFERENCE TO RELATED APPLICATIONS
[0001] Not Applicable
STATEMENT RE: FEDERALLY SPONSORED RESEARCH/DEVELOPMENT
[0002] Not Applicable
BACKGROUND
[0003] The present invention is directed toward improved systems and methods for collecting and reporting Hierarchical Condition Categories (HCC). More particularly, the present invention comprises training programs and software systems useful by health plans and medical practitioners to more accurately code and report HCC to comply with the Centers for Medicare and Medicaid Services (CMS) documentation and reporting requirements.
[0004] Essential to high quality and cost-effective healthcare is the proper diagnosis of a patient's condition. From a proper diagnosis, the appropriate medical attention utilized to treat the underlying condition, whether it be the performance of a medical procedure, laboratory tests, and/or prescription of medication, can be determined. To that end, and as is well-known in the art, standard diagnoses codes are extensively utilized pursuant to conventional disease classification techniques that provide a quick, well-understood method to document medical care administered to a patient. Exemplary of, and perhaps most widely utilized of such formats, is the International Classification of Diseases 9th Edition (ICD-9) three digit codes. Likewise, with respect to the medical treatment that has been rendered, such procedures are typically referenced according to Current Procedural Terminology (CPT). Also frequently referenced in connection with the delivery of healthcare are drug codes (e.g., National Drug Code, or NDC), other service codes (e.g., Healthcare Common Procedure Coding System, or HCPCS), among others.
[0005] The Balanced Budget Act of 1997 (BBA) mandated a change in Medicare's payment methodology intended to pay health plans, and subsequently medical providers, based on a patient's health status through a process called Risk Adjustment Factor (RAF). Prior to the implementation of risk adjustment, reimbursement was based solely on demographic factors, such as, age, sex, Medicaid status, county of residence, etc.
[0006] In 2004, the Centers for Medicare and Medicaid Services (CMS) implemented a new model, the Hierarchical Condition Categories (HCC), as an additive model to adjust Medicare capitation payments to private healthcare plans for their expenditure risk of enrollees based on serious or chronic conditions. In theory, the CMS-HCC model pays more accurately for predicted health expenditures, based on health status and some demographic factors. In short, treat the patient appropriately and get reimbursed for doing so.
[0007] The collection and reporting of HCCs provides important benefits to patients and improves reimbursement. When health plans and/or practitioners have their own programs for documenting, auditing, and reporting HCCs, there is an opportunity to identify those at-risk enrollees/patients who, because of their disease markers, would benefit from increased frequency of visits and intensity of services, enrollment in complex care management, chronic care programs, and/or transitional care programs when appropriate - all designed to ensure the best possible clinical outcome for patients and cost savings for health plans and practitioners. Examples of such other programs are described in U.S. Pat. Nos. 7,657,442 and 7,464,041 and U.S. patent application Ser. Nos. 11/352,028 and 12/834,767, the entire teachings of which are collectively incorporated by reference herein.
[0008] Accordingly, there is a need in the art for a program designed to train and support health plans and practitioners the art and skill of correctly coding and reporting HCC to comply with CMS-HCC documentation and reporting requirements.
BRIEF SUMMARY
[0009] One aspect of the present invention is directed toward methods of recording a patient's medical documents. The methods include obtaining medical data from the patient, storing the data in electronic medical records embodied on a computer readable medium, evaluating the data via a computer capable of interpreting said electronic medical records to ensure that the data entry is complete, and presenting a notification to a user if any of the data is found to be incomplete or incorrect. The medical data obtained from the patient may include any of various relevant data, such as demographic information, medications taken, and symptoms suffered, but particularly includes disease codes. For example, the disease codes may be ICD-9 codes.
[0010] The data evaluation may take numerous forms, for example, whether for each disease code there is recorded a corresponding diagnosis of the disease, status of the disease, and plan of action for the disease and/or whether an improper code has been entered for each disease. More particularly, the obtained disease code may be evaluated to determine whether a more specific code should be used in its place. For example, whether a current disease has been improperly coded as a history of the disease. Another possible evaluation is whether there are likely disease codes that the patient may be suffering from that were not recorded. One example of this is when the patient is suffering from diabetes. A majority of patients suffering from diabetes have complications due to the diabetes. A notification may be provided to the user that complications of diabetes should be properly coded.
[0011] The medical data obtained may further include medication prescriptions of the patient and evaluating whether there is a linking disease code for each medication prescription. Additionally, a notification may be presented to the user of the system to review the medical records for commonly unreported diagnosed diseases within a set population of patients. Examples of commonly unreported diagnosed diseases include chronic kidney disease, neuropathy, peripheral vascular disease, and malnutrition.
[0012] Another aspect of the present invention is directed toward methods of training healthcare providers to properly record medical documents. This training includes evaluating the healthcare provider's current medical documentation process, training the healthcare provider in methods of recording medical documents, providing a system for recording medical documents, and training the healthcare provider in use of the system. The system includes a computer readable medium capable of storing medical data obtained from patients, including disease codes, a computer with software capable of evaluating the data stored on the computer readable medium for completeness, and a notification system capable of presenting to the user of the system a warning if any of the data is found to be incomplete or incorrect.
[0013] In particular, the training provided may include instructing the healthcare provider to ensure the medical documents are sufficiently detailed and coded to achieve the correct RAF score for each patient.
[0014] Yet another aspect of the present invention contemplates a system for recording medical documents. The system includes a computer readable medium capable of storing medical data obtained from patients, including disease codes, a computer with software capable of evaluating the data stored on the computer readable medium for completeness, and a notification system capable of presenting to the user of the system a warning if any of the data is found to be incomplete or incorrect.
[0015] For example, the notification system may present a warning if a disease code does not have a corresponding recorded diagnosis of disease, status of disease, and plan of action for the disease, if an improper disease code has been entered, if there are likely disease codes that have not been recorded and/or if a medical prescription is recorded without a linking disease code for the medication.
BRIEF DESCRIPTION OF THE DRAWINGS
[0016] These and other features and advantages of the various embodiments disclosed herein will be better understood with respect to the following description and drawings, in which like numbers refer to like parts throughout, and in which:
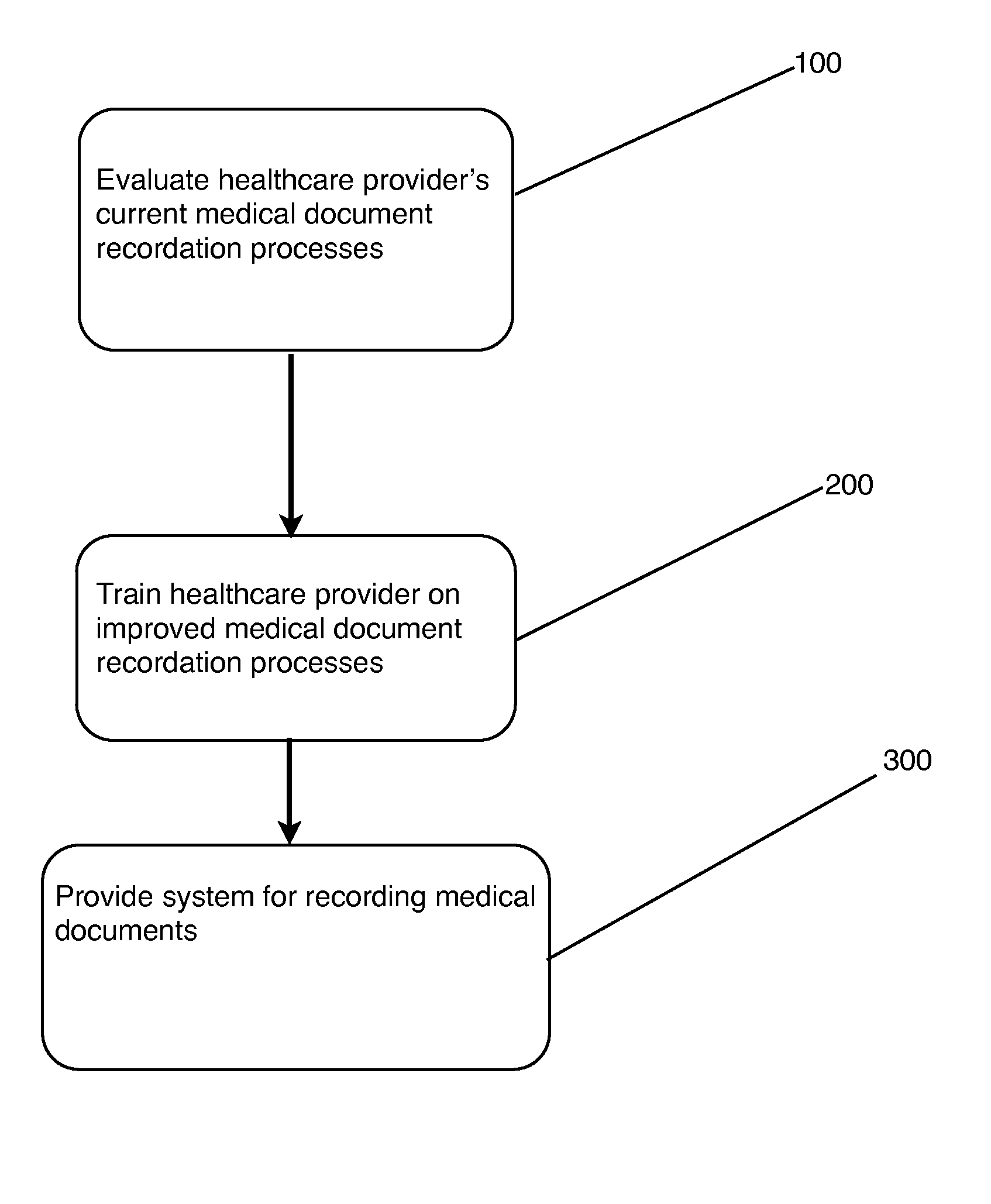
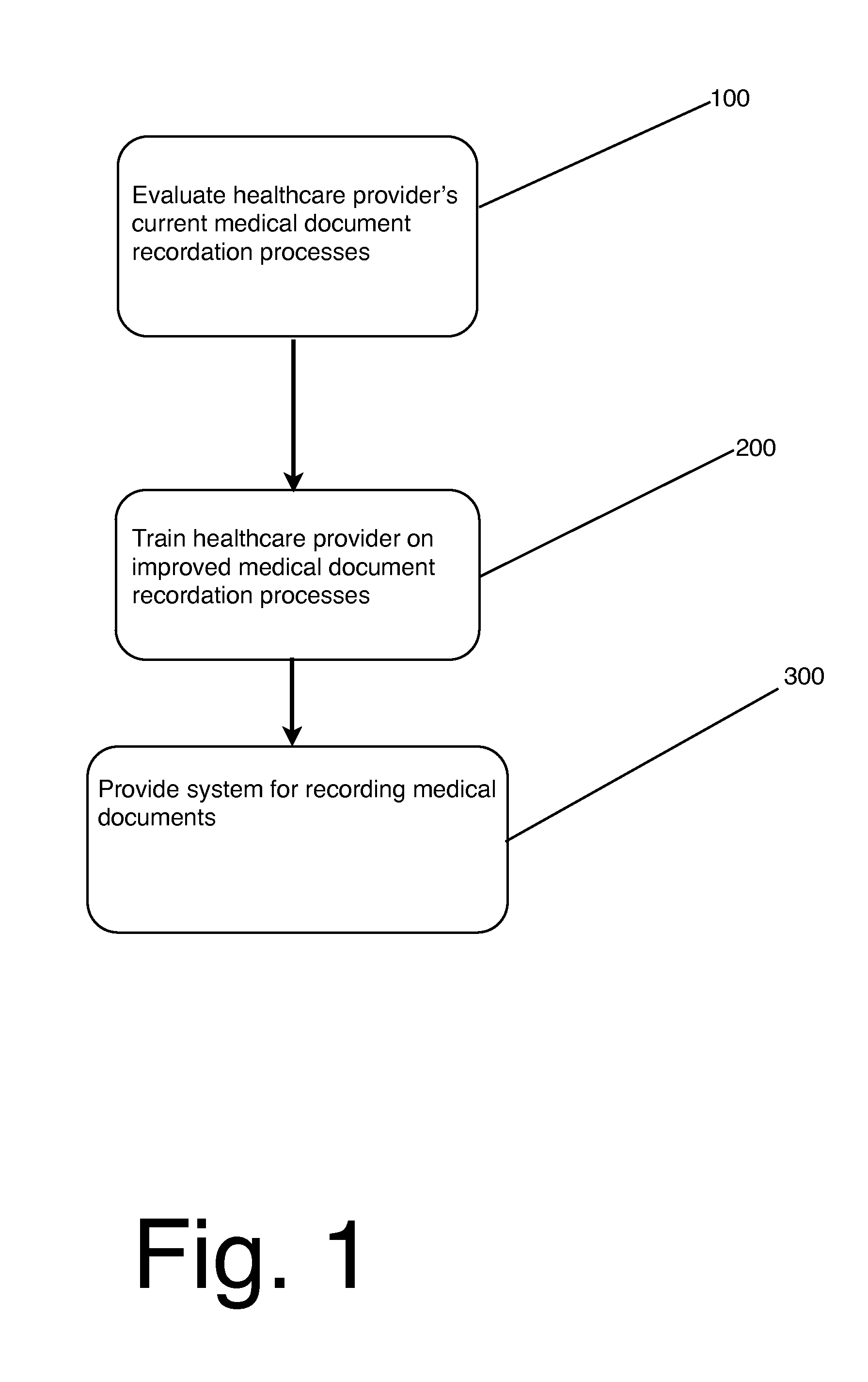
[0017] FIG. 1 is a flowchart depicting the steps for practicing the present invention as it relates to training healthcare providers in improved medical document recordation practices.
DETAILED DESCRIPTION
[0018] The detailed description set forth below is intended as a description of the presently preferred embodiment of the invention, and is not intended to represent the only form in which the present invention may be constructed or utilized. The description sets forth the functions and sequences of steps for constructing and operating the invention. It is to be understood, however, that the same or equivalent functions and sequences may be accomplished by different embodiments and that they are also intended to be encompassed within the scope of the invention.
[0019] Referring now to FIG. 1, there is schematically illustrated the various steps by which a method of the present invention operates to train healthcare providers in improved medical document recordation practices. In particular, there is a first step 100 of evaluating the healthcare provider's current medical document recordation processes. For example, a team consisting of physicians, nurses, and financial auditors may conduct a two day on-site evaluation of the client's current HCC activities to determine data extraction and reporting methodology and validates the client's current RAF score.
[0020] A written report may be given to the client outlining the team's findings and recommendations that include staffing requirements, system requirements, and/or a program training and implementation work plan.
[0021] The second step 200 includes a comprehensive educational training program. For example, the training program may be offered as a ten day class with overhead presentations, case studies, and reference material, with topics including risk adjustment methodology, documentation training, Hierarchical Condition Coding (including commonly unreported or miscoded conditions), and training on systems for recording medical documents. The training section 200 may include a ninety day post-implementation followup with client's staff to evaluate program progress and/or an at least annual update to keep client apprised of changes in the CMS-HCC model.
[0022] The third step 300 is providing to the healthcare provider a system for recording medical documents, wherein the system includes at least a computer readable medium capable of storing medical data obtained from patients, wherein the data comprises disease codes; a computer with software capable of evaluating the data stored on the computer readable medium for completeness; and a notification system capable of presenting to the user of the system a warning if any of the data is found to be incomplete or incorrect. Examples of data to be recorded and warnings that may be presented by the system are discussed in greater detail below.
Risk Adjustment Methodology and Documentation Training
[0023] In order for the diagnostic classification system of the present invention to function properly the following principles may be used: 1) diagnostic categories should be clinically meaningful; 2) diagnostic categories should predict medical expenditures; 3) diagnostic categories that will affect payments should have adequate sample sizes to permit accurate and stable estimates of expenditures; 4) in creating an individual's clinical profile, hierarchies should be used to characterize the person's illness level with each disease process; 5) the diagnosis classification should encourage specific coding; 6) the diagnostic classification should not reward coding proliferation; 7) providers should not be penalized for recording additional diagnoses; 8) the classification system should be internally consistent; 9) the diagnostic classification should assign all ICD-9 codes; and 10) discretionary diagnostic categories should be excluded from payment models.
[0024] The Risk Adjustment Factor (RAF) is calculated by adding together a demographic factor (based upon, for example, the age and sex of the patient) and the total of a Hierarchical Condition Category (HCC) risk adjusted diagnosis. There are seventy disease categories, with over 3,100 diagnoses, available to apply toward the HCC risk adjusted diagnosis. A particular numerical "risk factor" is assigned to each category. Since the HCC is an additive model, the risk factor from all diagnoses are combined to reach the total RAF. Furthermore, the HCC is a predictive model, i.e., it is utilized to determine a future year payment based on coding this year's date of service. In summary, a higher RAF is obtained by sicker patients, thereby resulting in higher payments; whereas healthier patients will have a lower RAF, resulting in lower payments.
[0025] In particular, payments are determined through diagnosis coding after providing face to face patient evaluation at least once a year. As such, appropriate chart documentation and diagnosis reporting is required for accurate reimbursement. This documented information is submitted from the healthcare provider to the patient's health plan (HP), which in turn submits the data to the Centers for Medicare and Medicaid Services (CMS). CMS then takes the provided data and scrubs it for duplication and accuracy. The scrubbed data is then used by CMS to determine the revenue to provide to the HP. The HP then reimburses the health care provider based upon their contract. As such, it can readily be seen that proper diagnosis coding drives the RAF scorers, which in turn drives the reimbursement. Without proper documentation, the full reimbursement will not be retained.
[0026] It is important to note that with proper coding, patient care remains the priority. Once appropriate care is delivered to the patient, how to properly code for that care becomes important. However, care is not altered to meet coding strategies; rather, the reverse is the case, i.e., proper care drives proper coding. CPT codes reflect the level of care provided, but ICD-9 codes reflect the disease state addressed. Disease states submitted for a specific visit must be addressed and documented for that visit. The most missed diagnoses in senior patients are chronic kidney disease, peripheral vascular disease, peripheral neuropathy, and major depression. In order to properly document a patient visit, the chart must contain the patient's name (on each page, if the notes span multiple pages), the patient's date of birth or some other unique identifier, the date of service, and a handwritten or electronic signature of the caregiver, including credentials. Furthermore, validated HCC coding requires three documented points: 1) The diagnosis or assessment; 2) the status or condition (e.g., stable, condition worsening, medication adjusted, tests ordered, documentation reviewed, condition improving, etc.); and 3) a plan of action. Under the official ICD-9 coding guidelines, a diagnosis can only be coded when it is explicitly spelled out in the medical record. Accordingly, all documentation used for coding must be specific, and the mere fact that a patient has a condition is not sufficient on its own. Additionally, under ICD-9 guidelines, a diagnosis cannot be coded unless it is stated in the current visit documentation. All conditions that coexist at the time of the visit should be coded if they require or affect patient care, treatment, or management and are addressed in the medical record for the specified visit.
[0027] As discussed above, merely listing diagnoses is not sufficient documentation, as a diagnosis, status, and plan of action must all be documented for proper coding. Furthermore, merely listing medications does not meet documentation requirements to indicate that an evaluation for that condition was done. Also, superbills, encounter forms, and referrals are not acceptable forms of documentation as they are not considered a part of the medical record. Therefore, when a diagnostic report is provided it must be interpreted by the medical practitioner and documented for proper coding purposes. Additionally, a diagnosis must be presented unconditionally, without using terms such as "ruled out", "probable", "consistent with" and the like.
[0028] In an attempt to verify that diagnoses are being properly documented, CMS annually audits medical records. These audits are called Risk Adjustment Data Validation (RADV). Health plans, hospitals, medical groups, and physician offices are required to comply with CMS requests for medical records, and unsubstantiated diagnoses may result in recoupment of payments. In particular, the documentation substantiating that the patient was evaluated, monitored, or treated for the condition is a requirement for receiving reimbursement and must include all three of a diagnosis, status, and plan of action.
[0029] It is important to note that causal relationships of diseases need to be explicitly stated in the record, they cannot be inferred. Accordingly, linkage can be established in the chart with terms such as the specific disease being "due to", "associated with", "secondary to" or the like should be used to establish a cause and effect relationship. Terms such as "with", "probable", "more than likely" and the like do not sufficiently support linkage. For example, merely charting Type II Diabetes and Chronic Kidney Disease results in a significantly lower HCC RAF weight than would a proper charting of Type II Diabetes with Renal Manifestations and Chronic Kidney Disease due to Diabetes. Coding in the latter manner leaves no room for error in interpretation as to the disease states.
[0030] Another key aspect of proper charting is the correct documentation of a patient's "history of" a disease. The "history of" a disease should only be charted when the patient has been cured and is no longer being actively treated for the disease. A "history of" indicates that the medical condition no longer exists and the patient is not receiving any treatment, but there is the potential for recurrence and therefore requires continued monitoring. A "history of" a disease should not be used to describe a current acute or chronic condition even if it is controlled on medication. As long as the condition exists, despite totally successful and stable status, the condition must be coded as an active condition.
[0031] On an at least annual basis, a patient's chronic and active conditions should be documented so as to not overlook certain conditions. For example, chronic heart failure (CHF), chronic obstructive pulmonary disease (COPD), diabetes mellitus (DM), chronic kidney disease (CKD), neuropathy, and peripheral vascular disease (PVD) are chronic conditions that should be charted and are commonly unreported diagnoses. Furthermore, the patient's medication list should be reviewed to ensure there is a diagnosis associated with each medication. While patient care remains the priority at all times, without proper documentation in the medical record reimbursement will not occur. Following are certain examples of chronic conditions and proper methods of charting.
Diabetes
[0032] More than sixty percent of seniors with diabetes have a manifestation or complication of the diabetes. These complications must be properly charted, but are the most frequently omitted conditions in physician medical records. Good quality of care and reimbursement rely on the details. For example, it needs to be documented whether the patient suffers from Type I or Type II, whether there are complications associated with the diabetes, which systems are affected by the complications, and whether the blood glucose levels are controlled or uncontrolled.
[0033] When complications are due to diabetes, the documentation must make that connection explicitly. Additionally, every patient with diabetes should be evaluated for the many manifestations, complications, and co-morbidities of the disease, with progress notes and tests to show the evaluation was done. Exemplary possibilities are renal, ophthalmic, neurological, circulatory, other specified, and unspecified manifestations. Diabetes with manifestation codes have higher RAFs and, therefore, receive higher reimbursements. Even though only the highest weighted diabetes code will count toward the risk adjusted HCC model, all applicable manifestations should be charted.
[0034] Diabetes with manifestations require at least two separate codes; one for the diabetes with manifestation and one for the supporting associated diagnosis. For example, a patient with "diabetes with renal manifestation", aside from receiving a code for the diabetes, would also require a second code for what the manifestation is. Incomplete coding of the diabetes with renal manifestation by itself does not fully describe the manifestation or complication and would not receive the appropriate RAF.
Chronic Kidney Disease
[0035] Coding for CKD conforms to the stages of CKD, including stages I-IV based on a patient's glomerular filtration rate (GFR) (estimated from a urinalysis and/or serum creatinine levels) and/or kidney damage. However, some patients with "normal" creatinine levels have significant renal function impairment. As such, CKD-I and CKD-II are commonly missed. For those at risk of renal disease, creatinine clearance of GFR should be estimated at least twice per year. Further, the cause of the CKD should be checked and coded for a cause and effect linkage, for example, diabetes or hypertension. Unspecified kidney issue terminology such as chronic renal disease, chronic renal failure, and chronic renal insufficiency do not affect the RAF and should be avoided in favor of more specific diagnoses.
Cardiology
[0036] An important issue when documenting a significant cardiac diagnosis is to be specific. For example, less specific terms, such as, coronary artery disease or atherosclerotic heart disease, should be avoided if the patient has more specific diagnoses, such as, angina or history of myocardial infarction (MI). An acute MI is considered to be present for the first eight weeks after occurrence. If a patient is seen eight weeks after an acute MI and has not continued anginal symptoms, the coding should be changed to recent, old, or history of MI.
[0037] Cardiac angina is coded if currently being treated and may be continue to be coded even if asymptomatic due to pharmacological treatment. Other ongoing chronic cardiac conditions, such as, atrial fibrillation or arrhythmias should be documented and coded whether symptomatic or asymptomatic if continued pharmacological treatment or interventional cardiology is present. Of note, congestive heart failure is always a chronic condition after diagnosis, and echocardiograms should be used to evaluate and document diastolic heart failure.
Malnutrition
[0038] Malnutrition is often observed in senior patients due to conditions that limit nutrient ingestion and absorption, such as, cancer, pancreatitis, alcohol abuse, liver disease, obesity, CHF, COPD, end stage renal disease (ESRD), celiac disease, cystic fibrosis, depression, and dementia. However, malnutrition is often underreported and merely reported as being "underweight", "failing to thrive", or "loss of appetite" which do not affect the RAF. In these situations, occurrences of malnutrition should be identified.
Psychiatry
[0039] Episodic mood disorders are mental diseases that include mood disturbances such as major depression. The characteristics of these mood disturbances should be carefully documented and specific mental disorder terminology should be used in the final diagnosis, otherwise there will be no RAF adjustment. Furthermore, maladaptive patterns of substance use, leading to clinical impairment or distress should be coded as a dependence, rather than abuse.
Oncology
[0040] Malignancies are only coded until the patient has completed definitive treatment, such as surgery, chemotherapy, and/or radiation therapy aimed at eradicating the malignancy. Furthermore, breast and prostate cancer patients on adjuvant therapy are coded as having the active disease. However, once a patient has completed therapy, he or she can only be coded with a "personal history of cancer" diagnosis even if undergoing surveillance for reoccurrence of the malignancy.
[0041] It is extremely important to document when metastatic disease is present, as it has a separate coding section and CMS-HCC payment group. In this case, lack of specificity in the documentation can lead directly to a lower payment rate. Often, metastases are not clearly identified, thereby improperly leading to the coding of multiple primary malignancy sites.
Podiatry
[0042] Commonly under-diagnosed HCC conditions may be uniquely discovered by podiatrists, such as peripheral vascular disease, peripheral neuropathy, and skin ulcers. Again, if these conditions are due to a patient's diabetes, it is important to document by using two separate codes: one for the diabetes with circulatory or neurological manifestations and one for the supporting manifestation code.
Software for Electronic Medical Records
[0043] As can be seen from the examples provided above, there are numerous pitfalls that can be fallen into when documenting a patient's medical record, resulting in improperly coded, and under-reimbursed, diagnoses. Certain goals of the present invention are to train caregivers to properly document medical diagnoses and to provide a software platform for taking, storing, and aiding the caregiver in properly coding the medical records of patients.
[0044] Aside from, and in addition to, the training provided to caregivers in proper coding methodologies, as discussed in greater detail above, the present invention envisions a software platform (herein referred to as iCode) to improve compliance with CMS' s correct coding initiative and HCC extraction and reporting. iCode allows for the enhanced care of Medicare Advantage enrollees, provides valuable information to the caregiver at the point of care, reduces duplicate and costly services by providing a comprehensive clinical history for each patient, and assists with capturing qualifying CMS-HCC codes.
[0045] In particular, iCode is capable of importing data from a caregiver's current medical records, billing files, health plan claim files, and the like. iCode then auto-populates each field from the data import to create new electronic medical records, analyzes the data, and creates reports of the analyzed data. Examples of such reports include, patient demographic information, health plan eligibility history, outstanding tests/procedures affecting performance per HEDIS measurements, summary of reported chronic conditions, list of potential unreported HCCs per review category, list of three year medical history by ICD-9 and CPT classifications, last six months of pharmacy data, and notes and comments. All captured data fields can be output as an iCode report.
[0046] Of particular relevance, however, is the ability of iCode to recommend potential missed coding opportunities based upon the medical conditions that have been entered in relation to historically incorrectly reported or underreported conditions. For example, iCode may recommend to the caregiver that in order for proper coding, a diagnosis of a disease, the status of the disease, and a plan of action must all be recorded.
[0047] Similarly, iCode may recommend to the caregiver that certain disease codes which do not affect the RAF have similar codes that do affect the RAF and may have been overlooked. For example, if a caregiver records a "history of" a disease, when in fact the patient is still suffering from the disease state, or if the records indicate less specific terminology for a disease state which may be more accurately described with a condition that does affect the RAF.
[0048] Another example of a suggestion iCode may make to the care giver is whether related complications of a disease have been improperly coded, or not coded at all. For example, patients suffering from diabetes typically have other disease states that are complications from the underlying diabetes. Unless these conditions are coded as deriving from the underlying diabetes, the RAF score is not properly assigned.
[0049] Additionally, iCode may recommend, upon annual reviews, that each medication prescribed to the patient needs a corresponding disease diagnosis coded, or recommend potential commonly miscoded or unreported diseases, such as chronic kidney disease, peripheral vascular disease, or malnutrition.
[0050] Along these lines, the recommendations provided by iCode are just that, recommendations. It is noted that the iCode software will never make changes or adjustments on its own to the entered medical records, but rather acts as a warning system to the caregiver for potentially overlooked diagnoses that should be coded on further inspection by the caregiver.
[0051] Additional modifications and improvements of the present invention may also be apparent to those of ordinary skill in the art. Thus, the particular combinations of parts and steps described and illustrated herein is intended to represent only certain embodiments of the present invention, and is not intended to serve as limitations of alternative devices and methods within the spirit and scope of the invention.
* * * * *
D00000

D00001

XML
uspto.report is an independent third-party trademark research tool that is not affiliated, endorsed, or sponsored by the United States Patent and Trademark Office (USPTO) or any other governmental organization. The information provided by uspto.report is based on publicly available data at the time of writing and is intended for informational purposes only.
While we strive to provide accurate and up-to-date information, we do not guarantee the accuracy, completeness, reliability, or suitability of the information displayed on this site. The use of this site is at your own risk. Any reliance you place on such information is therefore strictly at your own risk.
All official trademark data, including owner information, should be verified by visiting the official USPTO website at www.uspto.gov. This site is not intended to replace professional legal advice and should not be used as a substitute for consulting with a legal professional who is knowledgeable about trademark law.